Poster Presentation - Top Oral Abstract
Antibiotic Stewardship
Identifying Outpatient-Specialized High-Volume Prescribers of Antibiotics in Older Adult Populations – Philadelphia, PA 2021
- Giovanny Zapata, Jenna Scully, Tiina Peritz, Jane Gould
-
- Published online by Cambridge University Press:
- 16 September 2024, p. s1
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Inappropriate antibiotic use promotes antibiotic resistance which poses a threat to public health. Outpatient settings are responsible for 80-90% of all antibiotic use, yet up to 50% of these prescriptions may be inappropriate and at least 33% completely unnecessary. To promote outpatient antibiotic stewardship (AS), the Philadelphia Department of Public Health (PDPH) identified outpatient high-volume prescribers (HVPs) in Philadelphia and provided them with peer comparison letters along with evidence-based AS educational resources. Method: We identified HVPs using overall and drug specific antibiotic volume and rates from the Centers of Medicare and Medicaid Services (CMS) Part D Prescribers by Provider and by Provider and Drug publicly available datasets for 2021. We restricted analyses to Philadelphia prescribers specializing in internal medicine, family practice, or general practice with antibiotic and beneficiary claim counts ≥ 11. We further restricted the Provider and Drug dataset to prescribers of high-consequence drugs: levofloxacin, ciprofloxacin, and azithromycin. Prescribers with subspecialities where these three drugs are commonly used appropriately were excluded from letter distribution. We analyzed U.S. Census Bureau American Community Survey (ACS) data for overall HVPs on census tract-level to describe health equity demographic characteristics. Result: A total of 1,001 prescribers with 67,145 total antibiotic claims, and 306 unique prescribers (77 levofloxacin, 176 ciprofloxacin, and 250 azithromycin) with 37,057 total antibiotic claims met the inclusion criteria in the Provider and the Provider and Drug datasets, respectively. There were 101 overall HVPs, and 89 unique drug-specific HVPs (20 levofloxacin, 45 ciprofloxacin, and 63 azithromycin) based on the highest 10% and 25% of prescribers by antibiotic volume, respectively. The overall HVPs contributed 42.0% of all antibiotic claims. The drug-specific HVPs contributed 60.5% of all antibiotic claims and 55.5% of levofloxacin, ciprofloxacin, and azithromycin claims. These 3 drugs contributed 45.1% of all antibiotic claims. Among the overall and drug-specific HVPs, we sent peer comparison letters to the top 10 by rate per 1,000 beneficiaries (overall) and per 1,000 antibiotic claims (drug-specific), who fell within the following prescribing rates: overall 954-2,714, levofloxacin 84-396, ciprofloxacin 288-723, and azithromycin 496-1,000. Conclusion: This initiative identified prescribers at risk for inappropriate use of antibiotics, and empowered these same prescribers to self-reflect on how they prescribe antibiotics. Efforts by local health departments to provide HVPs with peer comparison feedback and AS educational resources may improve the provider knowledge and prescribing habits across different healthcare systems, targeting prescribers at highest risk for misuse or overuse of antibiotics.
Disclosure: Jane Gould: Spouse receives salary support- Incyte
COVID-19
Association between hospital-onset SARS-CoV-2 and ending universal admission testing and masking at five US hospitals
- Theodore Pak, Sanjat Kanjilal, Cara McKenna, Chanu Rhee, Michael Klompas
-
- Published online by Cambridge University Press:
- 16 September 2024, pp. s1-s2
-
- Article
-
- You have access Access
- Open access
- Export citation
-
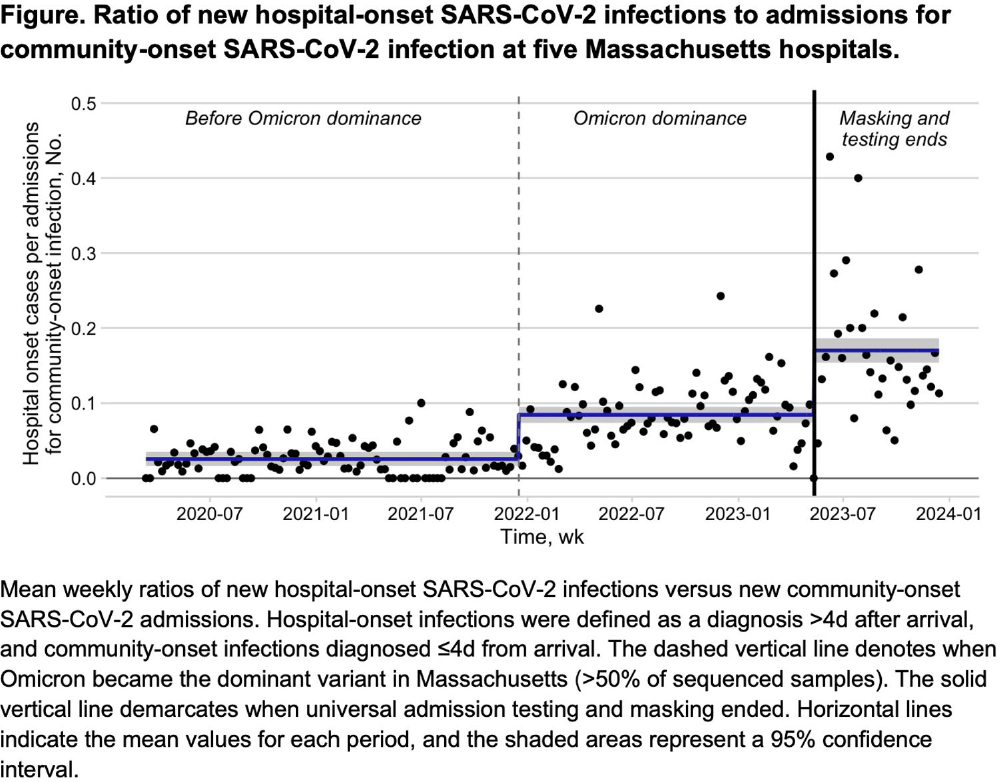
Background: Many US hospitals have stopped universal masking and testing all patients on admission for SARS-CoV-2. We assessed the association of ending universal masking and admission testing with the incidence of hospital-onset SARS-CoV-2 infections in five Massachusetts hospitals. Method: We conducted a retrospective study of all patients admitted between March 6, 2020 and December 14, 2023 and identified hospital-onset SARS-CoV-2 infections (newly positive SARS-CoV-2 PCR tests >4d after arrival) and community-onset infections (newly positive ≤4d after arrival). We excluded cases if local infection control teams discontinued precautions within 4d (suggesting a false positive or remote/resolved infection). We calculated weekly ratios between hospital-onset and community-onset SARS-CoV-2 cases to account for changes in community SARS-CoV-2 incidence over time. We then performed interrupted time series analysis, looking for changes in the ratio of hospital-onset to community-onset cases across three periods: pre-Omicron period with universal testing and masking in place (March 6, 2020–Dec 16, 2021); Omicron period with universal testing and masking in place (Dec 17, 2021–May 11, 2023); and Omicron period without universal testing and masking (May 12, 2023–Dec 14, 2023). We performed medical record reviews on 100 randomly selected hospital-onset cases after May 12, 2023 to examine if community-onset cases were being misclassified as hospital-onset cases. Result: During the study period, there were 626,908 patient admissions, including 24,980 with community-onset and 1,510 with hospital-onset SARS-CoV-2 infections. The mean weekly ratio of new hospital-onset to community-onset SARS-CoV-2 infections rose from 2.6% before Omicron, to 8.5% (95% CI, 7.0–9.9%) during Omicron, to 17% (95% CI, 15–19%) after universal admission testing and masking ended (Figure 1). There was a significant immediate level change after the pre-Omicron-to-Omicron transition (140% relative increase; 95% CI, 40–240%) and after universal admission testing and masking ended (110% relative increase; 95% CI, 73–150%). On medical record review of 100 randomly selected hospital-onset SARS-CoV-2 cases after universal admission testing had ended, 89% had new symptoms at the time of testing, 80% had PCR cycle thresholds ≤30, 27% had a known COVID-19 exposure, and 97% met at least one of these criteria. In-hospital mortality occurred in 8% of the 100 reviewed cases. Conclusion: Stopping universal masking and admission testing of all hospitalized patients at five Massachusetts hospitals was associated with a significant increase in hospital-onset COVID-19. Nosocomial COVID-19 remains a common complication of hospital care. Preventing nosocomial infections in this vulnerable population remains an important safety goal.
Disclosure: Theodore Pak: Founder/CEO - The East Harlem Software Company, Inc.
DEI
Iterative Health Equity Analyses of Central Line-Associated Bloodstream Infection (CLABSI) Events at a Pediatric Hospital
- Ana Vaughan-Malloy, Phillip Hahn, Paula Lamagna, Jenny Chan Yuen, Dionne Graham, Jennifer Ormsby
-
- Published online by Cambridge University Press:
- 16 September 2024, p. s2
-
- Article
-
- You have access Access
- Open access
- Export citation
-
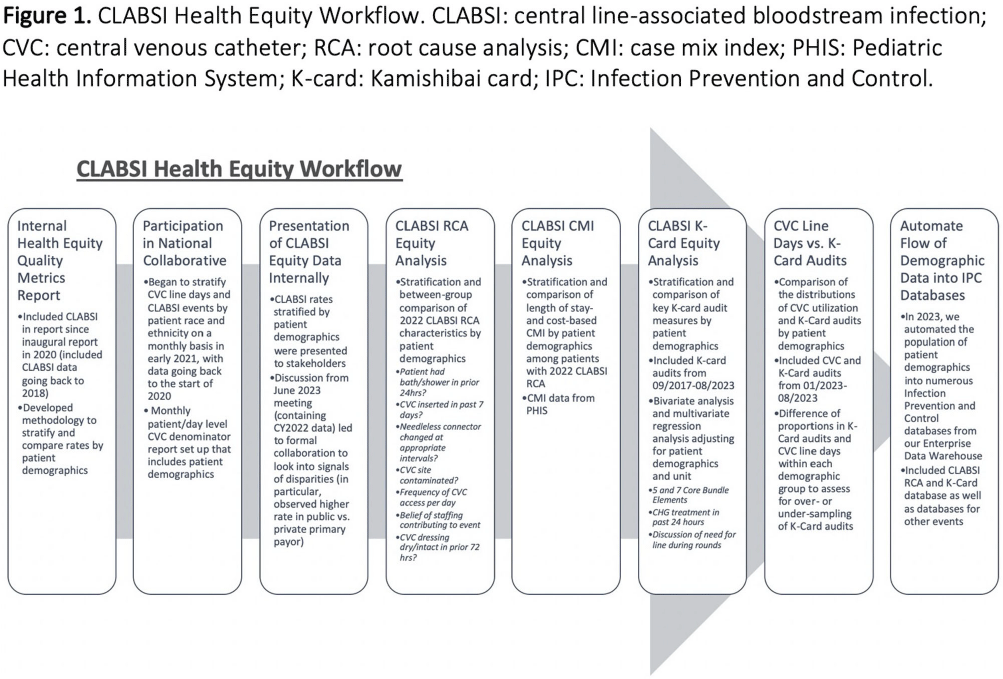
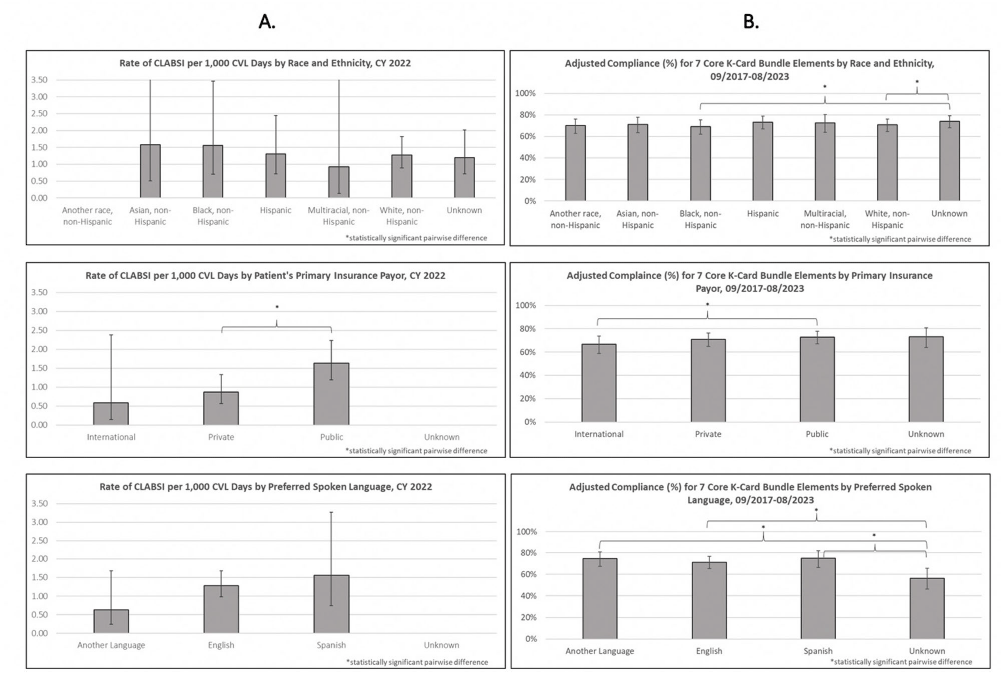
Background: Per the Centers for Disease Control and Prevention, health equity stipulates all have a fair, just opportunity to attain their highest level of health. Limited evidence exists for disparities in health equity and healthcare-associated infections (HAI), with no evidence on language or primary insurance payor. While reviewing quality metrics, a disparity signal in central line-associated bloodstream infections (CLABSIs) prompted a multidisciplinary deep dive, with iterative analyses to understand potential inequities to identify improvement opportunities. Methods: CLABSI data was stratified and analyzed for evidence of disparity by race/ethnicity, primary insurance payor, and preferred spoken language utilizing an internal methodology. Subsequent analyses included a root cause analysis (RCA), case mix index (CMI) analysis, analysis of CLABSI Kamishibai card (K-card) rounding to monitor maintenance bundle reliability, and comparison of distribution of central venous catheter (CVC) line days to K-card audits [Figure 1]. Chi-square tests were used to test for significant differences for categorical variables in RCA and K-card analyses. ANOVA was used to compare CMI between demographic groups. Multiple logistic regression was used to compare K-card compliance rates by demographic groups. Results: When stratifying CLABSI rate by primary payor, pairwise comparisons indicated patients with a public payor had a statistically higher rate of CLABSI compared to private (p=0.02) [Figure 2A]. RCA analysis revealed when compared to patients with private payors, those with public had significantly higher rates of overdue needless connector changes (p = 0.03) and increased number of daily CVC entries (p = 0.05), while patients speaking another language (p = 0.02) were significantly more likely to have CVC contamination events. CMI analyses on CLABSI cases did not show patient acuity to vary significantly between demographics. Bivariate analysis of K-card data revealed minor differences in reliability with 7 Core Maintenance Bundle Elements by demographics; adjusting for all demographics and accounting for unit, pairwise comparisons indicated public payors had significantly higher compliance than international [Figure 2B]. We found no major differences in demographic distribution of CVC line days compared to K-card audits, suggesting we representatively audit maintenance bundle process measures. Conclusions: Our review of health equity in CLABSI events ultimately led to subsequent questions requiring analysis of other data sets. Utilizing an exploratory approach and assembling a multidisciplinary team to identify potential drivers of identified disparities adds value to health equity analyses. This is the first description of HAI data beyond race and ethnicity and can assist other institutions in their process of evaluating healthcare disparities and HAIs.
Exploring Socioeconomic Disparities in Surgical Site Infections
- Michael Dewitt, Caroline Reinke, Michael Inman, Werner Bischoff, Shelley Kester, Mindy Sampson, Anupama Neelakanta, Katie Passaretti
-
- Published online by Cambridge University Press:
- 16 September 2024, pp. s2-s3
-
- Article
-
- You have access Access
- Open access
- Export citation
-
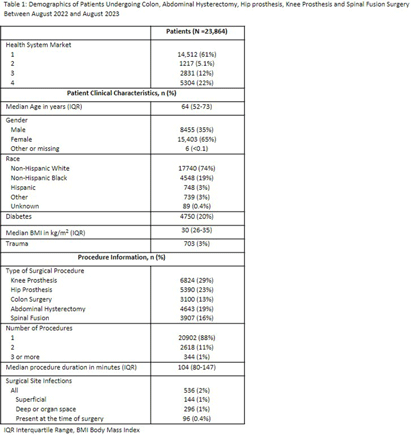
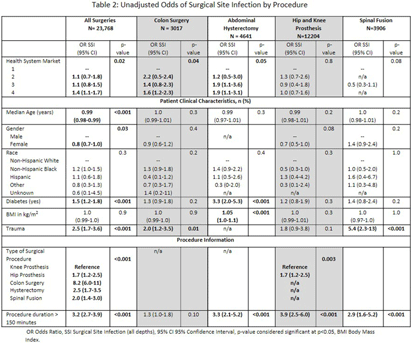
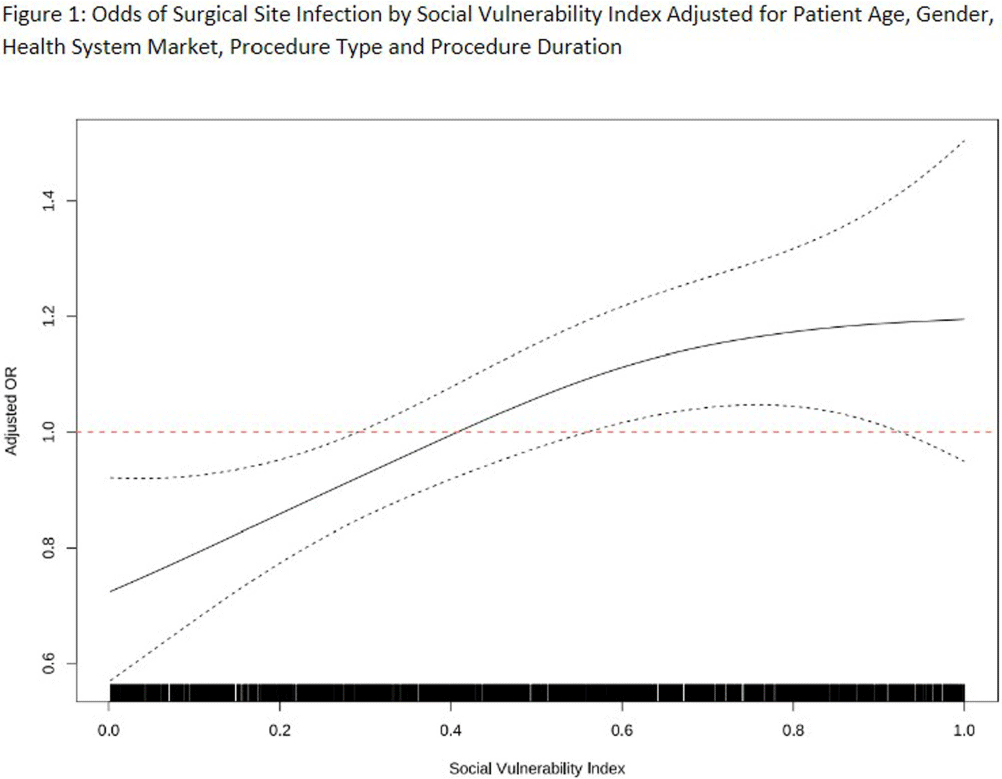
Introduction: Social disparities have been shown to impact a wide variety of healthcare outcomes. Surgical site infections (SSIs) are associated with substantial patient morbidity, but studies on the intersection of social disparity and SSI are limited. We sought to evaluate the association between SSI and the Center for Disease Control and Prevention’s social vulnerability index (SVI). Methods: Patients with National Health Safety Network (NHSN) procedure codes for colon, abdominal hysterectomy, hip prosthesis, knee prosthesis and spinal fusion surgeries were retrieved from the electronic medical records of 20 hospitals across 4 geographic markets. SSIs were identified by trained infection preventionists using NHSN definitions. Descriptive statistics were used for baseline demographic and clinical characteristics. Univariate logistic regression was performed to assess the association of demographic, clinical, and procedural factors with the outcome of SSI. Further univariate subgroup analysis was completed by procedure. To account for the nonlinear relationship between the social vulnerability index and SSIs, smoothing splines were used in a Bayesian hierarchical logistic regression model, with random effects to account for the different market practices. Nonlinear effects of procedure duration were also investigated while adjusting for the patient age, procedure type, and health system market. Results: 23,864 surgical procedures among 22,319 unique patients identified between 1 August 2022 and 31 August 2023. 96 patients with infection present at time of surgery were excluded. The study population was mostly white (74%) and female (65%) (Table 1). Less than 13% of the patients had more than one procedure during this time. In a univariate analysis, we found evidence of market and procedure effects, with colon surgery being associated with the highest odds of SSI. Procedure duration was significantly associated with SSI in both univariate and multivariable models, with a drastic increase in the odds of SSI for procedures > 150 mins. In the multivariable model we found that SVIs lower than 0.4 (95% CI 0.28 to 0.55) are associated with an adjusted odds ratio (aOR) < 1. (Figure 1) Conclusions: Our study shows that the relationship of social vulnerability and adverse outcomes is highly complex with nonlinear dynamics at play. After adjusting for procedure type, duration, patient age, gender and health system market the odds of SSIs increase sharply in patients with higher SVI until leveling off at an elevated risk.
Poster Presentation - Top Poster Abstract
Antibiotic Stewardship
Multifaceted Implementation Strategy to Improve the Comprehensive Assessment of Penicillin Allergies in Perioperative Patient
- Eileen Carter, Carol Schramm, Katherine Zavez, Meagan Zolla, Katelyn Baron, David Banach
-
- Published online by Cambridge University Press:
- 16 September 2024, pp. s3-s5
-
- Article
-
- You have access Access
- Open access
- Export citation
-
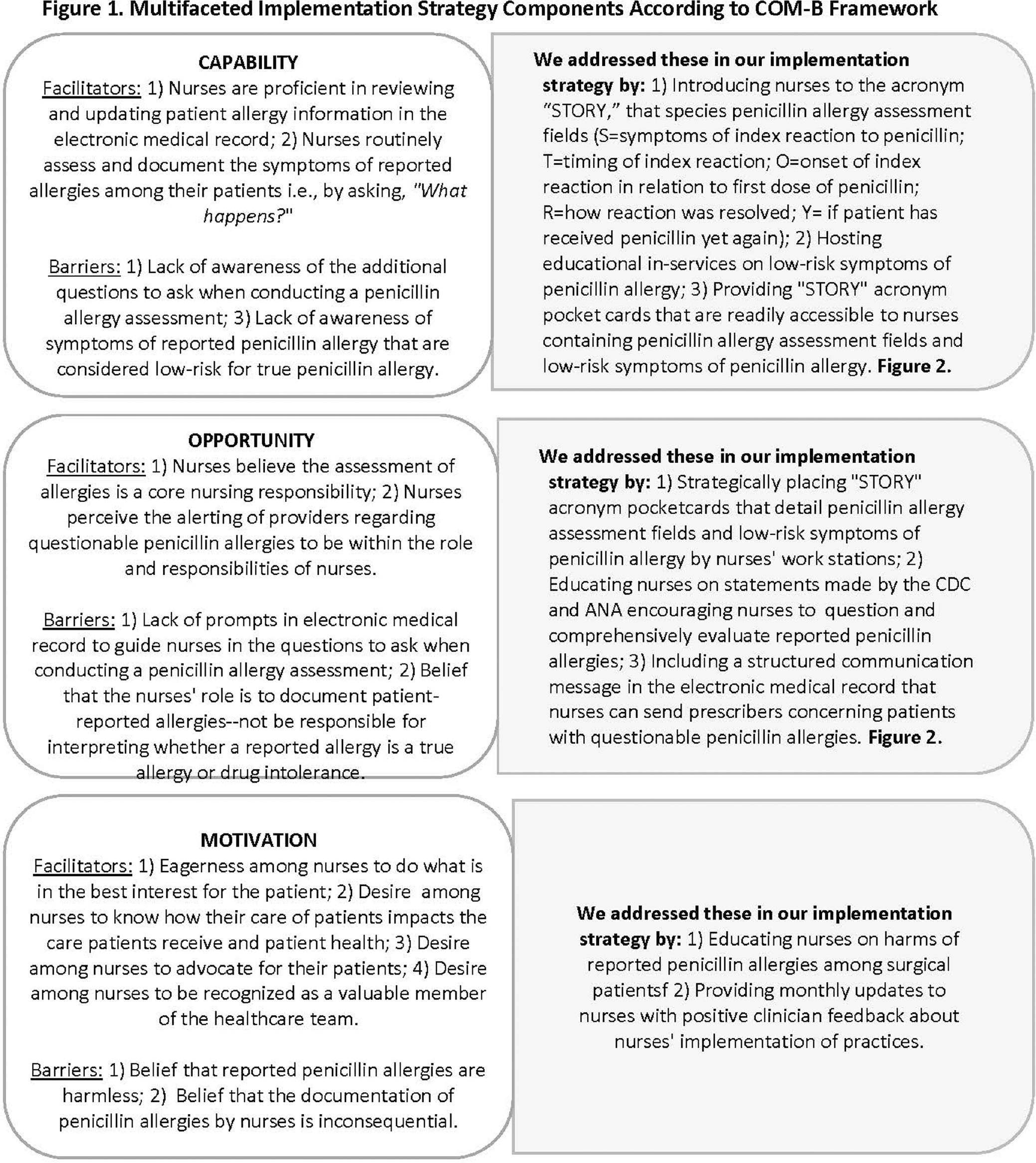
Background: The CDC recommends that nurses improve the evaluation of penicillin allergies as part of antimicrobial stewardship programs. We evaluated the feasibility of a multifaceted implementation strategy to improve nurses’ documentation of penicillin allergy histories and to encourage nurses to notify prescribers of patients with low-risk symptoms of reported penicillin allergy. The implementation strategy was guided by the COM-B model of behavior change and addressed nurses’ capability, opportunity, and motivation to implement practices (Figure 1). The implementation strategy included education on the STORY mnemonic that details the questions of a penicillin allergy history, education on low-risk symptoms of penicillin allergy, dot phrases in EPIC to facilitate nurses’ documentation of STORY and communication of patients with low-risk penicillin allergy symptoms, and educational pocket cards and flyers. We define feasibility as the implementation and acceptability of practices. Methods: This was a six-month feasibility study conducted in an outpatient perioperative area. We compared penicillin allergy documentation pre- and post- implementation strategy and report on nurses’ notification of prescribers regarding patients with low-risk penicillin allergies in the post-implementation period. We engaged nurses in a focus group to assess factors that facilitated or hindered practice adoption. Results: A total of 426 unique patients with 482 penicillin allergy records were included in our study (n= 207 records pre-implementation, n = 275 records post-implementation). We found little to no change in the percentage of records that included symptom information post vs. pre-implementation (88.36% vs 88.41%). A greater percentage of allergy records in the post vs. pre-implementation periods included information on: timing/years since reaction (25.6% vs. 8.2%), onset of reaction (20.7% vs. 0%), resolution of symptoms (20.4% vs. 0%), and penicillin re-exposure (21.1% vs. 2.4%). There were 24 documented instances of nurses’ notifying prescribers of patients with a low-risk penicillin allergy. Focus group data revealed nurses perceived their comprehensive documentation of penicillin allergies highly acceptable and likely to improve patient care and outcomes. Whereas nurses’ notification of prescribers concerning patients meeting low-risk penicillin allergy criteria had little appeal. Nurses described the STORY mnemonic, pocket cards describing the penicillin allergy assessment mnemonic, and the associated dot phrase in EPIC as particularly helpful. Conclusions: A multifaceted implementation strategy showed promise in improving the comprehensive documentation of penicillin allergy histories. Future studies are needed to determine the efficacy of the multifaceted implementation strategy on penicillin allergy documentation, the selection of antibiotic prophylactic treatment, and clinical outcomes among surgical patients.
User-Centered Education for Patients/Caregivers about Urinary Tract Infections, Asymptomatic Bacteriuria, and Antibiotics
- Alistair Thorpe, Karen Fong, Hannah Hardin, Brandi Muller, Julie Szymczak, Andrea White, Valerie Vaughn
-
- Published online by Cambridge University Press:
- 16 September 2024, pp. s5-s6
-
- Article
-
- You have access Access
- Open access
- Export citation
-
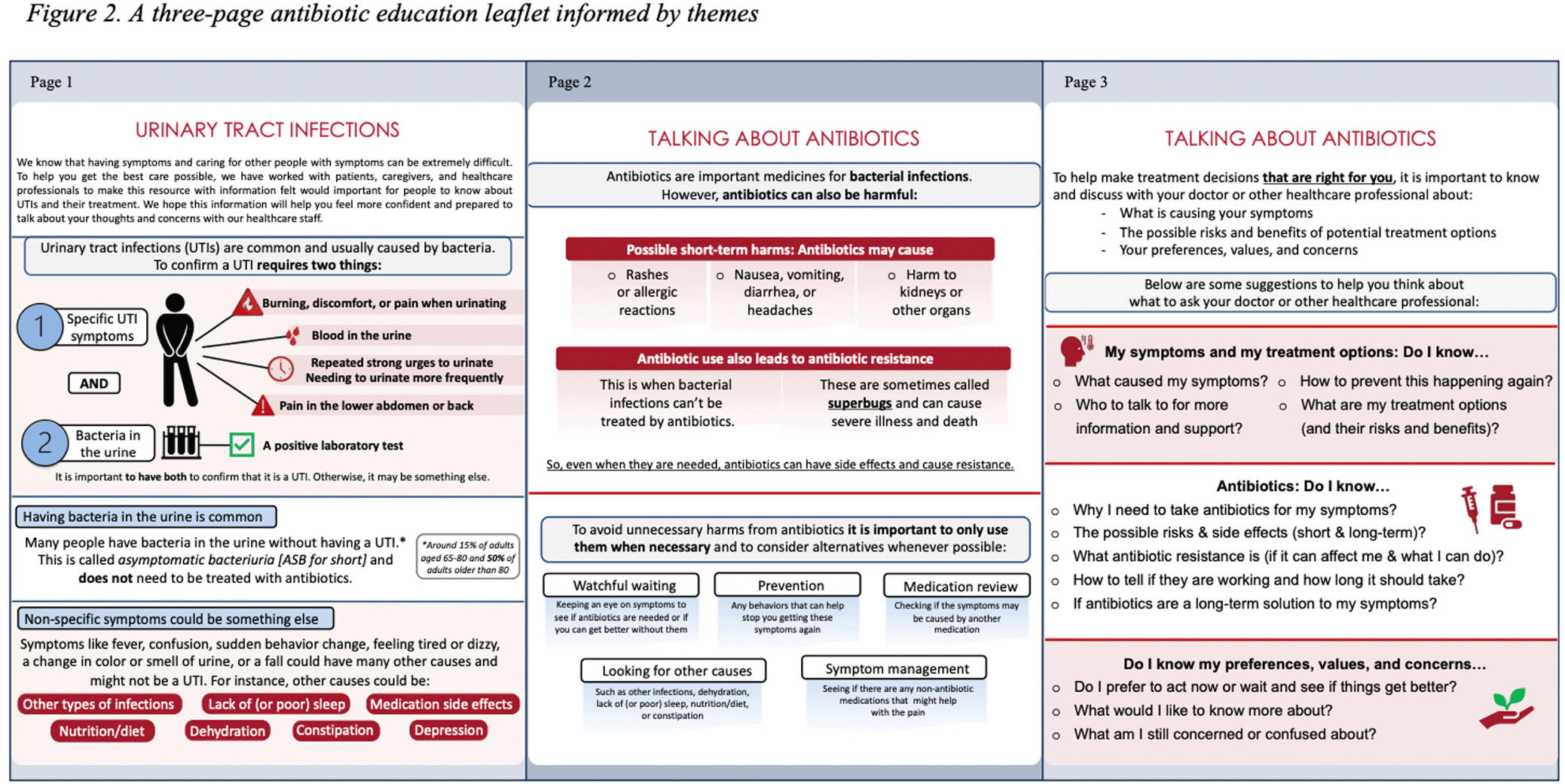
Background: Older adults (aged ≥65) are at high risk of harm from overdiagnosis and overtreatment of urinary tract infections (UTIs) with antibiotics. Involving patients/caregivers in their antibiotic treatment decisions has potential to improve prescribing. To engage effectively, patients/caregivers must have sufficient knowledge about UTIs, asymptomatic bacteriuria (ASB: bacteria in the urine without signs of UTI), and antibiotics and opportunities to share their concerns and treatment preferences with healthcare staff. Patient education is one of the core elements of antibiotic stewardship recommended by the Centers for Disease Control and Prevention but, there are few resources for patients/caregivers about UTIs and antibiotics, leaving a knowledge gap as to what effective patient/caregiver antibiotic education for UTIs looks like. We sought to better understand the perspectives of patients/caregivers at high-risk of antibiotic overuse for UTIs and create an educational leaflet on UTIs, antibiotics, and ASB. Method: Between 11/2022 and 03/2023, we conducted virtual semi-structured interviews with patients ≥65yrs who had experienced UTI and caregivers about their needs, experiences, and preferences for educational support. Interviews lasted ~1 hour. Audio recordings were transcribed verbatim. NVivo software managed the data, which we analyzed using thematic analysis. Results: We conducted 9 interviews (5 patients, 4 caregivers). Interviewees expressed desire to be involved in their treatment decisions and learn more about antibiotics and alternative strategies (themes shown in Figure 1). Reported reasons for limited involvement in decisions included lacking the knowledge and confidence to ask questions, emotional factors (e.g., embarrassment/stress), deference to healthcare staff, and time constraints. Healthcare staff behaviors were described both as barriers (e.g., assertive treatment decisions) and facilitators (e.g., effective communication) of patient/caregiver engagement. Interviewees were eager for printed and digital educational support that could provide tailored content to help improve their knowledge and prepare for future conversations with healthcare staff. From this feedback we developed an educational leaflet (Figure 2). Conclusions: Involving patients/caregivers in antibiotic treatment decisions represents an opportunity to intervene before patients experience antibiotic overuse. Our findings offer important insights on patient/caregiver’ educational needs and preferences as well as perceived barriers to engaging in antibiotic treatment decisions for UTI. We used these insights to inform the development of educational materials about UTIs, ASB, and antibiotics for patients/caregivers and plan to test their use through multiple mediums with tailoring for unique patient needs, experiences, and backgrounds.

Antimicrobial Use in Veterans Affairs Community Living Centers, 2015 - 2019
- Christian Dalton, Tina Willson, Brigid Wilson, Taissa Bej, Nadim El Chakhtoura, Sunah Song, Oteshia Hicks, Corinne Kowal, Makoto Jones, Steven Handler, Robin Jump, Vanessa Stevens
-
- Published online by Cambridge University Press:
- 16 September 2024, pp. s6-s7
-
- Article
-
- You have access Access
- Open access
- Export citation
-
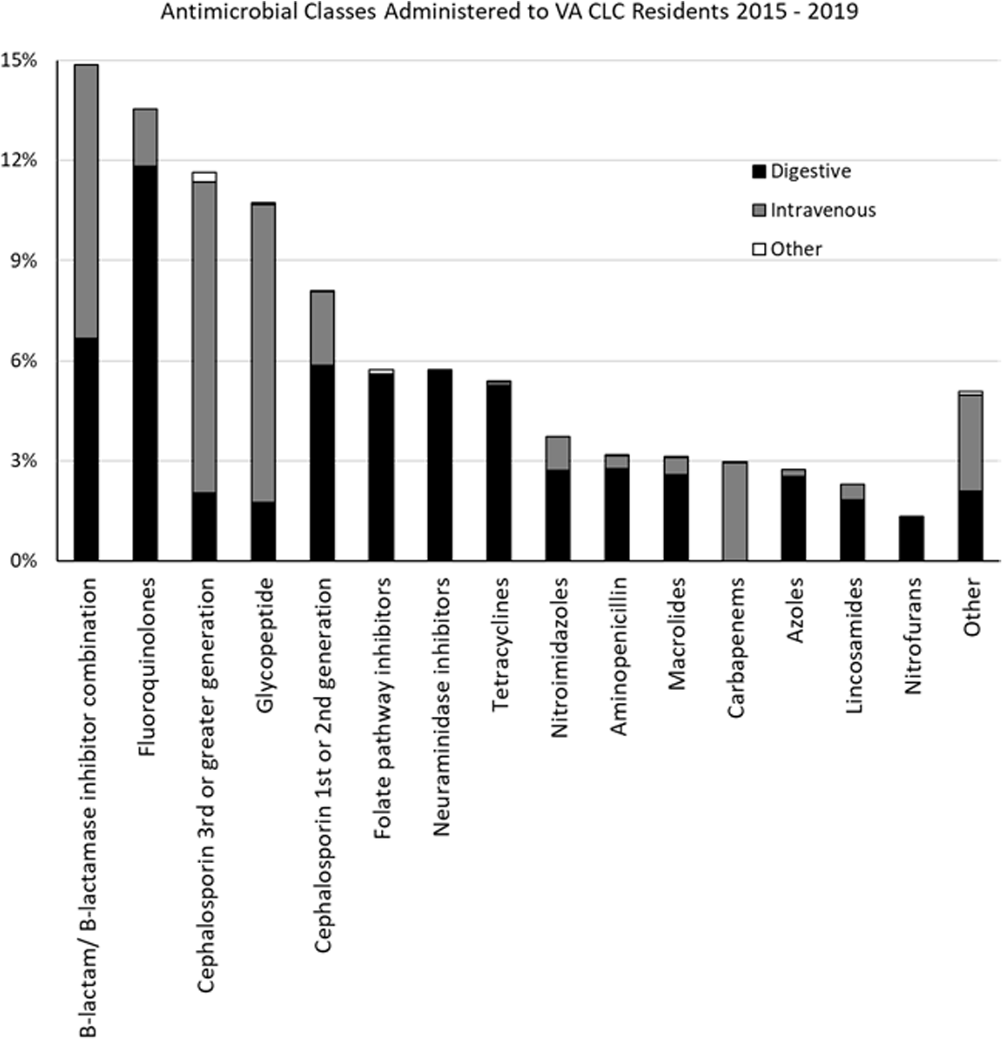
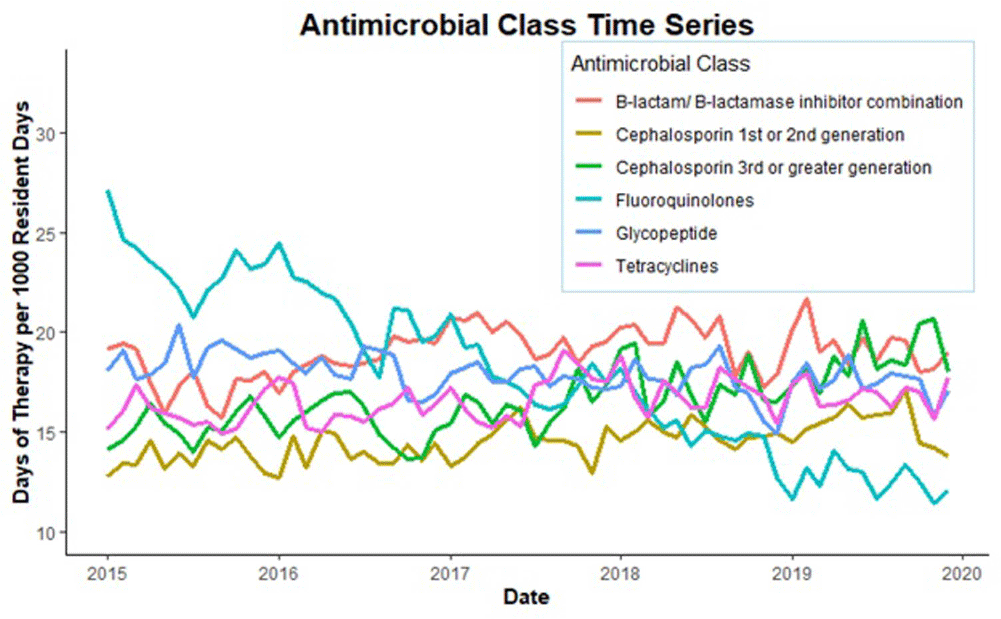
Background: Optimizing antimicrobial use (AU) among post-acute and long-term care (PALTC) residents is fundamental to reducing the morbidity and mortality associated with multidrug-resistant organism (MDROs), as well as unintended social consequences related to infection prevention. Data on AU in PALTC settings remains limited. The U.S. Department of Veteran Affairs (VA) provides PALTC to over 23,000 residents at 134 community living centers (CLCs) across the United States annually. Here, we describe AU in VA CLCs, assessing both class and length of therapy. Methods: Monthly AU between January 1, 2015 and December 31, 2019 was extracted from the VA Corporate Data Warehouse across 134 VA CLCs. Antimicrobials and administration routes were based on the National Healthcare Safety Network AU Option protocol for hospitals. Rates of AU were measured as the days of therapy (DOT) per 1,000 resident-days. An antimicrobial course was defined as the same drug and route administered to the same resident with a gap of ≤ three days between administrations. Course duration was measured in days. AU Rates were measured as the days of therapy (DOT) per 1,000 resident-days. Results: The most common class of antimicrobial course administered during the study period was beta-lactam/beta-lactamase inhibitor combinations (15%) followed by fluroquinolones (14%), extended-spectrum cephalosporins (12%) and glycopeptides (11%; Figure 1). Neuraminidase inhibitors had the longest median (IQR) course duration (10 (IQR 8) days), followed by tetracyclines (8 (IQR 8) days), and then folate pathway inhibitors, nitrofurans and 1st/2nd generation cephalosporins (7 (IQR 7) days). Overall, 60% of antimicrobial courses were administered orally, with fluroquinolones the most frequently administered orally (20%). From 2015 – 2019, the annual rate of total antimicrobial use across VA CLCs decreased slightly from 213.6 to 202.5 DOT/1,000 resident-days. During the 5-year study period, fluroquinolone use decreased from 27.47 to 13.36 DOTs/1,000 resident-days. First and 2nd generation cephalosporin use remained relatively stable, but 3rd or greater generation cephalosporin use increased from 14.70 to 19.21 DOTs/1,000 resident-days (Figure 2). Conclusion: The marked decrease in the use of fluoroquinolones at VA CLCs from 2015-2019 is similar to patterns observed for VA hospitals and for non-VA PALTC facilities. The overall use of antibacterial agents at VA CLCs decreased slightly during the study period, but other broad-spectrum agents such as 3rd or greater generation cephalosporins increased over the same period. The strategies used to decrease fluroquinolone use may have application for other antibiotic classes, both in VA and non-VA PALTC settings.
Disclosure: Robin Jump: Research support to my institution from Merck and Pfizer; Advisory boards for Pfizer
The Uncharted Patterns of Antibiotic Prescribing in Urology Ambulatory Practices: A Four-Year Analysis
- Sonal Munsiff, Kathleen Holt, Sucharu Ghosh, Ghinwa Dumyati
-
- Published online by Cambridge University Press:
- 16 September 2024, pp. s7-s8
-
- Article
-
- You have access Access
- Open access
- Export citation
-
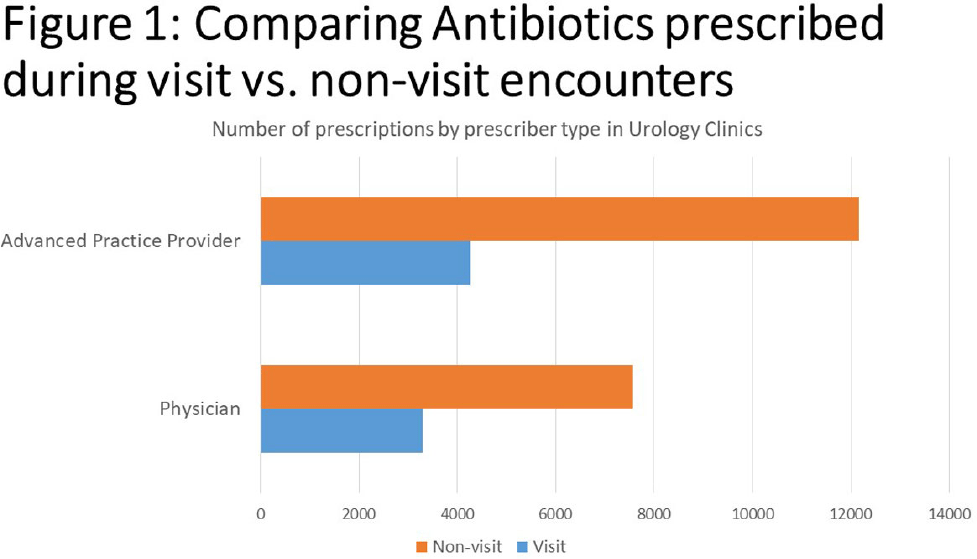
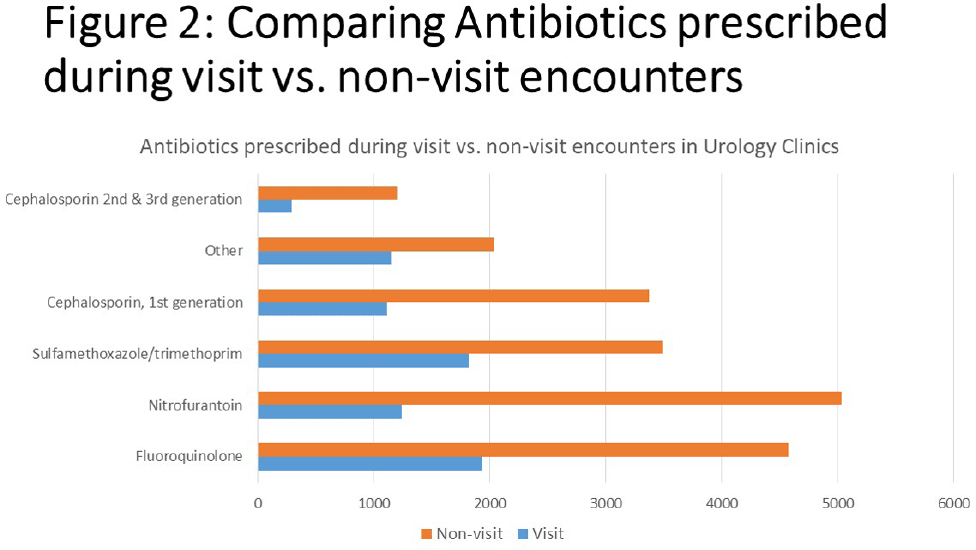
Background: Urinary tract infections (UTIs) represent a prevalent indication for outpatient antibiotic usage, yet limited data exist regarding antibiotic prescriptions within urology specialties. This study aimed to assess antibiotic prescribing patterns in urology offices over a four-year period, providing insights for potential stewardship interventions. Methods: The analysis focused on antibiotic prescribing trends in adults between 2018 and 2021 during both visit and non-visit (e.g. telephone and chart messages) encounters across 15 ambulatory Urology clinics in an academic medical center in Western New York. Exclusions were made for antivirals, antiparasitics, antifungals, oral suspensions, selected non-UTI antibiotics, duplicate orders on the same day or week, and prescriptions exceeding 28 days. Prescriptions were categorized into single doses administered in the clinic and those prescribed for 2-28 days, with descriptive statistics and trend analyses conducted using SAS v9.14. Results: Over the four-year period, 54,282 prescriptions were analyzed. Of these, 26,944 (49.7%) were single doses administered in the clinic, predominantly for pre-procedure prophylaxis. The most commonly prescribed antibiotics for prophylaxis were fluoroquinolones (FQ) (47.5%), followed by ceftriaxone (19.2%), nitrofurantoin (13.2%), trimethoprim/sulfamethoxazole (8.6%), and gentamicin (4.2%). Among the 27,288 prescriptions for 2-28 days, 72.3% were from non-visit encounters, with 61.6% prescribed by advanced practice providers (APPs) (Figure 1). The mean number of prescriptions per patient was 2.07, with women receiving more prescriptions than men (2.39 vs. 1.88, P < 0.001). FQ remained the most commonly prescribed antibiotics during all encounters (23.7%), followed by nitrofurantoin (23.0%) (Figure 2). The antibiotic duration was longer for visit-based compared to non-visit-based prescriptions (mean 10 vs. 7 days, P < 0.001). Notably, there was a significant decrease in fluoroquinolone use between Q1 2018 and Q4 2019 for both male and female patients, followed by insignificant changes thereafter. Conclusions: Antibiotic use in urology outpatient settings is substantially underestimated if only prescriptions made during visit encounters are considered. More than two-thirds of prescriptions for 2-28 days were from non-visit encounters, with the majority originating from APPs. The average therapy duration exceeded guideline recommendations. Moreover, approximately half of the antibiotics were administered in the office for pre-procedure prophylaxis. To enhance antibiotic prescribing in these specialized clinics, interventions should focus on non-visit prescriptions and provide education for APPs, alongside adjustments to default durations in electronic orders. Further evaluation is essential to assess the appropriateness of single doses for pre-procedure prophylaxis.
Evaluation of Predictors Associated with Slow Clinical Response with Extension of Outpatient Parenteral Antimicrobial Therapy
- Kristen McSweeney, Fang Yu Liu, Rachel Erdil, Majd Alsoubani, Tine Vindenes, Shira Doron, Kap Sum Foong
-
- Published online by Cambridge University Press:
- 16 September 2024, p. s8
-
- Article
-
- You have access Access
- Open access
- Export citation
-
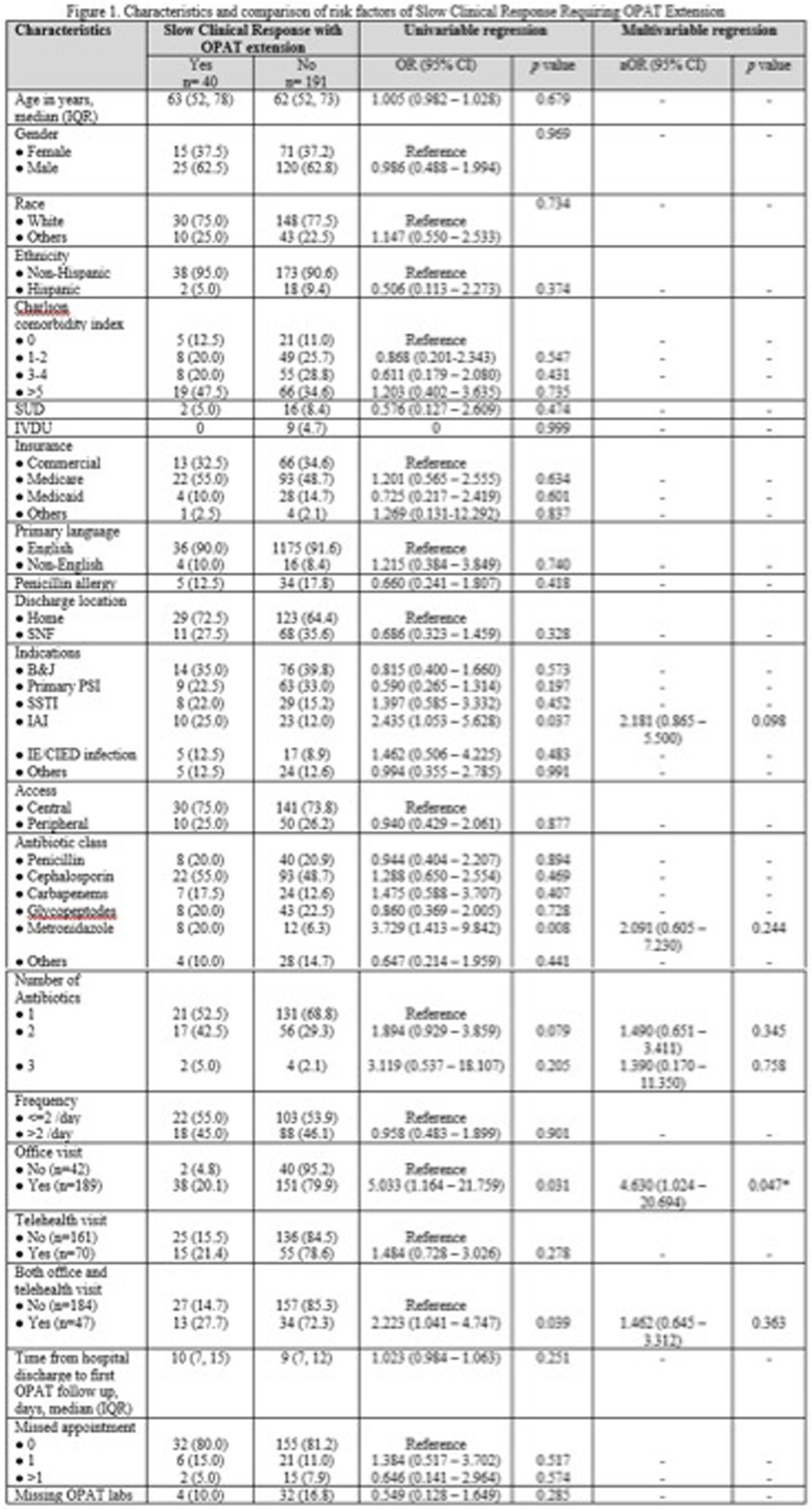
Background: Outpatient parenteral antimicrobial therapy (OPAT) provides a safe and effective alternative to prolonged hospitalization for patients with infectious diseases requiring elongated antimicrobial therapy. One study found that 35.6% of OPAT episodes met the composite definition for treatment failure, with unplanned extension of OPAT as the most common reason for treatment failure. Our study sought to identify factors predicting higher likelihood of extension of OPAT due to slow clinical response to treatment and determine how therapy extension relates to complications. Method: This retrospective cohort study included all patients aged ≥18 years discharged on OPAT between April 2022 and October 2022. Demographic, treatment, outcome, and complications data were extracted through chart review. The primary outcome was the proportion and predictors of OPAT extension due to slow clinical response to treatment. The secondary outcomes were OPAT complication rate, 30-day ED visit and 30-day readmission rates related to OPAT complications. We used univariable and multivariable logistic regression models for the primary outcome of slow clinical response requiring OPAT extension. Variables with p < 0.1 in the univariable analyses were included in the multivariable model. Result: 231 patients received OPAT during the six-month study. Among them, 40 (17.3%) patients required an extension of therapy. In univariable analysis, patients who had slow clinical response requiring extension of OPAT were more likely to have intraabdominal infection (odds ratio [OR], 2.435; 95% confidence interval[CI], 1.053–5.628), receipt of metronidazole (OR, 3.729; 95% CI, 1.413–9.842), and were more likely to be followed up through office visit (OR, 5.033; 95%CI, 1.164–21.759) or combination of office visit and telemedicine (OR, 2.223; 95%CI 1.041–4.747). Other variable comparisons are detailed in Figure 1. In the multivariable regression analysis, the independent predictor associated with extended of OPAT was follow-up via office visit (adjusted OR, 4.630; 95% CI, 1.024-20.694). Rates of complications related to intravenous access and antibiotic were similar between patients with and without extension; 15% vs. 11% (p=0.430) and 7.5% vs. 7.3% (p=1.000), respectively. There were no significant differences in 30-day ED visits and readmission rates between the 2 groups: 7.5% vs. 5.8%(p=0.715) and 12.5% vs. 7.3% (p=0.338). Conclusion: Our study highlights patient’s office visit follow-up is associated with the OPAT extension due to slow clinical response. However, extended therapy did not result in a significant increase in complications or hospital readmissions. These findings suggest the importance of careful patient selection and monitoring for OPAT, potentially guiding more efficient and targeted healthcare practices.
Implementing an Antimicrobial Stewardship Lecture Series for Family Medicine Residency Programs in South Carolina
- Kayla Antosz, Pamela Bailey, Majdi Al-Hasan, Brandon Bookstaver, Hana Winders, Sarah Battle
-
- Published online by Cambridge University Press:
- 16 September 2024, pp. s8-s9
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Family medicine physicians are one of the leading prescribers of antimicrobials in both the inpatient and ambulatory setting, however appropriate education on antimicrobial stewardship (AS) is lacking. The Antimicrobial Stewardship Collaborative of South Carolina (ASC-SC) created a family medicine AS lecture series to increase awareness of stewardship, improve antimicrobial prescribing throughout the state, and ultimately combat antimicrobial resistance. Methods: All family medicine residency programs in South Carolina (n=17) were contacted to determine interest in a four 1-hour long lecture series regarding various AS topics provided by infectious diseases physicians and pharmacists. The introductory AS lecture included topics such as interpreting minimal inhibitory concentrations, utilizing antibiograms, guidelines for diagnosing and treating common infections, and antibiotic essentials. Lectures were given on-site, and eight identical pre- and post-lecture questions were asked to assess baseline knowledge and efficacy of the introductory lecture. Not all the attendees answered all the pre- and post-lecture questions. A Chi-square analysis was used to determine statistical significance. Results: To date, 7 family medicine residency programs were given the introductory antimicrobial stewardship lecture and were included in the total analysis. Respondents included 1st year (25 of 99 responses, 25%) and 2nd year family medicine residents (17 of 99 responses 17%). When asked “How familiar are you with the concept of antimicrobial stewardship?”, 43 of 106 (41%) respondents were at least familiar or very familiar prior to the lecture compared to 81 of 93 (87%) after the lecture (p < 0.001). When asked “How confident are you in using antibiograms for antimicrobial decisions?”, 41 of 107 (38%) were confident or very confident pre-lecture and 83 of 101 (82%) post-lecture (p < 0.001). When given a case-based question on using an antibiogram to determine an appropriate empiric agent for inpatient pyelonephritis, 59 of 107 (55%) respondents were able to answer the question correctly pre-lecture compared to 85 of 99 (86%) post-lecture (p < 0.001). Among those who answered the question incorrectly, 60% selected the agent with the highest percentage susceptible rate in the antibiogram, despite it being an inappropriate agent for pyelonephritis. Conclusion: The ASC-SC lecture series was an effective tool to increase awareness and knowledge of antimicrobial stewardship to family medicine providers. This lecture series survey data helps determine what family medicine residents commonly misunderstood in AS concepts and helps guide future initiatives.
Infectious Diseases Consultation Reduces Antibiotic Duration for Uncomplicated Gram-Negative Bacteremia
- Mary Acree, Sandra Naegele, Bianca Baik, Urmila Ravichandran, Nirav Shah
-
- Published online by Cambridge University Press:
- 16 September 2024, p. s9
-
- Article
-
- You have access Access
- Open access
- Export citation
-
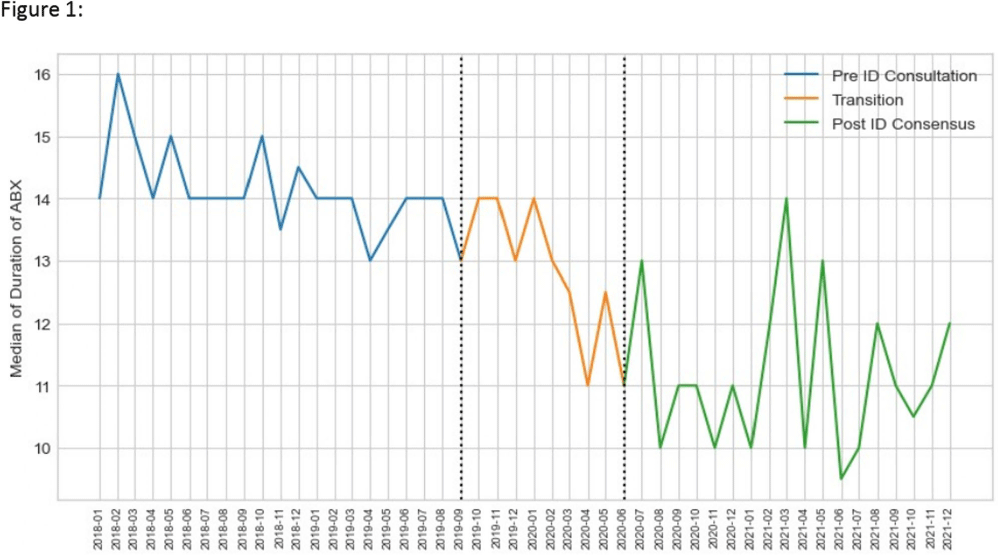
Background: Unlike Staphylococcus aureus bacteremia, the impact of ID consultation for gram negative bacteremia (GNB) has not been well studied. Recent literature has supported shorter courses of antibiotics in adults with uncomplicated GNB. We examined duration of therapy for adult patients with uncomplicated GNB over a period of time during which ID consultation for GNB was made mandatory. Method: NorthShore University HealthSystem is a 4 hospital, 828 bed hospital system located in the northern suburbs of Chicago. Data were collected retrospectively from 1/1/2018 through 12/31/2021 for patients 18 years or older hospitalized with an uncomplicated bloodstream infection due to Escherichia coli, Klebsiella species or Proteus species. This study was approved by the Institutional Review Board. All sources of infection were included. Days of effective antibiotic therapy were extracted manually by two pharmacists and an infectious diseases physician. During the study period, two major changes occurred: 1) the Physician Practice Council of NorthShore University Healthsystem voted in favor of a mandatory ID consultation for GNB and 2) the ID division developed a treatment algorithm for GNB management with an emphasis on shorter antibiotic duration in uncomplicated cases. This study was divided into three time periods: Pre-ID consultation – 1/1/2018 – 8/31/2019; Transition – 9/1/2019 – 5/31/2020 (after mandatory ID consultation, before ID division consensus achieved); Post-ID Consensus – 6/1/2020 – 12/31/21. Primary outcome was duration of antibiotic therapy. Secondary outcomes included in-hospital all-cause mortality and 30 day readmission. Continuous variables were described using median and interquartile range, and categorical data using frequency and prevalence. Kruskal-Wallis rank sum test for continuous and χ2 for categorical variables was used to verify similarity among the pre-ID consultation, transition and post-ID consensus periods. The analysis was performed using Python. Result: 1026 patients were included in the study. Pathogens included 773 E. coli (75.4%), 193 Klebsiella species (18.8%) and 60 Proteus species (5.9%). Length of stay, 30 day readmission and in-hospital mortality were not statistically significantly different when comparing pre-ID consultation and post-ID consensus time periods. Total duration of therapy was statistically significantly shorter in the post-ID consensus period (p < 0.001). Conclusion: Mandatory ID consultation and development of an ID consensus approach can shorten antibiotic duration in uncomplicated GNB. Further analysis will explore timing of transition to oral therapy and syndromic differences.

Capitalizing on Implementation Science to Advance Antimicrobial Stewardship and Health Equity in Treating Pediatric UTI’s
- Holly Maples, Jessica Snowden, Valerie Harfield, Geoff Curran
-
- Published online by Cambridge University Press:
- 16 September 2024, p. s10
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Pediatric urinary tract infections represent the most common pediatric infection with increasing gram-negative antibiotic resistance. Overutilization of antimicrobials including third generation cephalosporins are known drivers of this resistance. Antimicrobial stewardship (AS) efforts have recently shown that antibiotic selection may be influenced by patient race. Implementation science (IS) can provide frameworks and strategies to improve antimicrobial utilization and equity. Methods: This was a pre/post study of 2 geographically different children’s hospitals general pediatric floors assessing the impact of a set of implementation strategies developed to improve provider knowledge of best practice antimicrobials (based on local susceptibilities for treatment of UTI’s) and influence uptake of best practice prescribing. IS strategies included provider education, local clinical champion and opinion leader involvement, leadership involvement, local policy changes, and stakeholder co-design of decision support tools (a clinical pathway, a specific ITI antibiogram, and a dynamic order set). No education was provided regarding racial differences in prescribing habits. Outcomes were measured utilizing a portion of the RE-AIM Framework of assessing adoption of “Right” antibiotic, order set adoption, and equitable reach (racial differences in prescribing). Results: Hospital A and B had a first-generation cephalosporin prescription rate of 29.7% (n=441) and 20.6% (n-557) pre implementation and 44.6% (n=84) and 47.5% (n=118) post (p < 0 .001). Both hospitals also saw a significant reduction in third-generation cephalosporins. In Hospital A, APRN’s were more likely to prescribe a first generation cephalosporin (52.4%) than a DO (42.1%) or MD (26.4%) pre-implementation (p=0.004). In Hospital B, APRN’s were less likely to prescribe first generation cephalosporins (5.4%) than a DO (28.9%) or MD (19.4%) pre-implementation (p=0.004). No statistical significance was seen post implementation for antimicrobial selection by provider type for either hospital. Based on race, both hospitals had Black and Other patients receiving more first-generation cephalosporins while white patients were more likely to receive third-generation cephalosporins (p=0.033) pre implementation. No statistical significance was seen post implementation for antimicrobial selection based on race. No improvement was seen in order set utilization. Conclusion: With order set utilization not improving with implementation of new dynamic order set, other strategies such as education, clinical champion and opinion leader involvement, and provision of a local UTI antibiogram were likely contributors to the improvement in best antimicrobial for treatment of UTI’s. Further mixed method research is warranted to improve understanding of the relative performance of our strategies, especially the lack of provider adoption of the novel dynamic order set.
Disclosure: Jessica Snowden: Advisory board - Pfizer
C. difficile
Molecular and Epidemiological Characterization of Pediatric and Adult C. difficile Infection in Canadian Hospitals, 2015-2022
- Timothy Du, Kelly Baekyung Choi, Anada Silva, Cassandra Lybeck, George Golding, Romeo Hizon, Sean Ahmed, Blanda Chow, Ian Davis, Meghan Engbretson, Gerald Evans, Charles Frenette, Jennie Johnstone, Pamela Kibsey, Kevin Katz, Joanne Langley, Jenine Leal, Bonita Lee, Yves Longtin, Dominik Mertz, Jessica Minion, Michelle Science, Jocelyn Srigley, Kathryn Suh, Reena Titoria, Nisha Thampi, Alice Wong, Jeannette Comeau, Susy Hota
-
- Published online by Cambridge University Press:
- 16 September 2024, pp. s10-s11
-
- Article
-
- You have access Access
- Open access
- Export citation
-
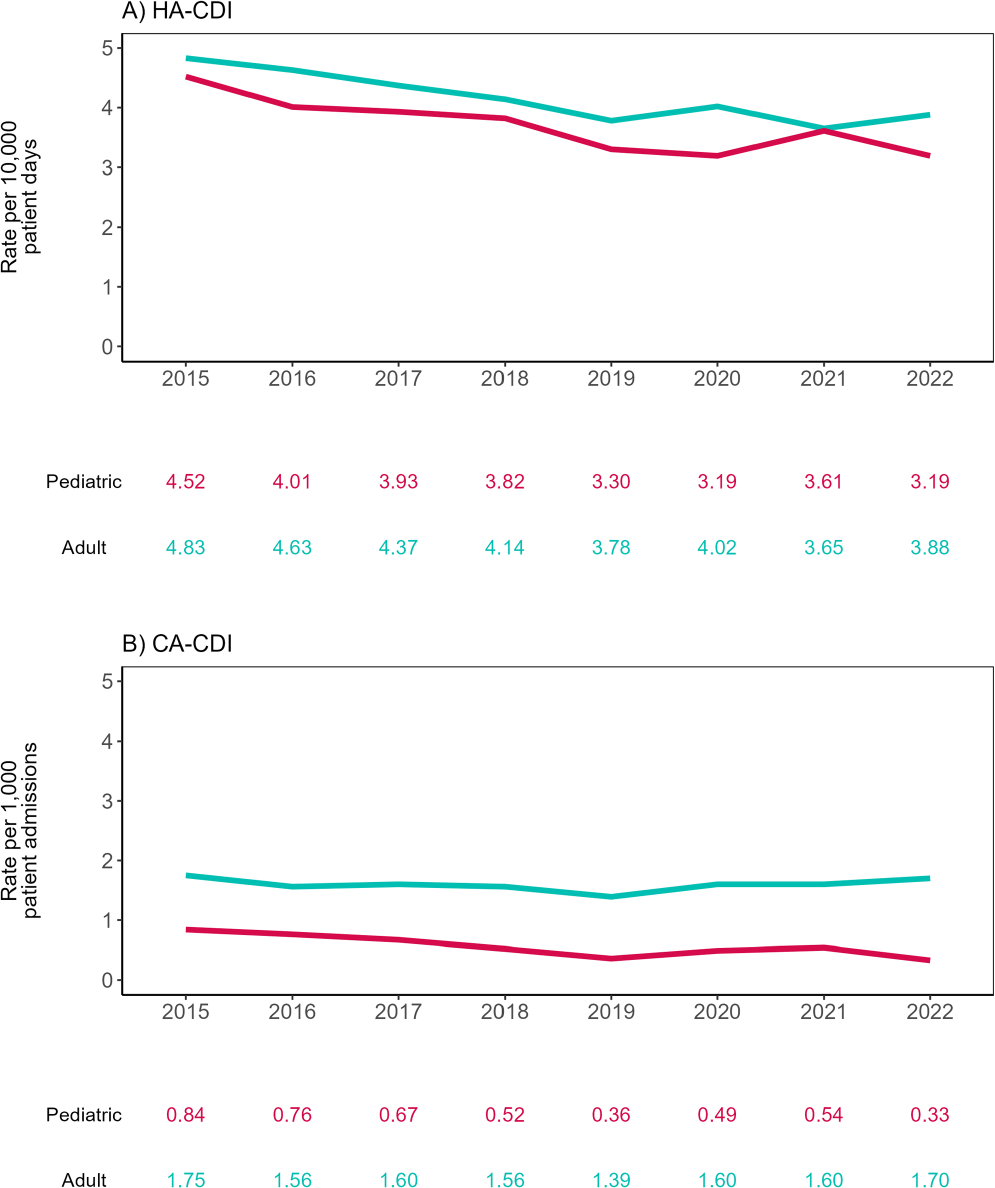
Background: The molecular and epidemiological landscape of C. difficile infection (CDI) has evolved markedly in the last decade; however, limited information is available contrasting differences between adult and pediatric populations. We describe a multicenter study evaluating healthcare-associated (HA) and community-associated (CA) adult and pediatric-CDI identified in the Canadian Nosocomial Infection Surveillance Program (CNISP) network from 2015 to 2022. Methods: Hospitalized patients with CDI were identified from up to 84 hospitals between 2015–2022 using standardized case definitions. Cases were confirmed by PCR, cultured, and further characterized using ribotyping and E-test. We used two-tailed tests for significance (p≤0.05). Results: Of 30,817 cases reported, 29,245 were adult cases [HA-CDI (73.2%), CA-CDI (26.8%)] and 1,572 were pediatric cases [HA-CDI (77.7%), CA-CDI (22.3%)]. From 2015 to 2022, HA-CDI rates decreased 19.7% (p=0.007) and 29.4% (p=0.004) in adult and pediatric populations, respectively (Figure 1). CA-CDI rates remained relatively stable in the adult population (p=0.797), while decreasing 60.7% in the pediatric population (p=0.013). Median ages of adult and pediatric patients were 70 (interquartile range (IQR), 58–80) and seven (IQR, 3–13) years, respectively. Thirty-day all-cause mortality was significantly higher among adult vs. Pediatric CDI patients (11.0% vs 1.4%, p < 0.0001). No significant differences in other severe outcomes were found. Ribotyping and susceptibility data were available for 4,620 samples: 3,558 adult (77.0%) and 1,062 pediatric (23.0%). The predominant adult and pediatric ribotypes (RT) were 106 (12.2/16.2%), 027 (11.4/3.2%), and 014 (8.8/8.2%). Overall, RT027 prevalence significantly decreased from 17.9% in 2015 to 3.2% in 2022 (p=0.003), while RT106 increased from 8.5% to 14.4%. Resistance rates among adult and pediatric isolates were similar for all antimicrobials tested except moxifloxacin (16.2% vs. 6.2%, p < 0.0001, respectively). Adult moxifloxacin resistance decreased from 30% to 6.3% from 2015 to 2022 (p=0.006). Adults with moxifloxacin-resistant CDI were older (median: 74 vs. 69 years, p < 0.001) and had higher thirty-day all-cause mortality (13% vs. 9.8%, p=0.041) and recurrence (10% vs. 5.7%, p < 0.001) compared to those with moxifloxacin non-resistant CDI, while these trends were not observed in pediatric patients. Among RT027 strains, moxifloxacin resistance decreased from 91.0% in 2015 to 7.1% in 2022. There was one metronidazole-resistant pediatric sample in 2018 and no resistance to vancomycin or tigecycline in either population. Conclusion: We have found differences in the epidemiological and molecular characteristics of adult and pediatric CDI, with higher thirty-day all-cause mortality among adults. Overall, RT106 has replaced RT027 as the predominant ribotype with a concomitant decrease in fluoroquinolone resistance.
CLABSI
Impact of Vascular Access Teams on Central Line Associated Bloodstream Infections
- Shelley Kester, Katie Passaretti, Mindy Sampson, Anupama Neelakanta, Robert Rose, David Tincopa, Johnna Parsons, Audrey Weaver, Abby Avery, Barbi Mills, Candice Dickerson
-
- Published online by Cambridge University Press:
- 16 September 2024, p. s11
-
- Article
-
- You have access Access
- Open access
- Export citation
-
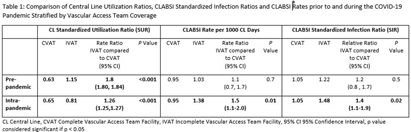
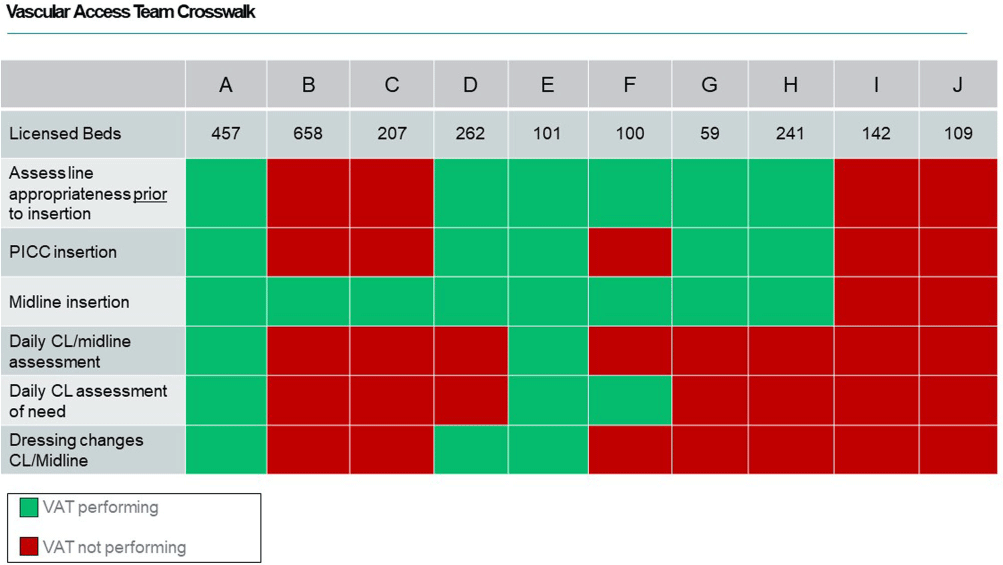
Background: During the COVID-19 pandemic, rates of central line bloodstream infections (CLABSI) increased nationally. Studies pre-pandemic showed improved CLABSI rates with implementation of a standardized vascular access team (VAT).[PL1] [PL2] [mi3] Varying VAT resources and coverage existed in our 10 acute care facilities (ACF) prior to and during the pandemic. VAT scope also varied in 1) process for line selection during initial placement, 2) ability to place a peripherally inserted central catheter (PICC), midline or ultrasound-guided peripheral IV in patients with difficult vascular access, 3) ownership of daily assessment of central line (CL) necessity, and 4) routine CL dressing changes. We aimed to define and implement the ideal VAT structure and evaluate the impact on CLABSI standardized infection ratios (SIR) and rates prior to and during the pandemic. Methods: A multidisciplinary workgroup including representatives from nursing, infection prevention, and vascular access was formed to understand the current state of VAT responsibilities across all ACFs. The group identified key responsibilities a VAT should conduct to aid in CLABSI prevention. Complete VAT coverage[mi4] was defined as the ability to conduct the identified responsibilities daily. We compared the SIR and CLABSI rates between hospitals who had complete VAT (CVAT) coverage to hospitals with incomplete VAT (IVAT) coverage. Given this work occurred during the pandemic, we further stratified our analysis based on a time frame prior to the pandemic (1/2015 – 12/2019) and intra-pandemic (1/2020 - 12/2022). Results: The multidisciplinary team identified 6 key components of complete VAT coverage: Assessment for appropriate line selection prior to insertion, ability to insert PICC and midlines, daily CL and midline care and maintenance assessments, daily assessment of necessity for CL, and weekly dressing changes for CL and midlines[NA5] . A cross walk of VAT scope (Figure 1) was performed in October 2022 which revealed two facilities (A and E) which met CVAT criteria. Pre-pandemic, while IVAT CLABSI rates and SIR were higher than in CVAT units, the difference was not statistically significant. During the pandemic, however, CLABSI rates and SIR were 40-50% higher in IVAT compared to CVAT facilities (Incident Rate Ratio 1.5, 95% CI 1.1-2.0 and SIR Relative Ratio 1.4, 95% CI1.1-1.9 respectively) (Table 1). Conclusions: CLABSI rates were lower in facilities with complete VAT coverage prior to and during the COVID-19 pandemic suggesting a highly functioning VAT can aid in preventing CLABSIs, especially when a healthcare system is stressed and resources are limited.
COVID-19
The Impact of COVID-19 on Healthcare-Associated Infections: A Survey of Acute Care Hospitals
- Monika Pogorzelska-Maziarz, Julia Kay, Tara Schmidt, Anika Patel, Pamela De Cordova
-
- Published online by Cambridge University Press:
- 16 September 2024, pp. s11-s12
-
- Article
-
- You have access Access
- Open access
- Export citation
-
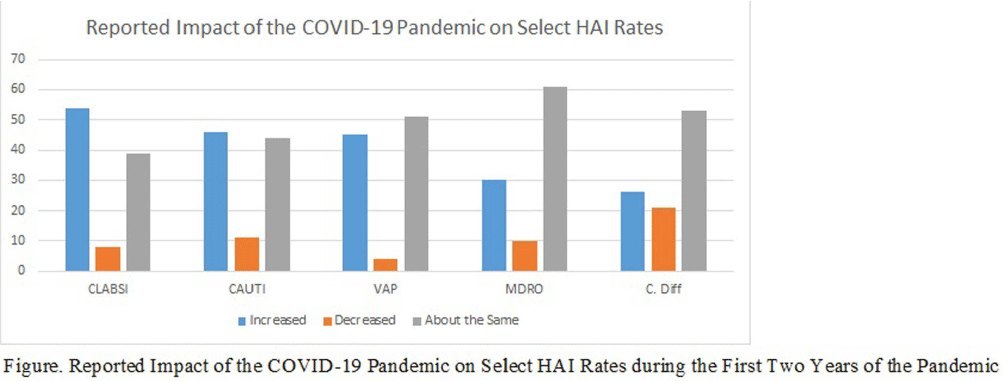
Background: The COVID-19 pandemic has placed an enormous strain on the healthcare system, including infection prevention and control. The response to the COVID-19 pandemic required extraordinary resources, which were often diverted from routine infection prevention and control activities and may have contributed to increased rates of HAI in the acute care setting. However, the impact of the COVID-19 pandemic on infection prevention and control departments, including staffing and resources, and on routine infection prevention and control activities is not well-described. The objective of this study was to describe the impact of the COVID-19 pandemic on IPC departments and department response to the pandemic. Methods: Between August and December of 2023, we conducted an electronic survey of all acute care facilities participating in the National Healthcare Safety Network. Survey data were analyzed using descriptive statistics. Results: Over 594 infection control departments participated in the survey, representing 1,400 NHSN facilities (20% response rate based on number of eligible NHSN facilities). Half of the respondents reported that their hospital experienced increases in the following HAI rates during the first two years of the pandemic: central-line associated bloodstream infections (54%), catheter-associated urinary tract infections (46%) and ventilator associated pneumonia (45%). When asked to identify the top three contributors to increased HAI rates in their facility, respondents cited the following factors: staffing shortages (70%), patient acuity (69%), use of travel nurses (48%), increased device utilization (37%), and reduced bedside acuity (31%). Respondents reported that their department utilized the following actions to decrease these HAI rates: increased rounding and monitoring of IPC procedures (81%), reeducation of frontline staff on IPC policies and procedures (77%), environmental care rounds (69%), monitoring of isolation compliance (66%), HAI Task Force/Committee (57%), nurse-driven catheter removal protocols (53%), and insertion prevention protocols (53%). When asked if the department experienced applied pressure or attempts to influence HAI reporting due to the increase in HAI rates in the facility experienced in the wake of the pandemic, 19% of respondents reported increased pressure from management/C-suite and 7% reported increased pressure from providers. Conclusion: The COVID-19 pandemic had a substantial impact on IPC departments in acute care hospitals and had a profound effect on IPC staffing, resources and routine IPC activities. Future work needs to identify best practices and lessons learned from the pandemic to inform future pandemic preparedness.
Decolonization Strategies
Temporal decreases in pathogen colonization and infection among hospitalized neonates following routine skin antisepsis with chlorhexidine gluconate: Botswana 2022 – 2023
- Chimwemwe Tembo, Jonathan Strysko, Boingotlo Gopolang, Tshiamo Zankere, Teresia Gatonye, Tlhalefo Dudu Ntereke, Kgomotso Kgomanyane, Janet Thubuka, Britt Nakstad, Susan Coffin, Carolyn McGann, Corrado Cancedda, Ebbing Lautenbach, Naledi Betsi Mannathoko, Melissa Richard-Greenblatt, David Goldfarb, Ashley Styczynski, Gemma Parra, Rachel Smith, Kagiso Mochankana, Neo Mogotsi, Tapoloso Keatholetswe
-
- Published online by Cambridge University Press:
- 16 September 2024, p. s12
-
- Article
-
- You have access Access
- Open access
- Export citation
-
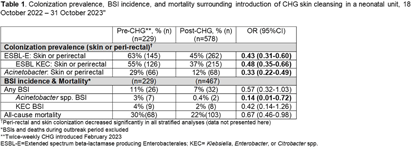
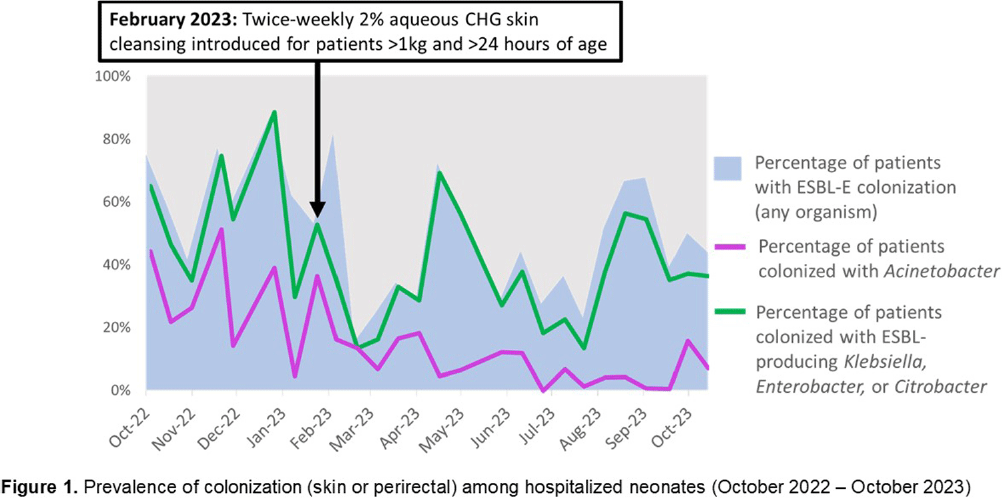
Background: Multidrug-resistant Gram-negative bacteria are a major cause of sepsis among hospitalized neonates globally. Aqueous chlorhexidine gluconate (CHG) skin antisepsis has been shown to be safe for use in infants; however, its sustained effectiveness in preventing Gram-negative pathogen colonization, bloodstream infection (BSI), and mortality is unclear. Methods: We conducted a period prevalence survey, with 26 sampling events over 12 months (18 October 2022 – 31 October 2023) at a 33-bed neonatal unit in a tertiary public hospital in Botswana where ESBL-producing Klebsiella pneumoniae and carbapenem-resistant Acinetobacter baumannii are leading causes of BSI. Perirectal and periumbilical skin swabs were collected every two weeks from all inpatients. Swabs were inoculated onto chromogenic media selective and differential for extended-spectrum beta-lactamase producing Enterobacterales (ESBL-E) and Acinetobacter spp. (CHROMagar™ ESBL, Acinetobacter). Colonization status was determined based on culture growth and colony morphology. Contemporaneous data on all-cause mortality and BSI were abstracted from routine surveillance records. Pre- and post-CHG prevalences were compared using a simple Chi-square test. During the surveillance period, an outbreak of K. pneumoniae linked to contaminated multi-use vials was detected, thus BSIs and deaths during the outbreak period (2 February–6 April, 2023) were excluded. In February 2023, the hospital infection prevention and control (IPC) team introduced twice-weekly whole-body cleansing with commercially available 2% aqueous CHG, performed by caregivers and healthcare workers on neonates >24 hours old and weighing ≥1 kg until discharge. Results: There were significant decreases in ESBL-E and Acinetobacter skin and perirectal colonization following the CHG intervention (Table 1; Figure 1). After the CHG intervention, the incidence of Acinetobacter BSIs declined significantly and there was a trend toward a decline in other BSIs and mortality. No adverse events associated with CHG were reported. Conclusions: Twice-weekly CHG application was temporally associated with significant reductions in neonatal ESBL-E and Actinetobacter skin and perirectal colonization and Acinetobacter BSI. This analysis was limited by a short pre-intervention surveillance period and thus may have been influenced by confounders such as seasonality, and intensified IPC efforts following the outbreak. Analysis of the routine CHG use in other settings and over longer surveillance periods are needed to better understand its effectiveness as an IPC strategy in settings where neonatal sepsis incidence is high. Table 1. Colonization prevalence, BSI incidence, and mortality surrounding introduction of CHG skin cleansing in a neonatal unit, 18 October 2022 – 31 October 2023.
Dialysis
Candida auris Response in a Tennessee Dialysis Facility, 2023
- Alex Kurutz, Joshua Key, Autumn Edwards, Simone Godwin
-
- Published online by Cambridge University Press:
- 16 September 2024, p. s13
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Candida auris, a multi-drug resistant fungal pathogen, was introduced to Tennessee in 2021. There are limited studies on the spread of C. auris in highly specialized care settings including outpatient dialysis facilities. Facilities are concerned that C. auris transmission is difficult to prevent in this setting due to patient vulnerability, treatment frequency and length, and isolation challenges. As a result, these facilities may reject patients based on their positive colonization status. In 2023, the Tennessee Department of Health (TDH) conducted two containment-driven colonization screenings in response to a colonized patient receiving dialysis treatment for one month without their status being known to the facility. Methods: An initial point prevalence survey (PPS) was conducted to assess for ongoing transmission among dialysis patients. Patient screening was prioritized for the cohort of patients who received dialysis at the same time as the index patient (Cohort A). The screening was broadened to include patients dialyzed directly before Cohort A (Cohort B) by request of the Cohort B patients. A second PPS was conducted 7 weeks later, targeting the same cohorts. Specimens were collected through supervised patient self-collection of a skin swab from the axilla and groin. Flocked Eswabs were used for collection and transferred in Amies transport media to the Tennessee State Public Health Lab. The presence of C. auris was detected via Polymerase Chain Reaction (PCR). Results: Twenty-three patients (12 from Cohort A; 11 from Cohort B) were screened in the first PPS. One patient from Cohort A tested positive. This colonized patient was determined to be a known C. auris case first detected four months prior, but the patient’s status was never communicated to the dialysis facility from the discharging acute care facility. Eleven patients, excluding the previously identified positives, participated (9 from Cohort A; 2 from Cohort B) in the second PPS; no positives were identified. Discussion: The index patient and an additional patient identified by the PPS both received dialysis at this facility for up to 4 months without facility knowledge. These results suggest that the standard infection control practices at this dialysis facility were adequate to prevent the transmission of C. auris among dialysis patients on multiple shifts. Additionally, patient self-collection identified a known C. auris patient. Future TDH work includes further evaluating the risk of C. auris transmission and developing targeted infection prevention and control practices for the outpatient dialysis setting.
Infection Prevention in Low and Middle-Income Countries
Rapid Scale-Up of Screening for Early Detection of Sudan Virus Disease (SVD) in Healthcare Facilities (HCFs) during the 2022 Outbreak in Uganda
- Shillah Nakato, Judith Nanyondo, Martin Esagala, Maureen Kesande, Andrew Kwiringira, Ahumuza Noelyn Komugisha, Morris Aheebwa, Abdullah Wailagala, Elizabeth Katwesigye, Juliet Kasule, Isabella Fabens, Janelle Kibler, Elizabeth Bancroft, Doreen Nabawanuka, Paul Katongole, Mohammed Lamorde
-
- Published online by Cambridge University Press:
- 16 September 2024, p. s13
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: The Uganda Ministry of Health (MoH) and implementing partners instituted an infection prevention and control (IPC) response strategy during the Uganda SVD outbreak in 2022 that involved rapid enhancement of screening capacity at HCFs. Rapid scale-up of screening for infectious diseases, such as SVD, is critical for early identification and triage of suspected or confirmed cases in HCFs. We describe the rapid deployment of a multimodal IPC strategy implemented in response to the SVD outbreak and the resulting impact on screening measures at HCFs. Methods: We implemented a multimodal IPC strategy in HCFs from five high risk districts to improve screening practices from November 2022–January 2023. The strategy included training health workers (HCWs) identified as IPC mentors; establishing screening areas; and providing screening supplies and communication materials. The three-day training utilized an MoH standardized training package with didactic and practice sessions. The mentors then cascaded screening information and skills to other HCWs through onsite trainings and mentorships and established screening areas. Baseline and endline (3 months after baseline) cross-sectional assessments were conducted using the MoH IPC Assessment Tool adapted from the WHO Ebola IPC Scorecard. The five main screening parameters assessed included presence of ≥ 1 meter distance between screener and the person screened, availability of a functional handwashing facility and infrared thermometer, correct record of each person’s temperature, and appropriate referral process for those suspected of having SVD to holding areas. IPC capacity was measured through the summation of each of these parameter results and calculated as an overall percentage. IBM SPSS Statistics 20 software was used for data analysis and a paired t-test done to determine any significant findings between mean scores (percentage) at baseline and endpoint. Results: A total of 296 IPC mentors were trained, screening information was cascaded to 3,899 HCWs, and screening areas were established in 1,135 HCFs. Based on the screening results from the MoH IPC assessment tool, capacity improved from 44% (SD=37) at baseline to 67% (SD=34) at endpoint. Screening capacity improved from baseline to endpoint among level II and public HCFs from 33% (SD=35) to 60% (SD=35) (p < 0 .05) and from 54% (SD=38) to 76% (SD=31) (p < 0 .05), respectively. Conclusion: Rapid implementation of a multimodal IPC strategy was successful in enhancing screening capacity across Uganda’s HCFs during a SVD response, which is critical for early identification of infected patients to interrupt transmission. This multimodal approach should be recommended for future response actions.
Medical Informatics
Natural Language Processing (NLP) Accurately Identifies LTCF Exposure from Clinical Notes: A Proof-of-Principle Study
- Katherine Goodman, Philip Resnik, Monica Taneja, Laurence Magder, Mark Sutherland, Scott Sorongon, Eili Klein, Pranita Tamma, Anthony Harris
-
- Published online by Cambridge University Press:
- 16 September 2024, pp. s13-s14
-
- Article
-
- You have access Access
- Open access
- Export citation
-
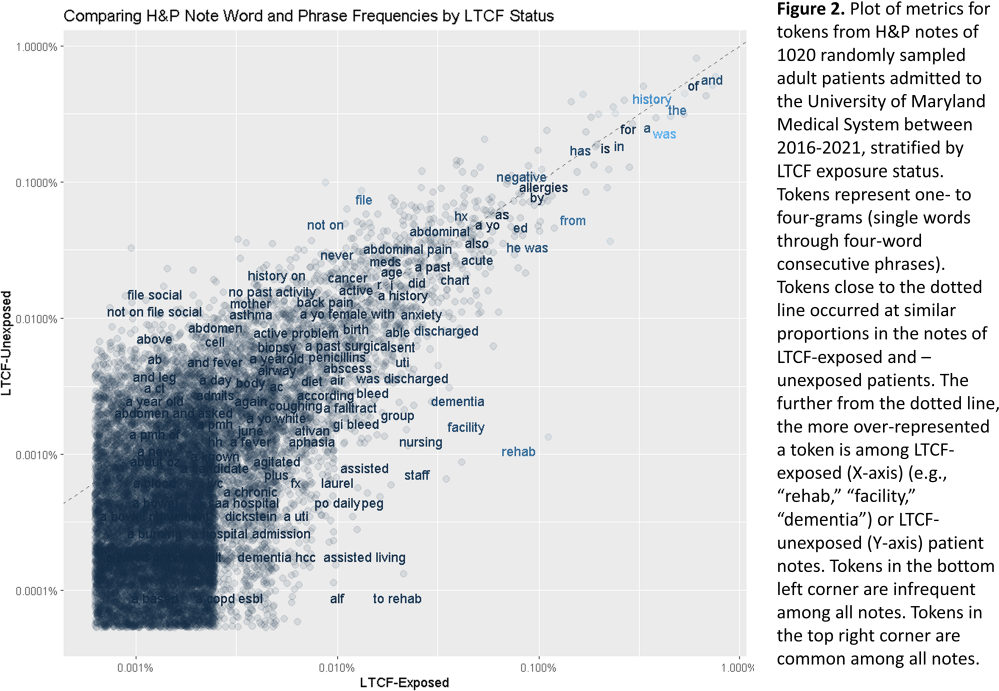
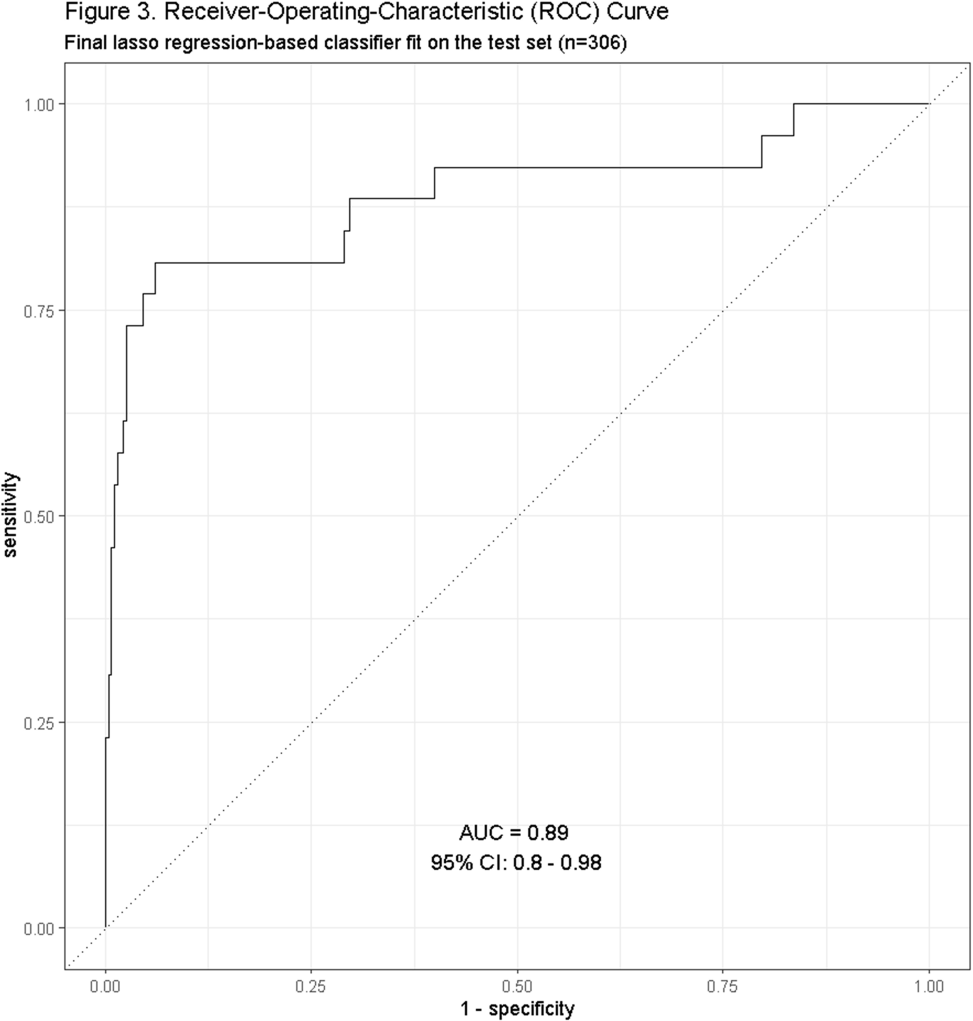
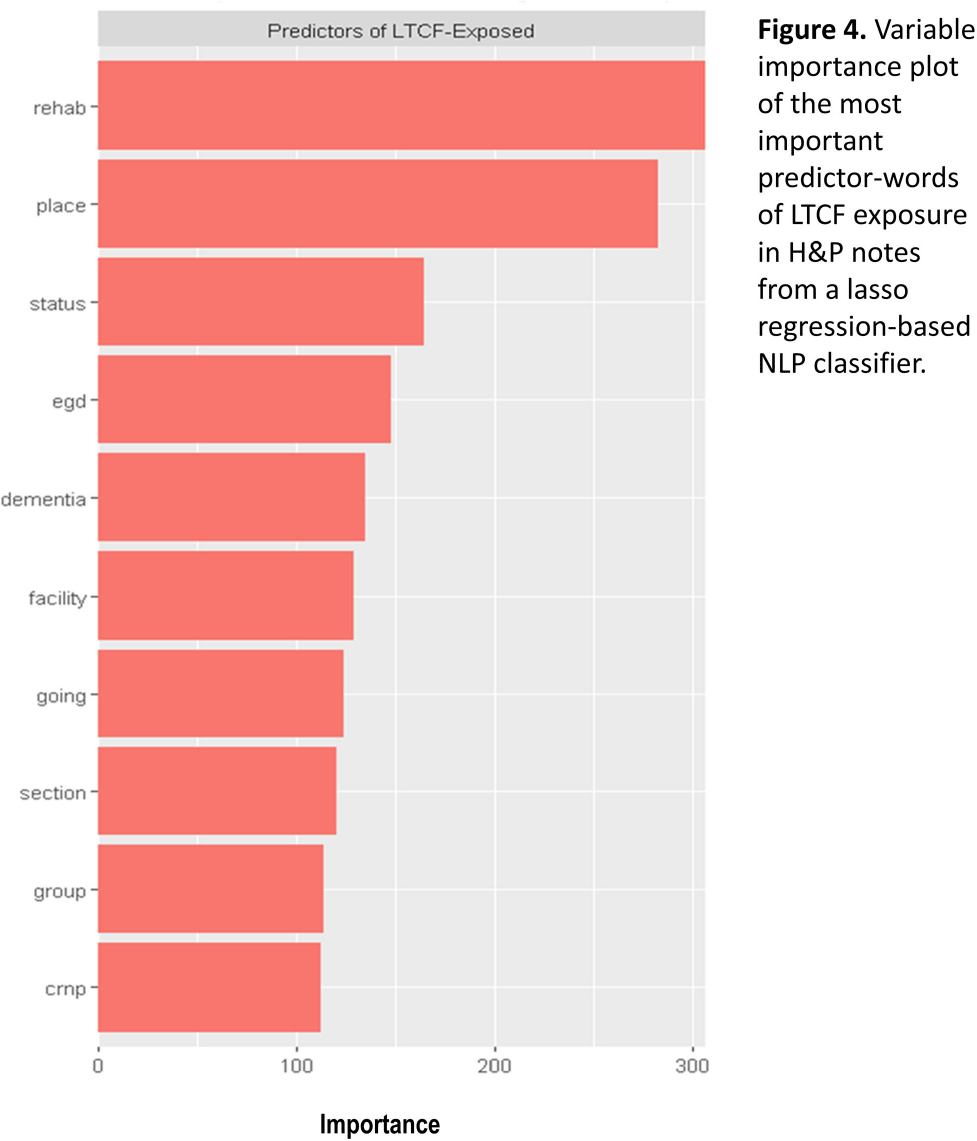
Background: Residence or recent stay in a long-term care facility (LTCF) is one of the most important risk factors for multidrug-resistant organism (MDRO) carriage and infection, making reliable identification of LTCF-exposed inpatients a critical priority for infection control day-to-day practice and research. However, because most hospital electronic health records (EHRs) do not include a dedicated field for documenting LTCF exposure, absent manual review of patient charts, identifying LTCF-exposed inpatients is challenging. We aimed to develop an automated, natural language processing (NLP)-based classifier for identifying LTCF exposure from clinical notes. Methods: We randomly sampled 1020 adult admissions from 2016-2021 across the 12-hospital University of Maryland Medical System and manually reviewed each admission’s history & physical (H&P) note for mention of LTCF exposure (Figure 1). After H&P pre-processing, we calculated feature representations for documents based on term frequencies and visually explored between-group (LTCF-exposed vs. LTCF-unexposed) feature differences. To predict LTCF status from the H&P notes, we trained and tuned a LASSO regression-based classifier on 70% of the data with 3-fold cross-validation and 1:1 up-sampling to address class imbalance. The final classifier was evaluated on the 30% held-out sample (not up-sampled), with calculation of the C-statistic (area-under-the-curve, AUC) with bootstrapped 95% confidence intervals, and construction of receiver-operating-characteristic and variable importance plots (R Version 4.3.2). Results: 7% (n=76 cases) of H&P notes documented LTCF exposure. In our visual analysis, the H&P words and phrases that were over-represented among LTCF patients had high face validity (Figure 2). The final LASSO-regression-based classifier achieved a C-statistic of 0.89 (95% CI: 0.80–0.98) on the held-out data for identifying LTCF exposure from the H&P notes (Figure 3). The most important model predictors (i.e., words) for distinguishing LTCF-exposed from LTCF-unexposed patients are reflected in Figure 4. The most important predictor-words of LTCF-exposure were “rehab,” “place,” “status,” “egd,” and “dementia.” Conclusion: In this multi-center study, even a simple NLP classifier demonstrated very strong discrimination for identifying LTCF exposure status from H&P notes, which could substantially reduce the manual review time required to identify LTCF-exposed inpatients. If automated in the electronic health record, it could also inform real-time MDRO screening decisions. Future research is planned to build more sophisticated classifiers using machine learning best practices, to build classifiers for additional MDRO risk factors, and to externally validate NLP classifiers on notes from an external healthcare system.

Molecular Epidemiology
Large-Scale S. aureus Screening with Molecular Epidemiology; the Role of MSSA and Community MRSA in Hospital Transmissions
- Courtney Takats, Gregory Putzel, Drew Siskin, Alejandro Pironti, Bo Shopsin, Sarah Hochman
-
- Published online by Cambridge University Press:
- 16 September 2024, p. s15
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: The frequency of Staphylococcus aureus transmission in hospitals is unknown: symptomatic infection may occur months after transmission and colonization, and infection prevention efforts rely on indirect measurements, rather than direct detection of transmission events. We implemented a hospital-based S. aureus screening program, combined with whole genome sequencing of S. aureus surveillance and clinical cultures and data extracted from the electronic health record, to identify S. aureus clonal complex-, patient- and location-specific factors associated with S. aureus transmission in our health system. Methods: Screening S. aureus cultures were obtained at admission by nasal swab for adults admitted to Medicine, Transplant, Oncology and intensive care, and weekly by swab of nares, axilla and groin for children admitted to intensive care and Oncology at NYU Langone Health in New York City. All methicillin-resistant S. aureus (MRSA) from screening and clinical (blood, wound, sputum) cultures and all methicillin-susceptible S. aureus (MSSA) from screening and blood cultures underwent whole genome sequencing. Isolates from distinct patients with < 2 0 single nucleotide pair differences were considered genetically related. Electronic health data was extracted for descriptive statistics and for spatiotemporal plots to assess plausible transmissions. We used REDCap electronic data capture tools hosted at NYU Grossman School of Medicine and SAS software for data analysis to evaluate S. aureus transmissions between November 2022 and November 2023. Results: We analyzed 8,567 S. aureus isolates: including 6,552 screening cultures, 1,008 blood cultures, and 1,007 clinical cultures. We found 424 plausible S. aureus hospital transmissions using sequencing and electronic health data. Screening cultures identified 75% of transmissions that would have otherwise been missed with blood and clinical cultures alone. The majority of positive screening cultures isolated MSSA, but the proportion of transmissions due to MSSA differed by age. In children, MSSA colonization accounted for 62% of transmissions. In adults, only 15% of transmissions were due to MSSA colonization, whereas MRSA colonization accounted for 56% of transmissions. Analysis of adult MRSA isolates by clonal complex found that 45% of transmissions were due to CC8, higher than the 17% among isolates agnostic of transmissions. Emergency departments and the neonatal intensive care unit had the highest number of transmissions. Patients involved in transmissions had longer lengths of stay and frequent hospitalizations. Conclusions: A S. aureus screening program, coupled with genome sequencing and electronic health data, can identify patient group, hospital locations and clonal complexes that are at high risk for S. aureus transmissions.


























