The high prevalence of overweight and obesity in childhood is unfortunate, since overweight children suffer from both short- and long-term health consequences( Reference Ebbeling, Pawlak and Ludwig 1 , Reference Reilly 2 ). Moreover, overweight in childhood and adolescence increases the risk of overweight in adulthood, which is associated with increased morbidity and risk of premature mortality( Reference Reilly 2 ). In Denmark( Reference Mølgaard, Dela and Froberg 3 ), as in most Western countries( Reference Shrewsbury and Wardle 4 ), the prevalence of overweight and obesity is highest among children of parents with low socio-economic status (SES).
Both physical activity and diet are believed to be important factors in the prevention of overweight and obesity among children. According to the results from the Danish National Dietary Survey, the general diet of Danish children (aged 4–14 years) does not comply with the official dietary recommendations. For the intakes of macronutrients, added sugar, dietary fibre and fatty acids, the recommendations are as follows: protein, 10–20 energy percentage (E%); fat, 25–35 E%; SFA, < 10 E%; MUFA, 10–15 E%; PUFA, 5–10 E%; carbohydrates, 50–60 E%; added sugar, < 10 E%; dietary fibre 25–35 g/d or 3 g/MJ (for adults) and >10 g/d at school age, gradually increasing to reach the recommended level during adolescence (for children)( 5 ).
The diet among Danish children is generally too high in fat and added sugar, and the content of dietary fibre does not show the recommended increase during school age( Reference Pedersen, Fagt and Groth 6 ). This is not ideal since consumption of energy-dense foods, due to a high fat and/or sugar content, may increase the risk of overweight( 7 ). Studies have moreover shown that children of parents with low SES have unhealthier eating habits compared with children of parents with high SES, including a lower intake of fruit and vegetables and a higher intake of sweets, soft drinks and fast food( Reference Cribb, Jones and Rogers 8 – Reference Stea, Overby and Klepp 12 ). This has also been reported among Danish adolescents (age >11 years)( Reference Rasmussen and Due 13 ), whereas a more recently published study including younger Danish children (aged 4–14 years) has found that the different eating habits according to SES are most pronounced among boys( Reference Groth, Christensen and Knudsen 14 ).
Public schools are one of the suggested arenas for introducing health-promoting initiatives among children( Reference Wechsler, Devereaux and Margarett 15 ), due to their potential to reach all children and adolescents independent of ethnicity and SES( Reference Van Cauwenberghe, Maes and Spittaels 16 ). Therefore, the Copenhagen School Child Intervention Study (CoSCIS) was initiated in 2001. It was based on the initiative of the municipality of Ballerup that intended to promote health and well-being among the local school children. The intervention focused on improving both dietary intake and physical activity among the children.
The aims of the present study were to examine the effect of intervention on the dietary intake and, more specifically to examine (1) the effect of CoSCIS on the dietary intake among children (macronutrients, fatty acids, added sugar and dietary fibre) and (2) whether the effects depended on parental SES (assessed as maternal education level).
We hypothesised that the children in the intervention group would change their diet in a more healthy direction (defined as closer to the dietary recommendations) as a consequence of the intervention, and that the effect would be greater among children of mothers with a long education.
Methods
Intervention
In 1999, all public schools (n 10) in Ballerup, a suburban municipality of Copenhagen, Denmark, introduced an initiative with the focus on improving health and well-being among the local school children( Reference Hasselstrom, Karlsson and Hansen 17 ). The intervention was multi-component (consisting of both classroom-based activities and environmental changes), and the components are briefly described below:
(1) Two additional physical education (PE) lessons per week: In all intervention schools, the two standard PE lessons per week (90 min) were increased to four PE lessons per week (180 min) throughout the school years from pre-school to third grade. In Denmark, the standard PE lessons are delivered as two weekly classes, and are mandatory for the pupils. The additional PE lessons were handled by the usual PE teachers( Reference Hasselstrom, Karlsson and Hansen 17 , Reference Andersen and Froberg 18 ).
(2) Additional education of PE teachers: Each year, the PE teachers participated in a 1-d course and six afternoon sessions (3 h) with practical and theoretical training focusing on the development of body, healthy living and diet( Reference Andersen and Froberg 18 ). Also, a network was established for the PE teachers to exchange knowledge( Reference Husby 19 ), and the facilities for PE were improved( Reference Hasselstrom, Karlsson and Hansen 17 , Reference Andersen and Froberg 18 ).
(3) Improvement of schoolyard environment: The schoolyard environment was improved to stimulate the children to be more physically active during recess( Reference Andersen and Froberg 18 ). However, the schoolyards were not all improved at day 1 of intervention, but were improved over a period of time.
(4) Parent involvement: Parents received regular information concerning a healthy diet from the municipality via newsletters from the school.
(5) Establishment of school canteens: School canteens that intended to sell healthy meals and snacks were established over time in the intervention schools with the aim of providing pupils an opportunity to buy nutritious meals in the school hours; promoting the use of school canteens by children who did not bring packed lunch from home; and improving the knowledge of children about healthy food by offering them an opportunity to be involved in running the canteen.
(6) Health education in the curriculum: Health education was incorporated into the general curriculum from the first grade to the third grade. The implementation of the intervention parts was carried out by the municipality of Ballerup, while pre- and post-measurements of diet, physical activity and anthropometrics were done by a research group. Pre- and post-measurements were also done for the comparison group.
Subjects
The ten schools in the municipality of Ballerup served as a non-randomised intervention group. All the eight public schools in Tårnby, another suburban municipality of Copenhagen, were chosen as the comparison group, as the community in Tårnby resembled the socio-demographic characteristics of Ballerup( Reference van Vught, Heitmann and Nieuwenhuizen 20 ). All the children entering pre-school class in a public school in Ballerup or Tårnby in 2001 (n 1024) were invited to participate in the present study. Written consent for participation was given by their parents or caregivers for 69 % of the children( Reference Hasselstrom, Karlsson and Hansen 17 , Reference van Vught, Heitmann and Nieuwenhuizen 20 ). Information on dietary intake, anthropometrics and physical activity was collected from the children before (in the school year 2001–2 at age 6 years) and after (in the school year 2004–5 at age 9 years) the intervention period. Only children with complete information on dietary intake, both before and after the intervention, and on maternal education level were included in the present study. In total, 701 (intervention group: n 411; comparison group: n 290) children participated in the present study, of whom dietary information was obtained from 499 (49 %, intervention group: n 292; comparison group: n 207) children pre-intervention (Fig. 1). Of those, 139 (intervention group: n 81; comparison group: n 58) children were excluded from the present study, as they did not participate in the dietary assessment post-intervention. An additional forty-nine (intervention group: n 26; comparison group: n 23) children were excluded due to missing information on maternal education, and four (intervention group: n 1; comparison group: n 3) children due to invalid dietary records, resulting in 307 (30 % of the invited population) children available for the final analyses. Of those, 184 (60 %) children were from the intervention group and 123 (40 %) were from the comparison group.

Fig. 1 Flow chart of participants included in the present study. SES, socio-economic status.
Ethics
The present study was conducted according to the guidelines laid down in the Declaration of Helsinki, and all procedures involving human subjects/patients were approved by the Ethical Committee of Copenhagen County (case no. KA00011gm). Furthermore, written information about the study was given to all school leaders, teachers and parents before the start of the study.
Dietary assessment
Information on dietary intake was recorded in Spring 2002 (pre-intervention) and 2005 (post-intervention) for 7 d by the parents or caregivers of children in pre-printed food records. The food records were divided into four sections: breakfast; lunch; dinner and in-between snacks according to a typical Danish meal pattern. Each meal was further divided into several subsections with beverages, bread, cereals, vegetables, etc., and pre-printed with the most common foods and drinks, and supplemented further with an open-ended category( Reference van Vught, Heitmann and Nieuwenhuizen 20 ). Household measurements and a photo series illustrating common Danish foods in different portion sizes were used to estimate the amount of food eaten( Reference van Vught, Heitmann and Nieuwenhuizen 20 , Reference Fagt, Biltoft-Jensen and Matthiessen 21 ). The food records were developed by the National Food Institute, Technical University of Denmark, and have been in use in the Danish nationwide dietary surveys since 1995( Reference Fagt, Matthiessen and Biltoft-Jensen 22 ). The food records were validated in 1994 and found useful for assessing the intake of food and drink among adults( Reference Larsen 23 ). Also, two studies have evaluated the pre-printed food record against an estimated energy expenditure using ActiReg measurements and a fixed physical activity level. The studies showed only modest misreporting among the children aged 7–8 years( Reference Trolle, Amiano and Ege 24 , Reference Rothausen, Matthiessen and Groth 25 ).
The completed food records were scanned using Eyes & Hands (version 5.2, 2005; Readsoft Ltd). Afterwards, individual intakes were calculated using the General Intake Estimation System (version 1.000, released 26 February 2010, and developed by the National Food Institute, Technical University of Denmark) and the Danish Food Composition Databank (version 6)( Reference Saxholt, Christensen and Møller 26 ). Based on the Nordic Nutrition Recommendations( 5 ), the total energy intake (kJ) was calculated as:
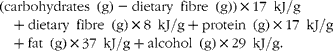 $$\begin{eqnarray} (carbohydrates\ (g) - dietary\ fibre\ (g))\times 17\ kJ/g + dietary\ fibre\ (g)\times 8\ kJ/g + protein\ (g)\times 17\ kJ/g + fat\ (g)\times 37\ kJ/g + alcohol\ (g)\times 29\ kJ/g. \end{eqnarray}$$
$$\begin{eqnarray} (carbohydrates\ (g) - dietary\ fibre\ (g))\times 17\ kJ/g + dietary\ fibre\ (g)\times 8\ kJ/g + protein\ (g)\times 17\ kJ/g + fat\ (g)\times 37\ kJ/g + alcohol\ (g)\times 29\ kJ/g. \end{eqnarray}$$
The content of dietary fibre in the Danish Food Composition Databank is mainly based on the data determined using the Association of Official Analytic Chemists method and includes chemically modified starch, resistant starch, cellulose, pectins, hydrocollids, lignin, tannins/polyphenols and phytate( 5 , 27 ).
Weight and height were measured by trained researchers to the nearest 0·1 kg and 1 mm, respectively, using an electronic scale (Seca 882; Medical Scales) and a transportable Harpenden stadiometer (Holtain)( Reference Eiberg, Hasselstrom and Gronfeldt 28 ). BMI was calculated as weight (kg)/height (m)2, and weight status was assessed according to the cut-off points recommended by the International Obesity Task Force( Reference Cole, Bellizzi and Flegal 29 ). The reported total energy intake was evaluated according to the estimated total energy expenditure based on BMR (estimated with a predictive equation( Reference Schofield 30 )) and physical activity. This has been described in detail elsewhere( Reference Jensen, Nielsen and Husby 31 ). Briefly, physical activity was measured using uniaxial accelerometers (MTI 7164; Manufacturing Technology, Inc.) placed on the lower back and worn all the time for four consecutive days except during sleep and water-based activities( Reference Eiberg, Hasselstrom and Gronfeldt 28 ). Water-based activity was corrected afterwards for the post-intervention measure since some of the additional PE lessons provided as a part of the intervention were swimming( Reference Bugge, El-Naaman and Dencker 32 ).
The dietary components included in the present study are macronutrients (protein (E%), fat (E%) and carbohydrates (E%)), fatty acids (SFA (E%), MUFA (E%), PUFA (E%)), added sugar (E%) and dietary fibre (g/d and g/MJ). The intervention effect on dietary fibre was assessed both as the absolute intake (g/d) and as the relative intake (g/MJ).
The change in intake was calculated as the intake pre-intervention subtracted from the intake post-intervention.
Additional information
Information about maternal education was self-reported and obtained using two questions pre-intervention. The first question was ‘What school education have you achieved or are you currently completing?’, which could be answered using one of four fixed answers (from less than 7 years of education to completion of high school or equivalent), or an open-ended answer with the possibility to state other types of education. The second question was ‘Do you have a vocational education?’, with the possibility to answer ‘No’, or ‘Yes’ with seven different types of vocational education. The answers were then grouped into three categories: short – completed elementary school only ( ≤ 10 years); medium – completed high school (12 years) or short education (3 years); long – completed college or university. Maternal education level was used as a proxy for SES in the present study, as it has been associated with eating habits of the children in several studies of cross-sectional( Reference Moreira, Santos and Padrao 33 – Reference Vereecken, Keukelier and Maes 35 ) and longitudinal( Reference Cribb, Jones and Rogers 8 , Reference Jones, Steer and Rogers 10 , Reference Rogers and Emmett 36 ) designs, and is assumed to be a useful indicator of SES in respect of this relationship.
The mothers also provided information on weight and height, which were used to calculate maternal BMI.
Statistical analysis
Descriptive characteristics of the participants pre-intervention were calculated by intervention and comparison groups, and differences between the two groups were tested using unpaired t test or Wilcoxon rank-sum test for continuous variables, depending on the distribution of the data, and using χ2 test for categorical variables. Data were analysed using Stata version 12.0 (StataCorp LP), and P< 0·05 was considered statistically significant.
Dietary intake is presented by intervention and comparison group and further divided by maternal education level and pre- and post-intervention. Differences in the intake between the intervention and comparison groups were tested using unpaired t test or Wilcoxon rank-sum test. Differences in intakes between the three groups of maternal education levels were tested using one-way ANOVA.
Multiple regression analyses were performed to assess the effect of intervention on the dietary intake among children. Regression analyses were conducted including intervention/comparison status of the child as the exposure and the change in each macronutrient (E%), fatty acid (E%), added sugar (E%) or dietary fibre (g/d and g/MJ) from pre- to post-intervention as the outcomes. The exposure (intervention/comparison status of the child) was included as a dichotomous variable with the comparison group as the reference group, and a dummy variable was created for the intervention group to illustrate the effect of being in the intervention group relative to being in the comparison group.
The analyses included a crude model (adjusted for pre-intervention intake of a dietary component of interest and a random effect by school) and an adjusted model (adjusted for pre-intervention intake of the dietary component of interest, a random effect by school and the three-category maternal education level).
Interactions were tested for between exposure (intervention/comparison group) and maternal education level and between exposure and sex. Also, Wald test for a non-linear association between pre-intervention intake and change in intake was conducted by adding a second-order polynomial into the model. For fat (E%), the association between pre-intervention intake and change in intake was significantly non-linear (P= 0·01); thus, pre-intervention intake of fat (E%) was included as a second-order polynomial in the analyses.
First, the analyses were conducted for all children adjusted for pre-intervention intake of the dietary component of interest, school and maternal education level. Analyses were repeated afterwards with stratification by maternal education level. Also, analyses stratified by maternal education level were adjusted for age and sex as sensitivity analyses to take into account possible differences between the groups. Regression analyses were repeated including all children with information on dietary intake pre-intervention and maternal education (n 415) (including children previously excluded due to missing information on dietary intake post-intervention), assuming no change in dietary intake from pre- to post-intervention.
Analyses were also repeated including only children who were assessed as acceptable reporters compared with the estimated total energy expenditure both pre- and post-intervention.
To visualise the changes in the intake of dietary fibre (g/d), protein (E%), fat (E%) and SFA (E%) in the intervention group relative to the comparison group, the change in the intake of each of these dietary factors from pre- to post-intervention in the intervention and comparison groups was calculated and illustrated in Fig. 2. In the figure, the comparison group served as the reference, with a value of zero, and a 95 % CI was applied for the change observed in the intervention group.

Fig. 2 Change in the intake of (a) dietary fibre (g/d), (b) protein (energy percentage, E%), (c) fat (E%) and (d) SFA (E%) from pre- to post-intervention stratified by maternal education level and adjusted for pre-intervention intake of the dietary component of interest and school. The comparison group was chosen as the reference group, and 95 % CI is presented for the intervention group. The figures thus show the differences in the change of dietary intake between the intervention and comparison groups in strata of maternal education level. For example, from pre- to post-intervention, the intake of dietary fibre changed 2 g/d (0·5–3·6) more in the intervention group than in the comparison group for children of mothers with a short education.
Power calculations were made using the PS – Power and Sample Size Calculation programme version 3.0.4 (http://biostat.mc.vanderbilt.edu/PowerSampleSize)( Reference Dupont and Plummer 37 , Reference Dupont and Plummer 38 ) to determine the level of difference possible to detect based on the number of participants, mean and standard deviations for the change in macronutrients (E%), fatty acids (E%), added sugar (E%) and dietary fibre intake (g/d, g/MJ), assuming a power of 80 % and a significance level of 5 %.
Based on the results of the power calculations, differences in change in dietary intake from pre- to post-intervention between the intervention and comparison groups should be detectable in the crude model as small as 0·6 E% for protein, 1·4 E% for fat, 0·8 E% for SFA, 0·6 E% for MUFA, 0·33 E% for PUFA, 1·4 E% for carbohydrates, 1·5 E% for added sugar and 1·4 g/d and 0·1 g/MJ for dietary fibre.
Results
Subjects
Descriptive characteristics of the participants are presented separately for the intervention and comparison groups in Table 1. No variable other than age and maternal education level differed between the two groups pre-intervention.
Table 1 Pre-intervention characteristics of the participants of intervention/comparison group (Mean values and standard deviations; number of participants and percentages)
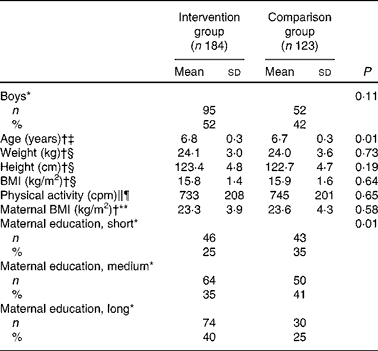
cpm, counts per min.
* Differences between intervention and comparison groups tested by χ2 test.
† Differences between intervention and comparison groups tested by unpaired t test.
‡ Comparison group (n 122).
§ Comparison group (n 121).
∥ Differences between intervention and comparison groups tested by Wilcoxon rank-sum test.
¶ Intervention group (n 160) and comparison group (n 102).
** Intervention group (n 176) and comparison group (n 118).
When comparing children included and not included in the analyses (due to missing information on one or more variables or lost to follow-up), there was a tendency towards that the children not included in the analyses had a higher BMI (P= 0·10). Also, the mothers of the children not included in the analyses had a shorter education (P= 0·09) and a higher BMI (P= 0·01) than the mothers of children included in the analyses. No differences were observed in sex, weight, height, age, comparison/intervention status or physical activity. The only observed dietary difference was a trend towards a higher intake of PUFA among the children included in the analyses compared with those not included (data not shown).
Before intervention, 8·7 % of the children of mothers with a long education were overweight or obese. This was not significantly different from the prevalence among the children of mothers with a shorter education (P= 0·34). After intervention, the prevalence of overweight/obese children tended to be lower among the children of mothers with a long education (6·8 %) than that among the children of mothers with a medium education (17·5 %) or a short education (15·9 %, P= 0·05; data not shown).
Mean dietary intake pre-intervention
Before intervention, a significantly larger proportion of the total energy intake in the comparison group was derived from fat (E%) compared with the intervention group (P= 0·03). Especially, a higher intake of MUFA (E%) was observed in the comparison group relative to the intervention group (P= 0·01). However, a trend towards a higher intake of PUFA (E%) (P= 0·08) was also observed, whereas no difference was observed for the intake of SFA (E%) (P= 0·46) (Table 2). In addition, there was a trend towards a larger proportion of the total energy intake from protein (E%) (P= 0·10) among children of the intervention group.
Table 2 Dietary intake pre- and post-intervention by intervention/comparison group (Mean values and standard deviations)

E%, energy percentage.
* Differences between intervention and comparison groups were tested by unpaired t test.
† Differences between intervention and comparison groups were tested by Wilcoxon rank-sum test.
Stratified by maternal education level, no significant mean differences were observed between the comparison group and the intervention group in dietary intake pre-intervention. A trend towards a higher intake of protein (E%) (P= 0·06) and a lower intake of MUFA (E%) (P= 0·09) was observed among the children of mothers with a long education in the intervention group compared with the comparison group. Also, a trend towards a higher intake of SFA (E%) was observed in the intervention group among the children of mothers with a short education (P= 0·10) (Table 3). Overall, the pre-intervention diet of the participants did not correspond to the Nordic Nutritional Recommendations( 5 ), as in both the intervention and the comparison groups, the mean proportion of energy derived from fat, SFA and added sugar was higher, and the intake of carbohydrates was lower than recommended. However, the intake of dietary fibre fulfilled the Nordic Nutritional Recommendations for that age group.
Table 3 Pre-intervention dietary intake of intervention/comparison group by maternal education level (Mean values and standard deviations)

E%, energy percentage.
* Differences between intervention and comparison groups were tested by unpaired t test.
† Differences between intervention and comparison groups were tested by Wilcoxon rank-sum test.
‡ Mean value was significantly different for dietary intake by maternal education levels (dietary fibre (g/MJ): P= 0·009, dietary fibre (g/d): P= 0·0006; ANOVA).
Evaluation of dietary intake
Out of 217 children with information on diet and physical activity both pre- and post-intervention, 167 children were assessed as acceptable reporters according to the estimated energy expenditure both pre- and post-intervention, and forty-eight children were assessed as under-reporters pre- or post-intervention (pre-intervention: n 11; post-intervention n 42). Two children were assessed as over-reporters pre-intervention, while none of the children was assessed as over-reporters post-intervention. Reporting status was not significantly different between intervention and comparison groups pre- or post-intervention (P>0·57). Significant differences in reporting status were observed with maternal education level (pre-intervention: P= 0·01; post-intervention: P= 0·004), where fewer children of mothers with a long education were assessed as misreporters.
Intervention effects on dietary intake
The dietary intake post-intervention was generally healthier among children from the intervention group compared with those from the comparison group (Table 2). Regression analyses did not show significant associations between intervention/comparison status of the child and change in dietary intake from pre- to post-intervention (both crude and adjusted models). A trend towards lower intake of fat (E%) (P= 0·10) and SFA (E%) (P= 0·09) was observed in the adjusted models (Table 4).
Table 4 Association between intervention/comparison status and change in nutrient intake from pre- to post-intervention* (β-Coefficients and 95 % confidence intervals)
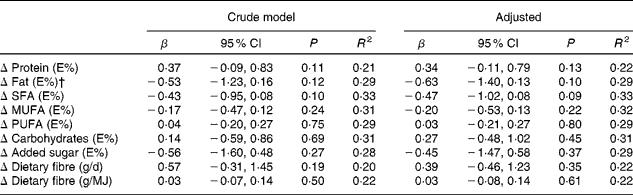
Δ, change in dietary intake from pre- to post-intervention; E%, energy percentage.
* Variables were analysed by multiple regression analyses with intervention/comparison status as dichotomous exposure (with the comparison group as reference) and adjusted for pre-intervention intake of the dietary component of interest and school in the crude analyses and additionally for maternal education level in the adjusted analyses.
† Regression analysis included a second-order polynomial for pre-intervention intake of fat (E%).
Intervention effects on dietary intake according to maternal education level
In the regression analyses stratified by maternal education level and adjusted for pre-intervention intake of the dietary component of interest and school, it was observed that the absolute intake of dietary fibre (g/d) increased (P= 0·01) among the children of mothers with a short education during the intervention period relative to the same group of children from the comparison group (Table 5). A similar trend was observed for the analysis of dietary fibre relative to the total energy intake (g/MJ), although it was non-significant (P= 0·28). Also, there was a trend towards an increased intake of protein (E%) (P= 0·05) and decreased intakes of fat (E%) (P= 0·09) and SFA (E%) (P= 0·10) among children of mothers with a short education during the intervention period, but these changes were of borderline significance (Fig. 2). Thus, among children in the intervention group of mothers with a short education, the intake of dietary fibre increased (P= 0·01) from 15·9 (sd 4·2) to 16·7 (sd 4·9) g/d, and the intake of protein showed a trend towards an increase from 14·1 (sd 2·0) to 14·8 (sd 2·2) E%, while the intake of fat tended to decrease from 36·3 (sd 4·3) to 33·9 (sd 4·8) E%, and the intake of SFA tended to decrease from 16·7 (sd 2·3) to 15·4 (sd 2·9) E%. Also, among the children of mothers with a long education, a significant decrease in the intake of SFA was observed from 16·1 (sd 2·5) to 15·4 (sd 2·6) E% (P= 0·04) (Tables 3 and 5, Fig. 2).
Table 5 Association between intervention/comparison status and change in dietary intake from pre- to post-intervention stratified by maternal education level* (β-Coefficients and 95 % confidence intervals)

Δ, change in dietary intake from pre- to post-intervention; E%, energy percentage.
* Variables were analysed by multiple regression analyses with intervention/comparison status as dichotomous exposure (with the comparison group as reference), stratified by maternal education level and adjusted for pre-intervention intake of the dietary component of interest and school.
† Regression analysis included a second-order polynomial for the pre-intervention intake of fat (E%).
Sensitivity analyses
Sensitivity analyses adjusted for age and sex showed overall similar trends in the results (data not shown).
Sensitivity analyses were also conducted including children with missing information on dietary intake post-intervention, with an assumption of a stable intake from pre- to post-intervention. In these analyses, the same trends were observed as those observed in the analyses including children with information on both dietary collections; however, the association was significant for the intake of dietary fibre (g/d) among the children of mothers with a short education (β = 1·57, 95 % CI 0·52, 2·62, P= 0·006; data not shown).
When the analyses were repeated, including only the children assessed as acceptable reporters, the increased intake of dietary fibre (g/d) among children of mothers with a short education was of borderline significance (β = 2·21, 95 % CI − 0·33, 4·75, P= 0·08, R 2 0·26), while a trend towards a decreased intake of dietary fibre (g/d) was observed among the children of mothers with a long education (β = − 1·42, 95 % CI − 3·03, 0·20, P= 0·08, R 2 0·30) (data not shown). The lower intake of dietary fibre remained significant among children of mothers with a long education when the intake of dietary fibre was assessed according to total energy intake (g/MJ) (β = − 0·17, 95 % CI − 0·30, − 0·03, P= 0·02, R 2 0·22). In the analyses including all children, we observed a significant decrease in the intake of SFA (E%) among the children of mothers with a long education, which remained significant when only the acceptable reporters were included (β = − 0·88, 95 % CI − 1·69, − 0·07, P= 0·04, R 2 0·41). However, the trend towards decreased intake of SFA (E%) observed among children of mothers with a short education was not evident among the children assessed as acceptable reports (β = − 0·66, 95 % CI − 2·40, 1·07, P= 0·43, R 2 0·31). Moreover, a trend towards a decreased intake of PUFA (E%) was observed among children of mothers with a short education (β = − 0·53, 95 % CI − 1·11, 0·06, P= 0·07, R 2 0·43).
Discussion
In the present study, we examined the effects on the dietary intake of the school-based intervention (CoSCIS), and whether these effects depended on maternal education level. After the 3-year intervention, we observed significant or borderline significant changes in the intake of dietary fibre (g/d), fat (E%), SFA (E%) and protein (E%) in the intervention group compared with the comparison group among the children of mothers with a short education, while a significant decreased intake of SFA (E%) was observed among the children of mothers with a long education.
Due to the less healthy eating habits among the children from low SES families compared with children from high SES families as reported in some studies( Reference Rasmussen and Due 13 , Reference Groth, Christensen and Knudsen 14 ), especially the changes observed among the children of mothers with a short education were encouraging. It suggests that school-based interventions might be successful in reaching the specific low SES subgroup that is often considered a group that is difficult to reach. Moreover, it is often considered the group that is in need of utmost changes and to be at the highest risk of developing non-communicable diseases such as overweight and obesity in the future.
We were able to identify only a limited number of published multi-component school-based intervention studies assessing the intervention effects on the dietary intake of macronutrients, fatty acids, added sugar or dietary fibre in children( Reference Caballero, Clay and Davis 39 – Reference Vandongen, Jenner and Thompson 46 ). Some of these studies have reported changes in the intake of fat in the intervention group during the intervention periods( Reference Caballero, Clay and Davis 39 , Reference Gortmaker, Cheung and Peterson 40 , Reference Haerens, Deforche and Maes 42 , Reference Luepker, Perry and McKinlay 44 , Reference Manios and Kafatos 45 ), but not all( Reference Kristjansdottir, Johannsson and Thorsdottir 43 , Reference Vandongen, Jenner and Thompson 46 ). In two studies, they found, similar to our finding, an increased intake of dietary fibre after the intervention period( Reference Gortmaker, Cheung and Peterson 40 , Reference Kristjansdottir, Johannsson and Thorsdottir 43 ). However, none of these studies assessed the intervention effect by SES.
In the Cretan study by Manios and Kafatos, the positive effect of their intervention was ascribed to the high degree of parent involvement, and to the provision of ‘heart-healthy’ alternatives in the intervention school tuck shops( Reference Manios and Kafatos 45 ). The introduction of school canteens was the main dietary intervention in the present study; however, we cannot separate the effects related to the use of canteens from those of parental involvement, or the fact that the municipality of Ballerup decided to focus on health, in general. Furthermore, we have no information on how many children had actually used the school canteens, and so we are not able to evaluate the effects on this. A process evaluation showed that in 2004, only seven of the ten intervention schools had a school canteen established( Reference Husby 19 ). Also, most servings in the school canteens were snacks rather than meals, and as modifications were made by some of the schools in the meals served, compared with the recipes originally provided( Reference Husby 19 ), the meals might not have been as healthy as intended. Therefore, the introduction of school canteens probably cannot solely explain the intervention effects observed in the present study.
We cannot deny that our findings, in part, may be explained as a regression towards the mean phenomena, where children of mothers with a short education have more room for improvement due to their worse eating habits pre-intervention. However, no differences were observed in the dietary intake pre-intervention across the levels of maternal education, except for the intake of dietary fibre (g/MJ), for which a higher intake was observed with increasing maternal education in the intervention group. Moreover, the analyses were adjusted for pre-intervention intake and stratified by maternal education level. Thus, regression towards the mean is a less likely explanation for the findings.
The observed increased intake of dietary fibre (g/d) among the children of mothers with a short education in the intervention group was attenuated when the intake of dietary fibre was examined relative to the total energy intake. This finding indicates that total energy intake is a confounder or a mediating factor since the increased intake of dietary fibre is a consequence of the overall higher energy intake. Also, the intake of dietary fibre (g/d) among children of mothers with a short education in the comparison group seemed to decrease from pre- to post-intervention; and it may be due to the overall lower energy intake reported in that group, since the intake of dietary fibre in g/MJ did not change.
Limitations are related to self-reported dietary intake such as under-reporting( Reference Livingstone, Robson and Wallace 47 , Reference Magarey, Watson and Golley 48 ), recall bias( Reference Livingstone, Robson and Wallace 47 ), social desirability bias( Reference Livingstone, Robson and Wallace 47 , Reference Livingstone and Robson 49 ) and, particularly for this age group, parent's limited knowledge about the child's dietary intake, especially during the time spent away from home( Reference Livingstone, Robson and Wallace 47 ). However, since Danish children, and particularly the young children, generally bring packed lunch boxes to school( Reference Fagt, Christensen and Groth 50 ), parents often have reasonable knowledge of the children's dietary intake during the school hours. Also, the reported dietary intake in the present study corresponds well with the intakes among children (aged 4–9 years) from the Danish National Survey from 2000 to 2004( Reference Pedersen, Fagt and Groth 6 ). The 7-d food record enabled analyses at the individual level, and the objectively measured physical activity level also enabled an evaluation of the reported total energy intake. An increased knowledge on health during the study period could have resulted in parents reporting a healthier dietary intake post-intervention, which would have inflated the observed effects of the intervention. Also, it should be kept in mind that the dietary intake was calculated using standard recipes and food portion sizes, which might have influenced the results, especially when assessing the change in intake.
The percentages of under-reporters were higher post-intervention than pre-intervention, which is in line with an increasing under-reporting with increasing age, which has been reported in other studies, including Danish children and adolescents( Reference Trolle, Amiano and Ege 24 , Reference Rothausen, Matthiessen and Groth 25 ). When the intervention effect was examined including children who were assessed as acceptable reporters, only the increased intake of dietary fibre (g/d) observed among the children of mothers with a short education and the decreased intake of SFA (E%) observed among the children of mothers with a long education remained borderline significant and significant, respectively. These latter results may be assumed to be more valid than the overall results. However, limitations are related to estimation of total energy expenditure and thus to the evaluation of the dietary intake as well. This is one more reason why the results of the dietary evaluation should be interpreted with caution. Thus, the observed effect may be influenced by under-reporting as our analysis among acceptable reporters revealed a borderline effect on dietary fibre intake, but still the strength of the association remained at the same degree.
More under-reporters were observed among children of mothers with short and medium educations post-intervention compared with those with a long education. That may strengthen the present results, since assuming that the children of mothers with a short education have under-reported their energy intake more than the other children, we would expect the intake of dietary fibre (g/d) to be lower as well. However, no difference in misreporting was observed between the intervention and comparison groups. Moreover, the evaluation was solely based on the total energy intake and did not provide information about selective misreporting.
Unfortunately, a substantial part of the invited children and their parents did not participate in the study, and especially for the dietary assessment, a low participation rate was obtained. This might have introduced some selection bias and resulted in insufficient power to detect differences between the two groups. If eating habits of overweight/obese children are more difficult to change, the lower BMI among the participants compared with non-participants and children not included in the analyses could have led to overestimated effects of the intervention. Also, the children and parents that chose to participate in the study might have been different from those not participating, and might have been more receptive to the intervention. Therefore, the results could have been affected by a selection bias, and might not be generalisable to Danish children overall, or to the initially invited study population. This may especially be the case for children of mothers with a short education where we mainly observed the intervention effects. However, as no difference was observed in BMI and physical activity pre-intervention between the children of mothers with a short education included and not included in the analyses, differences in health behaviours between those included and those not included in the analyses may, in fact, be limited.
We cannot completely eliminate that health-promoting activities were introduced in the comparison group during the 3 years of intervention, as this was not registered systematically. However, from an interview with the Deputy Head of the School Administration in Tårnby in 2005 by Husby I, we came to know that a school milk programme was introduced during the intervention period at the schools in Tårnby offering free milk (250 ml/d) for children in pre-school to seventh grade. To the knowledge of the Deputy Head, no other systematic changes regarding physical activity or dietary intake (e.g. implementation of school canteens) were established during the period (personal interview by Husby I of Jensen I, Deputy Head of the Public School Administration in Tårnby; 4 March 2005). Moreover, pre-intervention measures were collected during the school-year when the intervention was initiated, and were thus not pre-intervention measures as such. Both these factors, in worst case, could have attenuated the effect of intervention in the present study.
It cannot be denied that some of the effect of the intervention observed in the present study might have been caused by multiple comparisons that could have increased the risk of type I error( Reference Feise 51 ). When corrected for this using the Bonferroni method( Reference Bland and Altman 52 ), none of the results would remain significant. The Bonferroni method has, however, been criticised for being too conservative and increase the risk of type 2 errors( Reference Bender and Lange 53 , Reference Sainani 54 ). Also, in the twenty-seven analyses conducted when stratified by maternal education, only one finding should be expected to occur by chance. Moreover, the fact that the results are all in the same direction makes it unlikely that the findings in the present study are caused by chance alone.
This multi-component school-based intervention resulted in changes or trends towards changes in the intake of dietary fibre (g/d), protein (E%), fat (E%) and SFA (E%) that were seen mainly among children of mothers with a short education. Even though we cannot determine which parts of intervention were effective, the study implies that the general focus on, and the prioritising of health in the municipality appeared to change the dietary intake in a more healthy direction among the children of mothers with a short education. These results are encouraging and indicate that school-based interventions may be a way to reach children from low SES families in the future. Due to cultural variations and differences in school systems, the intervention may, however, be most applicable to a Danish context. The changes in the dietary intake were generally modest. Based on the dietary intake findings observed among the children, future studies should aim at reducing the intake of fat, and preferably the intake of added sugar, as well.
Acknowledgements
The present study was supported by TrygFonden, Centre for Intervention Research in Health Promotion and Disease Prevention (formerly Centre for Applied Research in Health Promotion and Prevention) (B. W. J., B. L. H., L. B. A., A. B. and B. E.-N.); The Danish Heart Foundation (B. W. J., grant no. 10-04-R79-A2844-22578; A. B., project no. 11297 and L. B. A.); the ‘Familien Hede Nielsen’ foundation (B. W. J.); University of Southern Denmark (B. W. J.); Helsefonden (L. B. A.) and GENDINOB (B. M. N., grant no. 09-067111). TrygFonden, The Danish Heart Foundation, the ‘Familien Hede Nielsen’ foundation, Helsefonden and GENDINOB had no role in the design and analysis of the study or in the writing of this article.
The authors' contributions are as follows: The study was designed by B. L. H., B. E.-N., A. B. and I. H.; L. B. A. participated in the data collection; B. W. J. and L. M. v. K. analysed the data; B. W. J. wrote the manuscript with supervision from B. M. N., E. T., I. H. and B. L. H. All the authors read and approved the final manuscript.
I. H. is in the board of the Arla Foundation. However, the Arla Foundation had no role in the design and analysis of the study or in the writing of this article. The authors have no conflicts of interest to declare.










