Delusional phenomena, so clearly described in psychiatric textbooks, are rarely unambiguous in practice. The textbook characteristics of incorrigibility, demonstrable falseness and cultural incongruity are rarely clear-cut in real life, and normal beliefs pass into a continuum of delusion-like experiences, overvalued ideas, preoccupations, obsessions, partial delusions and delusions proper, which can exist at varying levels of conviction and bizarreness. Nowhere is this complexity more apparent than in the diagnostic category of delusional disorders, resurrected from Kraepelin's ‘paranoia’ in DSM-III-R and continuing largely unchanged into DSM-IV (American Psychiatric Association 1987, 1994) and, reportedly, DSM-5 (www.dsm5.org).
Boundaries of a syndrome
Many psychiatrists will rarely encounter a patient with true delusional disorder. It is a secretive condition and most people with it manage to avoid coming to the attention of services. Although this suggests a degree of insight or mindfulness, those who do present have often come into conflict with those around them on the basis of their incorrigible beliefs. The rarity of such patients in clinic practice is often compensated for by the strangeness of their circumstances, making them common as subjects for case presentations and curiosities in journals.
Delusional disorders are difficult and unrewarding to study. Individuals are reluctant to cooperate with treatment, often fail to take medication and can be frustratingly garrulous during therapy sessions. They offer endless evidence to support their beliefs while creating ever more elaborate ways of refuting evidence against them through appeals to coincidence, misunderstanding or alternative interpretations of the ‘facts’. As a result, and despite limited research evidence, individuals with the disorder have continued to be classified on the basis of delusional content, derived from the many early eponymous ‘syndromes’ (see Reference Enoch and TrethowanEnoch 1991), and are placed within schizophrenia spectrum disorders.
Both DSM-IV and ICD-10 (World Health Organization 1992) agree on the essential characteristics of delusional disorder: the presence of persistent delusions, independent of any transient mood disorder and not fitting criteria for schizophrenia. There are, however, notable differences between ICD and DSM criteria: DSM requires 1 month of stable delusions, whereas ICD requires 3 months; ICD will allow transitory hallucinations in any modality (including auditory but not ‘third person’ or ‘running commentary’), whereas DSM will allow only tactile and olfactory hallucinations. In the proposals for DSM-5 these are unchanged, although the confusing subjectivity in deciding whether the behaviour is ‘non-bizarre’ has been removed. The only significant change proposed in DSM-5 is to distance delusional disorders further from a promising line of evidence that may link them to obsessive spectrum disorders such as body dysmorphic disorder by specifying that delusional disorder cannot be diagnosed if ‘the disturbance is not better accounted for by another mental disorder such as body dysmorphic disorder or obsessive compulsive disorder’ (DSM-5 Task Force 2011).
In fact, unlike the other disorders in the schizophrenia spectrum, delusional disorders are not associated with symptoms of thought alienation, passivity and negativity. Patients with these symptoms cannot, by definition, be diagnosed with delusional disorder. The limited work on the diagnostic relationships of delusional disorder include a study of monozygotic/dizygotic concordance rates for schizophrenia spectrum disorders, which found that delusional disorder is unlikely to be related to them (Reference Farmer, McGuffin and GottesmanFarmer 1987). This is supported by more recent genetic research evidence, which suggests that delusional disorder has no relation to the dopamine D1 receptor gene (Reference Debnath, Das and BeraDebnath 2010). There is a school of thought that considers delusional disorder to relate more naturally to a currently disparate group of disorders that contain both obsessional and delusional components (Reference Fear, Sharp and HealyFear 2000; Reference O'Dwyer and MarksO'Dwyer 2000; see also Reference HollanderHollander (1993) and Reference Hollander, Zohar and SirovatkaHollander et al (2011) for detailed commentary).
Constitutional vulnerabilities
Kraepelin distinguished between dementia praecox (later renamed schizophrenia) and paranoia (later called delusional disorder) on the basis that the former comprised incoherent delusions in a disintegrating personality, whereas in the latter the personality was intact and the delusions coherent. Reference JaspersJaspers (1923/1946) subsequently made a distinction between the true delusions of schizophrenia, ‘which go back to primary pathological experiences as their source, and which demand for their explanation a change in the personality’ (p. 106), and the term delusion-like experiences which is ‘reserved by us for those so-called “delusions” that emerge comprehensibly from other psychic events and can be traced back psychologically to certain affects, drives, desires and fears’ (pp. 106–107). Sérieux and Capgras postulated a hypertrophy of attention in which the individual focuses on particular issues to the exclusion of others, recalling the 19th-century concepts of idées fixes (for a review, see Reference Fear, McMonagle and HealyFear et al 1998). Reference KaffmanKaffman (1981) investigated this with people with delusions, finding true experiences at the root of delusion-like experiences.
Over the past two decades, these theories have been supported by data from studies of attributional, attentional and reasoning processes, including ‘hypertrophy of attention’ in such individuals (Reference Fear, McMonagle and HealyFear 1998). The Australian National Survey of Mental Health and Wellbeing found that delusion-like experience occurred in approximately 8% of their study population (n = 8841) and was more common in individuals who were under situations of ‘non-specific psychological stress [but] otherwise well’ (Reference Saha, Scott and VargheseSaha 2011). It has since been found that there is an association between post-traumatic stress disorder (PTSD), trauma and delusion-like experience (Reference Scott, Chant and AndrewsScott 2007), with a positive correlation between traumatisation and intensity of delusional ideation. Negative cognitions of self were associated with level of delusional ideation, preoccupation and distress, whereas negative cognitions about the world were associated with paranoia (Reference Calvert, Larkin and Jellicoe-JonesCalvert 2008). These findings would support a model of delusion-like experiences arising from a ‘pathology of attention’ in which individuals are sensitised into a particular belief system by a real experience, subsequently attending selectively to perceptions and experiences that support those beliefs through a mechanism that might have parallels in the re-experiencing cues of patients with PTSD. This is supported by findings of the centrality of self within the discourse of individuals with delusional disorder (Reference Noel-Jorand, Reinert and GiudicelliNoel-Jorand 2004) and the feature of self-reference found in 40% of a sample of 370 people with the disorder (Reference De Portugal, Gonzalez and HaroDe Portugal 2008).
It seems likely that delusional disorder, in its pure form, is a condition based on constitutional vulnerabilities that are part of an intact personality. Under variable levels of psychological stress, vulnerable individuals develop delusion-like responses which offer scenarios that allow them to manage the stress. The core cognitive bias is a pathology of attention in which a preoccupation with an idea is supported by cues, codes, checking and situational expression. Sadly, the lack of rigour in DSM's approach to delusional disorder has allowed a large variety of case reports claiming to describe delusional disorder where the delusions are clearly secondary to other pathology, such as multiple sclerosis (Reference Muzyk, Christopher and GaglardiMuzyk 2010), mania (Reference Vicens, Sarro and McKennaVicens 2011) and Wilson's disease with alcoholism (Reference Spyridi, Diakogiannis and MichaelidesSpyridi 2008); it has, in turn, ignored the clear links to obsessive spectrum disorders. The clear parallels between obsessional and delusional forms of jealousy, body dysmorphia, somatoform disorders and even anorexia nervosa are discussed later in this article.
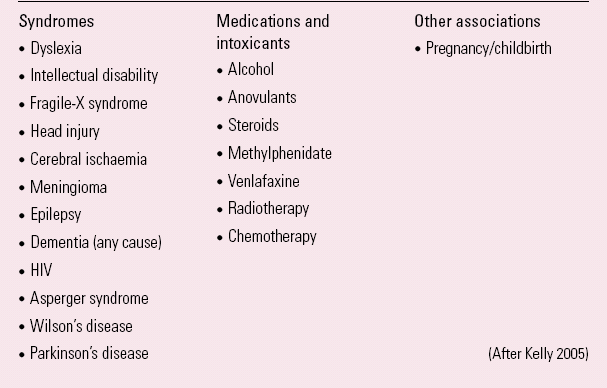
Recent reviews of two specific types of delusional disorder have proposed the distinction of ‘primary’ delusional disorder, where the diagnosis can only be made in the absence of other (psycho) pathology, and ‘secondary’ delusional disorder, where the primary pathology may be another psychiatric disorder, organic brain disorder or induced by psychoactive substances (Box 1) (Reference KellyKelly 2005; Reference Lepping, Russell and FreudenmannLepping 2007). For clarity, this review has, where possible, considered only treatment reports relating to the treatment of primary delusional disorder.
BOX 1 Medical, neuropsychiatric and other associations with delusional disorder
| Syndromes | Medications and intoxicants | Other associations |
|---|---|---|
|
|
|
(After Reference KellyKelly 2005)
Epidemiology
DSM-IV estimates the prevalence of delusional disorder in the USA to be about 0.03, suggesting that it accounts for 1–2% of hospital admissions (American Psychiatric Association 1994: p. 299). Subsequent large population studies have shown a prevalence of 0.18% in a Finnish sample aged over 30 (Reference Suvisaari, Pera and SaarniSuvisaari 2009), which equates with a finding of 2% in 378 982 out-patients and in-patients at a hospital in Thailand between 2003 and 2007 (Reference KosiyakulKosiyakul 2008). In the UK, of 227 patients presenting to an early intervention service over a 3-year period, 7% were found to have delusional disorder (Reference Proctor, Mitford and PaxtonProctor 2004). By contrast, the 467 out-patients with DSM-IV delusional disorder found in a case-register study in a south Barcelona population of 607 494 (0.08%) indicate the elusive nature of the condition. The most frequent subtypes were persecutory (48%), jealous (11%), mixed (11%) and somatic (5%); 23% were classified as ‘not otherwise specified’. Nearly 9% had a family history of schizophrenia and 42% a comorbid Axis II diagnosis, with paranoid personality disorder predominating (Reference De Portugal, Gonzalez and HaroDe Portugal 2008).
Two studies have looked at gender differences, finding a female:male ratio of 1.6:1 (Reference De Portugal, Gonzalez and MiriamDe Portugal 2010) and 1:1 (Reference Wustmann, Pillmann and MarnerosWustmann 2011), the difference between studies probably reflecting sample sizes. Men had more schizoid/schizotypal premorbid personality features, were younger at disorder onset, showed poorer long-term social functioning and were more likely to have the diagnosis changed later to schizophrenia or schizoaffective disorder. Women showed poorer initial social functioning, but regained functioning through their better engagement with therapeutic interventions; they were more likely to receive medication but their disorder was less likely to remit, although they were more able to compensate and live independently despite the delusions (Reference De Portugal, Gonzalez and MiriamDe Portugal 2010; Reference Wustmann, Pillmann and MarnerosWustmann 2011).
Diagnosis
Interviewing a patient with possible delusional disorder poses significant challenges. The patient rarely attends assessment by choice and may be encountered only when facing criminal charges or significant domestic difficulties as a result of their beliefs. Faced with someone who is, in all respects (other than their delusional system) entirely ‘normal’ and will probably be socially skilled, it may be difficult to understand where the delusional symptomatology lies. It is entirely plausible that their partner may be unfaithful; they may try to convince you that the celebrity they have been contacting has valued their contact and come armed with polite messages from them to suggest that this is the case; it is conceivable that the authorities have behaved prejudicially towards them or that the doctor missed that one diagnostic test that would have clinched the diagnosis. Interviews are likely to be a time-consuming mixture of standard psychiatric history-taking and dancing around an area that the patient is reluctant to discuss. The process may be time-consuming and is unlikely to be productive in the pressured environment of a standard psychiatric clinic.
Differential diagnosis
It is essential to take time to establish that there is no other mental or physical health problem that might better account for the presentation. The differential diagnosis includes a myriad of other psychiatric conditions, some of which are detailed in Box 2. It is essential to exclude schizophrenic and affective disorder symptoms and to distinguish from obsessive–compulsive spectrum disorders such as body dysmorphic disorder. This is done by a process of excluding other symptoms until there is a focus on the delusions as the primary issue. In practice, it can assist the building of rapport to exclude symptoms of mental health problems first rather than becoming mired in the delusional system from the outset.
BOX 2 Differential diagnoses of delusional disorder
-
• Affective psychosis: delusions are mood- congruent and the affective component is clear
-
• Anorexia nervosa: low weight and disordered body image are diagnostic
-
• Body dysmorphic disorder: preoccupation with appearance specifically excluded from delusional disorder classification
-
• Dissociative disorder: abnormal experiences occur during dissociative state only
-
• Emotionally unstable personality disorder: characteristic identity and attachment issues, risk-taking behaviour and pseudopsychotic experiences from late teens (may be comorbid)
-
• Panic disorder: loss of insight occurs as part of panic reaction only
-
• Paranoid personality disorder: general suspicion and mistrust; when formulated into a clear belief system may be comorbid with delusional disorder
-
• Obsessive–compulsive disorder: usually ego-dystonic repetitive intrusive thoughts with ‘undoing’ rituals
-
• Schizoaffective disorder: as schizophrenia but significant affective component
-
• Schizoid personality disorder: cold, reserved, aloof, lack of emotional engagement (may be comorbid)
-
• Schizophrenia: auditory hallucinations, thought alienation phenomena, negative syndrome
-
• Social phobia: loss of insight occurs in social situation or situation of public performance
-
• Somatisation disorder: history tends to be vague and multiple fluctuating symptoms as opposed to a clear delusional explanation
Understanding the delusional system
When approaching the delusional system, it is essential to establish a position whereby you neither accept nor refute the content of the beliefs. This is a genuine position since it is by no means certain that the person before you is deluded. The cultivation of an alliance in which patient and clinician agree to work together to establish the truth or otherwise of the beliefs is more likely to foster the individual's willingness to share their ideas in a setting where they feel less likely to be judged. Occasionally, it will be found that the beliefs are based on a true situation. This does not remove the possibility of delusional disorder since the circumstances in which those beliefs were formed may make them delusional even though true. For example, in the preparatory training in cognitive therapy for a research trial, a patient's therapy for delusional jealousy was affected by his wife's revelation that she was, in fact, leaving him for her lover. Although a serious problem to be managed in therapy, the jealousy was still delusional, given the basis on which the ideas were formed and their elaboration into a delusional system.
Often, a definitive position as to the truth of the underlying belief cannot be established. In such circumstances, it is necessary to proceed on the basis of available evidence, especially where the delusional belief is causing serious distress to the patient or their family.
Engagement with treatment
Having reached a diagnosis, it is necessary to engage the patient in treatment. Again, this can be done without being perceived to take sides. Some patients respond to an invitation to try treatment on the basis that they may be unwell and have nothing to lose: if the medication improves the condition, then all will be well; if it does not, then they may have another piece of evidence to support their beliefs.
It may be necessary to move to compulsory treatment. In these circumstances, it is important to recognise that the timescale for which treatment is required may be indefinite and the likelihood of a patient being taken seriously by the police, health providers, etc. will be affected by their diagnosis and compulsory status. This is not a decision to be taken lightly and must be a balance of risks.
Pharmacotherapy
First-generation (typical) antipsychotics
Although most antipsychotic medications have probably been tried in delusional disorder at some time or another, either intentionally or to treat symptoms diagnosed as schizophrenia prior to the condition's re-recognition by DSM-III-R, there is limited published evidence concerning efficacy.
From the early 1980s, a case has been made for the enhanced benefits of the diphenylbutylpiperidine antipsychotic pimozide following ‘the serendipitous response of a small number of patients with the somatic subtype’ noted by Reference MunroMunro (2006: p. 235; the whole chapter on treatment is worth reading to understand and reconsider the claims made from the studies). This led to a number of case reports reviewed by Reference Munro and MokMunro & Mok (1995). They were able to extract data on 209 individuals, the majority of whom were treated with pimozide and of whom they claimed recovery in over 50%, partial recovery in a further 28%, and no response in about 20%. It is difficult to know what to make of these claims, however, since some patients were tried on a number of drugs without full details being available, and all data were obtained from anecdotal reports, mostly of single cases or small series with an inevitable bias towards publication of reports in which benefit was observed. Nevertheless, this was sufficient evidence for pimozide to have an indication for monosymptomatic hypochondriacal psychosis (now delusional disorder somatic type) added to its datasheet and to continue to be used in spite of concerns about cardiotoxicity and sudden unexplained deaths. Three years later, a study reported on a series of seven patients who showed no response to pimozide treatment (Reference Silva, Jerez and RamirezSilva 1998).
The case for pimozide as a treatment for delusional disorder (and schizophrenia) was subjected to critical evaluation by the Cochrane Collaboration on the basis of all studies identified to July 2005 (Reference Rathbone and McMonagleRathbone 2011). Although there were 35 studies relevant for schizophrenia, none were identified for delusional disorder that had sufficient rigour to draw conclusions about efficacy. This would appear to offer a significant challenge to Munro's claims for the drug and, in view of the toxicity concerns, to render pimozide a choice of last resort given the variety of medications, particularly atypical antipsychotics, that are likely to be both safer and better tolerated. Atypical antipsychotics are now used so universally in psychosis that reports of treatment of delusional disorder with typical antipsychotics no longer feature in the psychiatric literature.
An interesting dimension was added by Reference Herbel and StelmachHerbel & Stelmach (2007), who reported on the fate of 22 offenders with delusional disorder who had been declared incompetent to stand trial and were committed for psychiatric treatment aimed to restore competency under US federal law. Sadly, the details of the delusional systems are not recorded, but the age range was 18–59 years, with a duration of untreated psychosis from 10 months to 24 years. Of those treated with first-generation antipsychotics, 12 offenders received monthly injections of haloperidol decanoate (25–150 mg), with all but 1 person (on 150 mg four-weekly) improving, while 2 failed to regain capacity on 12.5–25 mg of fluphenazine decanoate fortnightly and 1 improved on perphenazine 16 mg daily. In two cases it was necessary to add an antidepressant for post-psychotic depression. Of the seven patients who received atypical antipsychotics (see below), two failed to respond and one of the fluphenazine non-responders also failed to respond to olanzapine at 10 mg daily. The results suggest that delusional disorder can be improved with effective antipsychotic treatment. Nothing can be inferred about choice of drug except, perhaps, that adherence may be an issue, with benefits favouring the use of depot medication.
Second-generation (atypical) antipsychotics
The position of atypical antipsychotics is very much where first-generation drugs were at the time of Munro's initial studies. Like Munro, I found that patients' ‘inherent suspiciousness and specific rejection of psychiatrists’ (p. 229) prevented the completion of a double-blind placebo-controlled trial of risperidone in the early 1990s, adding, instead, a further single case report to the literature (Reference Fear and LibrettoFear 2002). There is, however, no reason to suppose that atypical antipsychotics would be any less effective than typical antipsychotics, provided the patient can be persuaded to adhere to treatment.
Reference Goreishizadeh, Farnam and MortazaviGoreishizadeh et al (2010) appear to have had more success in recruiting into a study 68 patients (54 male) with delusional disorder, mainly persecutory (n = 36) and jealous (n = 26) types. They report treating with ‘new generation antipsychotic drugs like risperidone’, with a complete response in 4.5% and more than 50% decrease in symptoms in a further 84%. Unfortunately, there is little detail in the paper on dosing or duration of treatment, no standardised assessment tool used to measure improvement, and no placebo control.
Reference Manshrek and KhanManshrek & Khan (2006) identified 224 cases of delusional disorder reported in the world literature over a 10-year period to 2004, but could find sufficient treatment and outcome data for only 134 individuals with predominantly somatic (35.7%) or persecutory (38%) types. Of these, 45% were treated with pimozide and the authors found a difference in recovery rates, favouring pimozide, that approached significance (P =0.055). Looking solely at the sample with somatic delusions, the results appear to favour pimozide, although the number of patients treated with this drug (47 out of 64) and the small sample size treated with other antipsychotics make the observed statistical difference (P = 0.0004) questionable. The most important observation from this review, however, is that nearly 94% of patients showed a favourable response regardless of the medication used. There were five case reports of patients who benefitted in decreased intensity of symptoms with clozapine treatment, following lack of success with typical antipsychotics.
Case reports of primary delusional disorder concerning a further 20 patients have been published since 2004: 17 of these cases were somatic type, delusions of infestation/parasitosis accompanied by tactile hallucinations. A further somatic type, again with tactile hallucinations, involved the delusion of reduplication of the patient's lower jaw with evidence of a possible temporoparietal abnormality on a positron emission tomography scan (Reference Akahane, Hayashi and SuzukiAkahane 2009). There was also one case report each of delusional jealousy and erotomania. Of the nine English-language reports where drug and dose were specified (details available from the author on request), four patients apparently responded to olanzapine (2.5–10 mg), four to risperidone (1–3 mg), one to aripiprazole (jealous type; 30 mg), and one to quetiapine (erotomanic type; 150 mg). A further three each responded to risperidone and aripiprazole, two to olanzapine and one to quetiapine, with no doses stated. A report of response of delusional parasitosis to aripiprazole in combination with antidepressants may simply reflect delusions secondary to depression (Reference Dimopoulos, Mitsonis and PsarraDimopoulos 2008). From the study of compulsory treatment to restore competency, cited earlier (Reference Herbel and StelmachHerbel 2007), one patient responded to risperidone (2–4 mg), one failed to respond to quetiapine (200–700 mg), and one failed to respond to trials of these drugs at similar doses and to olanzapine (10 mg).
Other drug treatment
Two single case reports of response of somatic delusional disorder to paroxetine (Reference Hayashi, Oshino and IshikawaHayashi 2004), and to an unspecified selected serotonin reuptake inhibitor (SSRI) (Reference AlexanderAlexander 2010), offer further evidence of the lack of rigour in applying the diagnosis to patients whose mood-congruent delusions of body odour and halitosis were highly likely to have been secondary to depression. Although there is no evidence for the role of SSRIs in the treatment of primary delusional disorder, as will be discussed below, the evidence for their use in other monodelusional conditions suggests that their investigation in delusional disorder is overdue.
Cognitive and behavioural therapy
The work of a number of groups during the 1990s focused on the management of individual psychotic symptoms, such as delusions and hallucinations, in isolation from their underlying conditions (e.g. Reference Rankin and O'CarrollRankin 1995; Reference Sharp, Fear and HealySharp 1997; Reference Garety and FreemanGarety 1999; Reference Bentall, Corcoran and HowardBentall 2001). Although these could be criticised for missing the point that associated affect and psychotic experiences can have a profound effect in maintaining an individual's delusional system, they were invaluable in providing an evidence base for exploring and challenging a patient's abnormal beliefs. Previously these had been avoided, either through the mistaken view that exploring the origins of beliefs provided validation and collusion or through the misunderstanding that all delusions were, by their nature, un-understandable. There is now overwhelming evidence that delusions can and do respond to lengthy and intensive individual cognitive therapy, but few study samples comprising only patients with delusional disorder (for a review, see Reference Freeman, Bentall and GaretyFreeman 2008).
Aside from single case reports, two studies have undertaken work with patients with delusional disorder. Reference Sharp, Fear and WilliamsSharp et al (1996) reported on a series of six patients, three of whom responded to cognitive therapy. The key factor predicting response was a reduction in conviction from 100% during the baseline phase of information gathering and before therapy actually started. Conviction was significantly associated with belief maintenance factors in all three individuals but there were no consistent associations. Affect associated with the belief, willingness to talk to others about the belief, negative behaviours and insight were associated with conviction in some, but not all, patients; preoccupation and acting on the belief varied systematically independently of belief conviction.
More recently, a Canadian group (Reference O'Connor, Stip and PelissierO'Connor 2007) has compared cognitive–behavioural therapy (CBT) v. attention placebo control in 24 patients with delusional disorder over a 24-week treatment period. Eleven patients completed the CBT treatment, whereas half dropped out of the attention placebo control group. In addition to a lower drop-out rate from therapy, CBT produced a greater reduction in affect relating to belief, strength of conviction and positive action on belief subscales of the Maudsley Assessment of Delusions Schedule. Although the delusions were not abolished by CBT, the positive changes provide a strong basis for further work on managing the individual's response to their delusional systems, improving social inclusion and reducing risk.
Electroconvulsive therapy
Although Reference FinkFink (1995) considered electroconvulsive therapy (ECT) to be an ‘antidelusional agent’, there have been few reports of its use and the reported benefits may have resulted from the resolution of underlying depression. A case report of somatic delusional disorder responding to ECT did not sufficiently exclude an affective component (Reference Ota, Mizukami and KatanoOta 2003). Furthermore, given that the response of psychotic phenomena in schizophrenia to ECT is not long lasting, there would appear to be no indication for the use of ECT in delusional disorder (for a review, see Reference Fear and ScottFear 2005).
The spectrum of disorders of attention bias
There are a number of conditions that involve a preoccupation with a single aspect of an individual's experience, including: morbid jealousy, where the core issue is a partner's fidelity; body dysmorphic disorder, where the focus is on appearance; somatoform disorders, involving illness; and anorexia nervosa, where the issue is body image. Each of these has a fundamental issue of attention bias and can show a range of pathologies from obsessive preoccupation, through delusion-like ideas, to true delusion. In the case of anorexia nervosa, it is not usually accepted that the incorrigible distortion of body image represents other than an ‘overvalued idea’, although there is evidence that such ideas reach delusional proportions (Reference Steinglass, Eisen and AttiaSteinglass 2007) and respond to olanzapine treatment (Reference Dunican and DelDottoDunican 2007). Indeed, there has long been a school of thought that recognises the apparent link between conditions involving obsession and those involving delusions (Reference Fear, Sharp and HealyFear 1995). Nowhere is this better demonstrated than in morbid jealousy and its delusional version (Reference Kingham and GordonKingham 2004). A variety of mechanisms have been proposed for this, including loss of insight and resistance to obsessions, depressive change and the finding that some individuals with obsessive–compulsive disorder have similar attention and attitudinal biases to those who develop delusional disorder, a ‘delusional diathesis’ (Reference Fear, Sharp and HealyFear 2000).
The possibility that delusional disorder may arise from a similar pathology of attention to obsessive disorders offers new ground to explore in pharmacotherapy. There is considerable evidence for obsessive–compulsive disorder and related disorders, particularly body dysmorphic disorder, responding to SSRIs (National Institute for Health and Clinical Excellence 2005). Although the published reports of response of delusional disorder to these drugs are few and can be explained through comorbid affective disorder, the potential of SSRIs to improve delusional disorder is worthy of serious exploration. If the conditions are, indeed, linked through a pathology of attention, it may be worth using higher doses of SSRIs in a way which is well-evidenced for obsessive spectrum disorders.
Conclusions
With the third revision to DSM since delusional disorders were resurrected as a diagnostic entity distinct from schizophrenia, there remains considerable confusion about their place in the psychiatric pantheon. It is perhaps only human nature that has caused a focus on the many and varied delusional contents, rather than underlying psychopathological form, even though these offer no prediction of likely response to treatment. Looking to the phenomenology, the meaning of delusion in delusional disorder has undergone considerable change, and is more akin to delusion-like ideas which have been shown to arise from cognitive biases, especially a pathology of attention that recalls the 19th-century notion of idées fixes. Although there is evidence that true delusional disorder is unlikely to be related to schizophrenia, the inflexibility of classification systems does not allow a condition that has delusional pathology without any affective disorder to be considered other than as a schizophrenia spectrum disorder. There remains considerable confusion in the literature as to what constitutes delusional disorder and which comorbidities are ‘allowed’: it would aid study greatly if journal editors and reviewers were more rigorous in their publication of papers purporting to describe these fascinating conditions.
Cognitive therapy has established a place in the management of delusional disorder but is time-consuming and the outcome data are limited. The increasing evidence for dysfunctional cognitive styles at the heart of delusional disorder suggests that further research into psychotherapeutic interventions is merited.
In respect of pharmacotherapy, a randomised controlled trial is still awaited from researchers able to overcome the significant challenges involved. Without this, we are left with case reports and series which appear to demonstrate response to antipsychotic medication, although not the specific response to pimozide that was previously reported. The nature of the condition dictates that concordance is likely to be an issue but, where patients were known to be adherent to the medication or it was given in the form of a long-acting injection, there is good anecdotal evidence to suggest a response. There is no evidence to suggest that first- or second-generation antipsychotics are likely to be more effective at controlling the symptoms, but ease of use in a reluctant patient would tend to favour atypical over typical antipsychotics (Box 3). Experience with obsessive–compulsive spectrum disorders with delusional components to them suggests a possible further line of treatment with SSRIs, but there is, as yet, no evidence. It is hoped that new generations of researchers will come forward to study these intriguing, but frustrating, patients.
BOX 3 Treating delusional disorder
Medication
-
• No randomised controlled trial evidence
-
• Case reports suggest that the disorder is amenable to treatment with any effective antipsychotic drug but that attention to adherence is important and patients may default on treatment without telling the clinician
-
• Drugs amenable to plasma-level assay allow monitoring of adherence
-
• Use a second-generation (atypical) antipsychotic for preference and begin with a low dose to reduce discontinuation due to adverse effects
-
• Increase the dose as required in accordance with product recommendations
-
• It may be necessary to try different drugs before finding one that the patient is prepared to take
-
• If treatment has to be offered compulsorily, use an orodispersible form and monitor taking, or use depot/long-acting injection
-
• No evidence for duration of maintenance treatment and it may be lifelong
Psychological therapy
-
• Evidence only for cognitive therapy, which has trial data but is intensive and may not be cost-effective
-
• Psychodynamic/psychoanalytical therapy has no evidence and may be harmful as it requires the patient to revisit their experiences in detail, thus re-affirming the delusional belief
-
• Symptomatic work based around anger management, social skills and living skills may be beneficial but will not address the core delusion
ECT
-
• No evidence for long-term benefit unless there is underlying affective disorder
MCQs
Select the single best option for each question stem
-
1 One antipsychotic drug with a licence for treating at least one delusional disorder subtype is:
-
a olanzapine
-
b paroxetine
-
c pimozide
-
d flupentixol decanoate
-
e methylphenidate.
-
-
2 The following is not a DSM-IV subtype of delusional disorder:
-
a body dysmorphic
-
b jealous
-
c erotomanic
-
d grandiose
-
e persecutory.
-
-
3 When assessing a patient with suspected delusional disorder:
-
a a police officer should usually be present
-
b it is essential to challenge the delusional belief from the outset
-
c the presence of first-rank symptoms confirms the diagnosis
-
d it is important to establish a rapport based on impartiality
-
e a family history of schizophrenia is not relevant.
-
-
4 The following psychological therapy has an evidence base for treating delusional disorder:
-
a psychodynamic
-
b cognitive
-
c anger management
-
d rational emotive therapy
-
e psychodrama.
-
-
5 The following type of hallucination can occur in delusional disorder subtypes:
-
a visual
-
b ‘third person’ auditory
-
c passivity experience
-
d Capgras syndrome
-
e tactile.
-
MCQ answers
| 1 | c | 2 | a | 3 | d | 4 | b | 5 | e |




eLetters
No eLetters have been published for this article.