Introduction
Depression is common (Waraich et al., Reference Waraich, Goldner, Somers and Hsu2004) with reported 1-year prevalence estimates ranging around 6.6% in the USA (Kessler et al., Reference Kessler, Berglund, Demler, Jin, Koretz, Merikangas, Rush, Walters and Wang2003), 5.5% in Canada (Patten et al., Reference Patten, Williams, Lavorato, Fiest, Bulloch and Wang2015), 7.4% in Finland (Markkula et al., Reference Markkula, Suvisaari, Saarni, Pirkola, Peña, Saarni, Ahola, Mattila, Viertiö and Strehle2015) and is associated with significant disease burden worldwide (Whiteford et al., Reference Whiteford, Ferrari, Degenhardt, Feigin and Vos2015). The causes and mechanisms behind depression are not fully understood but is commonly framed as a complex outcome of genetic, cognitive, behavioural and environmental risk factors operating in concert.
One of the environmental factors that continuously attracts attention from researchers and the public is how seasonal changes affects mood and depressive symptoms. Seasonal variations impact the prevalence and expression of certain diseases, with influenza serving as one example (Weinberger et al., Reference Weinberger, Krause, Molbak, Cliff, Briem, Viboud and Gottfredsson2012). A host of single studies suggest potential risk factors for depression may vary with seasons (Rosenthal et al., Reference Rosenthal, Sack, Gillin, Lewy, Goodwin, Davenport, Mueller, Newsome and Wehr1984; Roecklein and Rohan, Reference Roecklein and Rohan2005). For example, sleep patterns (Rosenthal et al., Reference Rosenthal, Sack, Gillin, Lewy, Goodwin, Davenport, Mueller, Newsome and Wehr1984; Lewy et al., Reference Lewy, Sack, Singer and White1987), levels of physical activity (Shephard and Aoyagi, Reference Shephard and Aoyagi2009), reproductive behaviours (Roenneberg and Aschoff, Reference Roenneberg and Aschoff1990; Bronson, Reference Bronson1995), a host of neurobiological factors (Carlsson et al., Reference Carlsson, Svennerholm and Winblad1980; Kivela et al., Reference Kivela, Kauppila, Ylostalo, Vakkuri and Leppaluoto1988; Avery et al., Reference Avery, Dahl, Savage, Brengelmann, Larsen, Kenny, Eder, Vitiello and Prinz1997; Neumeister et al., Reference Neumeister, Pirker, Willeit, Praschak-Rieder, Asenbaum, Brücke and Kasper2000; Lambert et al., Reference Lambert, Reid, Kaye, Jennings and Esler2002; Morera and Abreu, Reference Morera and Abreu2006; Kalbitzer et al., Reference Kalbitzer, Erritzoe, Holst, Nielsen, Marner, Lehel, Arentzen, Jernigan and Knudsen2010; Abell et al., Reference Abell, Stalder, Ferrie, Shipley, Kirschbaum, Kivimäki and Kumari2016) are reported to co-vary with seasonal variation and might impact on mood. However, the extent of this impact, and whether or not it translates to functional and clinical significance, remains controversial.
At the individual clinical level, some individuals report seasonal changes in mood that surpass thresholds of clinical significance (Rosenthal et al., Reference Rosenthal, Sack, Gillin, Lewy, Goodwin, Davenport, Mueller, Newsome and Wehr1984; Roecklein and Rohan, Reference Roecklein and Rohan2005). The label ‘seasonal affective disorder’ (SAD) emerged in the early 1980s to capture this phenomenon. Still, neither the ICD nor the DSM diagnostic system includes SAD as a distinct diagnosis. The DSM, since DSM-III-R, has included the possibility to specify if major depression or bipolar disorders occur in a seasonal pattern (Roecklein and Rohan, Reference Roecklein and Rohan2005). In ICD-11, seasonal pattern is now a specifier under mood disorders. The scientific controversy around the concept of SAD remains (Hansen et al., Reference Hansen, Skre and Lund2008; Traffanstedt et al., Reference Traffanstedt, Mehta and LoBello2016; Young, Reference Young2017).
Mood is influenced by perceptions and psychosocial factors (Crum and Phillips, Reference Crum and Phillips2015). One study found that more people searched for depression-related terms on Internet-based search engines in winter (Ayers et al., Reference Ayers, Althouse, Allem, Rosenquist and Ford2013). This could be due to more people suffering from depression in winter, but possibly also a stronger focus on depression in media and peers during this time of year. Those processes may also reinforce each other, and an increased societal and media focus could make people attribute ambiguous symptoms to the season and depression during winter. Attribution sets are also likely to influence research on subjects' experience of seasonality and has relevance for the most commonly used measurement of seasonality, the Seasonal Pattern Assessment Questionnaire (SPAQ). The items in that questionnaire make the intent of measure seasonal variations in mood and behaviour explicit for the respondents. It, therefore, invites a mix of seasonal variation but also reports that reflect subjects' attributions of their symptoms. The questionnaire is criticised for this feature as it might invite memory and confirmation bias (Nayyar and Cochrane, Reference Nayyar and Cochrane1996), and potentially lead to overestimation of seasonal effects. Furthermore, the reliability and validity of the SPAQ have been criticised (Mersch et al., Reference Mersch, Vastenburg, Meesters, Bouhuys, Beersma, van den Hoofdakker and den Boer2004), and it is not considered a valid measurement of depression (Traffanstedt et al., Reference Traffanstedt, Mehta and LoBello2016).
Knowing if, or how, depressive symptoms and mood fluctuate across seasons would contribute to an improved understanding of risk factors, mechanisms and epidemiology of depression. We therefore systematically reviewed the literature to examine if existing evidence supports the assumption of seasonal variation in the prevalence and symptoms of depression. Informed by the potential confirmation bias by self-report, we restricted our search to designs that circumvent this problem and asked, interviewed or collected data from participants without any explicit referral to seasonality as a topic of interest.
Methods
Literature search
We used a broad search strategy and selected the subset of papers on depression and depressive symptoms during the full-text paper review. The following databases were accessed as part of our search strategy: Cochrane Database of Systematic Reviews (via OVID), DARE (Database of Abstracts of Reviews of Effects via OVID), Cochrane Central Register of Controlled Trials (CENTRAL via OVID), Medline and Medline in Process (via OVID), Embase (via OVID), PsycINFO (via OVID) and the Cumulative Index to Nursing and Allied Health Literature (CINAHL via EBSCOHost). A search strategy was developed in consultation with a health sciences librarian (author LS) to identify keywords and Medical Subject Headings (MeSH) in Medline, which were then adapted for all other databases (see the Appendix). The search was conducted from the inception of each database to April 2015, with an updated search July 2017. There were no language exclusion criteria and no publication restrictions. All references were entered into Endnote for processing (n = 4393). After removal of duplicates, 2121 papers remained.
Inclusion and exclusion
Papers were included based on the following:
Type of study. General population studies, registrybased studies, experimental studies and self-report studies published in peer-reviewed journals were considered for inclusion. We did not restrict papers on language or date of publication.
Participants. Youth and adults in the general population (i.e. animal studies and studies with children were excluded).
Exposure. Participants or the sample must have been exposed to more than one season individually or as a group.
Comparison. Repeated measurements over a year or enough measurements per month or per season to provide meaningful comparisons. Time-points had to be defined and presented in the paper. In studies where each participant was measured only once, other design features must have been in place to reasonably assume unbiased selection of time of measurement between subjects.
Outcomes. For the broader search, outcomes were defined as depressive symptoms, anxiety symptoms, symptoms of mental illness, depression, anxiety, mental illness, insomnia, sleep problems, sleep duration and -length, difficulties initiating sleep, suicidal thoughts, suicidal acts, self-harm, suicide, psychiatric hospital admissions. For the purpose of this paper, we focused on depression and depressive symptoms, and hospital admissions and prescriptions related to depression. Most studies on depression prevalence used a screening tool with case identification by the cut-off score. We accepted the authors' approach in these cases and labelled this ‘depression’ despite not having used a diagnostic interview schedule.
Exclusion criteria
We excluded studies where the research hypothesis was available to the participants, or if the research hypothesis or variable measurement overtly related to seasonal variation. Due to these criteria, studies using the SPAQ or similar instruments eliciting the subjective experience of seasonality (Young et al., Reference Young, Hutman, Enggasser and Meesters2015) were excluded.
Procedure
Title and abstract (if available) from the search was listed. The selection procedure (Fig. 1) from the initial papers were done in two rounds. First, two independent evaluators went through the list and excluded papers based on title and abstract, according to the inclusion and exclusion criteria. Disagreement in this phase led to the paper being included in the next round for full-text evaluation. In the next phase, the remaining papers were collected in full text and split into three separate lists. Two persons appraised each of the papers on the list against inclusion criteria. In case of disagreement, the third of this team of three was consulted to reach consensus. The reasons for disagreement were recorded. From the final set of papers, we selected those that had data on seasonal variation in depression. In July 2017, we updated the search following the same process as outlined for the main search and identified additional studies from other sources (ancestry approach).
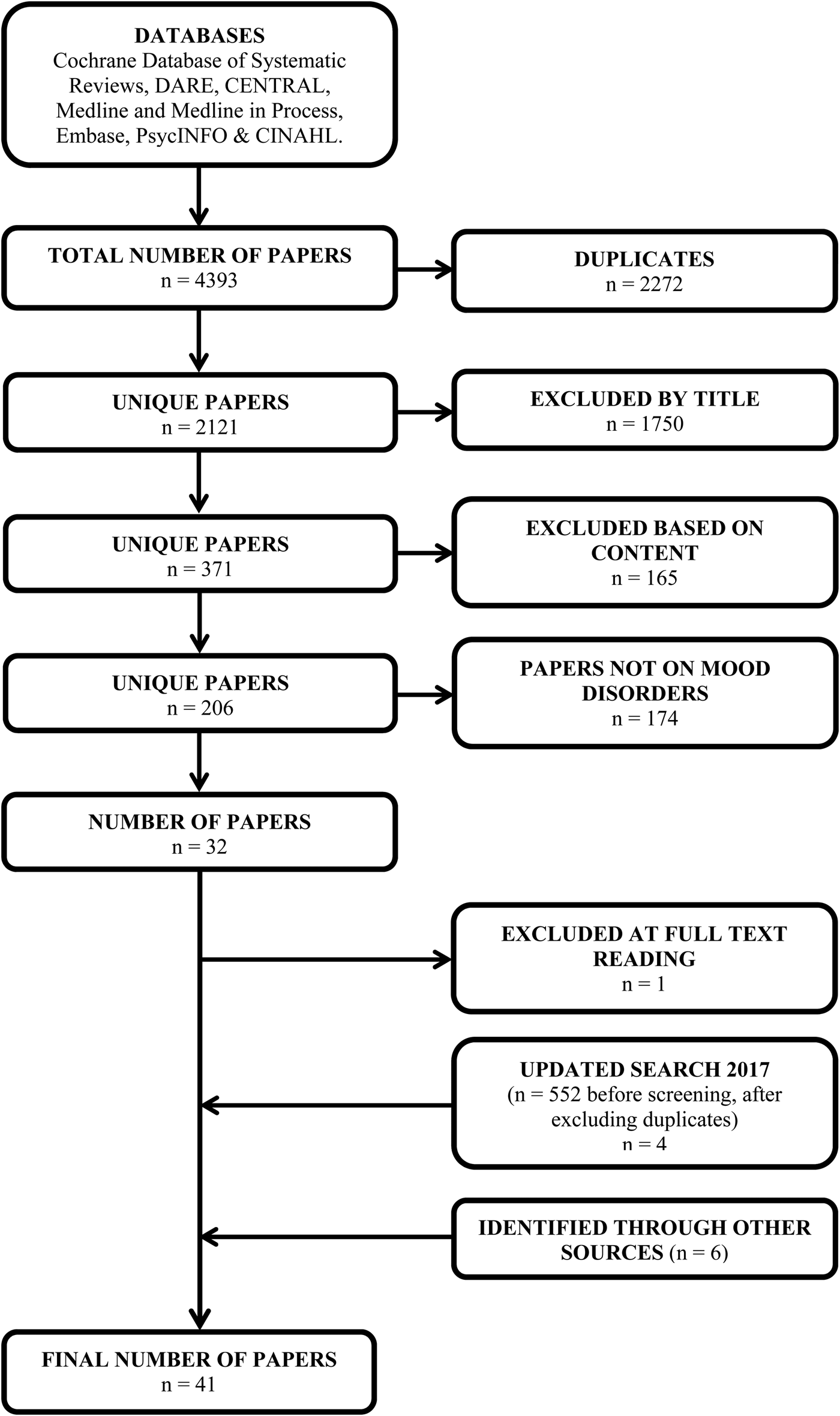
Fig. 1. Flow diagram of the literature search and study exclusion process.
Study quality
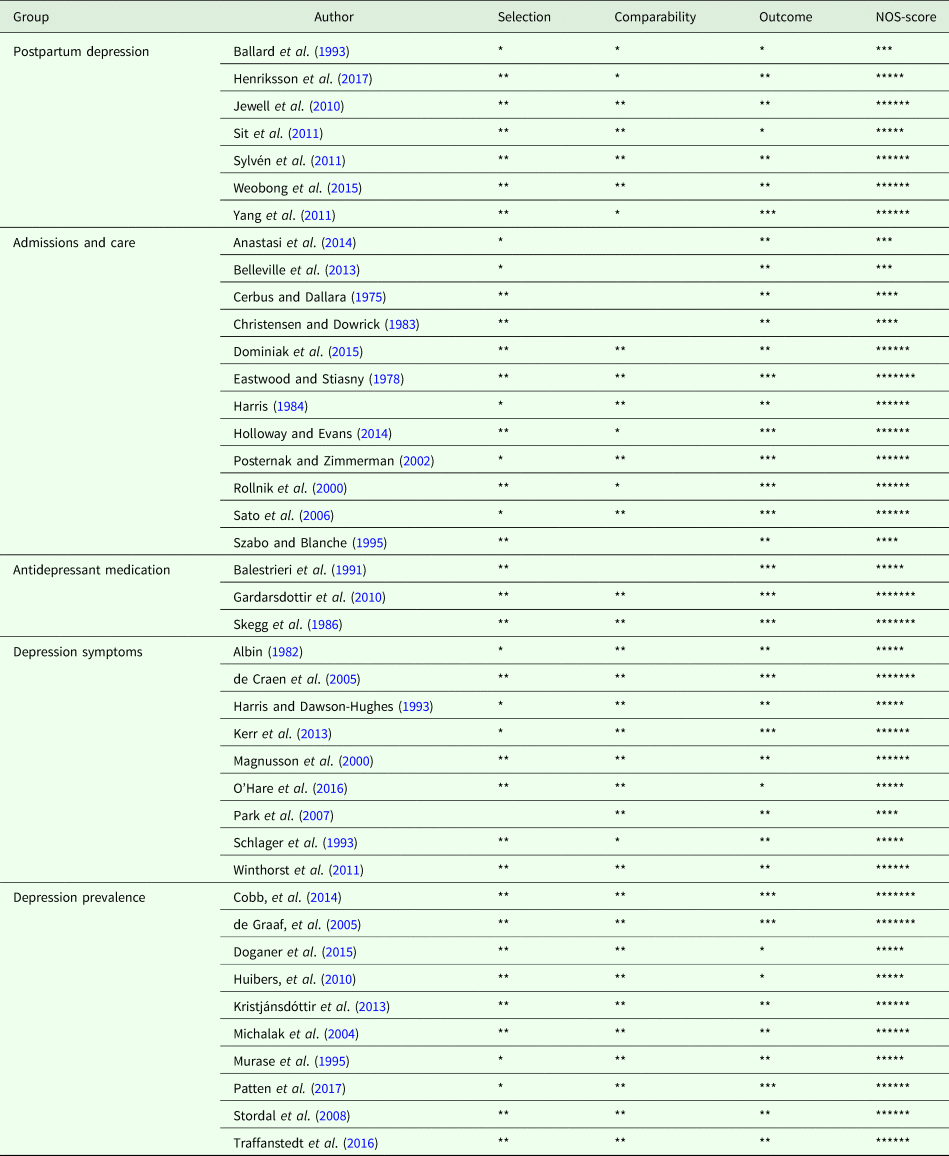
Individual study quality and risk of bias were examined through the use of an adapted version of the Newcastle-Ottawa scale (NOS) (Wells et al., Reference Wells, Shea, O'connell, Peterson, Welch, Losos and Tugwell2000). NOS is a tool to evaluate non-randomised studies. In its original form, it includes eight items across three dimensions: selection, comparability, and outcomes. Study quality is semi-quantified, with a maximum score of nine ‘stars’. The independent variable of interest in this study (seasons) leaves everyone exposed. There are therefore no non-exposed control groups in the studies. For this reason, we disregarded the second item of the scale (selection of the non-exposed cohort). Furthermore, as we were interested in the variability of depression over time (seasons), we excluded the fourth item of the scale (demonstration that outcome of interest was not present at the start of study) and were left with seven stars as the maximum.
Summary measures
We expected and observed large degrees of heterogeneity in definitions, method of assessment, and summary measures amongst the included studies. Consequently, a meta-analysis of studies was not possible and a descriptive review follows.
Results
Of the initial 2108 papers, 378 remained after title and abstract screening and were examined in full text. For the purpose of this review, a total of 32 papers were first included after exclusion by topic and study design (Fig. 1), one was discarded upon further examination of the full text. Another four papers were added after an updated literature search, and a total of six studies were identified through other papers and included. The final list comprised 41 papers (Table 1). Six and 18 studies got a high-quality rating with full score or only point deducted, respectively, using the adapted Newcastle-Ottawa rating scale (Table 2).
Table 1. Description and main findings of included studies
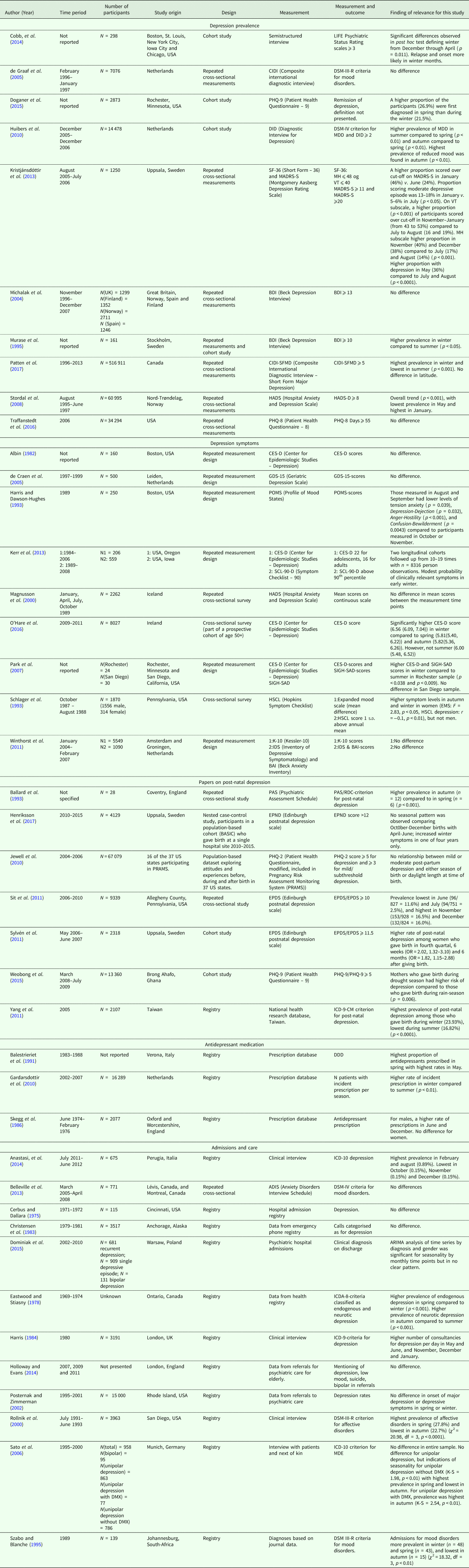
Table 2. Study quality assessment through an adapted version of the Newcastle-Ottawa Scale (NOS)
The studies were sorted in five categories defined by study content (Table 2): The first comprised ten studies on prevalence of depression. Six of these were cross-sectional studies with data collections that spanned across seasons, four were cohort studies of which one used a repeated measurement design. Five of the studies (Murase et al., Reference Murase, Murase, Kitabatake, Yamauchi and Mathe1995; Stordal et al., Reference Stordal, Morken, Mykletun, Neckelmann and Dahl2008; Kristjansdottir et al., Reference Kristjansdottir, Olsson, Sundelin and Naessen2013; Cobb et al., Reference Cobb, Coryell, Cavanaugh, Keller, Solomon, Endicott, Potash and Fiedorowicz2014; Patten et al., Reference Patten, Williams, Lavorato, Bulloch, Fiest, Wang and Sajobi2017) observed indications of seasonality with higher prevalence in winter compared to summer. Notably, Patten et al. (Reference Patten, Williams, Lavorato, Bulloch, Fiest, Wang and Sajobi2017) pooled data from ten surveys in Canada where depression was measured through standardised clinical interviews and found higher prevalence rates in the winter months. In Cobb et al. (Reference Cobb, Coryell, Cavanaugh, Keller, Solomon, Endicott, Potash and Fiedorowicz2014), indications of seasonality was found in a post hoc test where winter was defined as lasting from December through April. Huibers et al. (Reference Huibers, de Graaf, Peeters and Arntz2010) found indications of seasonality in depression, but with the highest prevalence in summer and autumn compared to spring. The study by Doganer et al. (Reference Doganer, Angstman, Kaufman and Rohrer2015) primarily focused on 6-month remission rates, but in their clinical sample, a higher rate were diagnosed in spring (26.9%) v. winter (21.5%). Three of the studies (Michalak et al., Reference Michalak, Murray, Wilkinson, Dowrick, Lasa, Lehtinen, Dalgard, Ayuso-Mateos, Vazquez-Barquero, Casey and Group2004; De Graaf et al., Reference de Graaf, van Dorsselaer, ten Have, Schoemaker and Vollebergh2005; Traffanstedt et al., Reference Traffanstedt, Mehta and LoBello2016) found no indications of seasonality.
Nine studies were sorted under depressive symptoms, all based on self-reported symptom levels through the use of questionnaires. Six of the studies used repeated measurement designs while three studies were single cross-sectional surveys spanning a year. In four of them, no indications of seasonality were found (Albin, Reference Albin1982; Magnusson et al., Reference Magnusson, Axelsson, Karlsson and Oskarsson2000; De Craen et al., Reference de Craen, Gussekloo, van der Mast, le Cessie, Lemkes and Westendorp2005; Winthorst et al., Reference Winthorst, Post, Meesters, Penninx and Nolen2011). Park et al. (Reference Park, Kripke and Cole2007) found higher mean scores on CES-D during winter in a subsample, while Harris and Dawson-Hughes (Reference Harris and Dawson-Hughes1993) found higher levels of depressive symptoms in October and November compared to August and September. Schlager et al. (Reference Schlager, Schwartz and Bromet1993) found seasonal variation among women with a variety of symptoms elevated in winter, but no similar variation in men. O'hare et al. (Reference O'Hare, O'Sullivan, Flood and Kenny2016) reported a cohort study in Ireland in which on a single cross-sectional measure, depression scores in autumn and spring only were lower than winter (summer scores were not significantly different). Kerr et al. (Reference Kerr, Shaman, Washburn, Vuchinich, Neppl, Capaldi and Conger2013) followed two independent cohorts from school age into adulthood with 10–19 measurements (8316 person observations). In both samples, they observed a modest increase in depressive symptoms in winter, but no effect on caseness.
Seven studies covered postpartum depression, thus consisting of populations that recently have given birth. The most common design in this group were studies with repeated cross-sectional measurements, and most common symptoms were assessed with the Edinburgh Postnatal Depression Scale (Cox et al., Reference Cox, Holden and Sagovsky1987). In four of these studies, the prevalence of depressive symptoms was higher among mothers who gave birth in winter/autumn (Ballard et al., Reference Ballard, Mohan and Davis1993; Sit et al., Reference Sit, Seltman and Wisner2011; Sylven et al., Reference Sylven, Papadopoulos, Olovsson, Ekselius, Poromaa and Skalkidou2011; Yang et al., Reference Yang, Shen, Ping, Wang and Chien2011). Henriksson et al. (Reference Henriksson, Sylven, Kallak, Papadopoulos and Skalkidou2017) reported no overall association in Swedish mothers at one hospital. Jewell et al. (Reference Jewell, Dunn, Bondy and Leiferman2010) used a large sample from the US PRAMS dataset and found no indications of seasonal variation in postpartum depression. In the final study in this group, Weobong et al. (Reference Weobong, Ten Asbroek, Soremekun, Danso, Owusu-Agyei, Prince and Kirkwood2015) found a higher prevalence of depressive symptoms in the drought season compared to the rainy season of Ghana (near the equator).
Two sets of studies focussed on health care use. Three studies used registry data on antidepressant prescriptions. All these three observed seasonal patterns; Balestrieri et al. (Reference Balestrieri, Bragagnoli and Bellantuono1991) found more prescriptions in autumn and spring. Skegg et al. (Reference Skegg, Skegg and McDonald1986) found a higher rate in December and June in men but not women, while the last study by Gardarsdottir et al. (Reference Gardarsdottir, Egberts, van Dijk and Heerdink2010) found more prescriptions in winter. Twelve studies addressed aspects of admissions and care based on individual contact with health services. With the exception of Belleville et al. (Reference Belleville, Foldes-Busque, Dixon, Marquis-Pelletier, Barbeau, Poitras, Chauny, Diodati, Fleet and Marchand2013), all were registry studies. Six of them (Cerbus and Dallara, Reference Cerbus and Dallara1975; Christensen and Dowrick, Reference Christensen and Dowrick1983; Posternak and Zimmerman, Reference Posternak and Zimmerman2002; Belleville et al., Reference Belleville, Foldes-Busque, Dixon, Marquis-Pelletier, Barbeau, Poitras, Chauny, Diodati, Fleet and Marchand2013; Holloway and Evans, Reference Holloway and Evans2014) found no indications of seasonality, including Sato et al. (Reference Sato, Bottlender, Sievers and Moller2006) that found no overall association, but higher rates of prescriptions for major depressive episode in spring among individuals with unipolar depression without depressed mixed states, and in autumn for bipolar and unipolar individuals with depressed mixed states. Szabo and Blanche (Reference Szabo and Blanche1995) found more admissions for mood disorder in winter. The remaining five studies in this group found indications of seasonality, but not in winter (Eastwood and Stiasny, Reference Eastwood and Stiasny1978; Harris, Reference Harris1984; Rollnik et al., Reference Rollnik, Dimsdale and Ng2000; Anastasi et al., Reference Anastasi, Eusebi and Quartesan2014; Dominiak et al., Reference Dominiak, Swiecicki and Rybakowski2015).
Discussion
Main finding
The main purpose of this study was to review the question of seasonality of depression excluding studies with high risk of bias through subjective reporting. Of 41 studies, 13 had a main conclusion that suggested more depression in winter (Table 3). The remaining studies either suggested no seasonal pattern, indications of seasonality but outside winter, or ambiguous results in terms of seasonality. The total evidence across the studies was highly equivocal with great heterogeneity in both research questions addressed, study design, definition of seasons, data collection, and statistical analysis. The results were not uniform across the studies, and it is not clear which months are implicated and how to define the season with increased risk. Half of the included studies on depression prevalence found results in line with seasonality in clinical depression. Beyond a possible impact of seasonality on clinical depression, we did not find convincing evidence for seasonality effect in depressive symptoms at the population level.
Table 3. Crude classification of number of papers with main result suggesting no seasonality, winter seasonality, other seasonality or ambiguous results in each of the study categories

Strengths and limitations
The main strength of this study was the systematic approach to search and appraise the literature with design constraints to minimise risk of bias. The broad search strategy could be both a strength and a limitation, but the opportunity to review adjacent aspects of depression together could be of value given the scattered literature on this topic.
We did not register a protocol for this review in advance, which is a limitation. The large heterogeneity of studies, data, and designs restricted us from conducting meta-analyses. It also precluded any approximation of the impact of publication bias, which typically results in non-conservative results (i.e. studies that support the associations of interest are more likely to appear in the published literature) (Dwan et al., Reference Dwan, Gamble, Williamson, Kirkham and Reporting Bias2013). Any bias that increases the likelihood of studies with no difference across seasons to remain unpublished would weaken the empirical support for seasonality of depression. Due to heterogeneity between study designs and reporting it was a challenge to find a standard tool to assess study quality. We ended up with adapting an existing framework (NOS), but assessment and analysis of study quality remained difficult due to the range of approaches used in this literature. Finally, study search and selection was challenging due to study heterogeneity and the broad scope we set up for this search. Some of the included studies were found through in additional searches and reference lists and additional relevant data and studies not identified by us may exist. Our scope for this review did not include careful differentiation between depression subtypes such as unipolar or bipolar depression.
Interpretation
There was a notable lack of consistency of effect in several studies observing seasonal effects. Skegg et al. (Reference Skegg, Skegg and McDonald1986) found a difference for males only and only after adjusting for a declining time-trend in antidepressant use. Schlager et al. (Reference Schlager, Schwartz and Bromet1993) found differences for women but no difference for men. Cobb et al. (Reference Cobb, Coryell, Cavanaugh, Keller, Solomon, Endicott, Potash and Fiedorowicz2014) found the difference in a post hoc test after the definition of winter was extended to include April, and Huibers et al. (Reference Huibers, de Graaf, Peeters and Arntz2010) found increased rates in summer and autumn. Park et al. (Reference Park, Kripke and Cole2007) found a trend in only one of two samples. The large study from Patten et al. (Reference Patten, Williams, Lavorato, Bulloch, Fiest, Wang and Sajobi2017) used a diagnostic interview to identify depression but still relied on subjective recall of onset, with some inherent risk of memory bias. Kerr et al. (Reference Kerr, Shaman, Washburn, Vuchinich, Neppl, Capaldi and Conger2013) used within-subjects repeated measurements. Although they found indications of more depressive symptoms in winter, effect sizes were minute. Many of the studies reported prevalence rates by month, rather than incidence rates that arguably are better suited to inform causal hypotheses on season and illness onset.
Four of seven studies on post-natal depression presented seasonal differences with higher prevalence among mothers who gave birth in autumn/winter compared to spring and summer. Biological causal models, often based on daylight deprivation, are frequently proposed. Social factors might also be of relevance and can coincide and/or reinforce with biological factors. For example, lack of social support is an acknowledged risk factor for postpartum depression (Kim et al., Reference Kim, Connolly and Tamim2014) and availability of social support could vary with seasons due to fewer outdoor activities or seasonal work patterns.
The studies on antidepressant prescriptions all observed seasonal variation, and two of them found the highest prescription rates in winter. These studies have high internal validity in that they present objective data with accurate dates, but they also reflect a response to illness rather than incidence of depression itself. Increased prescription rates can be a result of more severe episodes of clinical depression during the winter which increases both help-seeking and treatment response during those periods. It is also possible that some GPs more readily attribute symptom presentations to depression during certain seasons, which could also contribute to increased prescription.
The literature on seasonality of depressive illness have frequently cited access to daylight as a plausible mechanism, based on the phase shift hypothesis (Lewy et al., Reference Lewy, Sack, Singer and White1987) and the latitude hypothesis (Potkin et al., Reference Potkin, Zetin, Stamenkovic, Kripke and Bunney1986). Melatonin levels correlate negatively with light stimulus and promotes drowsiness (Srinivasan et al., Reference Srinivasan, Smits, Spence, Lowe, Kayumov, Pandi-Perumal, Parry and Cardinali2006). It is suggested that light deprivation brings on seasonal phase shifts in hormone levels, with Melatonin particularly implicated, which in turn may increase the risk of depression. Our results do not provide any clear support to this hypothesis as no clear population level trend was found and reiterates results of previous reviews of this question (Mersch et al., Reference Mersch, Middendorp, Bouhuys, Beersma and van den Hoofdakker1999). The latitude hypothesis and reduced daylight access have also given rise to light-therapy as intervention, but the evidence for its efficacy in preventing depression remains limited (Nussbaumer et al., Reference Nussbaumer, Kaminski-Hartenthaler, Forneris, Morgan, Sonis, Gaynes, Greenblatt, Wipplinger, Lux, Winkler, Van Noord, Hofmann and Gartlehner2015).
This systematic review did not point towards a clear and unified pattern on seasonal variation in depression and depressive symptoms. This does not exclude that seasonal variation influences individuals. Neither does it exclude that for some, such variation may shift individuals to clinically relevant states. It is possible that environmental seasonal change to some extent affects everyone, but that we cope and adapt in ways embedded in culture, behavioural patterns, technology, and societal structures. As exemplified by Kerr et al. (Reference Kerr, Shaman, Washburn, Vuchinich, Neppl, Capaldi and Conger2013), other risk factors for depression seem more salient.
Our results are relevant for the longstanding discussion around seasonal affective disorder. Some of the studies included here did point to a change in the prevalence of depression with seasons. However, we do not see the results from the studies included in this review to be in support of any strong general and public health relevant effect of seasons on mood.
Suggestions for future research in this field
The identified studies used highly heterogeneous study designs and the fragmented results suggest a potential for methodological improvements in this research. The many ways to measure and operationalise depression was also reflected here in terms of scales used, cut-offs and case definitions. Regarding measurement density, some studies had two measurements over the course of a year, while others had monthly registrations. There was also little consensus as to how seasons or winter was defined across studies. Some examined specific months while others used broader categories such as spring and autumn. For example, Cobb et al. (Reference Cobb, Coryell, Cavanaugh, Keller, Solomon, Endicott, Potash and Fiedorowicz2014) included April in winter, while Michalak et al. (Reference Michalak, Murray, Wilkinson, Dowrick, Lasa, Lehtinen, Dalgard, Ayuso-Mateos, Vazquez-Barquero, Casey and Group2004) defined April as part of spring. Yet others defined seasons in relation to winter and summer solstice and in many studies definitions of seasons remained unclear.
Many of the studies included in this review used cross-sectional data collections that ran over time and covered the seasons of interest, but that was set up for other purposes than to study seasonality. This design ensures that participants were indeed blind to the research hypothesis. A disadvantage is that design features, such as choice of measurement, timing and frequency seemed less than optimal for many of the papers. For many of the cross-sectional data collections, it was unknown when cases had their onset. As such, cases identified at a given time point may both reflect increased incidence at that time, but also reduced remission rates. This challenges interpretations.
Our results suggest there is a need for more high quality, unbiased studies on seasonal variation in depression. Nominal exposure categories such as ‘winter’ is a crude term to describe exposures, and future studies should accurately state the time-period definitions coupled with informative data on the assumed underlying mechanism. Where possible, analyses should include geographical data and other contexts that could relate to observations such as climate and weather. There may also be important confounders to consider, such as physical activity, sleep and food intake that could both be confounders but also potential mechanisms between season and mental health. Clinical registry data could provide an excellent data source by providing incidence rates per time. Repeated surveys with screening tools will most often reflect prevalence, which could both be a derivative of seasonal variation in remission rates as well as seasonal onset. Precision around these features of studies is important for interpretation and allow for meta-analysis in future reviews in this area.
Conclusion
We conclude that there is some support for seasonal variation in clinical depression, but that this is not likely due to a broad and general mechanism where entire populations are shifted towards lower mood and more sub-threshold symptoms at regular intervals throughout the year. This could be an important nuance for the public, particularly those exposed to major shifts in daylight that frequently get information that suggest winter and less daylight will bring down your mood. Further development in this field will require higher study quality and more unbiased population-based studies on the potential relationship between seasonal changes and depression.
Availability of data and materials
All data for this review are available in the included papers. Details on quality assessment of single studies is available upon request to the corresponding author.
Author ORCIDs
Simon Øverland, 0000-0001-6967-9355; Ian Colman, 0000-0001-5924-0277.
Acknowledgements
We acknowledge the contributions from Anja Steinsland Ariansen and Alexanda Loro who assisted in the initial screening for relevant papers.
Financial support
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Conflict of interest
None of the authors have any competing interests to report.
Appendix
Search terms used for: seasonality and symptoms of depression: a systematic review of the literature
Approach
The following databases were accessed during the electronic component of the systematic review: Cochrane Database of Systematic Reviews, DARE (Database of Abstracts of Reviews of Effects), Cochrane Central Register of Controlled Trials (CENTRAL), Medline and Medline in Process (via OVID), Embase (via OVID), PsycINFO (via OVID) and the Cumulative Index to Nursing and Allied Health Literature (CINAHL). A search strategy was developed to identify keywords and Medical Subject Headings (MeSH) in Medline, which were then adapted for all other databases.
=2121
Medline in Process and OVID Medline
1. Seasons/
2. (season* adj3 varia*).tw.
3. seasonalit*.tw.
4. (season* adj2 pattern*).tw.
5. (periodic* adj3 varia*).tw.
6. (periodic* adj3 fluctuation*).tw.
7. (season* adj2 adjust*).tw.
8. (season* adj2 change*).tw.
9. (season* adj2 rhythm*).tw.
10. (season* adj2 inciden*).tw.
11. or/1-10
12. Depression/
13. exp Self-Injurious Behavior/
14. exp Anxiety/
15. exp Anxiety Disorders/
16. exp Mood Disorders/
17. exp Sleep Disorders/
18. depress*.tw.sea
19. parasuicide*.tw.
20. automutilation.tw.
21. (self adj1 harm*).tw.
22. (self adj1 destruct*).tw.
23. (self adj1 injur*).tw.
24. (self adj1 mutilat*).tw.
25. suicid*.tw.
26. anxiet*.tw.
27. nervousness.tw.
28. hypervigilance*.tw.
29. (anxi* adj3 (dis* or syndrome* or neuros#s)).tw.
30. (personalit* adj2 anankastic*).tw.
31. agoraphob*.tw.
32. (panic adj2 (disorder* or attack*)).tw.
33. hoard*.tw.
34. (phobia adj2 disorder*).tw.
35. (stress adj3 disorder*).tw.
36. (hyperkinetic adj2 heart adj2 syndrome*).tw.
37. (neuros#s adj2 cardiac*).tw.
38. (effort* adj2 syndrome*).tw.
39. (neurocirculator* adj2 asthenia*).tw.
40. (affective adj2 (disorder* or psychos#s)).tw.
41. (mood adj1 disorder*).tw.
42. (bipolar adj2 disorder*).tw.
43. manic-depressi*.tw.
44. melancholi*.tw.
45. (cyclothymic* adj2 disorder*).tw.
46. insomn*.tw.
47. (sleep adj2 (dis* or dysfunction* or syndrome* or deprivation or paroxysm* or myoclonu* or hyponea* or apnea*)).tw.
48. dyssomnia*.tw.
49. hypersomnia*.tw.
50. (excessiv* adj2 somnolence*).tw.
51. hypersomnolence*.tw.
52. narcoleps*.tw.
53. (gelineau adj1 syndrome*).tw.
54. catalep*.tw.
55. (kleine-levin adj1 syndrome*).tw.
56. (toneless* adj1 syndrome*).tw.
57. (nocturnal adj2 myoclon*).tw.
58. (henneberg adj1 syndrome*).tw.
59. (restless adj3 syndrome*).tw.
60. (periodic adj3 movement adj1 disorder*).tw.
61. (willis-ekbom adj1 (dis* or syndrome*)).tw.
62. (wittmaack-ekbom adj1 (dis* or syndrome*)).tw.
63. (apnea adj2 central*).tw.
64. (central adj3 hypoventilation*).tw.
65. (ondine adj2 syndrome*).tw.
66. (pickwickian adj2 syndrome*).tw.
67. or/12-66
68. exp Adult/
69. Adolescent/
70. adult*.tw.
71. adolescent*.tw.
72. teen*.tw.
73. or/68-72
74. 11 and 67 and 73
Embase
1. exp season/
2. (season* adj3 varia*).tw.
3. (season* adj2 pattern*).tw.
4. (periodic* adj3 varia*).tw.
5. (periodic* adj3 fluctuation*).tw.
6. (season* adj2 adjust*).tw.
7. (season* adj2 change*).tw.
8. (season* adj2 rhythm*).tw.
9. (season* adj2 inciden*).tw.
10. seasonalit*.tw.
11. or/1-10
12. exp depression/
13. automutilation/
14. anxiety/
15. exp anxiety disorder/
16. exp mood disorder/
17. sleep disorder/
18. depression.tw.
19. parasuicide*.tw.
20. (self adj1 harm*).tw.
21. (self adj1 destruct*).tw.
22. (self adj1 injur*).tw.
23. (self adj1 mutilat*).tw.
24. suicid*.tw.
25. anxiet*.tw.
26. nervousness.tw.
27. hypervigilance*.tw.
28. (anxi* adj3 (dis* or syndrome* or neuros#s)).tw.
29. (personalit* adj2 anankastic*).tw.
30. (panic adj2 (disorder* or attack*)).tw.
31. agoraphob*.tw.
32. hoarder*.tw.
33. (phobia adj2 disorder*).tw.
34. (stress adj3 disorder*).tw.
35. (hyperkinetic adj2 heart adj2 syndrome*).tw.
36. (neuros#s adj2 cardiac*).tw.
37. (effort* adj2 syndrome*).tw.
38. (neurocirculator* adj2 asthenia*).tw.
39. (affective adj2 (disorder* or psychos#s)).tw.
40. (mood adj1 disorder*).tw.
41. (bipolar adj2 disorder*).tw.
42. manic-depressi*.tw.
43. melancholi*.tw.
44. (cyclothymic* adj2 disorder*).tw.
45. insomn*.tw.
46. (sleep adj2 (dis* or dysfunction* or syndrome* or deprivation or paroxysm* or myoclonu* or hyponea* or apnea*)).tw.
47. dyssomnia*.tw.
48. hypersomnia*.tw.
49. (excessiv* adj2 somnolence*).tw.
50. hypersomnolence*.tw.
51. narcoleps*.tw.
52. (gelineau adj1 syndrome*).tw.
53. catalep*.tw.
54. (kleine-levin adj1 syndrome*).tw.
55. (toneless* adj1 syndrome*).tw.
56. (nocturnal adj2 myoclon*).tw.
57. (henneberg adj1 syndrome*).tw.
58. (restless adj3 syndrome*).tw.
59. (periodic adj3 movement adj1 disorder*).tw.
60. (willis-ekbom adj1 (dis* or syndrome*)).tw.
61. (wittmaack-ekbom adj1 (dis* or syndrome*)).tw.
62. (apnea adj2 central*).tw.
63. (central adj3 hypoventilation*).tw.
64. (ondine adj2 syndrome*).tw.
65. (pickwickian adj2 syndrome*).tw.
66. or/12-65
67. adult/
68. adolescent/
69. adult*.tw.
70. adolescent*.tw.
71. teen*.tw.
72. or/67-71
73. 11 and 66 and 72
PsycINFO
1. seasonal variations/
2. seasonalit*.tw.
3. (season* adj2 adjust*).tw.
4. (season* adj2 change*).tw.
5. (season* adj2 inciden*).tw.
6. (season* adj2 pattern*).tw.
7. (season* adj2 rhythm*).tw.
8. (season* adj3 varia*).tw.
9. (periodic* adj3 fluctuation*).tw.
10. (periodic* adj3 varia*).tw.
11. or/1-10
12. exp affective disorders/
13. exp self destructive behavior/
14. exp anxiety/
15. exp anxiety disorders/
16. exp sleep disorders/
17. depress*.tw.
18. parasuicide*.tw.
19. automutilation.tw.
20. (self adj1 harm*).tw.
21. (self adj1 destruct*).tw.
22. (self adj1 injur*).tw.
23. (self adj1 mutilat*).tw.
24. suicid*.tw.
25. anxiet*.tw.
26. nervousness.tw.
27. hypervigilance*.tw.
28. (anxi* adj3 (dis* or syndrome* or neuros#s)).tw.
29. (personalit* adj2 anankastic*).tw.
30. agoraphob*.tw.
31. (panic adj2 (disorder* or attack*)).tw.
32. hoard*.tw.
33. (phobia adj2 disorder*).tw.
34. (stress adj3 disorder*).tw.
35. (hyperkinetic adj2 heart adj2 syndrome*).tw.
36. (neuros#s adj2 cardiac*).tw.
37. (effort* adj2 syndrome*).tw.
38. (neurocirculator* adj2 asthenia*).tw.
39. (affective adj2 (disorder* or psychos#s)).tw.
40. (mood adj1 disorder*).tw.
41. (bipolar adj2 disorder*).tw.
42. manic-depressi*.tw.
43. melancholi*.tw.
44. (cyclothymic* adj2 disorder*).tw.
45. insomn*.tw.
46. (sleep adj2 (dis* or dysfunction* or syndrome* or deprivation or paroxysm* or myoclonu* or hyponea* or apnea*)).tw.
47. dyssomnia*.tw.
48. hypersomnia*.tw.
49. (excessiv* adj2 somnolence*).tw.
50. hypersomnolence*.tw.
51. narcoleps*.tw.
52. (gelineau adj1 syndrome*).tw.
53. catalep*.tw.
54. (kleine-levin adj1 syndrome*).tw.
55. (toneless* adj1 syndrome*).tw.
56. (nocturnal adj2 myoclon*).tw.
57. (henneberg adj1 syndrome*).tw.
58. (restless adj3 syndrome*).tw.
59. (periodic adj3 movement adj1 disorder*).tw.
60. (willis-ekbom adj1 (dis* or syndrome*)).tw.
61. (wittmaack-ekbom adj1 (dis* or syndrome*)).tw.
62. (apnea adj2 central*).tw.
63. (central adj3 hypoventilation*).tw.
64. (ondine adj2 syndrome*).tw.
65. (pickwickian adj2 syndrome*).tw.
66. or/12-65
67. 11 and 66
68. limit 67 to (200 adolescence or ‘300 adulthood’)






