INTRODUCTION
Transmission of infectious disease during commercial air travel has been recently reviewed [Reference Mangili and Gendreau1]. The seating location of passengers during air travel has been associated with the transmission of infections such as tuberculosis [Reference O'Connor2], meningococcal disease [Reference Binotto3], influenza [Reference Marsden4, Reference Moser5] and SARS [Reference Olsen6]. Gastroenteritis associated with air travel has also been reported [Reference Lester7]. An outbreak of norovirus (NV) infection following a transatlantic flight may have been related to infected cabin crew [Reference Widdowson8]. However, there are few published reports of passenger location in relation to the spread of gastrointestinal (GI) illness on international flights.
Outbreaks of NV infection frequently occur on cruise ships and surveillance of GI illness on cruise vessels visiting US ports is an essential monitoring component of the Vessel Sanitation Program (VSP) of the Centers for Disease Control and Prevention (CDC) [9]. Travel packages for cruises and holidays often include a segment of air travel and outbreaks of illness due to Salmonella infection [Reference Reid and Ritchie10], cholera [Reference Eberhart-Phillips11] and NV infection [Reference Outerbridge12] have been associated with such flights.
In January 2007, routine GI illness surveillance on a cruise vessel operating in New Zealand waters identified an outbreak of illness among passengers who had travelled on a long-haul, trans-Pacific flight. This outbreak was investigated by New Zealand public health agencies.
Investigation
The cruise ship operated a series of 14-day summer cruises in Australia and New Zealand between October 2006 and February 2007. On 19 January 2007 a total of 1157 passengers embarked in Auckland and joined 571 crew and 23 passengers who remained on board from the previous voyage – giving a total shipboard population of 1751. The vessel sailed at 18:00 hours and from early on 20 January 2007 an increasing number of people reported to the ship's medical centre with signs and symptoms consistent with GI illness. The ship's master reported the outbreak to local public health authorities, as required under Section 76 of the New Zealand Health Act 1956. The medical staff commented that some of the passengers were from a party who arrived at Auckland International Airport at 06:00 hours on 19 January 2007 after a 12½-h flight from Los Angeles.
The ship's medical centre had identified the index case as a passenger who had a sudden episode of projectile vomiting while in the aircraft cabin en route to Auckland.
The index case was interviewed by telephone about 2 weeks after the cruise had finished when he had returned to the United States. The passenger reported that immediately prior to boarding the aircraft he felt slightly unwell with a ‘squeamish stomach’ and some abdominal discomfort. He did not eat aircraft food because of this discomfort. About 6 h into the flight he felt a sudden urge to vomit – he said this was not ‘air sickness’ but vomiting from an ‘uncomfortable stomach’. He was sitting in seat 35J (middle of the row in zone C) and could not find an air sickness bag in the row of seats. He had to wake the sleeping passenger in the aisle seat (35H) before walking aft to the toilet. He vomited in the aisle just before reaching the toilet. He tried to control this with his hands but said he could have splashed people sitting in the aisle seats in his haste to get to the toilet. He vomited a second time when in the toilet cubicle, soiling the inside surfaces of the cubicle. He attempted to clean up the vomit using paper towels and tissues and told the cabin crew about the mess before he returned to his seat. The cabin crew cleaned the toilet and also the aisle and covered the cleaned floor area with blankets (personal communication between airline agent and G.S.). The passenger remarked that the crew did not appear to have any disinfectant to ‘sanitize the rest room’. A third bout of vomiting occurred about 1 h later but he managed to reach the same toilet without incident.
A second passenger, also seated in row 35 but unrelated to the index case, started to experience abdominal pains during the flight at about the same time as the vomiting incident. This passenger had bouts of diarrhoea but no vomiting and used a toilet in the same block as the index case. This second passenger has been classified as a co-primary index case and excluded from the analyses.
The index and co-primary cases are ‘Reportable GI illness’ according to CDC VSP criteria of (1) diarrhoea (⩾3 episodes of loose stools in a 24-h period) or (2) vomiting and one additional symptom including ⩾1 episode of loose stool in a 24-h period, or abdominal cramps, or headache, or muscle aches, or fever [13].
METHODS
Staff at the ship's medical centre collected health information from all passengers reporting GI illness in the format suggested for the GI illness log by the VSP. This information was extracted from the GI illness log as a Microsoft Excel file (Microsoft Corp., USA) and analysed using Epi-Info version 3.3.2 [Reference Dean14] and WinPepi [Reference Abramson15]. Public health staff liaised with the vessel, the airline, the New Zealand Ministry of Health and Border Agencies to locate additional passengers on the flight. Written contact was made with 36 other passengers who were seated next to ill passengers and 19 (52·8%) completed a questionnaire relating to onset of signs and symptoms of GI illness and their data were added to the Excel file from the ship. Only the index case was interviewed and the co-primary case responded to email questions. No food history was obtained from any passengers.
RESULTS
The outbreak was reported to public health authorities several days after the sentinel event. This retrospective cohort investigation was based on information from the GI illness log supplemented by questionnaires from 19 other passengers on the aircraft.
The ship had information about 203 passengers who formed the aircraft tour group. The additional questionnaires from 19 passengers, seated in zones C and D and two cabin crew, resulted in information about 224 of the 413 (54·2%) people on the flight. Figure 1 gives details of the respondents and shows that 63 people on the plane (28·4%) reported signs of GI illness at some time following the flight.

Fig. 1. Response of travellers on board the long-haul flight.
Case definition
The case definition of GI illness used for this study is ‘a person who travelled on the flight from Los Angeles to Auckland and after disembarkation suffered ⩾3 episodes of loose stools in 24 h or one bout of vomiting and one additional symptom including ⩾1 episode of loose stool in a 24-h period, or abdominal cramps, or headache, or muscle aches, or fever.’
The onset of illness for the 63 people who met the case definition is shown in the epidemic curve (Fig. 2). The distribution is consistent with a point-source outbreak but also suggests secondary transmission among passengers on board the ship. Laboratory confirmation of the cause of illness was not possible because the ship's medical centre could not obtain stool specimens from any of the passengers. The symptoms of projectile vomiting and diarrhoea among >50% of cases (Table 1) meet Kaplan's criteria for viral gastroenteritis [Reference Kaplan16]. The median incubation period was 34·5 h (range 17–51 h) based on exposure being about 03:00 hours on 19 January 2007. The pathogen was likely to have been NV because of the incubation period of between 10 and 50 h (usually 24–48 h) and the pattern of symptoms [Reference Heymann17]. Only those people who developed symptoms before 12:00 hours on 21 January have been included in the analysis. This is seems a generous cut-off because the onset time of the last case in the primary group was 51 h after the vomiting episode (06:00 hours on 21 January). Illness in the remaining 11 passengers was considered to have been caused by secondary infection after the flight.

Fig. 2. Epidemic curve for aircraft passengers. ■, Index+co-primary; □, ship+aircraft; ![]() , aircraft only.
, aircraft only.
Table 1. Symptoms experienced by people with reported illness
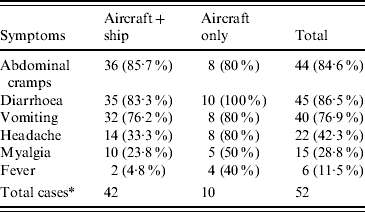
* Excludes index case and co-primary case.
The aircraft
The aircraft was a Boeing 747-400 with a passenger configuration of 56 business class seats (zones A, B, F) and 356 economy class seats (zones C, D, E). The flight had a 96·8% occupancy with 399 passengers and 14 cabin crew.
Aircraft seating
The seat location of the passengers who developed symptoms of GI disease within 60 h of arrival in Auckland demonstrates infection among passengers in five seating zones of the aircraft (Fig. 3). However, passengers seated in zones C and D had three times the relative risk (RR) for illness compared with those in zone E (Table 2). Furthermore passengers seated on the right side of zone C were twice as likely to develop illness compared with those on the left side of the cabin.

Fig. 3. Seating arrangements on the flight.
Table 2. Attack rates for various zones of the aircraft
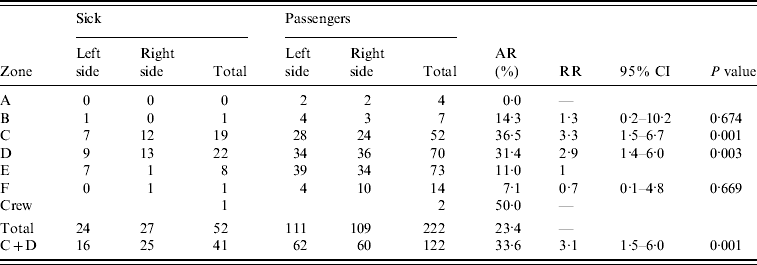
AR, Attack rate; RR, relative risk; CI, confidence interval.
The index cases are excluded from the number of sick passengers and total passengers for the calculation of AR and RR.
Relative risk of illness for passengers sitting right side of the cabin compared with those sitting on the left side of cabin in zone C was 2·0 (95% CI 0·9–4·3, P=0·06), for those in zone D the RR was 1·4 (95% CI 0·7–2·8, P=0·39) and for the combined zones C+D the RR was 1·6 (95% CI 0·96–2·7, P=0·06).
Toilet facilities
There were 10 toilets available for use by the 356 economy class passengers (1 toilet/35·6 passengers) compared to five toilets for the 56 business class passengers (1 toilet/11 passengers).
Only one of the 56 passengers seated in business class (zone A, and the front two rows in zone B in the main cabin and zone F on the upper deck) developed symptoms of illness within 50 h of the vomiting incident (Table 2).
Cabin air supply
There are separate ceiling-level air-supply ducts for the upper deck and main cabin and the incoming air is mixed by vortices with air in the cabin. The air is then extracted through return air grilles at floor level and/or gaps in the ceiling panels. There are no return air grilles in the upper deck so airflow migrates either through panel gaps to the overhead crown area or down the stairwell. There are no return air grilles over the wing box in the main cabin so the return airflow migrates back to grilles aft of the wings (S. Angers, Boeing Aircraft, Seattle, personal communication). Air is flowing continuously and mixing in the cabin giving an air change rate of 20 times per hour on the B747-400. The galleys and toilets have a separate air supply with air extraction rates greater than the air supply rate inside the toilet cubicles (R. Johnson, Boeing Aircraft, Seattle, personal communication) giving a negative pressure.
DISCUSSION
Why did 52 people on the trans-Pacific flight develop GI illness following an episode of in-flight vomiting by one passenger? Passengers seated near the aisle in zone C were probably infected by aerosol droplets or by contact with contaminated surfaces [Reference Caul18, Reference Mark19]. The co-primary index case may have also contaminated the toilet door latch, fittings and interior of the toilet cubicle. The solitary case in zone B was the travel companion of the co-primary case and symptoms started about 20 h after the vomiting incident and so may have been infected before the flight. The one case in business class had an incubation time of 34 h which is consistent with infection on the plane. The toilet cubicle(s) used by the index cases would probably be used by people sitting on the right side (seats F–K) of zones C and D. Contamination of the toilet cubicle(s) could account for the higher rates of infection seen in passengers in zone D, compared to zone E. Passengers from zones D and E sitting on the right side would pass through the contaminated area in zone C to exit and so could have been exposed to contaminated fomites on the floor and seats [Reference Evans20].
The effectiveness of aircraft air recirculation may account for the very low rate of illness in passengers in business class. Transport of aerosol droplets to the upper deck or the forward zones of the main cabin would not be expected from the air circulation patterns of modern aircraft [Reference Hunt21]. Therefore, the pattern of airflow within the aircraft cabin is unlikely to account for the distribution of subsequent illness amongst passengers.
The airline uses national cleaning protocols which require the crew to wear gloves, masks, gowns and scoops while cleaning after vomiting incidents. Sachets of granular sodium dichloroisocyanurate dihydrate (stabilized chlorine granules) are applied to the areas of vomitus and release chlorine in the presence of water. Chlorine is effective against NV and the index case was mistaken in stating there was no disinfectant to sanitize the rest room.
The International Health Regulations 2005 (Annex 9) require incoming aircraft on international flights to report ‘Persons on board with illnesses other than air sickness or the effects of accidents (including persons with symptoms or signs of illness such as rash, fever, chills, diarrhoea) …’ as the Health Part of the Aircraft General Declaration [22]. In this instance the aircraft notified their Auckland Airport staff that there had been passenger sickness during the flight but ‘no individual occurrence raised concern that there was a significant risk for the transmission of communicable sickness’ (personal communication between airline agent and G.S.). The airline did not report the vomiting episode as pre-arrival health information because the crew considered the passenger had ‘air sickness’. It can be difficult to differentiate between passengers with air sickness and those with persistent vomiting due to a communicable disease unless the passenger tells the cabin crew of subsequent attacks of vomiting, or is observed by cabin crew to have further bouts of vomiting. Presumptive NV infection should be suspected in any person who has a sudden onset of projectile or explosive vomiting in the absence of other causes [Reference Caul18].
This incident highlights the potential for apparently minor vomiting episodes to infect a significant number of people. It also raises issues about effective disinfection of surfaces on aircraft. Surface cleaning with detergent-based products has been shown to be ineffective against NV but after 1 min disinfection with a hypochlorite cleaner, containing 5000 ppm chlorine, no NV was detected on smooth surfaces [Reference Barker, Vipond and Bloomfield23]. The use of liquid hypochlorite is problematic because it may cause corrosion of the aluminium aircraft structure. Any cleaning agents used on aircraft must meet specifications approved by the aircraft manufacturer because contact with aircraft structural components or fittings may result in structural damage.
Passengers should be made aware that aircraft surfaces could be a source of infection and advised to perform thorough hand hygiene before eating or putting their hands to their mouth. Aircraft provide hot water, soap and paper towels in toilets. The limited space inside the toilet cubicles and the configuration of aircraft hand basins may discourage people from following CDC advice about washing hands with water and soap for 15–20 s before rinsing and drying [24, 25]. Hand washing with soap and water is required for heavily soiled hands. Prominent display of information on hand hygiene in toilet cubicles would remind passengers about hand washing. The use of an alcohol-based hand-sanitizing product will reduce some viral and bacterial skin organisms [Reference Lee26, Reference Löffler27] and they have been shown to reduce respiratory illness transmission in community settings. Alcohol hand gels have been promoted as an alternative when hands are not visibly soiled. They are used on board many cruise vessels although alcohol is unlikely to be effective against a non-enveloped virus such as NV [Reference Kramer28]. All travellers should be encouraged to thoroughly wash their hands with warm water and soap after using the toilet and dry them with disposable towels. However, in situations where access to adequate water for hand hygiene is limited, it is reasonable to provide and encourage the use of alcohol hand sanitizers as a means of achieving a degree of hand hygiene. Consideration should be given to providing alcohol-based hand gels for passengers on long-haul aircraft where access to toilet facilities may be limited. Creating greater awareness of the need for good hand hygiene is one way to reduce possible transmission of NV through contact with fomites. Regular use of gels as a hand sanitizer may reduce the infection risk if access to soap and water is limited.
ACKNOWLEDGEMENTS
The authors thank the captain and medical staff of the cruise ship and the shipping company for their full cooperation. Thanks are also due to Alyson Baker, Dr Andrea Ford (Ministry of Health, Wellington), Al Campbell (Nelson Marlborough Public Health Service), Dr Brad Novak, Jasmine Mohiuddin, John Whitmore, Shikha David, Jackie Rapana, Dr Simon Thornley (Auckland Regional Public Health Service), Ken Parker (New Zealand Customs Service).
DECLARATION OF INTEREST
None.







