Introduction
Frailty is a syndrome common in older adults, which predicts death, functional decline, and disability (Clegg, Young, Iliffe, Rikkert, & Rockwood, Reference Clegg, Young, Iliffe, Rikkert and Rockwood2013). Frailty was noted long ago by the Roman philosopher Seneca: “You live as if you were destined to live forever, no thought of your frailty ever enters your head, of how much time has already gone by you take no heed” (Basore, Reference Basore1932). The lay definition of frailty is concise: “The condition of being weak and delicate” (English Oxford Living Dictionaries, n.d.). In medicine, the term “frailty” was used in early geriatric writings (Supplement 2772, 1948; Warren, Reference Warren1946); often in conjunction with debility, disability, and advanced illness (Warren, Reference Warren1946). Some used the term “frail ambulant” to categorize those with disability yet who were still mobile, and required care in long stay annexes (Cosin, Reference Cosin1947). Early risk measures of frailty incorporated cognitive loss, functional loss, and incontinence (Arnold & Exton-Smith, Reference Arnold and Exton-Smith1962). These measures are similar to frailty measures used in large population–based epidemiological studies, such as the rules-based frailty measures of the Canadian Study of Health and Aging (CSHA) (Rockwood et al., Reference Rockwood, Stadnyk, MacKnight, McDowell, Hebert and Hogan1999). Another model of frailty, initially proposed by Brocklehurst (Reference Brocklehurst1985) was subsequently refined as the “dynamic model of frailty” by Rockwood et al. (Rockwood, Fox, Stolee, Robertson, & Beattie, Reference Rockwood, Fox, Stolee, Robertson and Beattie1994). This model proposed a fluid state of assets and deficits in multiple domains. When the balance tips in the direction of deficits, an individual is more vulnerable to adverse outcomes – in effect, they are frail.
The two most recently described theories of frailty in medicine are the “frailty as a phenotype” model (Fried et al., Reference Fried, Tangen, Walston, Newman, Hirsch, Gottdiener and McBurnie2001) and the “accumulation of deficits” model (Mitnitski, Mogilner, & Rockwood, Reference Mitnitski, Mogilner and Rockwood2001; Rockwood & Mitnitski, Reference Rockwood and Mitnitski2007; Searle, Mitnitski, Gahbauer, Gill, & Rockwood, Reference Searle, Mitnitski, Gahbauer, Gill and Rockwood2008). Currently, these are the most widely used clinical definitions. The former proposes that frailty is a distinct state characterized by unintentional weight loss, exhaustion, weakness, slow walking speed, and low physical activity. It is conceptualized as a distinct syndrome distinguishable from the effects of multimorbidity and disability. Conversely, the “accumulation of deficits” model of frailty proposes that frailty is the cumulative effect of multiple deficits in multiple domains which pile up over time, resulting in a high risk of adverse outcomes. Common to both theories is the acceptance of complex causal mechanisms operating over long time frames, and the desire to move beyond simple disease-based measures of disease (Bergman et al., Reference Bergman, Ferrucci, Guralnik, Hogan, Hummel, Karunananthan and Wolfson2007).
Although considerable academic discussion has centered on the definition of frailty, the perspective of older adults has received less attention. Grenier (Reference Grenier2007) conducted interviews with older women and found that the participants did not define themselves as frail. Yet they often subverted the notion of frailty in order to secure services, such as home care services, which were targeted to frail older adults. Kaufman (Reference Kaufman1994) had also observed the care process for older individuals defined as frail. She found that the definition of frailty was socially produced in response to cultural discourses about surveillance and individualism. She maintained that the definition of frailty evolves over the course of geriatric assessment, and recommended further discussion and study of this process. Nicholson, Meyer, Flatley, and Holman’s (Reference Nicholson, Meyer, Flatley and Holman2012) qualitative psychosocial examination of frailty in older persons identified a dynamic reconceptualization of the concept not defined solely by loss but which also includes the maintenance and creation of new social and emotional connections. Despite a large number of publications on theoretical models of frailty from an academic and clinical viewpoint, relatively few studies describe the views of older adults themselves. This is particularly true for older men. In order to address this gap in the literature, we sought to obtain definitions of frailty from male participants of a prospective cohort study.
The study’s specific objectives were to (1) explore the definitions of frailty of older men; and (2) determine if these definitions matched commonly used clinical definitions of frailty.
Methods
Sample
The methods of the Manitoba Follow-up study (MFUS) have been described in detail elsewhere (Tate, Cuddy, & Mathewson, Reference Tate, Cuddy and Mathewson2015). Briefly, the MFUS is a cohort study of 3893 men who qualified as aircrew in the Royal Canadian Air Force during the Second World War. Since the cohort was sealed in 1948, these men have been followed regularly with routine clinical examinations and with their medical records obtained. Since 1996, a successful aging questionnaire (SAQ) has been included in the survey. This survey includes items on functional status, health-related quality of life, and an open-ended question on successful aging. Since 1948, 30 men have been lost to follow-up (excluding deaths). The study receives annual approval from the Research Ethics Board of the University of Manitoba.
In the spring 2015 mailing of the annual SAQ, we added questions related to frailty. The survey was mailed to 231 surviving MFUS members with current addresses. There was an 81 per cent response rate with 25 surveys returned marked “moved” or “deceased”, 14 surveys returned with proxy responses, and 147 with the frailty page completed by the MFUS member himself, without assistance.
Measures
Age was self-reported at the time of the survey. Functional status was measured with 25 items reflecting the ability to perform activities of daily living (ADLs) and instrumental ADLs (IADLs). Health-related quality of life (HRQoL) was measured using the RAND 36-Item Short Form Survey (SF-36) (Ware & Sherbourne, Reference Ware and Sherbourne1992). We added five items pertaining to frailty:
(1) What is YOUR definition of frailty?
(2) Do you think that YOU are frail?
(3) Rate YOUR frailty on this scale [a 7-point frailty scale].
(4) Is the notion of frailty important to you?
(5) Do you think that people can accurately rate their frailty?
For these analyses, we considered items 1, 4, and 5. These questions were open ended and added into the SAQ in a manner similar to that which was used to elucidate the notion of successful aging in this cohort. Specifically, the item on the definition of frailty was chosen to mirror the question asked about successful aging.
Data Analysis
We considered the responses to the open-ended question about frailty (Pope, Ziebland, & Mays, Reference Pope, Ziebland and Mays2000). Two authors reviewed these answers for the 147 participants. We included the direct response to the question, and comments in other parts of the survey, such as the open-ended space provided at the end of the survey for general comments. Key words were identified, and responses were grouped into themes. These themes reflect the domains of frailty which the older men themselves reported. Reviewer disagreements were resolved by discussion to achieve consensus. We also determined which clinical theoretical model most closely matched the response from the participant. Here, we grouped the responses to most closely fit one of the theoretical models, noted in the results section. We mapped the domains considered onto the respective theoretical model and created a table.
Results
We received responses to the survey from 147 men. The mean age of the participants was 93.0 (SD 2.7); 51 per cent were married and 46 per cent were widowed; the mean score on the Physical Component Score of the RAND SF-36 was 36.5 (SD 10) and 55.7 (SD 8.0) on the Mental Component Score. The mean number of impaired ADLs was 1.3 (SD 2.1), and the mean number of IADL impairments was 3.4 (SD 2.4). Most of the participants did not feel that they were frail (56%) whereas 13 per cent felt that they were; 13 per cent responded “yes and no”; and 18 per cent left their response blank or answered “don’t know”. A majority of men (64%) felt that frailty was important to them. Some men felt that frailty was important, just not at that point in their life: “No it isn’t important to me. It probably will occur to me if I live long enough. If I am mentally alert, I will be O.K. with that condition.” Some noted that frailty could predispose people to psychological problems: “Yes, it would lead to depression.” Some participants expressed the importance of persisting in the face of physical frailty.
Several themes emerged from the responses of the airmen. Examples of responses and the thematic group into which we categorized them are shown in Table 1. These themes were not mutually exclusive. The number of men giving each response is shown in Figure 1. More than 20 per cent of the participants left the question blank. The most common response was that frailty was related to ADL impairment. Poor physical performance, which included poor mobility, falls and fall risk, was also a common theme, as was weakness and fatigue.
Table 1: Definitions and themes of frailty of older airmen
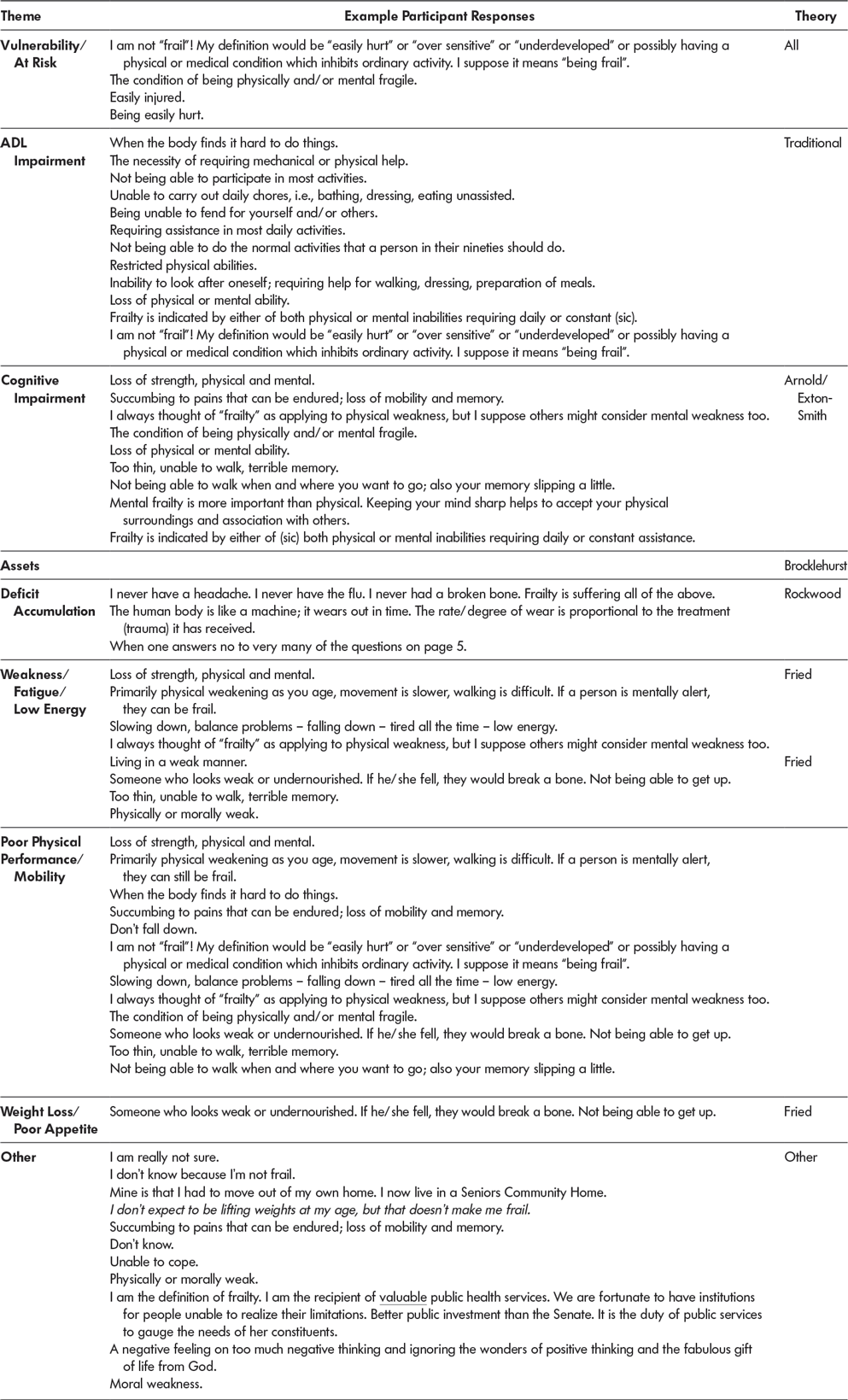
Note. Italicized comments are relevant statements from other parts of the survey questionnaire.
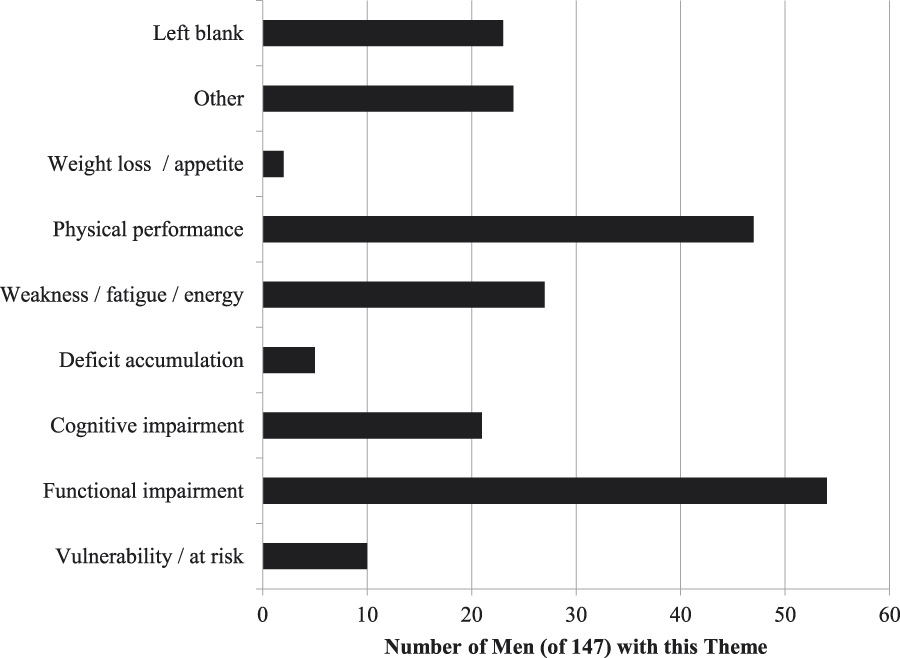
Figure 1: Themes of frailty of older men
We attempted to match the participants’ responses to definitions of frailty, which are, or have been, used in clinical practice. We have organized the responses by the earliest to the latest theory identified.
1. “Frailty as disability” is the traditional description from the early writings in geriatrics which used the term interchangeably with impairment in activities of daily living, debility, and disability (Cosin, Reference Cosin1947). Here the domain considered is functional decline. This was the most commonly noted definition of the participants. Some of the example responses we received follow:
Not being able to participate in most activities.
Unable to carry out daily chores, i.e., bathing, dressing, eating unassisted.
Some of the participants noted that these tasks may be age dependent:
Not being able to do the normal activities that a person in their nineties should do.
2. The “dynamic model of frailty” is the definition initially proposed by Brocklehurst (Reference Brocklehurst1985), later refined and described by Rockwood et al. (Reference Rockwood, Fox, Stolee, Robertson and Beattie1994). This proposes that frailty is a fluid state, balancing deficits in multiple domains against assets in multiple domains. If the balance shifts in favor of deficits, then one could become frailer. Multiple domains – including functional status, cognitive status, medical status, caregiver supports, and social isolation – are considered, and both assets and deficits are noted. This conceptualization of frailty was not commonly noted in participants’ views. An example response (which was not in response to the question but written in the extra comments section of the SAQ) was:
Frailty varies and may not be the same all the time.
3. “Frailty as disability and cognitive loss” are definitions similar to those operationalized in Arnold and Exton-Smith’s (Reference Arnold and Exton-Smith1962) risk index, and the rules-based frailty measure of the CSHA (Rockwood et al., Reference Rockwood, Stadnyk, MacKnight, McDowell, Hebert and Hogan1999). The included domains are functional impairment, cognitive impairment, and urinary incontinence. Examples of responses we received follow:
Loss of physical or mental ability.
Frailty is indicated by either of both physical or mental inabilities requiring daily or constant assistance.
4. “Frailty as a phenotype” (Fried et al., Reference Fried, Tangen, Walston, Newman, Hirsch, Gottdiener and McBurnie2001) – postulates that frailty is a distinct syndrome independent of multimorbidity and disability and is characterized by poor performance on physical performance measures. Domains included are unintentional weight loss, exhaustion, muscle weakness, low gait speed, and low levels of activity. Examples:
Primarily physical weakening as you age, movement is slower, walking is difficult. If a person is mentally alert, they can still be frail.
Slowing down, balance problems – falling down – tired all the time – low energy.
5. “Frailty as the accumulation of deficits” (Mitnitski et al., Reference Mitnitski, Mogilner and Rockwood2001) considers frailty as a state of vulnerability due to the cumulative piling up of multiple deficits in multiple domains over time. Again, multiple domains are considered. Examples:
The human body is like a machine; it wears out in time. The rate/degree of wear is proportional to the treatment (trauma) it has received.
When one answers no to very many of the questions on page 5 [morbidity and limitations in activities of daily living].
Most responses either did not match any theory commonly used in clinical practice or were idiosyncratic to the individual (Figure 2). Examples of responses are shown in Table 1. The most common definition of the participants’ example responses matched the traditional “frailty as disability” definition used in early geriatric reports and writings. Only a minority matched either of the two most commonly used definitions of frailty in the literature: Fried’s “frailty as a phenotype” or Rockwood’s “frailty as accumulation of deficits”. A fairly high percentage of the men reported the importance of cognition to frailty.
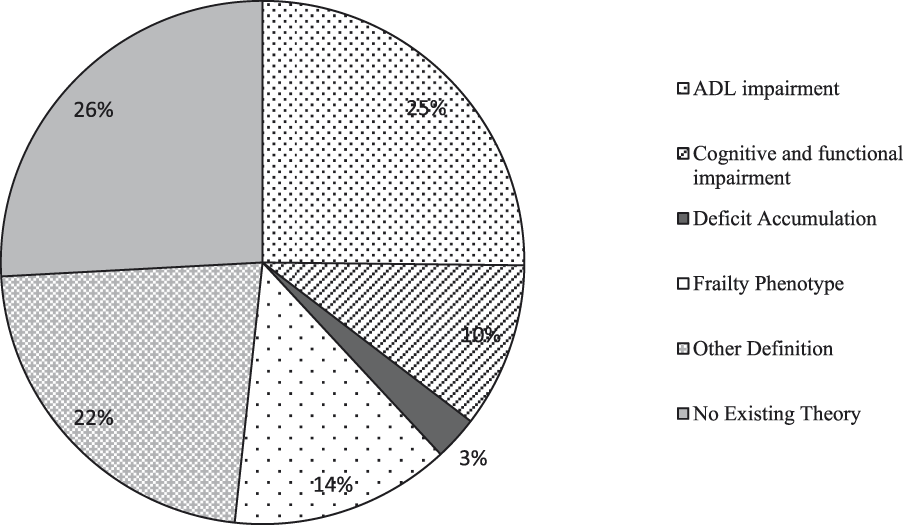
Figure 2: Frailty definitions of older men in relation to definitions of frailty. These are the percentages of older men whose response corresponds most closely to the clinical theory.
Discussion
We have attempted to explore the definition of frailty that older persons themselves use, and whether the issue is important to them. We found that older men thought frailty was important. However, many themes characterizing frailty emerged, all of which have been components in previous models of this construct. The most common theme identified by respondents was the presence of impairment in ADLs. Other common themes were poor mobility or poor physical performance, and weakness or fatigue. We also found that the definitions provided did not fully match the most commonly used models of frailty in clinical care. Furthermore, there was considerable heterogeneity in the responses of the men.
To our knowledge, few attempts have been made to ascertain the definitions of frailty used by older adults themselves. Grenier’s (Reference Grenier2007) interviews with older women found that although they were resistant to use of the term frailty, they nonetheless often co-opted the term for their own purposes. Often, this was to become eligible for assistance or services. Other researchers have reported individual responses to the term “frail” (Richardson, Karunananthan, & Bergman, Reference Richardson, Karunananthan and Bergman2011). This lack of study is in contrast to the numerous attempts to define frailty from the perspective of researchers and clinicians. These definitions and theoretical models have been studied, debated, and refined over time, with unsuccessful attempts to reach consensus (Rodriguez-Manas et al., Reference Rodriguez-Manas, Feart, Mann, Vina, Chatterji, Chodzko-Zajko and Vega2013).
There are strengths and limitations to our approach. First, the cohort was established, and we had the ability to integrate open-ended questions into a survey. Second, MFUS participants had experience with the approach and were familiar with responding to open-ended questions. The approach also built on previous analyses of successful aging questionnaires, with which the researchers were also familiar (Tate, Swift, & Bayomi, Reference Tate, Swift and Bayomi2013). The sample, however, is fairly small, and limited to men over the age of 90. This is both a strength and a limitation. To date, few studies have examined frailty in aging men – particularly very old men. Our study adds to this small evidence base. On the other hand, many of the concepts of frailty may be gendered – for instance, the focus on “shrinking” size, and diminishing strength would be better explored in studies of both men and of women. There may also be sociocultural variations in the definitions of frailty we cannot study, and other people in other parts of the world may have different perspectives. Moreover, the cohort represents a group of men with shared life experiences, which may affect their attitudes and beliefs. Second, the amount of space available on the survey to record responses was limited, which may have resulted in truncated responses. Third, we used an open-ended question to allow for a large number of responses in a broad range of domains. We did not specify that we were referring to frailty in health domains only. This may have led to some confusion in the responses we noted, with some participants defining frailty in non-health domains. We also did not directly speak to the older men. Direct interviews or focus groups would have added further detail and allowed more time for more detailed elaboration of participant perspectives. Finally, we asked the question: “What is YOUR definition of frailty?” This may measure their own experience with frailty, rather than their conceptualization of frailty more generally.
Our findings are important for several reasons. First, most of the participants responded to the question and felt that frailty was important to them. The British Geriatrics Society (BGS) Fit for Frailty report (Turner & Clegg, Reference Turner and Clegg2014) notes the central role of recognizing frailty and considering it in clinical care and in health care delivery, yet cautions against using the term directly with older adults. Indeed, there is a BGS blog devoted to frailty, where frailty is referred to as the “F word”. However, older adults may not be offended by the notion of frailty, but rather may welcome a discussion of frailty, impairments in ADLs, and other geriatric syndromes. Second, there was considerable heterogeneity in the responses provided. No dominant definition of frailty emerged. This is perhaps not surprising, since clinicians have not reached consensus on a definition either. Our findings are broadly consistent with the findings in the social sciences (Kaufman, Reference Kaufman1994; Grenier, 2012) wherein the concept of frailty may be more complex and multidimensional than is noted in clinical practice.
Furthermore, the meaning may evolve over time. Consequently, if an older adult or their family use the term “frail” to describe themselves or another older adult, clinicians should clarify their definition of frailty. Moreover, if clinicians and researchers use the term “frailty”, they too should clarify the definition with the older adult. Third, both our participants and researchers feel that frailty is an important issue. Finally, many participants considered components of frailty, which are not formally included in the common frailty measures. Notably, many participants noted the importance of cognition and mental health in their definition of frailty. This is consistent with a growing interest in “cognitive frailty” (Fougère, 2017) while at the same time consistent with some of the older measures of frailty. Researchers may consider incorporating cognition and other measures of well-being into frailty measures.
Conclusions
Considerable heterogeneity may exist in the definitions of frailty that older people consider. This merits further research and policy development. In the meantime, researchers and clinicians should consider different possible approaches. One approach could be a concerted attempt to define frailty, and reach a codified scientific definition for use by clinicians and/or researchers. The alternate approach would be for clinicians and researchers to consider various models of frailty. The theoretical model used may depend upon the research question, the measures one has at hand, and the tradition of the research group. We may never reach a consensus on the definition of frailty, since each person may incorporate their own values and experiences into their own sense of frailty. For some, this may be a physical slowing and fatigue; for others, it may be the experience of disability, or the cumulative weight of illness. Similar to the heterogeneous definitions of successful aging (Tate, Loewen, Bayomi, & Payne, Reference Tate, Loewen, Bayomi and Payne2009; Tate et al., Reference Tate, Swift and Bayomi2013), there may be a variety of different definitions of frailty which are equally valid and unique to a person at a particular time. Perhaps it is this unique perspective that should be sought in clinical encounters.





