The association between violence and schizophrenia has been the focus of many research investigations over the past decade. In spite of different sampling strategies (criminal offenders, psychiatric patients or unselected birth cohort) and different sources of information about violent behaviour (self-reports or official records), recent findings have consistently shown an increased risk for people with psychotic disorders to be violent (for a review see Reference Walsh, Buchanan and FahyWalsh et al, 2002). Between 3% and 10% of society's violence is attributable to schizophrenia specifically (Reference Walsh, Buchanan and FahyWalsh et al, 2002), although it is not a common disorder (Reference Jones and CannonJones & Cannon, 1998). Despite this, little is known about potential mechanisms for the association between schizophrenia and violence.
One important question yet to be answered is whether violent behaviour is a direct consequence of psychosis, or whether violent tendencies are already present from an early age in individuals who will develop psychotic disorders in adulthood. The longitudinal Dunedin study allows us to carry out such an analysis. This birth cohort has prospective measures of physical aggression throughout childhood, a self-report measure of psychotic symptoms at age 11 years, as well as measures of violent behaviour and psychiatric disorders at age 26 years. A previous analysis from the Dunedin study showed a strong concurrent relationship between violent behaviour and schizophreniform disorder when study participants were aged 21 years, the peak age for committing violent crimes (Reference Arseneault, Moffitt and CaspiArseneault et al, 2000). In this report we examine the association between violence and schizophreniform disorder in this group at age 26 years, controlling for comorbid substance dependence disorders, and investigate whether violent behaviour in adults with schizophreniform disorder can be accounted for by childhood psychotic symptoms or childhood physical aggression.
METHOD
Sample
Participants were members of the Dunedin Multidisciplinary Health and Development Study (Reference Silva and StantonSilva & Stanton, 1996), a longitudinal investigation of the health and behaviour of a complete birth cohort born in Dunedin, New Zealand, between April 1972 and March 1973. The cohort was established when the children were 3 years old, when 1037 children (91% of eligible births; 52% males) participated in the first follow-up assessment. These individuals constituted the base sample for the remainder of the study. Cohort families represent the full range of socio-economic status in the general population of New Zealand's South Island, and are primarily White. Assessments were conducted at ages 3 years (n=1037), 5 years (n=991), 7 years (n=954), 9 years (n=955), 11 years (n=925), 13 years (n=850), 15 years (n=976), 18 years (n=993), 21 years (n=961) and 26 years, when 980 individuals (96% of the 1019 living cohort members) were traced and interviewed. To ascertain the association between violence and schizophreniform disorder in adulthood, we studied 970 participants with complete data on both violence and mental disorders at age 26 years. To verify whether childhood psychotic symptoms or childhood physical aggression could account for violent behaviour among people with schizophreniform disorder, we studied 759 participants (74% of the living cohort members) who also had complete data on childhood psychotic symptoms and physical aggression. Missing data are mostly from the assessment at age 11 years, when 792 children were assessed at the research unit by a child psychiatrist, whereas the remainder were assessed in their schools and were not interviewed about psychiatric symptoms. There was no systematic difference between those who did and those who did not complete the psychiatric interview at age 11 years in terms of later substance misuse or psychiatric outcome (Reference Poulton, Caspi and MoffittPoulton et al, 2000; Reference Cannon, Caspi and MoffittCannon et al, 2002a ).
Adult schizophreniform disorder
Data on schizophreniform disorder at age 26 years were collected in a private interview using the Diagnostic Interview Schedule for DSM–IV (Reference Robins, Cottler and BucholzRobins et al, 1995). The reporting period covered the 12 months prior to the interview. At this assessment the diagnosis of schizophreniform disorder required:
-
(a) hallucinations;
-
(b) at least two other symptom types from criterion A of DSM–IV (American Psychiatric Association, 1994): delusions, disorganised speech, catatonic behaviour or negative symptoms;
-
(c) evidence of significant impairment in social or occupational functioning (work, interpersonal or self-care).
Our interview protocol ruled out symptoms occurring under the influence of alcohol or drugs. Following this protocol, 3.7% of the cohort assessed at age 26 years met diagnostic criteria for schizophreniform disorder, including 1% of the cohort who met full criteria for schizophrenia. Further details on the procedures for ascertaining schizophreniform disorder are explained elsewhere (Reference Poulton, Caspi and MoffittPoulton et al, 2000).
Adult substance dependence disorders
Seventeen per cent of the total sample met DSM–IV diagnostic criteria for alcohol dependence (12-month prevalence), 9.3% met diagnostic criteria for cannabis dependence and 3.6% met criteria for dependence on other drugs (amphetamines, sedatives, cocaine, crack cocaine, opiates, hallucinogens or inhalants). Because cannabis and alcohol dependence disorders were both associated with an increased risk of violence in this cohort (Reference Arseneault, Moffitt and CaspiArseneault et al, 2000), we created a categorical variable grouping participants who met diagnostic criteria for at least one of these three substance dependence disorders (23.3% of the cohort).
Adult violent behaviour
For this report we used two different measures of violent behaviour: court convictions and self-reports. Court convictions for violence in all New Zealand and Australian courts were obtained by searching the central computer system of the New Zealand police. In the Dunedin sample, violent convictions included inciting or threatening violence, using an attack dog on a person, presenting an offensive weapon, threatening a police officer, rape, manual assault, assault on a police officer, assault with a deadly weapon, aggravated robbery, and homicide. We focused on violent convictions at ages 21–26 years, because there were too few violent convictions in the year prior to the interview, when the participants were aged 26 years, to analyse separately. Forty-eight men and nine women (5.9% of the sample) were defined as violent offenders according to official records for this 5-year period.
To ascertain whether violent behaviours were occurring during the past-year reporting period for schizophrenic symptoms, self-reports of violence committed during the past year were obtained using a private standardised interview developed for the National Youth Survey and National Institute of Justice multi-site surveys (Reference Elliott, Huizinga and KleinElliott & Huizinga, 1989). Violent offences included information about seven different types of violence: simple assault, aggravated assault, gang fighting, robbery, forced sex, domestic violence, and hitting or otherwise hurting a child out of anger (with follow-up questions ruling out situations of physical discipline). A single simple assault was quite common (13.5%), but thereafter the distribution of the violence measure was strongly skewed to more serious offending; therefore individuals who reported two or more different types of violent offences, 4.4% of the sample (34 men and 9 women), were defined as self-reported violent offenders.
Self-reported and court-recorded violence overlapped in the sample. The odds of conviction were 18 times greater for people self-reporting two offence types than for people who did not (95% CI 9.3–36.7). A ‘combined’ violent group was constituted of 81 persons who either had self-reported committing at least two different types of violent offences in the past year or had been convicted of one (8.4% of the sample) in the past 5 years.
Childhood psychotic symptoms
At age 11 years, cohort members were administered the Diagnostic Interview Schedule for Children (DISC–C; Reference Costello, Edelbrock and KalasCostello et al, 1982) for DSM–III criteria (American Psychiatric Association, 1980) by a child psychiatrist (Reference Anderson, Williams and McGeeAnderson et al, 1987). The schizophrenia section of the DISC–C asked five questions about possible psychotic symptoms. The items were scored by the psychiatrist (0 no; 1 yes, likely; 2 yes, definitely). Participants were divided according to the strength of the symptoms: ‘no symptoms’ included children who did not report any symptoms (n=653, 86.0% of the 759 participants with complete childhood data); ‘weak symptoms’ included children who answered ‘yes, likely’ to one symptom (n=94, 12.4%); and 'strong symptoms' included children who answered ‘yes, likely’ to two symptoms or ‘yes, definitely’ to one symptom (n=12, 1.6%). We have previously shown that these self-reported psychotic symptoms at age 11 years predicted a schizophreniform diagnosis at age 26 years (Reference Poulton, Caspi and MoffittPoulton et al, 2000; Reference Cannon, Caspi and MoffittCannon et al, 2002a ).
Childhood physical aggression
Childhood fighting was assessed by the children's teachers at cohort ages 7 years, 9 years and 11 years, using the Rutter Child Scales (Reference McGee, Williams and BradshawMcGee et al, 1985). At each assessment age, teachers reported whether the child had fought with other children in the past year (0 no, doesn't apply; 1 yes, applies somewhat; 2 yes, certainly applies). We divided the sample into three discrete groups based on the levels of physical aggression between ages 7 years and 11 years:
-
(a) non-aggressive children were those who never fought at either 7, 9 or 11 years (n = 495, 65.2% of the 759 with complete childhood data);
-
(b) low-aggressive children were those for whom fighting ‘applied somewhat’ or ‘certainly applied’ only at one assessment point (n = 157, 20.7%);
-
(c) high-aggressive children were those for whom fighting ‘certainly applied’ at two or more of the three assessment points (n = 107, 14.1%).
Parental socio-economic status
The socio-economic status of participants' families was coded into one of six categories based upon the educational level and income associated with occupations in data from the New Zealand census (Reference Elley and IrvingElley & Irving, 1976). The scale ranged from 1 (unskilled labourer) to 6 (professional). The variable used in our analyses, parental socio-economic status, is the average of the highest socio-economic status level of either parent across the seven assessments of the Dunedin study from birth to age 15 years; thus, it reflects the socio-economic conditions experienced by the children while they grew up.
Statistical analyses
Logistic regression techniques were used to investigate the association between schizophreniform disorder at age 26 years and different measures of violence (self-reported, violent convictions, and the combined measure). In this analysis, we included all participants with complete data in adulthood (n=970). We report the risk, estimated by odds ratios with 95% confidence intervals, for people with schizophreniform disorder to be violent according to each of the three measures of violence. We report unadjusted odds ratios, odds ratios adjusted for gender and parental socio-economic status, and finally odds ratios adjusted for gender, parental socioeconomic status and substance dependence disorders at age 26 years, simultaneously. The addition of gender interaction terms did not yield significant improvements in the fit of models predicting violence above and beyond models with main effects only. Consequently, analyses were performed on the whole sample.
We then investigated whether the association between schizophreniform disorder and violent behaviour (using the combined measure) could be accounted for by childhood psychotic symptoms or childhood physical aggression. First, we ascertained the association between schizophreniform disorder and violence within the subsample of individuals with complete data at age 11 years (n=759) using logistic regression analyses. Second, we adjusted the model for self-reported psychotic symptoms at age 11 years (two groups: weak and strong symptoms). The hypothesis was that if violence were significantly associated with schizophreniform disorder at age 26 years and this association were reduced in the second analysis, this change would indicate that the initial association was partly due to the presence of psychotic symptoms prior to diagnosable schizophreniform disorder. Third, we adjusted the model for childhood physical aggression (two groups: low and high aggression). Finally, we adjusted the model for both childhood psychotic symptoms and childhood physical aggression simultaneously.
RESULTS
Concurrent association between schizophreniform disorder and violence
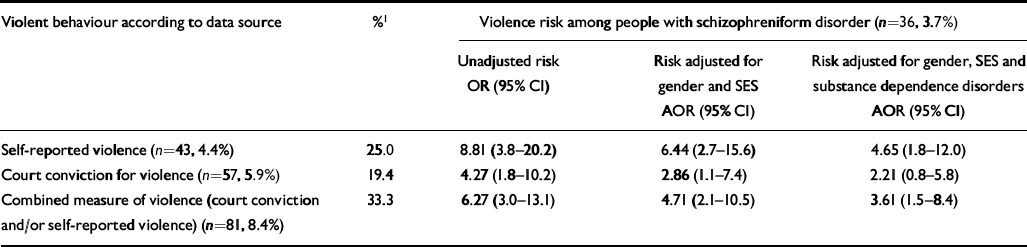
Individuals meeting diagnostic criteria for schizophreniform disorder were at elevated risk of being violent at age 26 years (Table 1). This finding held whether violence was measured using self-reports or court records. This risk decreased after controlling for gender, socio-economic status and concurrent substance dependence disorders, but remained significant. As a group, cohort members who had schizophreniform disorder and who were violent at age 26 years represented only 1.2% of the total sample (n=12). However, this small group of individuals represented 14.8% of the sample's 81 violent individuals, and they were responsible for 8.3% of the sample's total 168 violent court convictions and 10.4% of the sample's total 673 self-reported violent offences. Moreover, 8.9% of violence in the population was attributable to schizophreniform disorder, having controlled for gender, social class and substance dependence disorders.
Table 1 Proportions and risks of violent behaviour among participants with schizophreniform disorder at age 26 years
| Violent behaviour according to data source | %1 | Violence risk among people with schizophreniform disorder (n=36, 3.7%) | ||
|---|---|---|---|---|
| Unadjusted risk OR (95% CI) | Risk adjusted for gender and SES AOR (95% CI) | Risk adjusted for gender, SES and substance dependence disorders AOR (95% CI) | ||
| Self-reported violence (n=43, 4.4%) | 25.0 | 8.81 (3.8—20.2) | 6.44 (2.7—15.6) | 4.65 (1.8—12.0) |
| Court conviction for violence (n=57, 5.9%) | 19.4 | 4.27 (1.8—10.2) | 2.86 (1.1—7.4) | 2.21 (0.8—5.8) |
| Combined measure of violence (court conviction and/or self-reported violence) (n=81, 8.4%) | 33.3 | 6.27 (3.0—13.1) | 4.71 (2.1—10.5) | 3.61 (1.5—8.4) |
Childhood risk factors for violence among adults with schizophreniform disorder
Reduction in the sample size because of missing data at age 11 years did not affect the association we observed between violence and schizophreniform disorder within the complete sample: the risk of violent behaviour adjusted for gender and socio-economic status in the full sample was 4.71 (Table 1), compared with a risk of 4.07 in the reduced sample (Table 2, model 1). When we controlled for psychotic symptoms at age 11 years (Table 2, model 2), the risk of violence in individuals with schizophreniform disorder at age 26 years was reduced to 2.80, a reduction of 31.2%. This indicates that one-third of the risk of adult violence associated with diagnosable schizophreniform disorder at age 26 years was accounted for by psychotic symptoms in childhood.
Table 2 Association between schizophreniform disorder and violence at age 26 years: results of hierarchical logistic regression analyses controlling for childhood psychotic symptoms and childhood physical aggression (n=759)

| Variable | Violence risk among people with schizophreniform disorder (n=36, 3.7%) | |||
|---|---|---|---|---|
| Model 1 Risk adjusted for gender and SES AOR (95% CI) | Model 2 Risk adjusted for psychotic symptoms (age 11 years) AOR (95% CI) | Model 3 Risk adjusted for physical aggression (age 7—11 years) AOR (95% CI) | Model 4 Risk adjusted for psychotic symptoms and physical aggression AOR (95% CI) | |
| Schizophreniform disorder at age 26 years | 4.07 (1.5—11.2) | 2.80 (1.0—8.3) | 3.76 (1.3—10.6) | 2.51 (0.8—7.6) |
| Weak psychotic symptoms | 1.86 (0.9—3.8) | 1.96 (0.9—4.1) | ||
| Strong psychotic symptoms | 6.33 (1.5—26.9) | 5.55 (1.3—23.2) | ||
| Low physical aggression | 1.27 (0.6—2.7) | 1.17 (0.5—2.6) | ||
| High physical aggression | 3.72 (1.9—7.2) | 3.65 (1.9—7.1) | ||
When childhood physical aggression was entered into the model (Table 2, model 3), the risk slightly decreased from 4.07 to 3.76, indicating that childhood physical aggression accounted for a small proportion of the association between adult schizophreniform disorder and violence. Nevertheless, in model 4, when both childhood psychotic symptoms and childhood physical aggression were entered simultaneously, the risk of violence in people with schizophreniform disorder decreased to 2.51, a reduction of 38.3% of the initial violence risk, and became nonsignificant. This suggests an additive effect of childhood psychotic symptoms and childhood physical aggression in accounting for the association between violence and schizophreniform disorder in adulthood.
DISCUSSION
Using prospective measures of childhood psychotic symptoms and childhood physical aggression from a longitudinal birth cohort, this study shows that above and beyond risks associated with being male, growing up in deprived circumstances and meeting diagnostic criteria for substance dependence disorders, individuals with schizophreniform disorder were nearly four times more likely to commit violence compared with people without schizophreniform disorder. Only 1.2% of the Dunedin study cohort met diagnostic criteria for schizophreniform disorder and committed violent offences. However, these individuals were responsible for more than their fair share of community violence (8.3% of the sample's total violent convictions and 10.4% of the sample's total self-reported violent offences), and they represented 15% of all violent offenders in the sample. This risk for violence was accounted for by both childhood psychotic symptoms and childhood physical aggression.
Stability of the risk of violence in adults with schizophreniform disorder
The Dunedin study is the only existing longitudinal cohort study to report on the violence risk in people with schizophreniform disorder at two different assessment points. A comparison of this study with our previous report, when the cohort members were aged 21 years (Reference Arseneault, Moffitt and CaspiArseneault et al, 2000), reveals that the violence risk is relatively similar 5 years later (OR = 4.60 at age 21 years v. OR = 4.71 at age 26 years) and the population attributable risk remains non-trivial (10% at age 21 years v. 8% at age 26 years). Thus, the association between schizophreniform disorder and violence appears to be strong and stable in early adulthood.
Risk factors for violence among individuals with schizophreniform disorder
Researchers are now starting to examine potential risk factors and causal mechanisms for the association between schizophrenia and violence. Since the sine qua non of a cause is that it precedes the outcome, such research requires prospective longitudinal data. Cannon et al (Reference Cannon, Huttunen and Tanskanen2002b ) found that childhood attentional impairment was a risk factor for later violent and criminal behaviour in schizophrenia, and there was a marginally significant increased risk of violence among males with schizophrenia who had a history of labour or delivery complications. Hodgins et al (Reference Hodgins, Kratzer and McNeil2002) found that a history of neonatal complications increased the risk of offending by men with major mental disorders. In our previous study using the Dunedin cohort, we showed that a juvenile history of conduct disorders and an adolescent personality trait characterised by excessive perceptions of threat in the environment partly accounted for violent behaviour in adults with schizophreniform disorder (Reference Arseneault, Moffitt and CaspiArseneault et al, 2000). Supported by the study reported here, evidence is thus accumulating to suggest that at least some individuals with schizophrenia may be at risk of later violence for a variety of reasons (both neurodevelopmental and behavioural) long before a diagnosis is made.
Childhood psychotic symptoms
What role do psychotic symptoms have in the aetiology of violent behaviour? Although findings are not always replicated, cross-sectional studies show a significant association between violent behaviour and certain psychotic symptoms, particularly threat/control override symptoms (Reference Link, Andrews and CullenLink et al, 1992; Reference Link and StueveLink & Stueve, 1995; Reference Appelbaum, Robbins and MonahanAppelbaum et al, 2000). These symptoms refer to a feeling of threats by others (‘have you felt that there were people who wished to do you harm?’) and diminished self-control mechanisms (‘have you felt your mind dominated by forces beyond your control?’). Both the nature of these symptoms and the specificity of the association with these symptoms only were taken to suggest that psychotic disorder ‘causes’ violence (Reference Link and StueveLink & Stueve, 1995), but in fact the temporal relationship could not be assessed in previous cross-sectional studies. To our knowledge, our study is the first to examine the association between psychotic symptoms in childhood and later violent behaviour. We found that a history of self-reported psychotic symptoms in childhood accounts for a substantial proportion of the association between violence and schizophreniform disorders at age 26 years.
Childhood physical aggression
Our findings suggest that individuals with psychotic disorders do not manifest violent behaviour suddenly as their psychiatric disorder appears. Rather, some such individuals are likely to have had past experiences of fighting when they were children. It has been repeatedly demonstrated that a history of violence in childhood is associated with violence in adulthood (Reference FarringtonFarrington, 1994; Reference Tremblay, Pihl and VitaroTremblay et al, 1994; Reference Nagin and TremblayNagin & Tremblay, 2001; Reference Stevenson and GoodmanStevenson & Goodman, 2001), and individuals with schizophrenia are unlikely to be an exception. Further examination of our data indicated that 6.7% of participants with a high level of physical aggression in childhood met diagnostic criteria for schizophreniform disorder at age 26 years, compared with 3.7% of participants with a low level of physical aggression in childhood and 3.1% of participants with no history of childhood aggression. Indeed, we found that violence among adults with schizophreniform disorder could be partly accounted for by a history of early childhood physical aggression. However, a history of self-reported psychotic symptoms at age 11 years appeared to have a stronger effect.
Implications of the findings
This study provides support to previous findings from the Dunedin study in showing that violence by adults with schizophreniform disorder is accounted for by two different sets of early risk factors (Reference Arseneault, Moffitt and CaspiArseneault et al, 2000): conduct disorders and psychotic symptoms. Findings from this report go further in showing that these risk factors are present even in childhood.
Early signs of psychotic symptoms and childhood physical aggression ought to be taken seriously by mental health practitioners, parents and teachers interacting with children. Children's bizarre thoughts that indicate a sense of lack of control over their mind and body should be the target of screening. These symptoms not only represent a risk factor for later schizophreniform disorder (Reference Poulton, Caspi and MoffittPoulton et al, 2000), they also account for violent behaviour among these individuals. Early preventive strategies to reduce physical aggression among young children (Reference DodgeDodge, 2002) are likely to be more effective in decreasing violent behaviour among people with psychosis than is intensive case management in adulthood (Reference Walsh, Gilvarry and SameleWalsh et al, 2001).
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
▪ Adults with schizophreniform disorder show elevated risk for committing violent offences in the community, even when effects of substance dependence disorders are accounted for.
-
▪ Children displaying both early psychotic symptoms and physical aggression should be monitored closely as they are at high risk of later schizophreniform disorder complicated by violent behaviour.
-
▪ Our findings support recommendations that preventive intervention strategies must focus on physical aggression among young children.
LIMITATIONS
-
▪ Temporal relationships between childhood psychotic symptoms and physical aggression could not be examined because psychotic symptoms before age 11 years were not assessed.
-
▪ Findings are based on a small group of individuals who met diagnostic criteria for schizophreniform disorder and who committed violent offences. This limitation prevented us from examining interactions between risk factors.
-
▪ Cohort members had not yet reached the end of the risk period for developing psychotic disorders, implying that some future cases of schizophreniform disorder might have been missed.
Acknowledgements
We thank the Dunedin study members for their collaboration, data manager. HonaLee Harrington, Air New Zealand, and study founder Phil Silva. We also. acknowledge the contribution of Professor Pamela Taylor. The Dunedin. Multidisciplinary Health and Development Research Unit is supported by the New. Zealand Health Research Council. L.A. is supported by the Canadian Institute. of Health Research and the Virtual Institute of Severe Personality Disorder; M.C. is supported by the Wellcome Trust, the EJLB Foundation and the Theodore. and Vada Stanley Foundation; T.E.M. is a Royal Society-Wolfson Research Merit. Award holder. This study was funded by the US National Institute of Mental. Health grants MH45070, MH49414, and by the UK Medical Research Council.





eLetters
No eLetters have been published for this article.