The WHO has declared obesity as a global epidemic with high rates evident in both developed and developing countries( 1 ). The increasing prevalence of the condition in children and adolescents is of particular public health concern as evidence shows a positive association between childhood and adult obesity( Reference Freedman, Khan and Serdula 2 , Reference Serdula, Ivery and Coates 3 ). This suggests that the true health impact of obesity may exacerbate in the future, compelling public health ministries to declare obesity reduction as a priority population health objective( 4 ).
New Zealand has the third highest population obesity prevalence among the countries of the Organisation for Economic Co-operation and Development, behind the USA and Mexico( 5 ). Like most developed countries, New Zealand’s obesity rates are associated with deprivation, with higher levels observed in low-income groups( 6 – 8 ). Obesity is a major public health problem for Pacific peoples in New Zealand (comprising a diaspora from the South Pacific islands of Samoa, Cook Islands, Tonga, Niue, Fiji, Tokelau and Tuvalu). The conglomerate Pacific ethnic group occupies the lowest socio-economic strata in New Zealand( 9 ). On average, Pacific peoples have worse economic circumstances than the overall population, with the majority of Pacific peoples living in areas with the fewest economic resources( Reference Crampton, Salmond and Kirkpatrick 10 ). Economically, Pacific New Zealanders are over-represented among the unemployed, lower-skilled workers and the low income-earning group( 11 ). In general, communities with fewer economic resources tend to have poorer health outcomes, as lower incomes mean that many of the conditions or factors that support good health, such as good nutrition and quality housing, are less accessible( 12 – Reference Casey, Simpson and Gossett 14 ). Local evidence has shown how poverty in New Zealand compromises food security for these communities and consequently their poorer health status in New Zealand( Reference Rush, Puniani and Snowling 15 – Reference Teevale, Thomas and Scragg 17 ).
In terms of obesity prevalence, Pacific adults (63·7 %) and children (23·3 %) have an almost threefold higher risk of being obese compared with the general population (26·5 % for adults; 8·3 % for children)( 6 ). There is insufficient evidence about what obesity interventions work for this population group. The purpose of the present research was to investigate the acceptability of a weight-management programme for Pacific families with obese children and follow up drop-out participants, to uncover the barriers to programme completion.
Recent reviews on lifestyle interventions for the treatment of obesity in children have concluded that moderate- to high-intensity behavioural lifestyle programmes can reduce the level of paediatric obesity( Reference Whitlock, O’Connor and Williams 18 , Reference Oude Luttikhuis, Baur and Jansen 19 ). However, despite sustained efforts in the development of weight-management programmes to address childhood obesity, threats to efficacy include: low adherence to treatment cycles; behavioural relapse leading to weight regain; and high levels of attrition in interventions( Reference Theim, Sinton and Goldschmidt 20 ). Evidence suggests that in order for weight-management programmes to be effective, participants need to complete the full duration of the programme( Reference Oude Luttikhuis, Baur and Jansen 19 , Reference Hampl, Paves and Laubscher 21 – Reference Wrotniak, Epstein and Paluch 23 ). Inversely, premature termination from a weight-management programme results in incomplete health care for patients that can lead to failure experiences for both patients and health-care providers( Reference Grimes-Robison and Evans 24 ).
Non-compliance in weight-management programmes for children is a major concern for intervention studies. Within the current literature, many intervention studies do not report on factors that lead to participant drop-out in weight-management programmes( Reference Skelton and Beech 22 ). The 2009 Cochrane review found for those studies that reported drop-out rates in childhood obesity interventions, the non-completion rate was as high as 42 % (range 0–42 %). The drop-out rate at 6, 9 and 12 months post-intervention follow-up stages was in the range of 1–42 %, 8–34 % and 7–43 %, respectively( Reference Oude Luttikhuis, Baur and Jansen 19 ). More recently, studies have delved into identifying participant- or patient-level predictors of attrition. Clinic-based weight-management programmes, namely from North America, that reported on patient experiences informed that common factors for non-completion, including medical insurance status, African-American ethnicity, older age, depression, elevated parental BMI, overall health status, location and timing of programme delivery, unfulfilled parental and child expectations of weight loss and multiple previous weight-loss attempts in women, also predicted attrition( Reference Barlow and Ohlemeyer 25 – Reference Cote, Byczkowski and Kotagal 30 ). Fewer community-based weight-management interventions report on participant experiences leading to non-completion. Other possible non-completion factors in community-based lifestyle modification programmes include fear of weight stigmatisation, cultural incongruence between participants and providers, and imprecise programme intensity and duration( Reference Grimes-Robison and Evans 24 , Reference Jelalian, Hart and Mehlenbeck 31 , Reference Williams, Coday and Somes 32 ). The present study aimed to uncover the factors influencing both participant retention and conversely non-completion in a family-led weight-management programme for obese Pacific children in New Zealand. Improving participant retention and minimising attrition are crucial for individual participant success and critical for demonstrating programme efficacy, as well as quality improvement.
Methods
Study design
A qualitative research approach was favoured as it allowed the topic to be explored in depth. Semi-structured face-to-face interviews were completed with parents of obese children who were randomised into the intervention arm of the FANAU FAB weight-management programme. The title of the programme used the Samoan word fanau which translates to the word ‘children’ and the acronym FAB for Food, Activity and Behaviour. FANAU FAB was a parallel randomised controlled trial for obese Pacific children aged 5–12 years and their parent/primary caregiver. The community-based lifestyle behavioural modification programme involved eight weekly group therapy sessions of 90 min duration, delivered in local community venues (schools and churches) in South Auckland, New Zealand. South Auckland was chosen as the region for programme delivery as almost 70 % of Pacific New Zealanders live in Auckland city (177 936) with over one in four living in the South Auckland region. South Auckland is classed as a high deprivation socio-economic area( Reference Crampton, Salmond and Kirkpatrick 10 ). The FANAU FAB programme was guided by the theories of cognitive behavioural modification education used in similar family-based weight-management programmes( Reference Golan 33 – Reference Heinberg, Kutchman and Berger 35 ). At each session, both parents/primary caregivers and children would engage in a family activity in the first half-hour of each session. For the rest of the programme time, children were engaged separately in games and informational activities while their parents/primary caregivers were supported with information, goal-setting tasks and group processes of sharing their lived experiences around FAB (Food, Activity and Behaviour). Upon completion of the 8-week programme, families received maintenance support for 26 weeks, which involved one home visit per family and one follow-up telephone call and/or text message per week. Participant drop-outs were defined as families that completed ≤4 weeks out of the 8-week programme.
Forty-two parents completed post-intervention face-to-face semi-structured interviews. The average age range of participants was 36–45 years. Sampling continued until few new insights were achieved from subsequent interviews. Indigenous Pacific research principles, cultural processes and strategies were followed for interviews( 36 ). Three bilingual researchers in Samoan and Tongan language conducted the interviews. Interviewers familiarised themselves with the participants during their first and last session of the programme to explain the qualitative follow-up study. Interviewers then contacted each parent interviewee by telephone, email or face-to-face via door knocking, to schedule interviews to be held at a location of the participant’s choosing. Most interviews took place at the participants’ home and a few were held at their local church. Each interview lasted approximately 60 min and was recorded with consent, transcribed verbatim and then translated into English language. Participants were offered a $NZ 20 supermarket voucher as a token of appreciation.
The study was conducted according to the guidelines laid down in the Declaration of Helsinki and all procedures involving human subjects/patients were approved by the University of Auckland Human Subject Ethics Committee. Written informed consent was obtained from all participants and identities are protected through the use of pseudonyms in this manuscript and any other published material.
Participants completed a demographic form that captured household size, number of dependant children, birthplace, parental status, household employment status, household income, age range, ethnicity and languages spoken at home. Table 1 summarises the participants’ demographic profile.
Table 1 Demographic details of Pacific parents/primary caregivers (n 42), participants in the family-led FANAU FAB weight-management programme for obese Pacific children, New Zealand
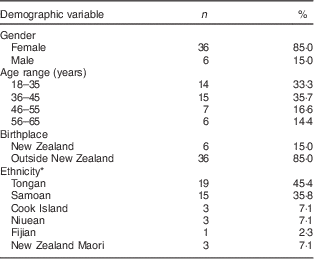
* Ethnicity-all-count, so percentages do not add to 100 %.
Materials
Two interview schedules were prepared, one for those participants who completed the 8-week programme and one for those who had dropped out of the programme. For completers, the scope of the interview included questions on their child’s overall health, physical, emotional and social well-being, the child’s weight-management history and the child’s overall progress in the weight-management programme. Questions on the programme included programme awareness (recruitment into the programme) and aspects of the weight-management programme including materials provided, information content, organisation, personnel and delivery. Participants were asked to identify what aspects of the programme were acceptable and why; and in concert, what aspects were deemed ineffective for changing food and physical activity behaviours in the home environment. Participants were asked questions about the effect of the programme on their child’s and their own weight management and aspects of the programme they found difficult. The interviews ended with questions on suggested future improvements of the programme.
The scope of questions posed to drop-out participants included questions on their child’s health status, programme awareness and recruitment, length of time on the programme and initial programme expectations. Participants then assessed each programme feature listed (materials provided, organisation, information content, personnel and delivery) depending on the length of their participation. For example, those participants who attended only one or two out of the eight weekly sessions would have experienced very minimal contact time at the weekly session(s), and this influenced their commentary. Reasons for non-completion were elicited, as well as future intent and suggestions on programme improvements.
Analysis
Thomas’( Reference Thomas 37 ) general inductive approach for analysis of qualitative evaluation data was used as the analysis framework. The general inductive approach provides a simple, straightforward approach for deriving findings in the context of focused evaluation questions. Two researchers reviewed each transcript and condensed the raw textual data using focused evaluation questions to guide the analysis. The purpose of the analysis was to categorise, summarise and present key themes in order of importance to participants. All available data were analysed to fit within evaluation research questions’ objective headings. The computer software program NVivo7 was used to analyse, sort and code the interview data.
Results
Table 1 shows the demographic details of study participants. The majority of participants were women who had not been born in New Zealand (85 %), and included mothers, aunts and grandmothers. Participants of Tongan ethnicity were most numerous, although 30 % of the participants were from multi-ethnic households. The average household size was 6·3 (range 1–11); the average number of dependant children per household was 3·1 (range 1–7). Eighty-five per cent of the participants were from two-parent households and 85 % were employed households. The average estimated household income, not equivalised to household size, was $NZ 50 000–60 000. Ninety per cent of the sample spoke an Island language at home; 60 % spoke at least two languages in the home.
Programme awareness and initial programme expectations
Participants identified the following ways they were recruited into the FANAU FAB weight-management research programme: through referral from their local school nurse; receiving a school newsletter home; hearing a church notice or announcement made after Sunday church service; through a doctor referral from a Pacific health provider; reading an advertisement in the local newspaper; receiving word-of-mouth information from a family member; and through interaction with a research project recruiter at a local shopping mall.
Parents were attracted to enlist in the weight-management programme because it was ‘family-based’ and therefore parents and children could actively participate together and provide support to each other. As one mother said: ‘I thought that it was good, ’cause he and I were doing it together, and he wasn’t doing it on his own’ (Tani, Cook-Island mother). Parents’ reasons for joining the programme included: addressing their child’s obesity for health reasons; to prevent a family history of diabetes; for children to be more active and gain energy; and to mitigate teasing and bullying for their overweight child. Some participants had expectations of a culturally delivered programme and were attracted to the programme because of its Pacific name.
Acceptable programme features
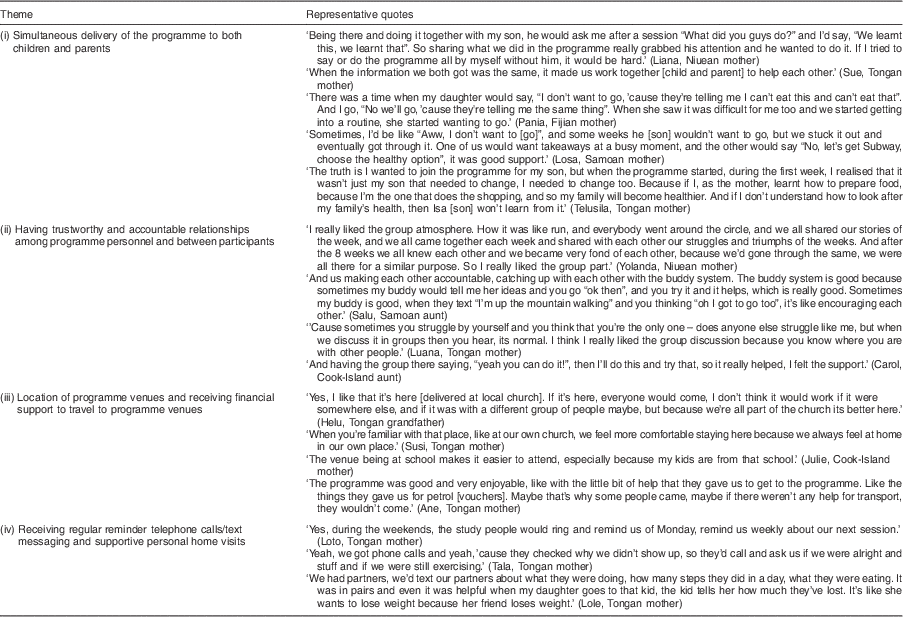
We identified four key themes from the data that participants identified as satisfactory programme features that had impacted their retention: (i) the simultaneous delivery of the programme to both children and parents; (ii) having trustworthy and accountable relationships among programme personnel and between participants; (iii) location of venues and receiving financial support to travel to programme venues; and (iv) receiving regular reminder telephone calls/text messages and supportive personal home visits. Table 2 outlines these four themes with representative quotes from participants illustrating each theme.
Table 2 Acceptable weight-management programme features and their representative quotes extracted from qualitative interviews with Pacific parents/primary caregivers (n 42), participants in the family-led FANAU FAB weight-management programme for obese Pacific children, New Zealand
Reasons for dropping out
The primary influencer on non-completion was an unpredictable lifestyle event that impacted participants’ time commitment to complete the programme. Changes in work schedules and work shifts at short notice severely impacted parents’ retention in the programme. Transport issues and having to rely on other working family members as drivers to attend the programme caused missed sessions. Cultural obligations like meeting extended family needs also had an impact on programme participation as illustrated by the following collection of quotes:
‘We missed the last few weeks, ’cause actually we had a funeral and we weren’t able to attend.’ (Ani, Tongan mother)
‘It became difficult when my husband’s work shift changed, he couldn’t be home to look after the family [members], so I had to stay home and we couldn’t do the programme.’ (Lana, Cook-Island mother)
‘Because my baby was sick, in the hospital, so we missed the last four sessions.’ (Mata, Samoan mother)
‘The only reason why I pull out from the programme was because my [elderly] mum came from the islands to stay with us … and there’s no one to look after her here at home.’ (Rosa, Samoan mother)
Suggested future programme improvements
Several participants talked about increasing the programme duration from 8 weeks to 12 weeks most commonly. This was related mainly to group members feeling like they needed more support for behavioural change, both for the child and for adults. As one mother stated, this was ‘so that the children can get more involved as a group with other children of the same age. If there was just maybe an extension group for the kids, bring in another activity or group thing to do, to keep them more together’ (Tala, Tongan mother).
‘I wish it could have been like 12 weeks, longer. Because like, just being in the programme, keeps you motivated, ’cause when you do it by yourself, just doing it yourself at home, it’s kind of hard. But when you have a group and you’re always there, it motivates you ’cause you’re hearing other people share their stories.’ (Loseta, Cook-Island mother)
‘I still think that the 8 weeks was enough, but ’cause some of us were worried we weren’t going to do it [on our own] because we’re so used to doing it every week.’ (Pania, Fijian mother)
Additionally, most participant suggestions for future programme improvements were related to more practical hands-on sessions like cooking demonstrations and healthy food shopping expeditions:
‘I would have loved it if there was a session on cooking, like, get in a chef or someone, a dietitian, to come, because its different, saying “take the fat from like the corn beef”, with actually showing it to the people. Those kind of things, like the portion sizes, come and show us the portion size, instead of maybe if the plate is this big, but actually show portion sizes to the parents so they can see it for themselves, see it being done.’ (Sana, Tongan mother)
‘If they had planned it where we were actually active, you know [say to us] “okay parents this is the scenario, there’s your [local] shopping centre over there and this is how much you’re going to spend”. And actually get us up and moving, going in with say 20 dollars to spend, and learning to create a family meal for what I can buy. That would have been good.’ (Varia, Cook-Island mother)
Much feedback was received on better culturally specific delivery of the programme. There was a clear language and therefore cultural barrier, especially for the programme delivered to one specific Island ethnic group:
‘For me if it were delivered in Tongan it would have been clearer, because the majority of us may not understand English. Remember, when it comes to the discussions, there are some that can speak English and others who can’t. There were times when we asked if it could be translated, and I think that time was wasted on translations. I remember they asked us questions and I hardly said anything … we’re shy people.’ (Eli, Tongan grandfather)
Aspects of a culturally appropriate Pacific programme were further suggested. A Pacific tailored approach was explained by one participant to be practical and grounded in real-life experiences. Many participants indicated a preference for ‘Pacific families that had gone through what you’re going through, come in and kind of tell you what they’d gone through, and what they’d learnt and what helped them. This would have helped me. …We’re more the “do” than the sit down [approach]. … Like we’re all brown faces, but it was evident that it was coming from a Palagi model. The types of questions that we were being asked, was like we were kind of ticking boxes, and that’s what it felt like sometimes. ’Cause they were looking at their papers, and just going through theory. And you don’t want to hear theory when you’re a mum. You want to hear real-life experience and what’s practical for us as Pacific people’ (Ata, Samoan mother).
There was a gender trend with the men participants indicating a preference for more physical activity/exercise inclusion as part of the programme, while the women were satisfied with the original predominantly discussions format.
One of the suggestions for future change was to include many more family members as part of the programme. This was to alleviate what most in the programme identified as the most difficult aspect of making household family-based food and activity changes: familial sabotage. As represented by the quote below, when other parents and children in the same household were not exposed to the programme, it proved difficult for participants to effect change in the home environment:
‘The thing I found most difficult was facing my family. During the first week, my kids weren’t use to the proportions I gave them on their plate. The biggest problem was my husband, because I’d try to cut back on the fizzy drinks but he goes and brings fizzy drinks … It was a lot more helpful, and easier when we were both part of it [weight-management programme] because we came to have a mutual understanding and about the importance of being healthy.’ (Telusila, Tongan mother)
Most participants confirmed that a programme scheduling of once weekly was sufficient and time-manageable. Programme delivery over both school term and school holidays was not problematic and timing for after-school or after-work hours was also preferred. Having the programme delivered on a weekday was favoured because families had obligations to meet on weekend days, like church and sporting activities.
Unintended benefits of the programme
Most participants explained that their initial expectations were only for their child to receive benefits from attending the programme. That is, that the weight loss and physical health benefits would accrue to their child only. Most participants were therefore pleasantly surprised at their own weight-loss achievements from the programme, as illustrated below:
‘When I started this programme, I was 89 kg but now it’s going down to 84 kg at the moment, which I thought “wow”. … Yeah, which I think it’s more from the activity and like portioning our food.’ (Faafetai, Samoan mother)
These unintended weight-loss experiences for parents spurred them on for more household health changes, applying changes in the home that affected other family members, who were then encouraged by their physical health changes and their role modelling within the home:
‘Eventually all our kids came and joined in; so we’ve got a 12-year-old and a 7-year-old and a 5-year-old; so they all came and do the exercise and that. So even the older one, she’s also watching what she’s eating now since we’ve done this, a lot more than before.’ (Carol, Cook-Island mother)
Being part of the programme gave some participants greater social engagement and they made new friends. Some participants with other children identified that the service provided by the programme for child care during the session enabled them to attend.
Discussion
The factors that influenced participant retention in a family-led weight-management programme for obese Pacific children included the strong emphasis on family and group participation and sharing learning experiences in tandem between children and parents. The shared experience and the adult role modelling seemed effective for children’s motivation to participate. In addition, the way in which children were able to encourage parents to attend or to hold firm in behavioural change was an unfamiliar finding. Parental modelling has been found in the literature to be effective in controlling children’s nutrition and weight control( Reference Wrotniak, Epstein and Paluch 23 , Reference Golan 33 , Reference Campbell, Crawford and Salmon 38 , Reference Brown and Ogden 39 ), while the way in which reciprocal social support was enacted from child to parent was interesting to find in the present project.
Participants alluded to being attracted to the weight-management programme through its emphasis on delivering a model suitable for a cultural group. As suggested programme improvements, having ethnic-specific Island-language delivery, having successful Pacific weight-loss role-model families and having more practical sessions (e.g. cooking classes and shopping expeditions at local food stores using a budget) were the particular features identified by participants in the trial. The study participants alluded to being attracted to joining the programme because it was targeting their particular ethnic grouping: Pacific. In this sense, they had expectations that its delivery would include some specific differences compared with, in their own words, ‘Palagi’ or non-Pacific mainstream Western models of delivery. Having information content delivered in a Pacific-Island language and having successful Pacific weight-loss role models were their particular recommendations for future programme delivery. In addition, having a programme with more practical application of theory or informational content (like food cooking demonstrations or food shopping expeditions) was also deemed more specifically ‘cultural’ than mainstream or typical models of programme delivery. Interestingly, the ideas for practical elements to be included in future programmes have been tested in other health interventions with promising results( Reference Kahn, O’Sullivan and Vannatta 40 , Reference Baic and Thompson 41 ). Hands-on cooking experiences were found to be more effective in retention of nutritional knowledge and consequential application in home cooking( Reference Levy and Auld 42 ). In addition, supermarket or food shopping tours have been used by other low-income population groups, showing positive effects in making healthy food choices( Reference Carson and Hedl 43 – Reference Liebman, Heffernan and Sarvela 45 ). Previous trials have identified that cultural dissonance in programme delivery predicted attrition( Reference Tershakovec and Kuppler 28 , Reference Carroll, Yancey and Spring 46 , Reference Yancey, Ortega and Kumanyika 47 ). The present study makes a contribution in identifying programmatic elements that could be modified to enhance retention for this at-risk group.
Additionally, the focus of the study was also to uncover the factors that predicted attrition in a family-led weight-management programme for obese Pacific children in New Zealand. The literature on community-based programme attrition can be described as currently being undersized. The present research found that unpredictable external life crises like extended family deaths, a change in job shifts, family illnesses (both acute and those requiring chronic management) and long-term family visitations affected participation and momentum. A loss of momentum through managing life crises was often difficult to overcome for participants, leading them to drop out of the weight-management programme. Uncovering previously unknown factors that predict non-completion is a necessary step to programme improvement. Interventionists can assess how these factors can be addressed for future programmes. The present study found that most drop-out participants preferred to defer their programme participation with hopes of re-committing to future programmes at another time. This recommendation from participants highlights the discordance between interventional weight-management programmes implemented for research purposes v. real-life scenarios which can often be successfully addressed in clinical settings. Our research study had to limit its definition of ‘participant’ and ‘drop-out’ because it was interested in capturing dose-and-effect outcomes in a limited-time intervention programme. In real-world settings, it is recommended for weight-management programmes to have rolling retention policies and procedures, to enable participants to be captured in the programme and to allow flexibility in their entry and exit. Like other behavioural change programmes in the health arena, for example in smoking( Reference Garvey, Bliss and Hitchcock 48 ) or alcohol management( Reference Brown, Vik and Patterson 49 ), weight management also involves periods of relapse and re-commitment( Reference Kaholokula, Mau and Efird 50 – Reference Wing and Phelan 52 ) that can be difficult to capture in limited-time research interventions. Our study enabled us to explore, with the participants, how they felt they could manage their programme participation in the face of trying to manage life crises and changes. Keeping in contact with drop-out participants over time and inviting them to re-enter future programmes is recommended.
Conclusions
Given the elevated and inequitable obesity risk for both child and adult Pacific New Zealanders, the results of the present research project will be of value in informing public health responses to addressing obesity risk in this population group. To the authors’ knowledge, no other evidence has been presented on the factors that predict attendance and attrition in weight-management programmes for this at-risk group. Identifying elements critical to producing efficacious weight-management programmes within the community has the potential to produce better and equitable health outcomes.
Acknowledgements
Acknowledgements: The authors thank the community interviewers, Ingrid Tanoa and Helen Tagaloa, for their research assistance. They also thank the FANAU FAB research team, Dr Ofa Dewes, Dr John Sluyter and Mr Gavin Faeamani, of the Pacific Health Department, University of Auckland, New Zealand. Financial support: HRC Post-doctoral Career Development Award, Pacific Health Department, University of Auckland for T.T. This work was supported by a grant from the Health Research Council of New Zealand. The Health Research Council of New Zealand had no role in the design, analysis or writing of this article. Conflict of interest: None. Authorship: T.T. designed the study, conducted interviews, analysed the transcripts and wrote the manuscript, S.T. conducted interviews, analysed the transcripts and contributed to the final manuscript, T.P. had overview of the project and contributed to the final manuscript. Ethics of human subject participation: The University of Auckland Human Subject Ethics Committee granted ethical approval for the study.







