Poster Presentation - Top Poster Award
Antibiotic Stewardship
Clinical factors and diagnoses associated with inappropriate urine-culture ordering in primary care
- Marissa Valentine-King, Barbara Trautner, Roger Zoorob, Michael Hansen, Jennifer Matas, Robert Atmar, Larissa Grigoryan
-
- Published online by Cambridge University Press:
- 29 September 2023, p. s1
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Inappropriate urine-culture ordering is associated with increased antibiotic prescribing in myriad care environments, including acute and long-term care. In primary care, where urinary tract infections (UTIs) are commonly encountered, the appropriateness of urine-culture ordering has not been well described. We examined the appropriateness of urine-culture ordering and factors associated with inappropriate urine-culture ordering in primary care. Methods: We conducted a secondary analysis of data from a previous prospective study that included patients aged ≥18 years presenting with provider-suspected UTI with an accompanying urine culture at 2 safety-net, primary-care clinics in Houston, Texas, between November 2018 and March 2020. Patients with complicated or uncomplicated UTI were included, but those with a urinary catheter and pregnant females were excluded. Urine cultures were considered appropriate if the patient had an evidence-based symptom of UTI (ie, dysuria, frequency, urgency, hematuria, fever, chills, costovertebral angle tenderness, suprapubic, pelvic, or flank pain, or nephrolithiasis) as a diagnostic code or listed in providers’ free-text documentation. Diagnostic codes for symptoms that were not evidence based were grouped into categories based on body system, visit type (eg, routine visit), or sign or symptom clusters. We evaluated the relationships among demographic and clinical factors, the clinic visited, and non–evidence-based diagnostic codes with inappropriately ordered cultures. Results: We examined 870 cultures from 807 patients. Overall, 61.5% of patients were Hispanic (61.5%) and 23% were African American or Black. Also, 70.6% were women; the mean age was 49.2 years (SD, 14.6); and the mean Elixhauser score was 1.9 (SD, 5.4). Among the 870 cultures, 210 (24%) were ordered inappropriately. Dysuria (n = 289), frequency (n = 129), and UTI or cystitis (n = 117) were the most common, evidence-based codes among appropriate cultures. In the adjusted model, the nonteaching clinic (aOR, 6.33) and diagnostic codes comprising the following categories were associated with inappropriate culturing: acute lower back pain (aOR, 5.42), cardiac-related visits (aOR, 2.41), urinary incontinence (aOR, 4.46), routine health visits (aOR, 3.66), urine characteristics (aOR, 14.32), voiding difficulties (aOR, 3.88), and well-woman visits with a gynecological exam or family planning aspect (aOR, 12.27) (all P < .05). Conclusions: This research highlights potential gaps or miscues in provider behavior related to urine culture ordering, and unveiled problematic culturing related to urine characteristics and to routine visits, especially of a gynecological nature. This information can be incorporated into diagnostic stewardship interventions to address misconceptions, and to further explore the reasoning or processes wherein urine cultures are ordered for routine visits.
Financial support: NIAID UM1AI104681
Disclosure: None
Impact of the COVID-19 pandemic on inpatient antibiotic use in Indonesia and the Philippines
- Amara Fazal, Olivia McGovern, Garrett Mahon, Fernanda Lessa, Ma Tarcela Gler, Jemelyn Garcia, Mark Festin, Kuntaman Kuntaman, Ida Parwati, Cherry Siregar, Jay Christian, Gina de Guzman Betito, Maya Montemayor, Arleen De Leon, Emmeline Borillo, Mark Llanes, Regina Berba, Musofa Rusli, Farizal Rizky, Mariyatul Qibtiyah, Bambang Semedi, Rosantia Sarassari, Leonardus Widyatmoko, Basti Andriyoko, Adhi Sugianli, Dewi Turbawaty, Ivo Ranita, Franciscus Ginting, Made Krisna, Rahmadania Marita Joesoef, Twisha Patel
-
- Published online by Cambridge University Press:
- 29 September 2023, pp. s1-s2
-
- Article
-
- You have access Access
- Open access
- Export citation
-
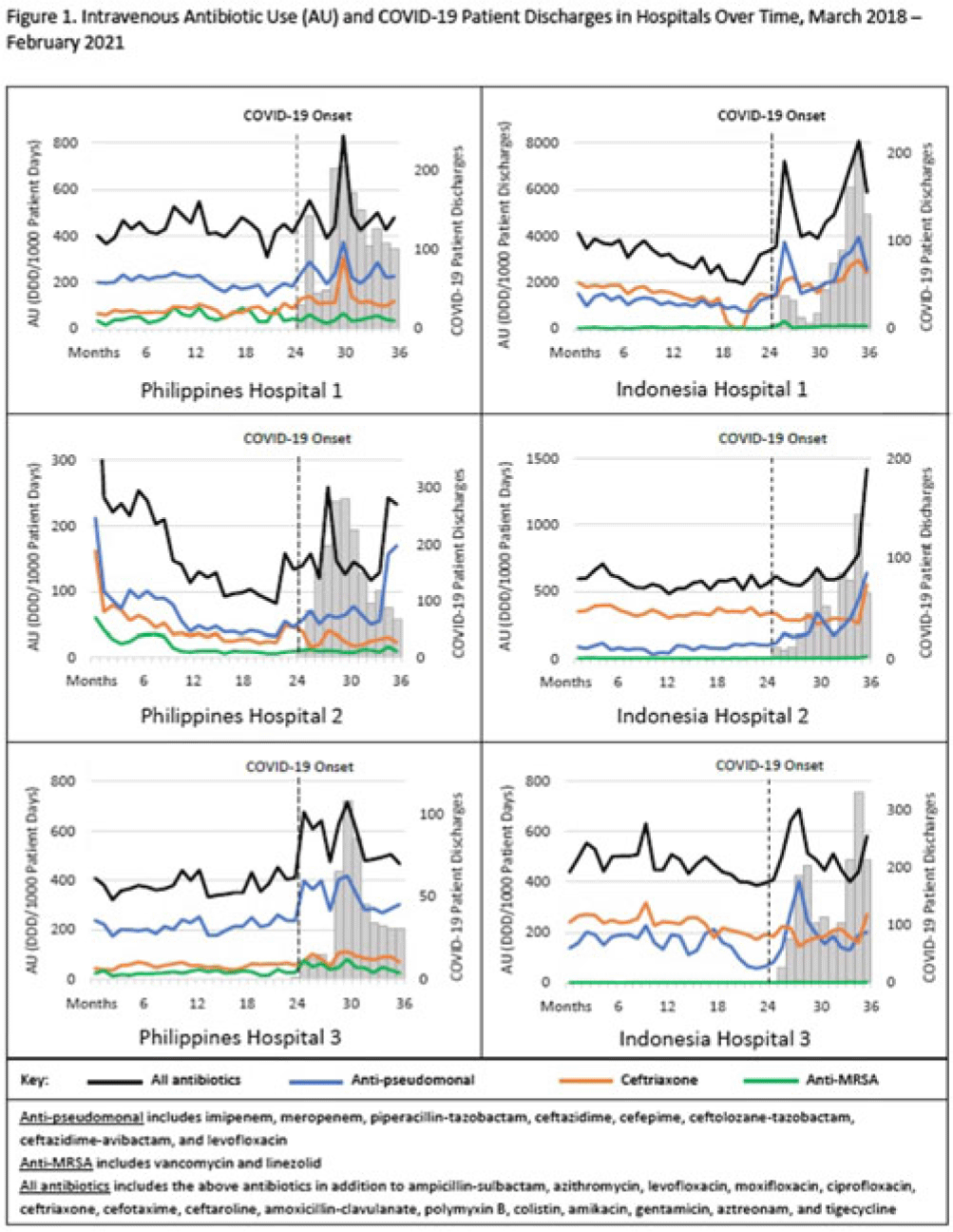
Background: The coronavirus disease 2019 (COVID-19) pandemic severely affected Southeast Asia, with >35 million cases and ~360,000 deaths. Despite relatively low rates of secondary bacterial infection among inpatients with COVID-19, several countries reported increased antibiotic use; raising concerns for worsening antimicrobial resistance. We assessed the impact of the COVID-19 pandemic on the use of antibiotics commonly used to treat respiratory infections in Southeast Asia. Methods: We evaluated intravenous antibiotic use among hospitalized adults in acute-care wards in 6 hospitals; 3 in Indonesia and 3 in the Philippines. We abstracted data on antibiotics that are commonly used to treat respiratory infections in these hospitals. We calculated antibiotic use rates for the 25 included antibiotics as monthly defined daily dose per 1,000 patient days (or patient discharges where patient days was unavailable) using data from pharmacy dispensing records and administrative records. Median antibiotic use rates for the prepandemic period (March 2018–February 2020) and the pandemic period (March 2020–February 2021) were compared, and percentage changes were calculated for (1) all 25 antibiotics combined; (2) ceftriaxone; (3) vancomycin and linezolid combined (anti-MRSA); and (4) broad-spectrum antibiotics with activity against Pseudomonas aeruginosa (anti-PSA). Monthly antibiotic use and COVID-19 patient discharges were graphed over the 36-month study period (March 2018–February 2021) to visualize trends (Fig. 1). The Wilcoxon rank-sum test was used to determine whether differences in median antibiotic use rates were statistically significant (2-tailed P < .05). Results: Overall, trends in antibiotic use were higher during months with increased COVID-19 patient discharges (Fig. 1). Use of all 25 antibiotics combined significantly increased in 4 of 6 hospitals (6.9%–63.6%) during the pandemic period compared to the prepandemic period. Ceftriaxone use significantly increased in 3 of 6 hospitals (37.1%–55.4%) and decreased in 3 of 6 hospitals (15.9%–31.9%). Anti-PSA antibiotic use significantly increased in 4 of 6 hospitals (16.1%–161.5%). Although anti-MRSA antibiotic use was low (comprising <2% of the overall included antibiotic use in Indonesia and <11% in the Philippines), use during the pandemic increased in 3 of 6 hospitals (59.8%–212.6%). Conclusions: We observed substantial increases in antibiotic use among hospitalized adults in Indonesia and the Philippines during the COVID-19 pandemic. The increased use of broad-spectrum antibiotics is concerning given the potential consequence of worsening antimicrobial resistance. Understanding how increases in antibiotic use compares to rates of bacterial infection, antimicrobial resistance, and antibiotic availability and accessibility during this time is important to contextualize results. These findings reinforce the importance of antibiotic stewardship practices to optimize antibiotic use, especially during pandemics.
Disclosure: None
Multi-faceted approach to decreasing inappropriate antibiotic prescribing for viral upper respiratory tract infections
- Jamilah Shubeilat, Dan Ilges, Angie Ton, Angela Huang, M. Teresa Seville
-
- Published online by Cambridge University Press:
- 29 September 2023, p. s2
-
- Article
-
- You have access Access
- Open access
- Export citation
-
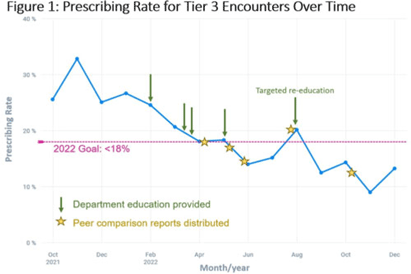
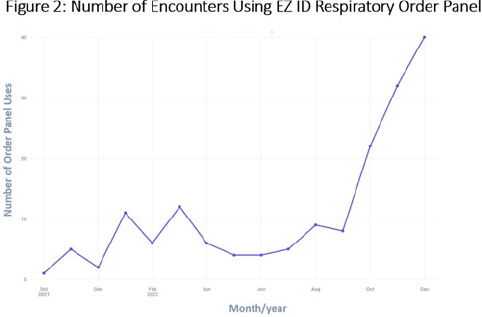
Background: Prescribing of antibiotics for viral upper respiratory infection (URI) remains a pressing public health problem. We sought to reduce inappropriate prescribing of antibiotics for viral URIs at primary-care practices at Mayo Clinic Arizona (MCA). Methods: Diagnostic codes for URIs commonly caused by viruses were categorized as tier 3 (ie, never prescribe). The inappropriate prescribing rate was defined as the number of tier 3 encounters resulting in a prescription for a URI antibiotic divided by the total number of tier 3 encounters. MCA primary-care departments, including family medicine, community internal medicine, emergency medicine, and women’s health internal medicine, were included in the intervention. Each department was briefed on the project, including baseline department prescribing data, and was provided education. Education topics included appropriate indications for antibiotics, patient-centered strategies for reducing antibiotic use, and a review of electronic resources developed specifically for the project. Resources included a syndromic ambulatory order panel (EZ ID Respiratory Order Panel) and a viral prescription pad, which contains simplified over-the-counter recommendations for symptomatic management of viral URIs and patient education. Quarterly peer comparison reports were provided to the department chairs and/or site leads. Our goal was to reduce inappropriate prescribing by 22% in 2022. An Epic dashboard (SlicerDicer model) was developed to track data on an ongoing basis. We used χ2 tests to compare categorical variables. Results: Department education was completed by June 2022 (Fig. 1). The annual antibiotic prescribing rate for tier 3 encounters decreased by 29% from a baseline rate 23.6% in 2021 to 16.4% in 2022 (P < .001). The posteducation prescribing rate (June 2022–December 2022) was 13.1%. Utilization of the EZ ID ambulatory order panel increased from an average of 1.5 uses per month in 2021 to 13.3 uses per month in 2022 (Fig. 2). Repeated healthcare contact for URIs within 14 days of tier 3 encounters did not differ among patients prescribed and not prescribed an antibiotic in all of 2022 (3.8% vs 3.9%; P = .91) or during the posteducation period (1.8% vs 4.2%; P = .14). There was no appreciable diagnostic shift over the course of 2022 (Fig. 3). Conclusions: A multifaceted intervention, which included baseline education, promotion of syndrome-specific order panels, dissemination of resources for symptomatic management, and distribution of peer comparison reports, resulted in significant reduction of inappropriate antibiotic prescribing for URIs.
Disclosure: None
Description of antibiotic stewardship expertise and activities among US public health departments, 2022
- Destani Bizune, Angelina Luciano, Melinda Neuhauser, Lauri Hicks, Sarah Kabbani
-
- Published online by Cambridge University Press:
- 29 September 2023, p. s3
-
- Article
-
- You have access Access
- Open access
- Export citation
-
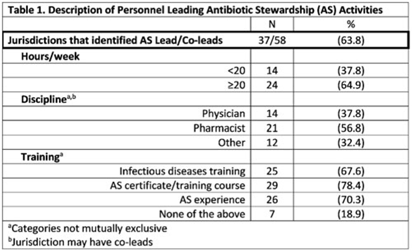
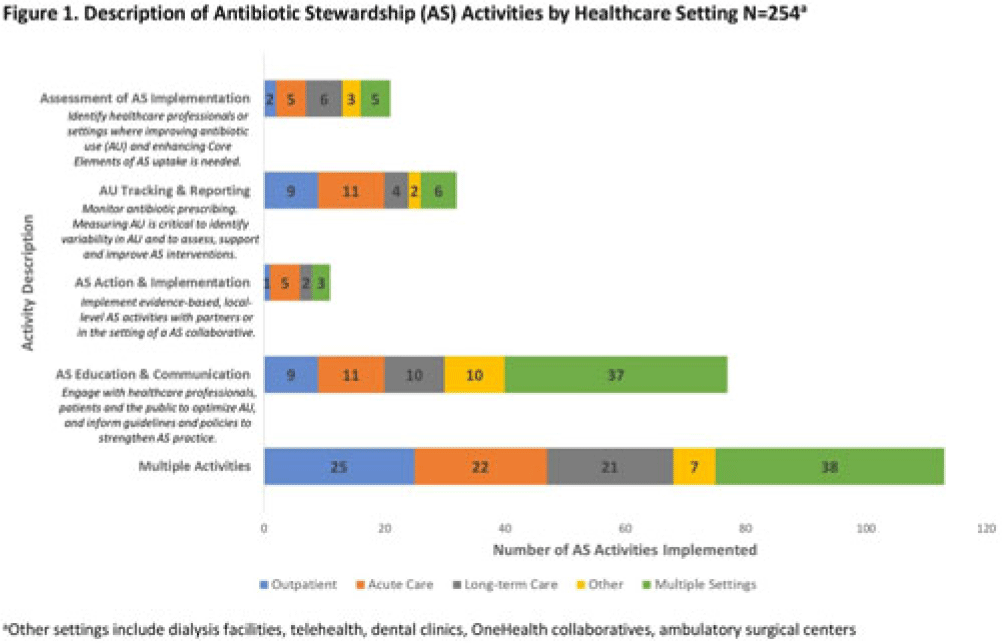
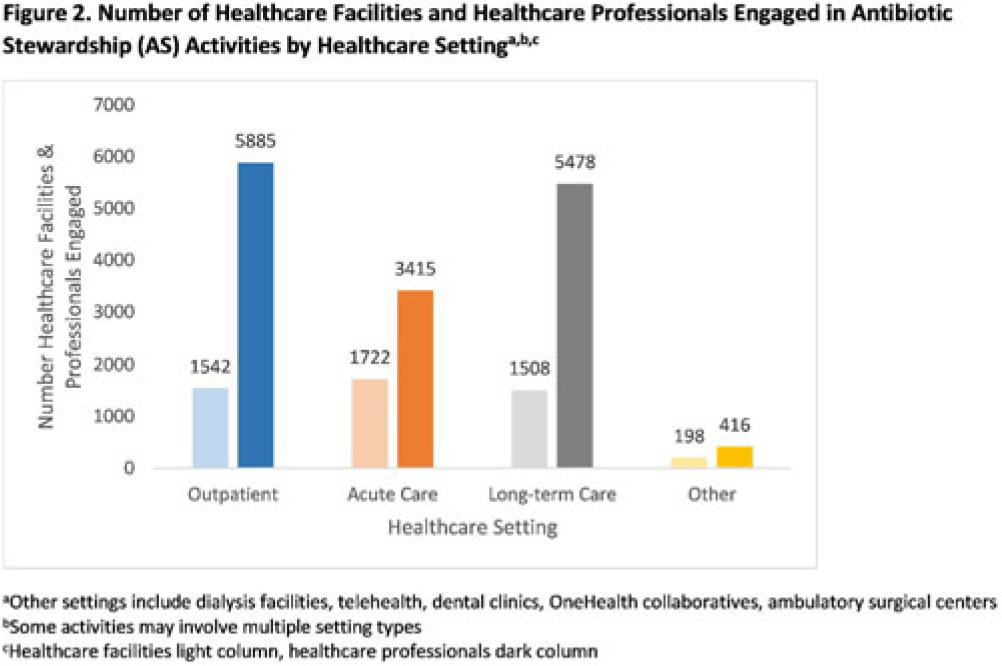
Background: In 2021, the CDC awarded >$100 million to 62 state, local, and territorial health departments (SLTHDs) to expand antibiotic stewardship expertise and implement antibiotic stewardship activities in different healthcare settings. Our objective was to describe SLTHD antibiotic stewardship personnel and activities to characterize the impact of the funding. Methods: SLTHDs submitted performance measures, including quantitative and qualitative responses, describing personnel supporting antibiotic stewardship activities, types of activities, and healthcare facilities and professionals engaged from January through June 2022. A quantitative analysis of performance measures and qualitative thematic analysis of select narrative responses are reported. Results: Most SLTHDs (58 of 62, 94%) submitted performance measures. Among them, 37 (64%) reported identifying an antibiotic stewardship leader or coleader; most were pharmacists (57%) or physicians (38%) with infectious diseases training (68%) (Table 1). Of the remaining STLHDs, 20 reported barriers to identifying a leader or coleader, including hiring process delays and programmatic barriers (Table 2). SLTHDs reported 254 antibiotic stewardship activities; most reported activities involving multiple activity types (44%). Education and communication (eg, providing stewardship expertise) was the most common single activity (30%), followed by antibiotic use tracking and reporting (13%), assessment of antibiotic stewardship implementation (8%), and action and implementation (eg, audit and feedback letters) (4%). The highest number of activities were implemented in multiple healthcare settings (35%), followed by acute care (21%), outpatient (18%), long-term care (17%), and other (9%) (Fig. 1). SLTHDs reported engaging 4,970 healthcare facilities and 15,194 healthcare professionals in antibiotic stewardship activities across healthcare settings, to date, as part of this funding opportunity (Fig. 2). Conclusions: Antibiotic stewardship funding to SLTHDs allowed for increases in capacity and expanded outreach to implement a variety of antibiotic stewardship activities across multiple healthcare settings. Sustaining STLHD antibiotic stewardship activities can help increase engagement and coordination with healthcare facilities, healthcare professionals, and other partners to optimize antibiotic prescribing and patient safety.
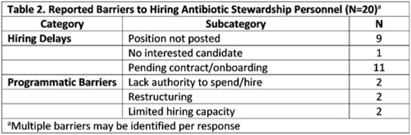

Disclosure: None
Fear of missing organisms (FOMO): Diabetic foot and osteomyelitis management opportunities
- Morgan Morelli, Andrea Son, Yanis Bitar, Michelle Hecker
-
- Published online by Cambridge University Press:
- 29 September 2023, pp. s3-s4
-
- Article
-
- You have access Access
- Open access
- Export citation
-
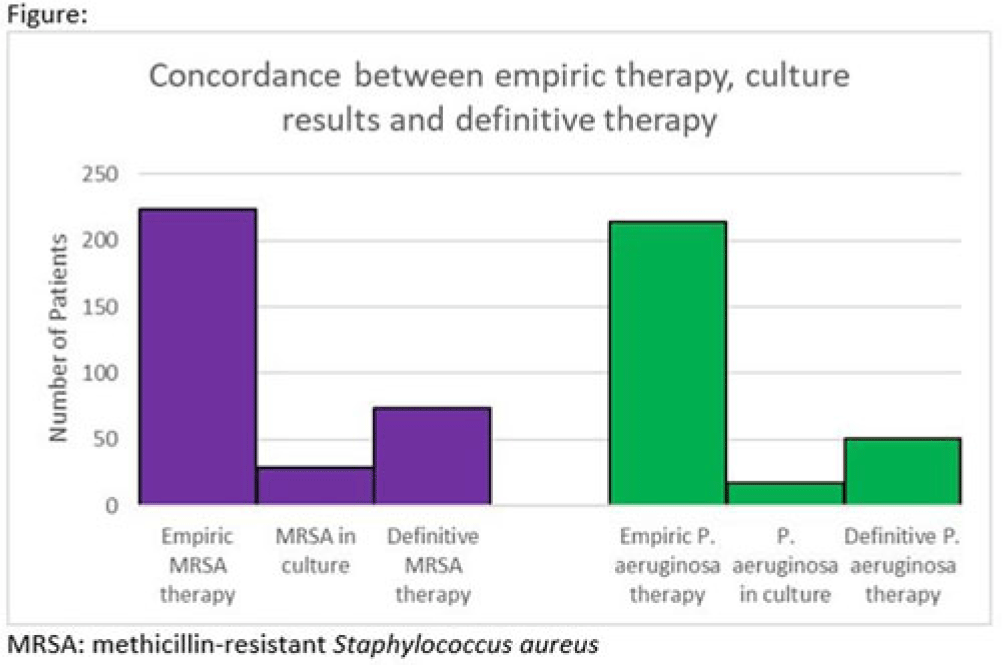
Background: Hospitalizations for diabetic foot infections and lower-extremity osteomyelitis are common. Use of empiric antibiotic therapy for methicillin-resistant Staphylococcus aureus (MRSA) and Pseudomonas aeruginosa is also common. Guidelines recommend antibiotic therapy based on severity of illness, risk factors for MRSA and P. aeruginosa, and local prevalence. We evaluated the concordance between empiric antibiotic therapy and both culture results and definitive antibiotic therapy with a focus on MRSA and P. aeruginosa. We also evaluated how well MRSA and pseudomonal risk factors were predictive of culture results with these organisms. Methods: We conducted a cohort study of all patients admitted to our hospital system in 2021 with a diagnosis of a diabetic foot infection or lower-extremity osteomyelitis. Patients were included if they had an International Classification of Disease, Tenth Revision (ICD-10) diagnosis code of M86, E10.621, E11.621, or E08.621. Patients were excluded if antibiotics were for another indication or if they were aged <18 years. In patients with multiple hospitalizations only the first hospitalization was included. Empiric antibiotic therapy included antibiotics started by the admitting team. Definitive antibiotic therapy included the final antibiotic course either completed during admission or prescribed at the time of discharge. MRSA risk factors included prior positive culture with MRSA within the last year, hospitalization with IV antibiotics within 90 days, intravenous drug use, or hemodialysis. Pseudomonal risk factors included prior positive culture with P. aeruginosa within the last year or hospitalization with IV antibiotics within 90 days. Results: In 2021, 260 unique patients were admitted with suspected diabetic foot infections or lower-extremity osteomyelitis. 68 patients had >1 admission. Empiric anti-MRSA and antipseudomonal therapy was administered to 224 (86%) and 214 (82%) patients, respectively. Definitive anti-MRSA and antipseudomonal therapy was administered to 76 (30%) and 51 (20%) patients, respectively. Of the 195 patients who had wound cultures, 29 (15%) and 18 (9%) had positive cultures for MRSA and P. aeruginosa respectively (Fig.). The negative predictive value of MRSA risk factors for predicting a negative culture with MRSA was 91%. The negative predictive value of pseudomonal risk factors for predicting a negative culture with P. aeruginosa was 95%. Conclusions: Our data suggest an opportunity for substantial reductions in empiric anti-MRSA and antipseudomonal therapy for diabetic foot infection and lower-extremity osteomyelitis. The absence of MRSA and pseudomonal risk factors was reasonably good at predicting the absence of a positive culture with these organisms.
Disclosure: None
Inpatient pediatric antimicrobial use for respiratory infections during the RSV surge
- Aaron Hunt, Rodrigo Burgos, Alfredo Mena Lora
-
- Published online by Cambridge University Press:
- 29 September 2023, pp. s4-s5
-
- Article
-
- You have access Access
- Open access
- Export citation
-
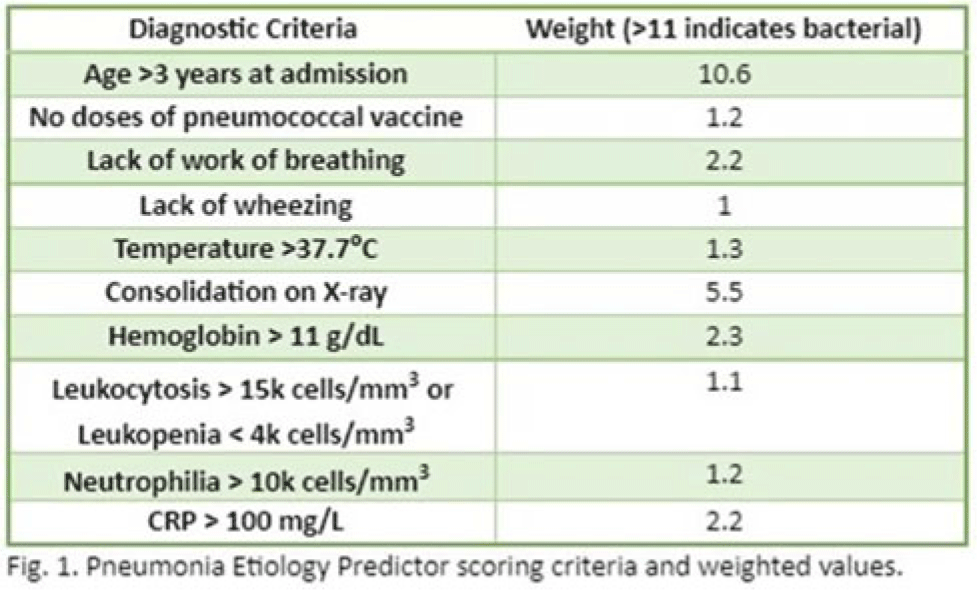
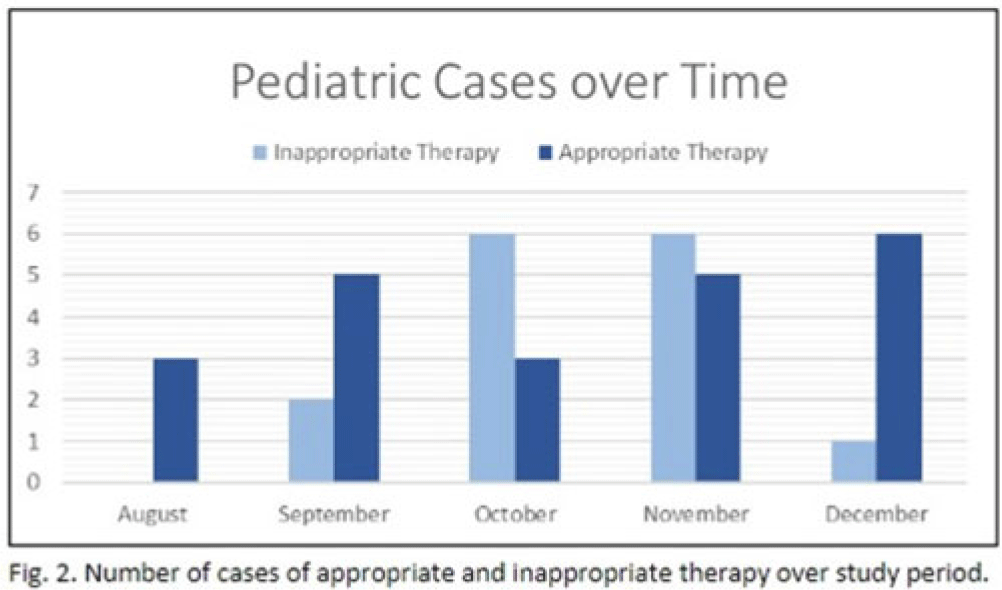
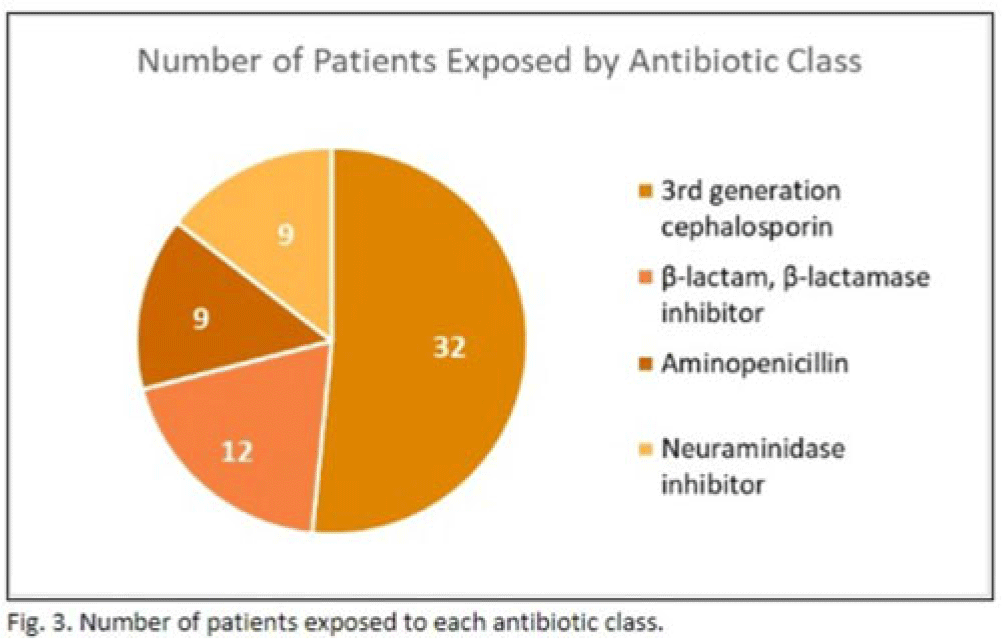
Background: In the United States, pneumonia causes >100,000 pediatric hospitalizations annually. On November 4, 2022, the CDC issued a Heath Advisory concerning an upcoming surge of respiratory illnesses including SARS-CoV-2, influenza, and respiratory syncytial virus (RSV). Differentiating between viral and bacterial causes is challenging and can lead to antimicrobial overuse. Currently, tools are being developed to distinguish between viral and bacterial pneumonia. The VALS-DANCE Pneumonia Etiology Predictor (PEP) provides clinical scoring criteria (Fig. 1) to determine probable cause of pneumonia with 93.1% sensitivity for bacterial pneumonia. Scores >11 have a >25% likelihood of having bacterial etiology. Given that antimicrobial exposure increases resistance rates, disrupts natural flora, and increases the risk of side effects, a core goal of researchers is to develop ways to promote stewardship and reduce inappropriate use. We assessed the patterns of use for antimicrobials in pediatric patients admitted with pneumonia at our institution. Methods: This retrospective review included pediatric cases admitted to an urban safety-net community hospital from July 22, 2022, to December 16, 2022. A daily list of all patients receiving antimicrobials was reviewed, and pediatric patients with diagnosis of a respiratory infection were included. Patients with additional indications for antimicrobial therapy, diagnosis of bronchitis, incomplete records, or without complete information were excluded from the scoring criteria. The primary objective was to assess the appropriateness of antimicrobial use for pneumonia, defined as use consistent with PEP scoring recommendations. Results: Of 53 patients reviewed, 37 met inclusion criteria. Of 37 patients, 22 (59.5%) met study criteria for appropriate therapy. The 15 patients (40.5%) who were inappropriate for treatment received an average of 4.67 ± 1.91 days of antibiotics. Of these 15 patients, 11 (73.3%) also had a positive viral test, further increasing the likelihood of a viral etiology. This subgroup had an average antibiotic exposure of 4.27 ± 1.79 days. Documented rationale for therapy included severity of illness (4 of 11), radiograph consolidation (4 of 11), and provider disagreement with radiograph interpretation (3 of 11). Conclusions: Pediatric respiratory infections represent a significant opportunity for antimicrobial stewardship. In this study, as many as 40% of pediatric patients may have received unnecessary antibiotic exposure. Use of the VALS-DANCE criteria may help clinicians identify patients with low likelihood of bacterial infection and reduce antimicrobial use. The national surge of viral infections serves to highlight the vital importance of appropriate diagnostic stewardship.
Disclosure: None
C. difficile
Integrated efficacy analysis from phase 3 studies of investigational microbiome therapeutic, SER-109, in recurrent Clostridioides difficile infection
- Matthew Sims, Michael Silverman, Thomas Louie, Elaine Wang, Colleen Kraft, Mayur Ramesh, Tatiana Bogdanovich, Kelly Brady, David Lombardi, Asli Memisoglu, Ananya De, Brooke Hasson, Christine Lee, Paul Feuerstadt, Darrell Pardi, Colleen Kelly, Peter Daley, Godson Oguchi, Barbara McGovern, Lisa Von Moltke
-
- Published online by Cambridge University Press:
- 29 September 2023, p. s5
-
- Article
-
- You have access Access
- Open access
- Export citation
-
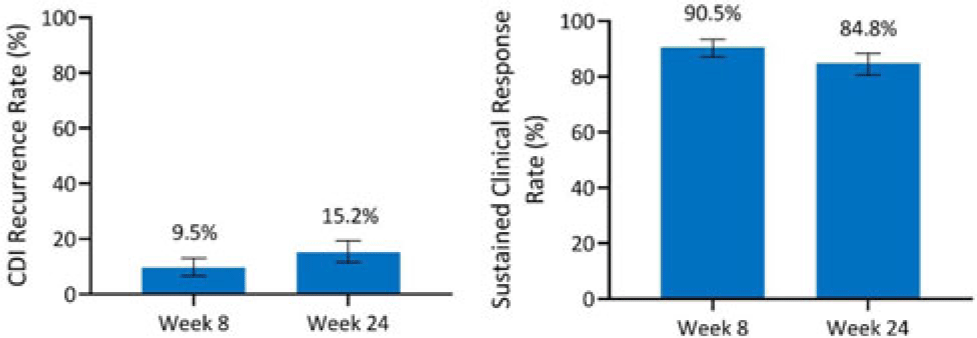
Background: Antibiotics alone are often insufficient to treat recurrent C. difficile infection (rCDI) because they have no activity against C. difficile spores that germinate within a disrupted microbiome. SER-109, an investigational, oral, microbiome therapeutic comprised of purified Firmicutes spores, was designed to reduce rCDI through microbiome repair. We report an integrated efficacy analysis through week 24 for SER-109 from phase 3 studies, ECOSPOR III and ECOSPOR IV. Methods: ECOSPOR III was a randomized, placebo-controlled phase 3 trial conducted at 56 US or Canadian sites that included 182 participants with ≥2 CDI recurrences, confirmed via toxin EIA testing. Participants were stratified by age (<65 years or ≥65 years) and antibiotic regimen (vancomycin, fidaxomicin) and were randomized 1:1 to placebo or SER-109 groups. ECOSPOR IV was an open-label, single-arm study conducted at 72 US or Canadian sites including 263 participants with rCDI enrolled in 2 cohorts: (1) rollover participants from ECOSPOR III who experienced on-study recurrence diagnosed by toxin EIA (n = 29) and (2) participants with ≥1 CDI recurrence (diagnosed by PCR or toxin EIA), inclusive of the current episode (n = 234). In both studies, the investigational product was administered orally as 4 capsules over 3 consecutive days following symptom resolution after standard-of-care antibiotics. The primary efficacy end point was rCDI (recurrent toxin-positive diarrhea requiring treatment) through week 8. Other end points included CDI recurrence rates and safety through 24 weeks. Results: These 349 participants received at least 1 dose of SER-109 in ECOSPOR III or ECOSPOR IV (mean age 64.2; 68.8% female). Overall, 77 participants (22.1%) enrolled with their first CDI recurrence. Four participants received blinded SER-109 in ECOSPOR III followed by a second dose of open-label SER-109 in ECOSPOR IV. Overall, the proportion of participants who received any dose of SER-109 with rCDI at week 8 was 9.5% (33 of 349; 95% CI, 6.6 %–13.0%), and the CDI recurrence rate remained low through 24 weeks (15.2%, 53 of 349; 95% CI, 11.6%–19.4%), corresponding to sustained clinical response rates of 90.5% (95% CI, 87.0%–93.4%) and 84.8% (95% CI, 80.6%–88.4%), respectively (Fig. 1). Most rollover participants (25 of 29, 86.2%) were from the placebo arm; 13.8% had rCDI by week 8. Conclusions: In this integrated analysis, the rates of rCDI were low and durable in participants who received the investigational microbiome therapeutic SER-109, with sustained clinical response rates of 90.5% and 84.8% at weeks 8 and 24, respectively. These data further support the potential benefit of microbiome repair with SER-109 following antibiotics for rCDI to prevent recurrence in high-risk patients.
Financial support: This study was funded by Seres Therapeutics.
Disclosure: None
Utilizing vancomycin as secondary prophylaxis for the prevention of recurrent Clostridioides difficile infection
- Zeitler Kristen, Andrew Nguyen, Candice Mateja, Ripal Jariwala, Carlos Bertran-Rodriguez, Cynthia Mayer, Diep Nguyen, Mindy Sampson
-
- Published online by Cambridge University Press:
- 29 September 2023, p. s5
-
- Article
-
- You have access Access
- Open access
- Export citation
-
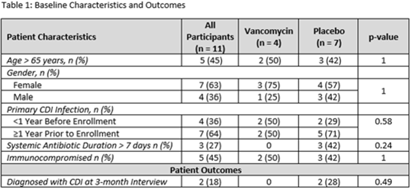
Background: Recurrent Clostridioides difficile infection (CDI) is associated with significant morbidity, mortality, and healthcare-related costs. Although data are minimal, agents including oral vancomycin have been used as secondary prophylaxis to prevent recurrent CDI. Methods: We conducted a randomized, double-blind, placebo-controlled trial to determine the effectiveness of vancomycin at preventing CDI from October 2019 to September 2022. Eligible patients had a history of at least 1 episode of CDI and were receiving systemic antibiotics for another condition. Participants were randomized 1:1 to oral vancomycin 125 mg by mouth twice daily and were interviewed at 1, 2, and 3 months thereafter to assess recurrence. We enrolled 26 patients: 15 completed the 1-month interview, 12 completed the 2-month interview, and 11 completed the full study. Those 15 participants who did not complete the 3-month interview were considered dropouts. The final sample for this study included those 11 participants who completed all interviews. Demographics and outcomes are shown in Table 1. Results: One case of recurrent CDI was reported at the 1-month interview and a second was reported at 3 months; both cases had received the placebo. The study was terminated early due to low enrollment. Conclusions: Although our results did not reach statistical significance and this study was limited in small sample size, our findings suggest that secondary prophylaxis with oral vancomycin may be beneficial in patients who are actively receiving antibiotics, which is consistent with prior retrospective studies. Future studies with larger sample sizes are still needed to examine this important question of whether secondary prophylaxis is useful for preventing recurrent CDI.
Disclosure: None
CLABSI
Relative risk of primary bloodstream infection in patients with mechanical circulatory support devices
- Rachel Wolansky, Patrick Burke, Ryan Miller, Thomas Fraser
-
- Published online by Cambridge University Press:
- 29 September 2023, p. s6
-
- Article
-
- You have access Access
- Open access
- Export citation
-
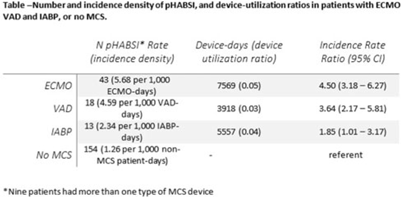
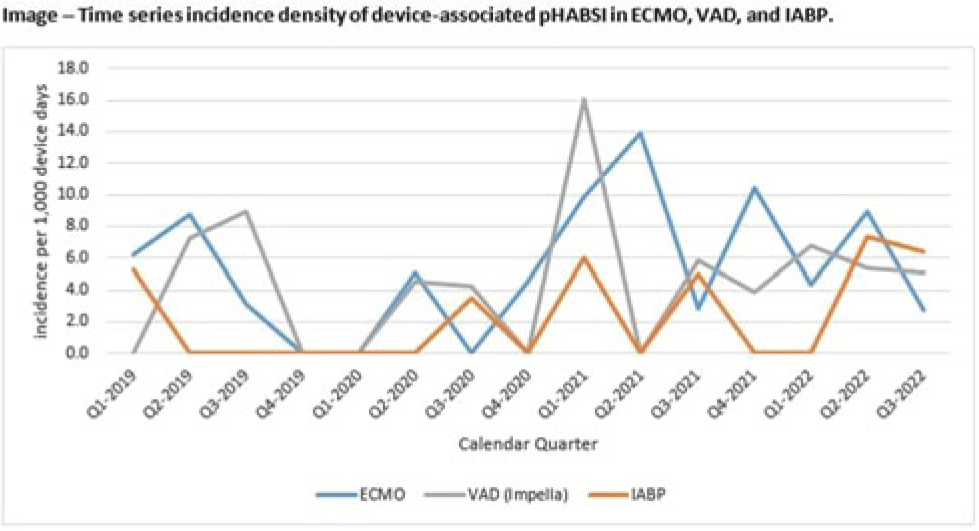
Background: Patients requiring mechanical circulatory support (MCS) during episodes of cardiogenic shock are at risk for hospital-acquired bloodstream infection (HABSI). Clinically MCS devices include extracorporeal membrane oxygenation (ECMO) devices, durable and temporary left ventricular-assist devices (VADs), and intra-aortic balloon pumps (IABPs). However, the MCS exclusion to the NHSN central-line–associated bloodstream infection (CLABSI) surveillance rules in 2018 did not include IABP as a qualifying device. We have described utilization and incidence of primary HABSI (pHABSI) in our patients requiring MCS. Methods: The setting for this study was 9 cardiothoracic and heart failure intensive care units with 131 total beds at the Cleveland Clinic Main Campus. Surveillance for HABSI to include determination of CLABSI was performed prospectively. MCS-associated pHABSI were patients who had ECMO, LVAD, or IABP present for >2 calendar days with device in place on the date of infection or removed the day before. A patient with 2 device types at time of infection was counted as a pHABSI for both groups. Patient, device, and MCS days were extracted from an electronic database. Non-MCS patient days were calculated as the difference between total patient days and total MCS days. The incidence of ECMO-, VAD-, and IABP-associated pHABSI were compared to each other and to non–MCS-associated pHABSI using OpenEpi version 3.01 software. Results: Surveillance results are shown in Table 1. During the observation period, there were 221 pHABSIs and 139,013 patient days. Moreover, 67 pHABSIs were associated with an MCS device over 17,044 total MCS days: 43 ECMO days, 18 VAD days, and 13 IABP days. Also, 9 patients had >1 type of eligible device and 7 (39%) of the IABP-associated pHABSIs were CLABSIs.
The cumulative incidences of pHABSI associated with ECMO, VAD, and IABP were 5.68, 4.59, and 2.34 per 1,000 MCS days, respectively. The incidence of IABP pHABSI was not significantly different from VAD pHABSI (P = .06), but it was different from ECMO pHABSI (P < .01). The pHABSI rate for non-MCS days was 1.26 per 1,000 patient days. Conclusions: In our patients requiring MCS, the risk of pHABSI associated with IABP was significantly greater than in patients without MCS and was similar to patients with VAD. MCS of all types should be considered a risk for HABSI in patients with cardiogenic shock beyond the presence of a central line. Protocols to further prevent HABSI morbidity in IABP patients are needed.
Disclosure: None
COVID-19
Healthcare personnel at non–acute-care facilities are at risk of COVID-19 from workplace and community exposures
- Armaghan-e-Rehman Mansoor, Caroline O’Neil, David McDonald, Victoria Fraser, Hilary Babcock, Jennie Kwon
-
- Published online by Cambridge University Press:
- 29 September 2023, p. s6
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Healthcare personnel (HCP) working in non–acute-care facilities are at high risk of COVID-19. We sought to determine SARS-CoV-2 seroprevalence, and analyzed behaviors and activities related to COVID-19 acquisition in this cohort. Methods: Between May and June 2021, HCP were enrolled at a skilled nursing facility and a memory care facility in St. Louis, Missouri. Data regarding demographics, prior SARS-CoV-2 testing, symptoms consistent with COVID-19 in the previous 6 months, COVID-19 vaccination, personal protective equipment (PPE) use, and COVID-19 exposures were collected via survey. Blood specimens were obtained to determine SARS-CoV-2 nucleocapsid IgG antibody seroprevalence (Abbott Laboratories). Study protocol was approved by the Washington University Institutional Review Board. Results: The survey was completed by 74 HCP. 82% of participants were female, and 31% reported >10 years of healthcare experience. The overall SARS-CoV-2 seropositivity rate was 8.9% (5 HCP). Of the surveyed HCP, 50% reported symptoms concerning for COVID-19 in the prior 6 months. Headache (38%), fatigue (35%) and fever (27%) were the most common self-reported symptoms. Among symptomatic HCP, only 35% sought medical care for these symptoms. All HCP reported having taken at least 1 COVID-19 test prior to study enrollment. Of note, 18.9% (14 HCP) had a self-reported prior positive SARS-CoV-2 PCR test, of whom 9 HCP were seronegative. All seronegative HCP with a self-reported history of COVID-19 reported infection >3 months before study participation. Completion of a primary COVID-19 vaccination series was reported by 86% of HCP. Known exposure to COVID-19 at work was reported by 28% of HCP. When asked about PPE at the time of workplace exposure, N95 mask use was reported by 81%, gloves by 57%, gowns by 33%, face shields by 29% and surgical masks by 14%. Known specific exposure to COVID-19 outside work was reported by 31% of HCP. Conclusions: One year after the initial COVID-19 pandemic impacted the St. Louis region, HCP at non–acute-care facilities had a SARS-CoV-2 seroprevalence of 8.9%. Similar frequency of exposures were reported from both the workplace and community, with high rates of PPE use at the workplace. HCP in such settings remain at high risk of COVID-19 exposure from workplace and community exposures. Ongoing efforts are needed to maintain PPE use to prevent SARS-CoV-2 transmission within non–acute-care facilities, and continue access to timely COVID-19 screening for HCP.
Disclosure: None
Low infectivity among asymptomatic patients with a positive SARS-CoV-2 admission test at a tertiary-care center, 2020–2022
- Ralph Tayyar, Melanie Kiener, Jane W. Liang, Gustavo Contreras Anez, Guillermo Rodriguez Nava, Alex Zimmet, Caitlin A. Contag, Krithika Srinivasan, Lucy Tompkins, Aruna Subramanian, John Shepard, Benjamin A. Pinsky, Jorge Salinas
-
- Published online by Cambridge University Press:
- 29 September 2023, p. s7
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Many hospitals have implemented admission SARS-CoV-2 testing to evaluate for the need for transmission-based precautions. However, a positive test in an asymptomatic patient may represent (1) active infection, signifying infectiousness; (2) false positivity; or (3) past infection with prolonged viral shedding. We used a strand-specific SARS-CoV-2 reverse real-time polymerase chain reaction (rRT-PCR) assay to assess infectivity among asymptomatic patients with a positive SARS-CoV-2 PCR admission test. Methods: We used a 2-step rRT-PCR specific to the minus strand of the SARS-CoV-2 envelope gene. We reviewed records of patients with a positive SARS-CoV-2 PCR who were also tested for the strand-specific SARS-CoV-2 PCR within 2 days of admission at Stanford Health Care during July 2020–April 2022. We restricted our analysis to each patient’s first test. We calculated the percentage of detectable minus strand-specific tests among asymptomatic patients over time and gathered descriptive statistics for age, sex, and immunocompromised state. Results: In total, 848 admitted patients had strand-specific SARS-CoV-2 assays performed. Of 532 patients with a strand-specific assay done within 2 days of admission, 242 (45%) were asymptomatic. Among asymptomatic patients, the mean age was 56 years (range, 19–99), 133 (55%) were male, 50 (21%) had immunocompromising conditions, and 30 (12%) were admitted for a surgical procedure. In total, 21 (9%; range, 4%–25% per quarter) had detectable minus strand-specific assays (Fig. 1). Conclusions: Most asymptomatic patients tested for SARS-CoV-2 on admission were not infectious. Hospitals using SARS-CoV-2 PCR admission testing may need to re-evaluate the continued use of this practice.
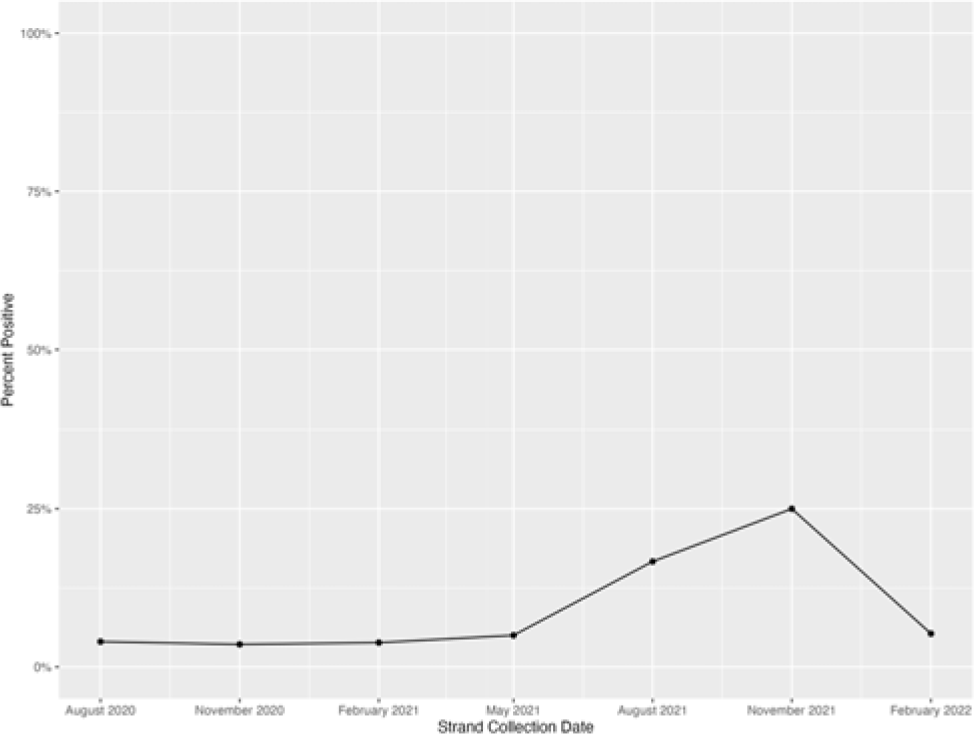
Fig. 1. Minus strand-specific SARS-CoV-2 assay percentage positivity per quarter among asymptomatic patients tested within 2 days of admission. The peak positivity in November 2021–January 2022 quarter coincided with the SARS-CoV-2 omicron variant surge in our county.
Disclosure: None
Hospital-onset COVID-19: Associations with population- and hospital-level measures to guide infection prevention efforts
- Emily Schmitz, Laura Anderson, Gabrielle Hatas, Marin Schweizer, Nasia Safdar, Daniel Shirley
-
- Published online by Cambridge University Press:
- 29 September 2023, p. s7
-
- Article
-
- You have access Access
- Open access
- Export citation
-
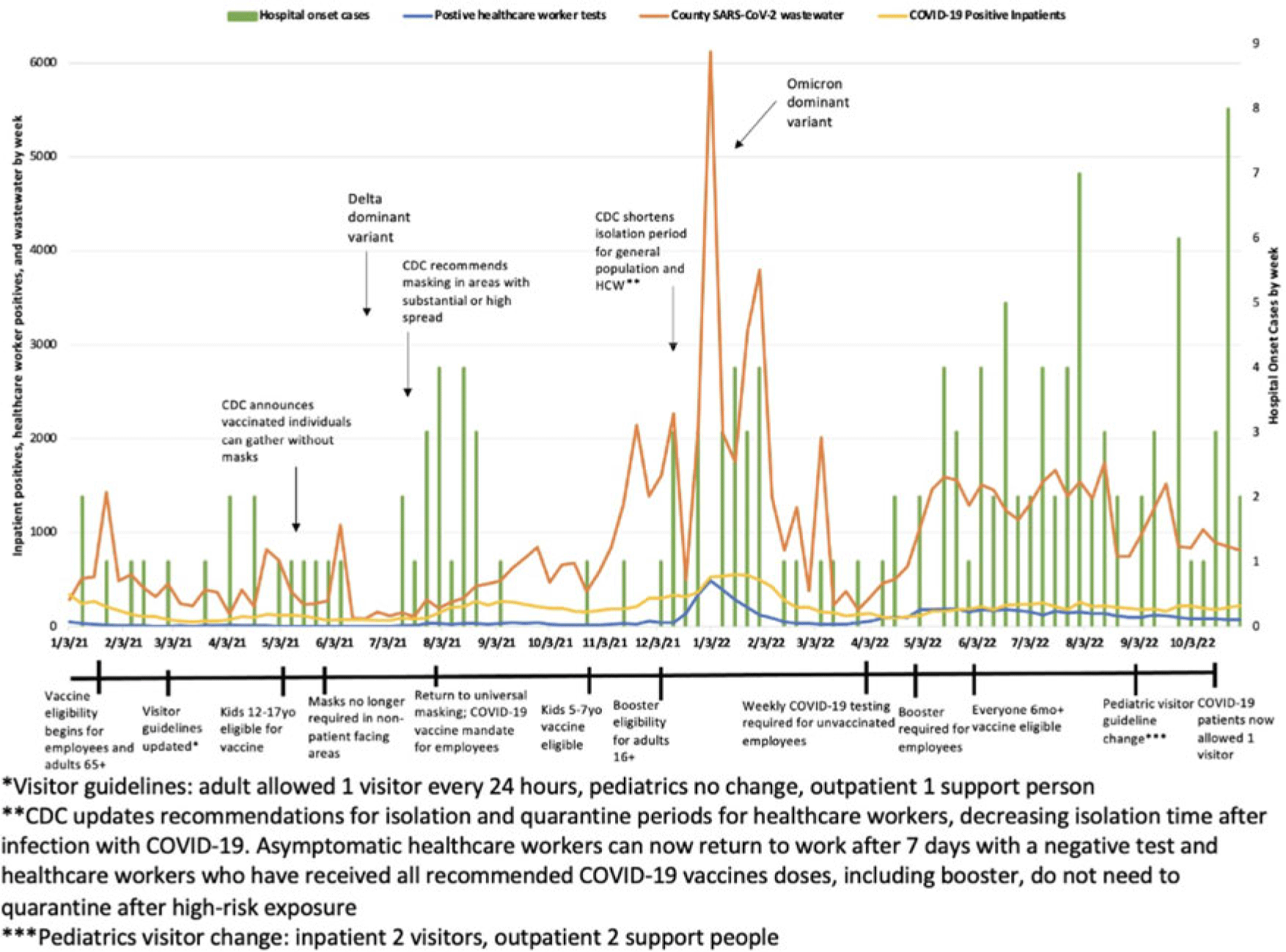
Objective: To characterize hospital-onset COVID-19 cases and to investigate the associations between these rates and population and hospital-level rates including trends in healthcare worker infections (HCW), community cases, and COVID-19 wastewater data. Design: Retrospective cohort study from January 1, 2021, to November 23, 2022. Setting: This study was conducted at a 589-bed urban Midwestern tertiary-care hospital system. Participants and interventions: The infection prevention team reviewed the electronic medical records (EMR) of patients who were admitted for >48 hours and subsequently tested positive for SARS-CoV-2 to determine whether COVID-19 was likely to be hospital-onset illness. Each case was further categorized as definite, probable, or possible based on viral sequencing, caregiver tracing analysis, symptoms, and cycle threshold values. Patients were excluded if there was a known exposure prior to admission. Clinical data including vaccination status were collected from the EMR. HCW case data were collected via our institution’s employee health services. Community cases and wastewater data were collected via the Wisconsin Department of Health Services database. Additionally, we evaluated the timing of changes in infection prevention guidance such as visitor restrictions. Results: In total, 156 patients met criteria for hospital-onset COVID-19. Overall, 6% of cases were categorized as definite, 24% were probable, and 70% were possible hospital-onset illness. Most patients were tested prior to a procedure (31%), for new symptoms (30%), and for discharge planning (30%). Also, 53% were symptomatic and 41% received treatment for their COVID-19. Overall, 38% of patients were immunocompromised and 27% were unvaccinated. Overall, 12% of patients died within 1 month of their positive SARS-CoV-2 test, and 11% required ICU admission during their hospital stay. Hospital-onset COVID-19 increased in fall of 2022. Specifically, October 2022 had 16 cases, whereas fall of 2021 (September–November) only had 3 cases total. Finally, similar peaks were observed in total cases by week between healthcare workers, county cases, and COVID-19 wastewater levels. These peaks correspond with the SARS-CoV-2 delta and omicron variant surges, respectively. Conclusions: Hospital-onset cases followed similar trends as population and hospital-level data throughout the study period. However, hospital-onset rate did not correlate as strongly in the second half of 2022 when cases were disproportionately high. Given that hospital-onset cases can result in significant morbidity, continued enhanced infection prevention efforts and low threshold for testing are warranted in the inpatient environment.
Disclosure: None
Decolonization Strategies
Effectiveness of a Staphylococcus aureus mupirocin decolonization protocol in a neonatal intensive care unit
- Andrea Ankrum, Felicia Scaggs Huang, Joshua Schaffzin
-
- Published online by Cambridge University Press:
- 29 September 2023, p. s8
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Staphylococcus aureus infections are a significant cause of morbidity in neonatal intensive care units (NICUs), and they are typically preceded by nasal colonization. Mupirocin decolonization protocols as an infection prevention tool can halt S. aureus outbreaks and prevent infections. We examined the effect of a mupirocin treatment protocol on S. aureus incidence, prevalence, decolonization, and infections in a level IV NICU. Methods: We conducted a retrospective before-and-after observational study from June 1, 2018, to May 31, 2020. Beginning June 1, 2019, patients identified with either methicillin-sensitive or -resistant S. aureus (MSSA or MRSA) received mupirocin ointment to bilateral nares 3 times daily for 5 days. Patients with central lines or surgical incisions were treated every 30 days. All NICU patients were screened weekly unless positive for MRSA. We defined MSSA decolonization as 3 consecutive negative screens following mupirocin treatment. We calculated monthly S. aureus incidence as any new positive per 1,000 patient days and monthly prevalence as a percentage of the average daily number of patients with S. aureus per the average monthly census. Total number of infections were compared. Statistical significance was determined using a 2 sample proportions test and P < .05. Decolonization was calculated as percentage of occurrences among treated patients. Results: Overall, 190 patients received mupirocin; 142 patients received 1 course and 48 received 2 or more courses. There was no difference in incidence of MSSA (P = .09), but prevalence decreased from 18.8% to 14.4% (P < .05) (Fig. 1). Of 66 patients with MSSA, 35% were decolonized. An additional mupirocin treatment for 16 of these patients had a 50% decolonization rate. For MRSA, incidence decreased from 0.24 to 0.20 (P = .36) and prevalence decreased from 21.9% to 18.6% (P < .05) (Fig. 1). There was no statistical difference in the number of total S. aureus infections (P = .91) or when stratified by MSSA (P = .72) or MRSA (P = .82). In the postmupirocin population, there were 5 MRSA and 7 MSSA infections. Of the MSSA-infected patients, 6 remained colonized at the time of infection. Conclusions: Implementing a single mupirocin treatment course for S. aureus decolonization in NICU was only effective in one-third of patients and had no effect on infection occurrence. Changes in incidence and prevalence could be confounded by other infection prevention practices. Further study is needed to determine whether continued screening and additional mupirocin treatment could improve effectiveness of S. aureus decolonization programs.
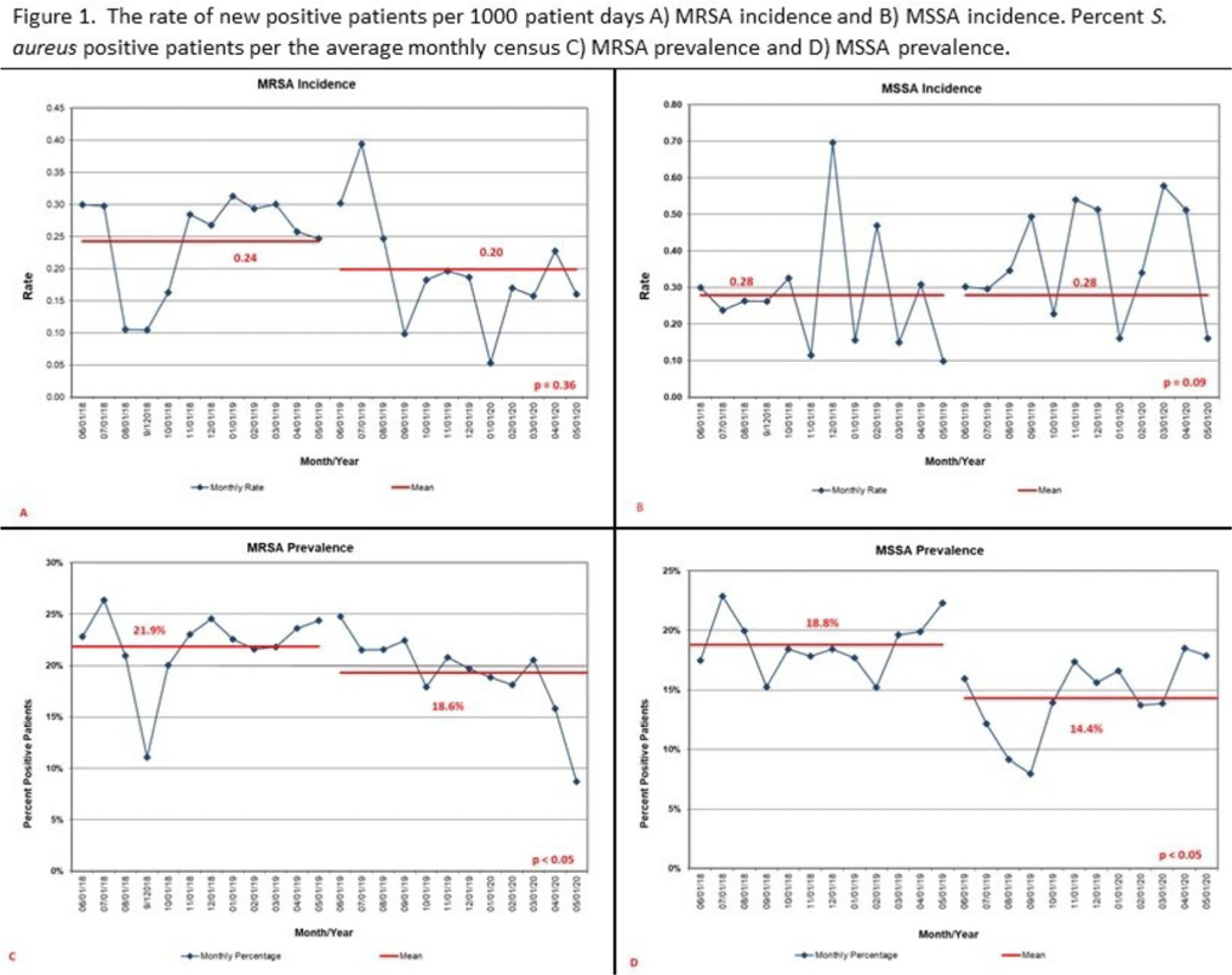
Disclosure: None
Diagnostic/Microbiology
Implementation of diagnostic stewardship in two surgical ICUs: Time for a blood-culture change
- Jessica Seidelman, Rebekah Moehring, Erin Gettler, Jay Krishnan, Christopher Polage, Margaret Murphy, Rachel Jordan, Sarah Lewis, Becky Smith, Deverick Anderson, Nitin Mehdiratta
-
- Published online by Cambridge University Press:
- 29 September 2023, pp. s9-s10
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Blood cultures are commonly ordered for patients with low risk of bacteremia. Liberal blood-culture ordering increases the risk of false-positive results, which can lead to increased length of stay, excess antibiotics, and unnecessary diagnostic procedures. We implemented a blood-culture indication algorithm with data feedback and assessed the impact on ordering volume and percent positivity. Methods: We performed a prospective cohort study from February 2022 to November 2022 using historical controls from February 2020 to January 2022. We introduced the blood-culture algorithm (Fig. 1) in 2 adult surgical intensive care units (ICUs). Clinicians reviewed charts of eligible patients with blood cultures weekly to determine whether the blood-culture algorithm was followed. They provided feedback to the unit medical directors weekly. We defined a blood-culture event as ≥1 blood culture within 24 hours. We excluded patients aged <18 years, absolute neutrophil count <500, and heart and lung transplant recipients at the time of blood-culture review. Results: In total, 7,315 blood-culture events in the preintervention group and 2,506 blood-culture events in the postintervention group met eligibility criteria. The average monthly blood-culture rate decreased from 190 blood cultures per 1,000 patient days to 142 blood cultures per 1,000 patient days (P < .01) after the algorithm was implemented. (Fig. 2) The average monthly blood-culture positivity increased from 11.7% to 14.2% (P = .13). Average monthly days of antibiotic therapy (DOT) was lower in the postintervention period than in the preintervention period (2,200 vs 1,940; P < .01). (Fig. 3) The ICU length of stay did not change before the intervention compared to after the intervention: 10 days (IQR, 5–18) versus 10 days (IQR, 5–17; P = .63). The in-hospital mortality rate was lower during the postintervention period, but the difference was not statistically significant: 9.24% versus 8.34% (P = .17). The all-cause 30-day mortality was significantly lower during the intervention period: 11.9% versus 9.7% (P < .01). The unplanned 30-day readmission percentage was significantly lower during the intervention period (10.6% vs 7.6%; P < .01). Over the 9-month intervention, we reviewed 916 blood-culture events in 452 unique patients. Overall, 74.6% of blood cultures followed the algorithm. The most common reasons overall for ordering blood cultures were severe sepsis or septic shock (37%), isolated fever and/or leukocytosis (19%), and documenting clearance of bacteremia (15%) (Table 1). The most common indications for inappropriate blood cultures were isolated fever and/or leukocytosis (53%). Conclusions: We introduced a blood-culture algorithm with data feedback in 2 surgical ICUs and observed decreases in blood-culture volume without a negative impact on ICU LOS or mortality rate.
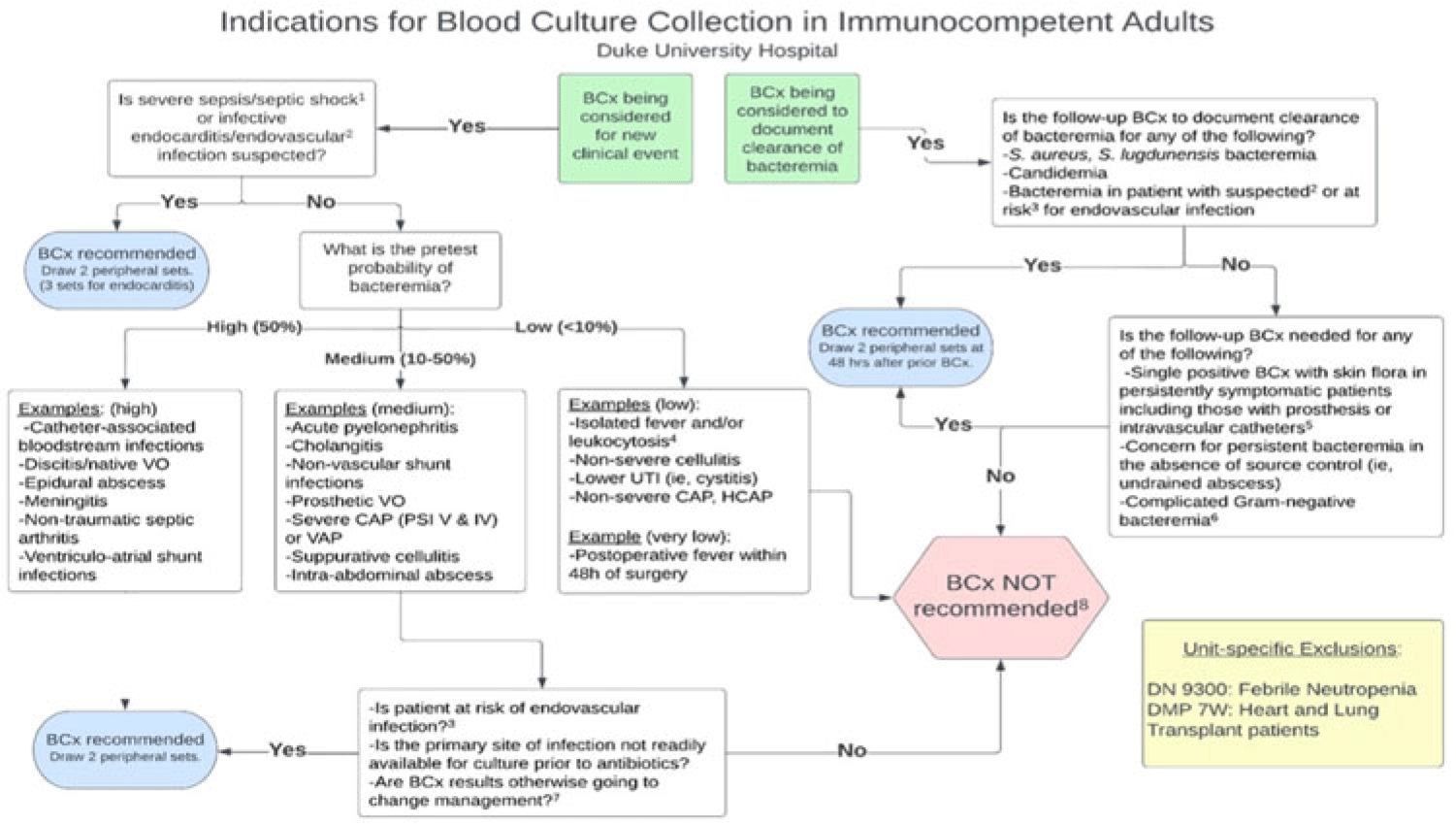
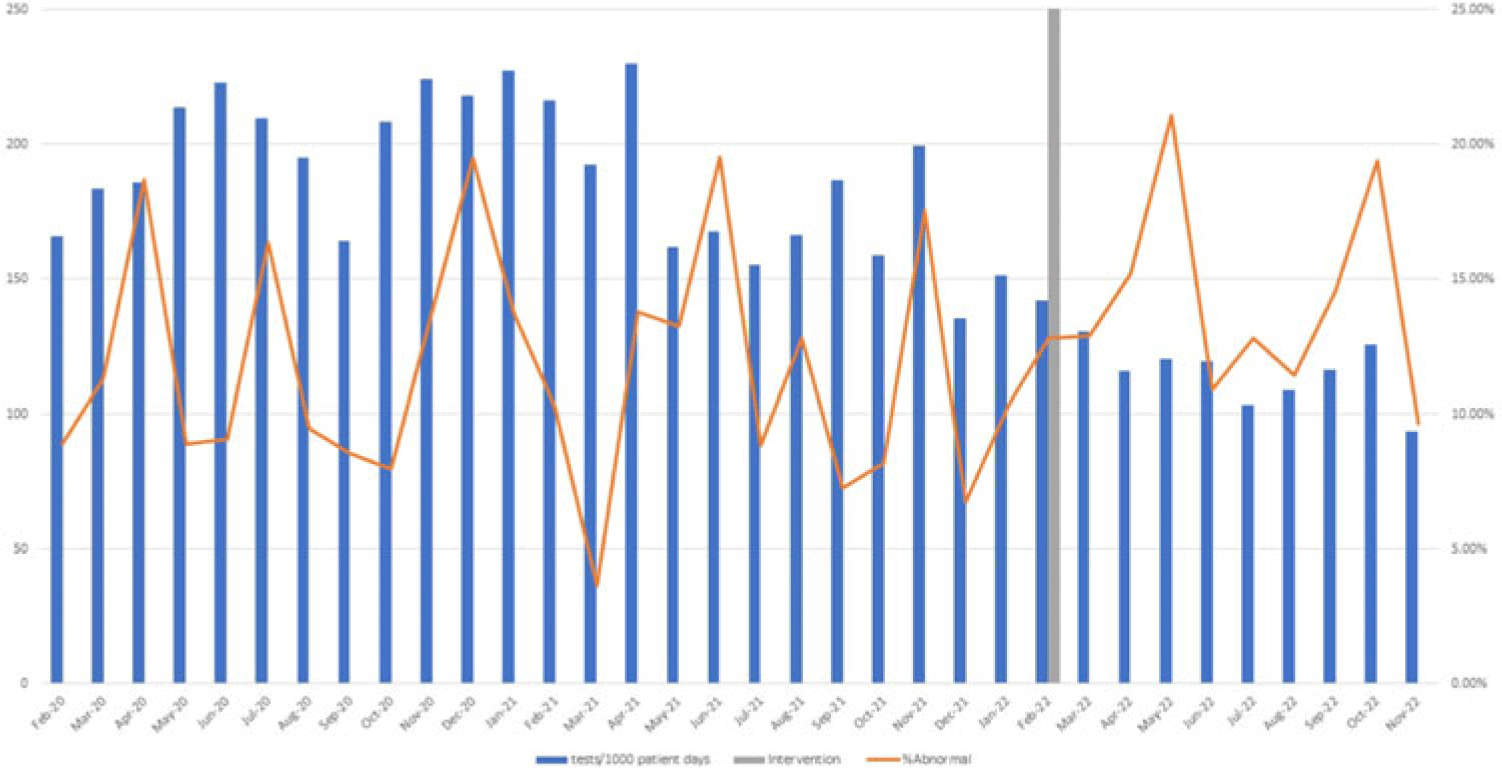
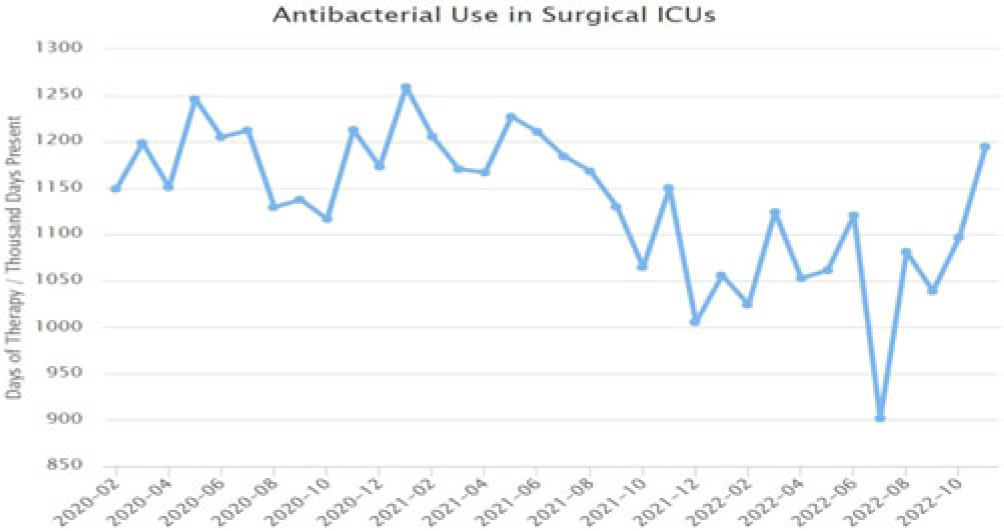
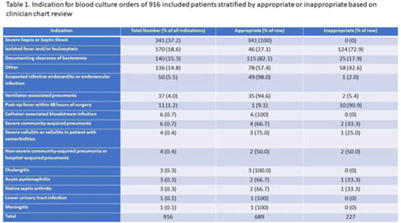
Disclosure: None
Emerging Pathogens
Alarming prevalence of Candida auris among critically ill patients in intensive care units in Dhaka City, Bangladesh
- Fahmida Chowdhury, Kamal Hussain, Sanzida Khan Khan, Dilruba Ahmed, Debashis Sen, Zakiul Hassan, Mahmudur Rahman, Sajeda Prema, Alex Jordan, Shawn Lockhart, Meghan Lyman, Syeda Mah-E-Muneer
-
- Published online by Cambridge University Press:
- 29 September 2023, p. s11
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Candida auris is a multidrug-resistant yeast capable of invasive infection with high mortality and healthcare-associated outbreaks globally. Due to limited labratory capacity, the burden of C. auris is unknown in Bangladesh. We estimated the extent of C. auris colonization and infection among patients in Dhaka city intensive care units. Methods: During August 2021–September 2022 at adult intensive care units (ICUs) and neonatal intensive care units (NICUs) of 1 government and 1 private tertiary-care hospital, we collected skin swabs from all patients and blood samples from sepsis patients on admission, mid-way through, and at the end of ICU or NICU stays. Skin swab and blood with growth in blood-culture bottle were inoculated in CHROMagar, and identification of isolates was confirmed by VITEK-2. Patient characteristics and healthcare history were collected. We performed descriptive analyses, stratifying by specimen and ICU type. Results: Of 740 patients enrolled, 59 (8%) were colonized with C. auris, of whom 2 (0.3%) later developed a bloodstream infection (BSI). Among patients colonized with C. auris, 27 (46%) were identified in the ICU and 32 (54%) were identified from the NICU. The median age was 55 years for C. auris–positive ICU patients and 4 days for those in the NICU. Also, 60% of all C. auris patients were male. Among 366 ICU patients, 15 (4%) were positive on admission and 12 (3%) became colonized during their ICU stay. Among 374 NICU patients, 19 (5%) were colonized on admission and 13 (4%) became colonized during their NICU stay. All units identified C. auris patients on admission and those who acquired it during their ICU or NICU stay, but some differences were observed among hospitals and ICUs (Figure). Among patients colonized on admission to the ICU, 11 (73%) were admitted from another ward, 3 (20%) were admitted from another hospital, and 1 (7%) were admitted from home. Of patients colonized on admission to the NICU, 4 (21%) were admitted from the obstetric ward, 9 (47%) were admitted from another hospital, and 6 (32%) were admitted from home. In addition, 18 patients with C. auris died (12 in the ICU and 6 in the NICU); both patients with C. auris BSIs died. Conclusions: In these Bangladesh hospitals, 8% of ICU or NICU patients were positive for C. auris, including on admission and acquired during their ICU or NICU stay. This high C. auris prevalence emphasizes the need to enhance case detection and strengthen infection prevention and control. Factors contributing to C. auris colonization should be investigated to inform and strengthen prevention and control strategies.
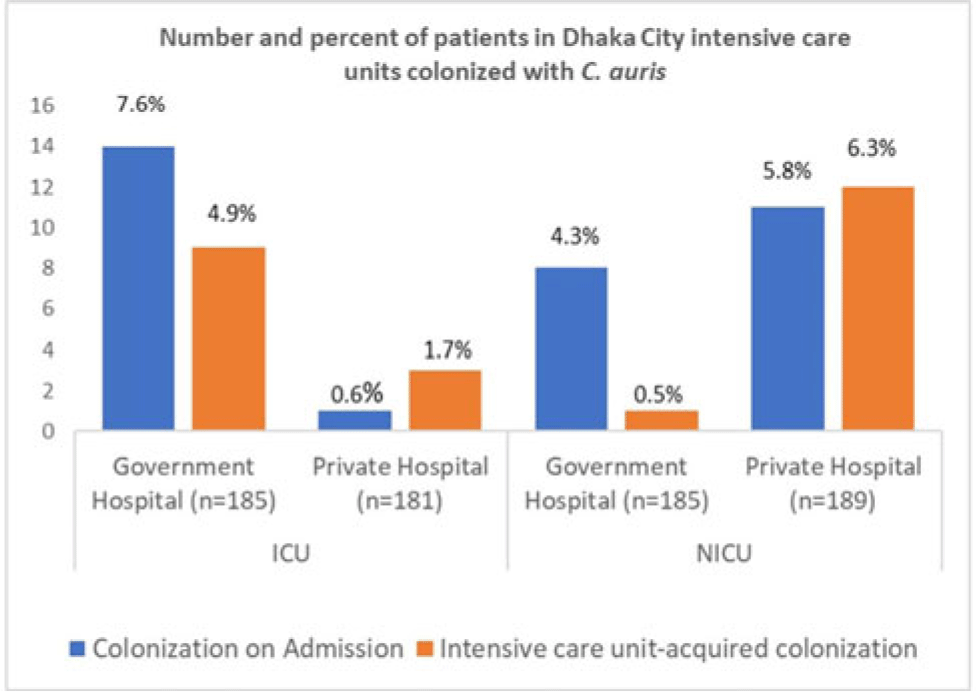
Disclosure: None
Environmental Cleaning
Modifying water use practices to eliminate Pseudomonas aeruginosa bloodstream infections in the neonatal intensive care unit
- Ingrid Camelo, Srilatha Neshangi, Amy Thompson
-
- Published online by Cambridge University Press:
- 29 September 2023, p. s11
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Objective: To describe the strategies implemented at a tertiary-care healthcare center neopnatal intensive care unit (NICU) to control and assure prevention of subsequent central-line bloodstream infections (CLABSIs) with Pseudomonas aeruginosa after 4 cases of CLABSI with this organism were detected. Methods: During the months of September 2020 to February 2021, 4 cases of CLABSI with Pseudomonas aeruginosa were reported in our NICU in patients meeting criteria for extremely low birthweight (ELBW) infants. All patients were treated according to IDSA guidelines for management of bloodstream infections. To avoid the appearance of new events and to improve existing policies, we implemented a stepwise approach by reviewing routine disinfection and/or cleaning procedures of isolettes: (1) liners for bath basins were applied, (2) sterile water was provided for bathing newborns, (3) we ensured timely biomed preventive maintenance of water reservoirs for patient care equipment (nebulizers, isolettes and fluid warmers), and (4) we implemented the installment of point-of-care filters for tap water. Results: Measures were implemented from February 2021 to July 2021. During the following year from July 2021 to June 2022, no CLBSIs related to Pseudomonas aeruginosa were reported in our NICU in patients meeting criteria for ELBW infants. Conclusions: Recognition of CLABSI from organisms from water resources is important to implementing focused prevention strategies targeting water resources and water utilization practices. In our institution, these interventions yielded complete resolution, with no new infection events.
Disclosure: None
Infection Control in Low and Middle-Income Countries
Approach for sustainable district-led production and distribution of alcohol-based hand rub in Uganda
- Maureen Kesande
-
- Published online by Cambridge University Press:
- 29 September 2023, pp. s11-s12
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: A sustainable, continuous supply of alcohol-based hand rub (ABHR) is essential for healthcare workers in health facilities. The WHO provides guidance for production in individual health facilities. In Uganda, using this guidance, an innovative approach was implemented at the district local government level to produce and subsequently distribute ABHR to primary-care health facilities that have limited capacity for local facility-level production. This project was supported by the CDC in collaboration with the Infectious Diseases Institute (IDI) and targeted governmental or district engagement with local partners to ensure sustainability. Methods: District stakeholders were engaged to obtain buy-in and define roles and responsibilities. Overall, 4 staff members in each of 6 supported districts were nominated by District Health Officers for training: 2 staff members were trained to produce ABHR and conduct internal quality control and 2 were trained on external quality control. Districts provided ABHR production-unit facilities and facilitated integration within the government essential supplies delivery system, National Medical Stores in Uganda, which supports last-mile delivery to facilities. An implementing partner purchased initial raw materials necessary for production. The cost of materials for local production was compared to the price of commercial ABHR available in Uganda. Results: Between January and August 2021, 23 staff members were trained, and 380 batches of quality-assured ABHR (17,820 L) were produced and distributed to 278 health facilities. Consumption of ABHR in the first distribution was used to benchmark predicted ABHR consumption per targeted facility in subsequent months. Increased demand for ABHR due to the COVID-19 pandemic and the Ebola virus disease outbreak in central Uganda (September 2022) was addressed through emergency requests on a case-by-case basis. ABHR local production costs $3 per liter for materials, less than half of commercial ABHR ($8 per liter). Conclusions: Early results suggest that this approach is potentially sustainable but requires national advocacy as well. Leveraging existing distribution systems while building local capacity for ABHR production and distribution may improve longevity of such innovations in similar resource-limited settings.
Disclosure: None
Infection Control in Low- and Middle-Income Countries
Assessment of ventilation in low-resource healthcare settings: Montserrado County, Liberia—2022−2023
- Krithika Srinivasan, Ronan Arthur, Ashley Styczynski, Ethan Bell, Thomas Baer, Jorge Salinas
-
- Published online by Cambridge University Press:
- 29 September 2023, p. s12
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Mitigating the risk of nosocomial respiratory disease transmission in the healthcare facilities of low- and middle−income countries (LMICs) poses unique challenges because mechanical ventilation and mixed−mode strategies are often unavailable. Carbon dioxide (CO2) can serve as a proxy for ventilation and, hence, airborne infectious disease transmission risk in naturally ventilated spaces. We assessed the adequacy of ventilation in Liberian hospitals. Methods: We sampled 3 hospitals, both urban and rural, in Montserrado County, Liberia. Moreover, 3 CO2 meters were concurrently utilized to measure CO2 levels at a 1-meter height in every patient-care room in each facility. We recorded temperature, humidity, room dimensions, and number of people in the rooms. From these variables, we calculated absolute ventilation using the ASHRAE equation to determine areas with the highest risk of nosocomial respiratory disease transmission. We also recorded qualitative observations about the sampled spaces. Results: From August 2022 to February 2023, 39 rooms in 3 healthcare facilities were sampled. Initial quantitative findings show that only 8 rooms (21%) met the WHO-recommended ventilation rate of 60 L per second per person. The average ventilation rate per person in the adequately ventilated settings was 86 L per second per patient, compared to 19 liters per second per patient in inadequately ventilated rooms. Additionally, 467 ppm mean CO2 was noted in well-ventilated rooms compared to 895 ppm mean CO2 in inadequately ventilated rooms.
Initial qualitative observations showed that facilities with lower CO2 readings tended to be older constructions that likely had been constructed with airborne disease such as tuberculosis in mind. Willingness to open windows was limited by lack of window screens for malaria prevention, and there was a pervasive fallacy that air conditioning was a source of ventilation. Correspondingly, of the 31 inadequately ventilated rooms, 22 (71%) had operating air conditioning units compared with 4 (50%) of the 8 adequately ventilated rooms. Overall, of the 13 rooms without air conditioning, 7 (54%) were more frequently characterized by open windows compared to only 5 of 26 (28%) of rooms that did have air conditioners. Conclusions: Being prepared for the next respiratory disease outbreak and creating more resilient healthcare systems in LMICs requires a frameshift of prevention strategies. Measuring CO2 provides a simple strategy for identifying areas at highest risk for nosocomial respiratory disease transmission, which can be prioritized for low-cost environmental interventions, such as provision of window screens, as part of routine infection prevention and control efforts.
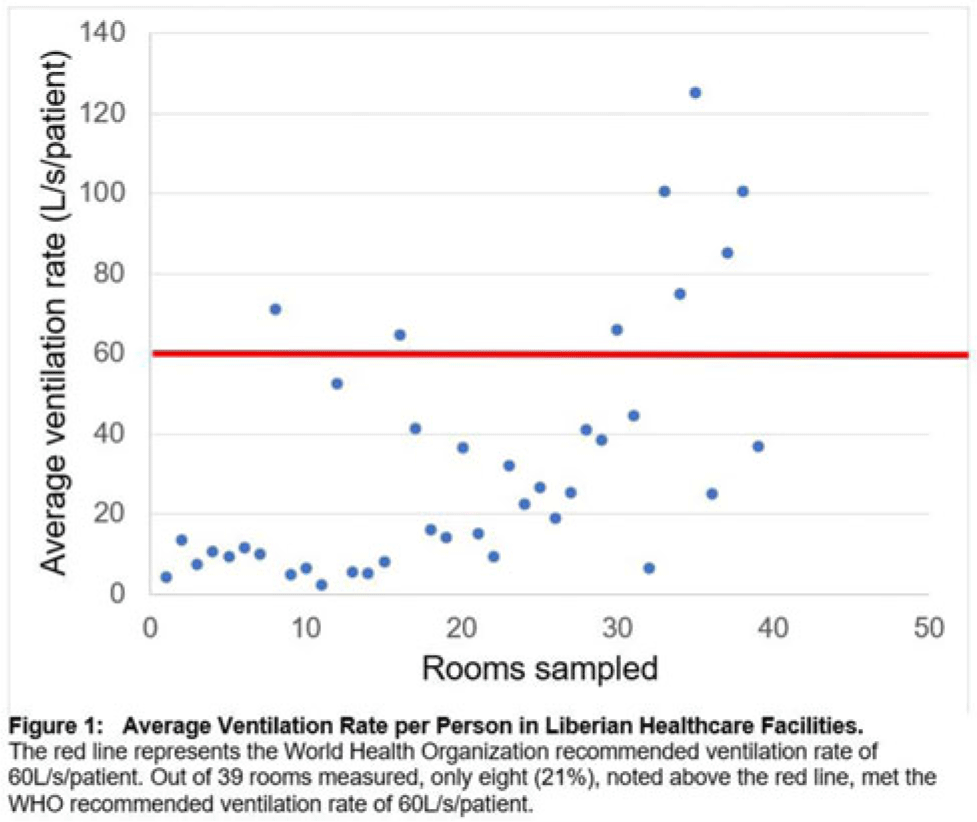
Disclosure: None
MDR GNR
Carbapenemase genes and mortality in patients with carbapenem-resistant Enterobacterales, Atlanta, Georgia, 2011–2020
- Lucy Witt, Ahmed Babike, Gillian Smith, Sarah Satola, Mary Elizabeth Sexton, Jesse Jacob
-
- Published online by Cambridge University Press:
- 29 September 2023, pp. s12-s13
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Carbapenemase genes in carbapenem-resistant Enterobacterales (CP-CRE) may be transmitted between patients and bacteria. Reported rates of carbapenemase genes vary widely, and it is unclear whether having a carbapenemase gene portends worse outcomes given that all patients with CRE infections have limited treatment options. Methods: Using active population- and laboratory-based active surveillance data collected by the US CDC-funded Georgia Emerging Infections Program from 2011 to 2020, we assessed the frequency of carbapenemase genes in a convenience sample of CRE isolates using whole-genome sequencing (WGS), and we investigated risk factors for carbapenemase positivity. Only the first isolate per patient in a 30-day period was included. We compared characteristics of patients with CP-CRE and non–CP-CRE. Using multivariable log binomial regression, we assessed the association of carbapenemase gene positivity and 90-day mortality. Results: Of 284 CRE isolates, 171 isolates (60.2%) possessed a carbapenemase gene (Table 1), and KPC-3 was the most common carbapenemase gene (80.7%), with only 7 isolates possessing NDM (Table 2). No isolates possessed >1 carbapenemase gene, and most isolates were from urine (82.4%) (Table 1). Carbapenemase gene positivity was associated with lower age, male sex, black race, infection with Klebsiella pneumoniae, polymicrobial infection, having an indwelling medical device, receiving chronic dialysis, and prior stay in a long-term acute-care hospital, long-term care facility, and/or prior hospitalization in the last year. The 90-day mortality rates were similar in patients with non–CP-CRE and CP-CRE: 24.8% versus 25.7% (P = .86). In multivariable analysis, carbapenemase gene presence was not associated with 90-day mortality (adjusted risk ratio, 0.82; 95% CI, 0.50–1.35) when adjusting for CCI, infection with Klebsiella pneumoniae, and chronic dialysis use. Conclusions: The frequency of CP-CRE among CRE was high in this study, but unlike prior studies, the 90-day mortality rates wer similar in patients with CP-CRE compared to non–CP-CRE. Our results provide novel associations (eg, lower age, male sex, infection with Klebsiella pneumoniae, and indwelling medical devices) that infection preventionists could use to target high-risk patients for screening or isolation prior to CP-CRE detection.
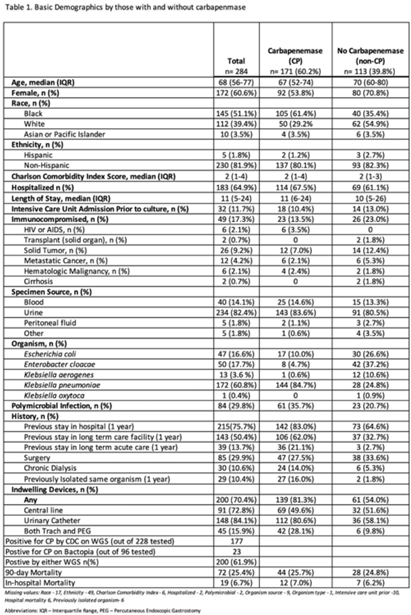
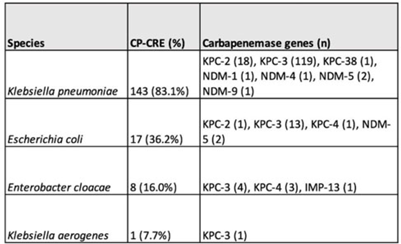
Disclosure: None
MRSA/VRE
Impact of discontinuation of contact precautions on surveillance- and whole-genome sequencing-defined MRSA infections
- Sharon Karunakaran, Lora Pless, Ashley Ayres, Carl Ciccone, Joseph Penzelik, Alexander Sundermann, Elise Martin, Marissa Griffith, Kady Waggle, Lee Harrison, Graham Snyder
-
- Published online by Cambridge University Press:
- 29 September 2023, pp. s13-s14
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Current guidelines recommend contact precautions to prevent transmission of methicillin-resistant Staphylococcus aureus (MRSA) in acute-care hospitals. Prior literature demonstrates that discontinuation of contact precautions for MRSA has not been associated with an increase in carriage rates including surveillance-defined healthcare-associated infection (HAI) while horizontal infection prevention strategies are implemented. Objective: To analyze the impact of discontinuation of contact precautions on the rate of MRSA infections, including surveillance-defined HAI and transmission events identified through whole-genome sequencing (WGS) surveillance. Methods: In this single tertiary-care center, retrospective, observational, quality improvement analysis, we measured 2 MRSA HAI outcomes before and after discontinuation of contact precautions (ie, gown and gloves no longer required for care of patients with prior or current MRSA infections or colonization, effective December 2, 2020). First, we conducted a time-series analysis using linear regression modelling of NHSN reported MRSA HAI rates (January 2019–November 2022). We also calculated the frequency of WGS-confirmed MRSA transmission events before in the discontinuation of contact precautions (January 2019–August 2019) and after the discontinuation of contact precautions (January 2022–November 2022) periods. Surveillance HAI events were determined using NHSN definitions; MRSA transmission events were defined as an isolate identified ≥3 days after hospitalization or within 30 days of a healthcare exposure, genetically related by ≤15 single-nucleotide polymorphisms compared to ≥1 previously sequenced MRSA isolate. Results: We identified 171 MRSA HAIs in the 23 months before discontinuation of contact precautions, corresponding to 4.24 HAI per 10,000 patient days, and 129 HAIs in the 24 months after discontinuation of contact precautions, corresponding to 3.01 HAI per 10,000 patient days (Fig.). We detected a nonsignificant change in the trend in HAI rate before and after discontinuation of contact precautions (P = .22) as well as a significant immediate decrease in the MRSA HAI rate (P < 0 .001) at the time of discontinuation of contact precautions. In the WGS analysis 8 months before discontinuation of contact precautions, 11 MRSA transmission events were confirmed, comprising 4 clusters (0.75 per 10,000 patient days). In the WGS for the 11-month analysis period after discontinuation of contact precautions, there were 23 confirmed MRSA transmission events comprising 10 clusters (1.22 per 10,000 patient days; incidence rate ratio, 1.61; 95% CI, 0.75–3.66; P = .19). Conclusions: After discontinuation of contact precautions, there was no significant increase in MRSA HAI or transmission events. Further evaluation of the individual WGS transmission clusters will be helpful to determine whether discontinuation of contact precautions led to MRSA transmission in this facility in the period after discontinuation of contact precautions.
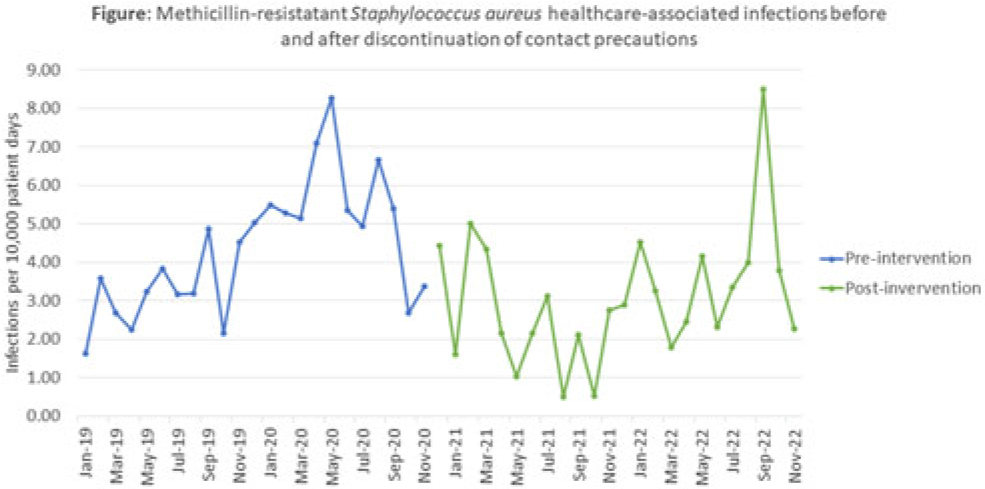
Disclosure: None



























