Recent undesirable events and subclinical depressive symptoms are known to correlate with subsequent onset of major depressive disorder (MDD) in adolescents (Reference Lewinsohn, Gotlib and SeeleyLewinsohn et al, 1995; Reference Goodyer, Herbert and TamplinGoodyer et al, 2000). These ‘proximal’ psychosocial processes do not appear sufficient to account for all episodes. Less attention has been given to the potential causal contribution of neuroendocrine factors, although elevated corticosteroids increase the liability for affective illness (Reference Lewis and SmithLewis & Smith, 1983). Are there individual differences in these steroids which could increase the risk of MDD either alone or in the presence of other psychosocial factors? A prospective study of post-pubertal adolescents at high risk for psychopathology indicated that dehydroepiandrosterone (DHEA) hypersecretion at 08.00 h tends to be followed by onset of major depression (Reference Goodyer, Herbert and TamplinGoodyer et al, 2000). This paper reports a more extensive analysis of the relationship between the timing of specific types of negative experience, additional measures of individual differences in endocrine activity and the subsequent onset of MDD.
METHOD
Population ascertainment
One thousand, four hundred and fifty-one 12- to 16-year-olds from three secondary schools in Cambridge took part. All parents were sent three screening questionnaires: a demographic form, lifetime exit events (Reference Goodyer and AlthamGoodyer & Altham, 1991) and the EAS (Emotionality, Activity, Sociability) temperament questionnaire focused on the adolescent (Reference Buss and PlominBuss & Plomin, 1984). The higher the score, the greater the level of the dimension. Seven hundred and thirty-two (50%) of 1451 parents returned the screens intact.
A life events screening questionnaire was completed by 1409 adolescents during school time, 42 being absent or unwilling. Also 1394 (99%) agreed to complete a 38-item checklist of psychological symptoms covering current mood, feelings and anxieties condensed from four questionnaires: Mood and Feelings (Reference Kent and VostanisKent & Vostanis, 1997), Revised Manifest Anxiety Scale (Reference Reynolds and PagetReynolds & Paget, 1983), Rosenberg Self Esteem Scale (Reference RosenbergRosenberg, 1965) and the Leyton Obsessional Inventory (Reference Berg, Rapoport and FlamentBerg et al, 1986).
There was no difference in the mean scores for adolescents whose parents did and did not return the questionnaires: returnees (n=690), 21.3 (s.d.=11.4) v. non-returnees (n=704), 21.6 (s.d.=10.8) (t=0.4, NS). There was also no difference in the number of life events reported by adolescents whose parents did or did not return forms (two or more events: returnees 410/690 (59%) v. non-returnees 411/704 (58%)). Since there were no parent data from non-returnees, any ascertainment bias on demographic features or family characteristics is not known. From this population subjects were chosen who met criteria for high risk for psychopathology.
Definition of high risk
Recent undesirable life events exert their greatest risk when they occur as additive experiences in multiples greater than 2 over the previous 12 months (Reference Goodyer and GoodyerGoodyer, 1995). Since it is not known which combination of risk factors is most likely to result in subsequent onsets, a range of risks were combined in the screen procedure. A subject at high risk was defined as any adolescent with two or more risk factors from the following list:
-
(a) two or more moderately to severely undesirable life events in the previous 12 months;
-
(b) current marital disharmony or past marital breakdown;
-
(c) two or more lifetime exist events (bereavement and/or permanent separation) of personal significance (relative or friend) to the adolescent;
-
(d) high (> 80 percentile) emotionality.
In addition, the presence of a history of parental psychiatric disorder by itself qualified as high risk.
Exclusion criteria were: adolescents with chronic and potentially life-threatening medical illnesses, including epilepsy, cancer, heart disease; learning difficulties that required formal special educational assistance (n=5); or limited understanding of English (n=3). There were no subjects with a potentially life-threatening illness.
Study entrants
Informed consent was given by 180 of the 250 invited (72%). There were no differences in risk factors, age or gender between those who consented and those who did not.
At entry all subjects completed a semi-structured interview, the Kiddie—SADS (Schedule for Affective Disorders and Schizophrenia) patient version (Reference Kaufman, Birmaher and BrentKaufman et al, 1997), to ascertain whether the subject had been free of mental illness over the previous 3 months. This assessment took place within 4 to 8 weeks of the screen procedures. Seven subjects were excluded. Individuals with depressive symptoms but without social or personal impairment were not excluded. One subject subsequently withdrew. Subjects were classified as either pre- or post-pubertal (Tanner stage > 1). One hundred and seventy-one subjects (age 12 years 2 months to 16 years 6 months — mean 13 years 6 months), completed both psychosocial and endocrine assessments at follow-up.
The current medications of all eligible subjects were recorded. Neither beta-methasone nor salbutamol had a significant effect on either salivary cortisol or DHEA levels (Reference Goodyer, Herbert and TamplinGoodyer et al, 2000).
Measures
Subjects completed a semi-structured psychosocial interview evaluating recent undesirable and desirable life events and friendships (Reference Goodyer, Herbert and TamplinGoodyer et al, 1997). The onset of each event that had occurred over the previous 12 months was dated to within 4 weeks. Undesirable events (those carrying a moderate to severe degree of negative impact) were categorised into four mutually exclusive groups as follows:
-
(a) Danger to self: expectation or occurrence of physical threat to the child, such as illness or accidents, involvement in a household or community disaster or being the subject of a personal attack.
-
(b) Danger to others: expectation or occurrence of physical threat where the person exposed is a parent, sibling, friend or significant other (e.g. teacher, first-degree relative, neighbour).
-
(c) Disappointments: failure of a previously held set of expectations and/or hopes (e.g. to the self includes breakdown of boyfriend/girlfriend relationship, examination failure; to another includes loss of job, new financial difficulties, extramarital affair).
-
(d) Loss: permanent state of no further contact with a valued other (includes only death and permanent separations).
Mood and Feelings Questionnaire
The self-report questionnaire on recent depressive symptoms used was the Mood and Feelings Questionnaire (MFQ), which is designed to cover the symptom areas as specified in DSM—IV (American Psychiatric Association, 1994) for MDD in children (Reference Kent and VostanisKent & Vostanis, 1997).
Other self-reports used at baseline in this population for current anxious and obsessional symptoms, ruminative cognitive style and lower self-esteem, have already been shown to exert no significant independent effects on onset of subsequent major depression, once the effects of high depressive symptoms have been taken into account (Reference Goodyer, Herbert and TamplinGoodyer et al, 2000).
Saliva samples
Subjects provided samples of saliva at 08.00 h and 20.00 h over 4 consecutive days within a week of the interview. They were instructed not to clean their teeth but to wash out their mouths before taking samples. Saliva was dribbled directly into plastic tubes, without using aids to salivation or swabs. Samples were stored in the subject's own freezer at less than 0°C.
Reassessment at 12 months
A positive response on the Kiddie—SADS short interview resulted in the full psychiatric assessment (n=48 of 171). An episode of major depression was deemed present if at any time over the previous 12 months a subject met DSM—IV criteria. Life events were re-evaluated, thereby giving a 24-month period (12 months before entry and a further 12 up to reassessment) over which events had been recorded. For those subjects who subsequently developed major depression, events were divided into before and after onset of the episode. Onset was taken as the best point estimate to the nearest week from the date of the interview, when depressive signs and symptoms were present and resulted in discernible worsening in personal and/or social functioning.
Onsets occurred throughout the 11 months after the first month of entry into the study. Thus, the 12-month period counted before onset is not the same 12 months for every case, although there is > 80% overlap in the time period covered for all cases. The event data in the cases is compared with the events that occurred in the non-cases group for the 12 months between entry and follow-up. The timing of events for non-cases was taken as the number of months prior to the date of reassessment.
Hormone measures
Each sample was assayed separately for cortisol and DHEA. Cortisol was measured by enzyme-linked immunosorbent assay (ELISA) on 20 μl samples of saliva without extraction (antibody Cambio, Cambridge, UK). Intra-assay variation was 5.7%; inter-assay variation was 5.6%. Dehydroepiandrosterone was measured by validated radioimmunoassay on 333 μl samples after extraction into hexane/ether (4:1) (antibody Bioclin, Cardiff, UK). Intra-assay variation was 5.1%, inter-assay variation was 7.4%. There is a good correlation between plasma and salivary levels for both steroids (Pearson's r=0.6 for cortisol; 0.9 for DHEA (Reference Goodyer, Herbert and AlthamGoodyer et al, 1996). Results are reported in ng/ml.
There were two indices of endocrine activity. The mean level of steroid at each time point was calculated from the four values obtained from each subject. This gave four indices at entry, and another four at follow-up (mean cortisol and DHEA at 08.00 h and 20.00 h).
A second index was also used, derived following a reconsideration of how best to reflect individual variation in hormone dynamics in samples collected over 4 days. This was based on whether or not a ‘peak’ value of a steroid occurred in any of the four samples. A peak was defined a priori as an extreme level, taken as > 80th percentile of the mean. Subjects were classified as ‘peak positive’ if they had one or more level greater than the 80th percentile of the daily mean of the group on 1 or more days of the 4-day sampling period.
The 80th percentile level for cortisol was calculated for males and females separately. For DHEA the 80th percentile was calculated for each age (in years 12-16) as well as for each gender.
Statistical analysis
Group comparisons were carried out using exact statistics for categorical data, and Bonferroni-corrected analysis of variance on log-transformed continuous data. Subjects were grouped for age and gender at entry and conditional fixed-effects logistic regression was used to determine the best fit for psychoendocrine variables that predicted the subsequent onset of major depression.
RESULTS
Characteristics of risk status
Of the subjects, 180 (73 boys, 107 girls) met criteria for high risk at entry. They ranged in age from 12 to 16 years (12 years n=29 (16%); 13 years n=53 (29%); 14 years n=41 (23%); 15 years n=44 (24%); 16 years n=13 (7%)). There was no difference between the proportion of boys and girls by age (χ2 (4)=5.043, P=0.283).
Onset of MDD
Thirty (18%) of the 171 reassessed subjects had experienced an onset of DSM—IV major depression over the follow-up period (cases). The remainder (non-cases) did not meet DSM—IV criteria for MDD during the follow-up period.
Life events
Burden of events
A comparison was made between the proportion of cases and non-cases who experienced none to four undesirable events focused on the self, prior to onset (MDD cases) or in the 12 months' follow-up (non-MDD cases). There were no differences between the groups overall, or analysed separately for males and females: overall, MDD cases v. non-MDD cases: none (3 (10%) v. 15 (11%)), one (9 (30%) v. 51 (36%)), two (11 (37%) v. 50 (35%)), three (7 (23%) v. 21 (15%)), four or more (0 v. 4 (3%)), exact test, P=0.781, indicating no association between the general burden of events and onset of major depression. There was no effect of age for either gender.
Timing of events
The frequency of moderate to severe undesirable events per month was <1 for both MDD cases and non-MDD cases. Events were therefore classified into four temporal groups: 1 month; 2-3 months; 4-6 months and 7-12 months, respectively, before onset (cases) or before follow-up (non-cases). The proportions of cases and non-cases who experienced one or more of any type of undesirable event in each time period is different between the two groups (χ2 (3)=16.08, P=0.0011).
MDD cases were more likely than non-MDD cases to experience events in the preceding month only (18/30 (60%) v. 31/141 (22%), exact test, P=0.0001, odds ratio 5.4; 95% CI 2.4-12.2). There were no gender differences in those reporting one or more events in this 1-month period. By contrast, significantly more girls than boys reported experiencing one or more events over the rest of the 2- to 12-month period (exact test, P=0.028, odds ratio=2.5; 95% CI 1.17-5.49).
Types of events
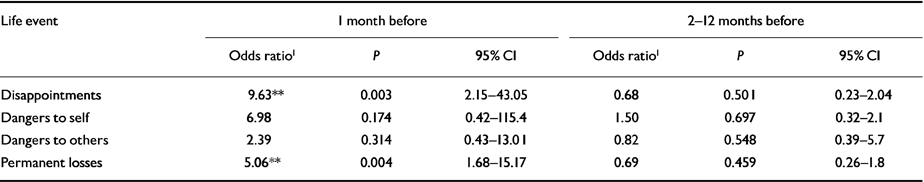
A conditional fixed-effects logistic regression was carried out to determine the best fit between the type and timing of events and subsequent MDD. The results are shown in Table 1.
Table 1 Odds ratios for the onset of DSM-IV major depressive disorder in 171 adolescents at high risk for psychopathology after exposure to different types of life events 1 and 2-12 months before onset
| Life event | 1 month before | 2-12 months before | ||||
|---|---|---|---|---|---|---|
| Odds ratio1 | P | 95% CI | Odds ratio1 | P | 95% CI | |
| Disappointments | 9.63** | 0.003 | 2.15-43.05 | 0.68 | 0.501 | 0.23-2.04 |
| Dangers to self | 6.98 | 0.174 | 0.42-115.4 | 1.50 | 0.697 | 0.32-2.1 |
| Dangers to others | 2.39 | 0.314 | 0.43-13.01 | 0.82 | 0.548 | 0.39-5.7 |
| Permanent losses | 5.06** | 0.004 | 1.68-15.17 | 0.69 | 0.459 | 0.26-1.8 |
Only disappointments and permanent losses in the first month before interview/onset were associated with subsequent MDD. The analysis was repeated with the total number of events over the 12 months as a further factor. There was no change in the final model (total number of events OR=1.1, P=0.824). The analysis reported in Table 1 was repeated, excluding dangers to others (i.e. focusing on self-related events only). The findings remained the same.
Hormones
Mean levels
There was a large diurnal variation in mean cortisol (am:pm ratio 12:8) and a much smaller one in DHEA (am:pm ratio 2:1). Mean salivary cortisol was higher in girls than boys at 08.00 h (F(1172)=6.24, P=0.013 (Bonferroni)) but not at 20.00 h. Mean salivary DHEA was also higher in girls than boys at 08.00 h (F(1164)=6.23, P=0.014) and at 20.00 h (F(1164)=4.23, P=0.041). Age was a significant covariate in both the DHEA analyses (levels of DHEA increase with age).
Peaks
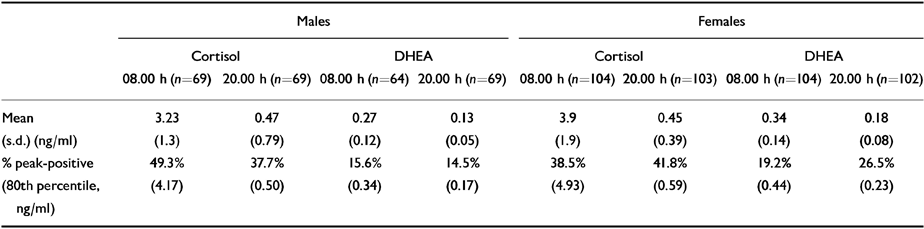
The proportions of peak-positive subjects (yes/no) for cortisol and DHEA are shown in Table 2, together with average mean levels over 4 days. The findings show that there were no significant differences in the proportion of peak-positive subjects at 08.00 h for either hormone in either males or females.
Table 2 Mean levels (ng/ml) of cortisol and dehydroepiandrosterone (DHEA) at entry and % of subjects with one or more daily peaks >80th percentile of the mean
| Males | Females | |||||||
|---|---|---|---|---|---|---|---|---|
| Cortisol | DHEA | Cortisol | DHEA | |||||
| 08.00 h (n=69) | 20.00 h (n=69) | 08.00 h (n=64) | 20.00 h (n=69) | 08.00 h (n=104) | 20.00 h (n=103) | 08.00 h (n=104) | 20.00 h (n=102) | |
| Mean | 3.23 | 0.47 | 0.27 | 0.13 | 3.9 | 0.45 | 0.34 | 0.18 |
| (s.d.) (ng/ml) | (1.3) | (0.79) | (0.12) | (0.05) | (1.9) | (0.39) | (0.14) | (0.08) |
| % peak-positive | 49.3% | 37.7% | 15.6% | 14.5% | 38.5% | 41.8% | 19.2% | 26.5% |
| (80th percentile, ng/ml) | (4.17) | (0.50) | (0.34) | (0.17) | (4.93) | (0.59) | (0.44) | (0.23) |
Those who were peak-positive for cortisol at 08.00 h and 20.00 h were significantly older than those who were not (08.00 h, 13.99 (s.d.=1.22) v. 13.53 (s.d.=1.14) F(1172)=6.25, P=0.013 (Bonferroni); 20.00 h, 14.98 (s.d.=1.21) v. 13.54 (s.d.=1.15) F(1172)=5.01, P=0.017 (Bonferroni). There were no age differences between DHEA peak-positive and peak-negative groups.
For cortisol, 71 (41.3%) had no peaks at either time point, 32 (18.6%) had morning only, 27 (15.7%) evening only, and 42 (24.4%) had both. For DHEA, the figures were 112 (67%), 18 (11%), 25 (15%) and 11 (7%), respectively. There were no significant differences in these proportions between males and females. There was no association between the proportions of subjects who were cortisol and DHEA peak-positive at either time point.
Peak hormones, life events and depressive symptoms at entry
There were no associations between peak positive status and any type of event either at 1 month or 2-12 months before onset or during follow-up. Neither were there any associations with the number of events. Mean scores on the MFQ scale were not significantly different between peak-positive and peak-negative groups for cortisol or DHEA at either time point.
Peak hormones, life events and subsequent MDD
Comparisons were made between MDD cases and non-MDD cases for the proportion of subjects with peak hormones. A significant association was found for peak cortisol at 08.00 h (18/28 (64%) v. 52/137 (38%), exact test P=0.012, odds ratio 2.9, 95% CI 1.3-6.7), and peak DHEA at 20.00 h (11/27 (41%) v. 25/136 (18%), exact test P=0.02, odds ratio 3.0, 95% CI 1.3-7.3) at entry, and subsequent MDD.
A conditional fixed-effects logistic regression was computed with case/non-case as the response variable and life events at one month, mood and feelings scores at entry, mean salivary cortisol and DHEA at both time points at entry, as the predictors. This showed that only disappointing and loss events contributed to the model. A second model was computed replacing the absolute hormone levels with the binary variable (peaks yes/no) for cortisol and DHEA at both time points. This model is shown in Table 3.
Table 3 Relative contribution of undesirable life events, mood and feelings and peak hormone-positive subjects at entry to onset of major depression

| Predictor variables present before onset | Odds ratio1 | P | 95% CI |
|---|---|---|---|
| Disappointments 1 month before onset | 58.9 | 0.0001 | 7.0-495.5 |
| Permanent losses 1 month before onset | 8.8 | 0.004 | 2.02-38.6 |
| Cortisol peaks 08.00 h | 7.1 | 0.008 | 1.67-30.4 |
| DHEA peaks 20.00 h | 4.2 | 0.02 | 1.2-14.7 |
| Lower mood and feelings | 1.1 | 0.051 | 1.00-1.13 |
The findings show that the onset of subsequent MDD is associated with being cortisol peak-positive at 08.00 h (OR=7.1; P=0.008, 95% CI=1.67-30.4); and DHEA peak-positive at 20.00 h (OR=4.2, P=0.02, 95% CI=1.2-14.7). The effects of both disappointments and loss events in the one month closest to onset remain highly significant, with higher self-report mood and feeling scores also being retained. The relationship between mean levels and peaks for both hormones was further examined by repeating these analyses with both means and peaks in the model. Absolute levels of either hormone did not contribute to this model.
DISCUSSION
Personal disappointments, loss and subsequent MDD
The findings in this paper suggest that, in adolescents at high risk for psychopathology, there are both psychosocial and endocrine contributions to the precursors for major depression. So far as recent undesirable life events are concerned, only those in the preceding month are associated with the onset of disorder. There is no evidence that this proximal process is influenced by the number of events in the preceding 11 months, or that it is dependent on social connectivity between similar types of events over this time frame. Both disappointments, the majority of which are events dependent on adolescents' own behaviour, and permanent losses, which are independent, contributed to onset. The gender difference in reporting of negative events is confined solely to events that are not associated with onset of disorder. This conclusion is limited however by the small number of boys with depression. The present evidence suggests that life events are part of the antecedent process of major depression for both high-risk boys and girls. These findings differ from those that suggest gender-differentiated effects of life events in the onset of subsequent disorder (Reference Peterson, Sarigiani and KennedyPetersen et al, 1991).
A previous paper showed that the onset of MDD occurs in >90% of cases from the high-risk population with antecedent ongoing psychosocial adversities (Reference Goodyer, Herbert and TamplinGoodyer et al, 2000). Thus, both long-standing and highly proximal psychosocial adversities contribute to onset in this adolescent population. This social model is similar to that previously described for adults and high-school students (Reference Brown, Bifulco and HarrisBrown et al, 1987; Reference Lewinsohn, Rohde and SeeleyLewinsohn et al, 1998).
Of the 30 episodes of MDD over the 12-month period, only 16 (53%) were preceded by either a disappointing or a loss event. Thus, nearly half of the episodes arise in high-risk individuals who are not exposed to these immediate proximal experiences. Provided that the recognition of proximal events is accurate, this suggests that there may be other factors predisposing to disorder.
Antecedent depressive symptoms
A post hoc examination of the characteristics of this high-risk sample showed no difference in MFQ scores at entry between those onsets with identified proximal events (‘events-driven’) 26.47 (s.d.=11.77) and those without 23.2 (s.d.=7.47). There were no differences in the psychosocial risk profiles of the two groups. Neither were event-driven cases significantly older or more likely to be girls.
However, there are additive effects between current mood at entry and the impact of proximal life events, further confirming that higher levels of depressive symptoms are associated with subsequent onset of MDD in this high-risk group (Reference Lewinsohn, Gotlib and SeeleyLewinsohn et al, 1995). In a recent longitudinal study, depressive symptoms over 4 years increased the risk for internalising disorder, with parent-child disagreements exerting their effects indirectly by increasing the level of depressive symptoms over time (Reference Rueter, Scaramella and WallaceRueter et al, 1999). It is possible that the non-event-driven cases occurring in the high-risk sample reported in this paper had increasing internalising symptoms over the 12-month follow-up period and are examples of slower-onset disorder with no provoking proximal events. This leads to the tentative conclusion that highly proximal events may exert their psychopathological effects by increasing an already rising level of depressive symptoms above clinical threshold.
Peak hormones and subsequent MDD
The second set of questions related to the putative role of cortisol and DHEA in the onset of major depression. It has already been suggested that mean salivary DHEA at 08.00 h is associated with subsequent MDD in a combined analysis of both low-and high-risk adolescents (Reference Goodyer, Herbert and TamplinGoodyer et al, 2000). This paper introduces a second index of antecedent hormone activity, defined as whether or not a subject had a ‘peak’ that lay at or above the 80th percentile of the mean value for the group for each gender (and age for DHEA). This type of measure has been used to estimate variability or ‘reactivity’ in cortisol in children (Reference GunnarGunnar, 1998). Measuring peaks gives a different perspective on endocrine function from determining mean values. The latter will not delineate subjects with extreme day-to-day variation of either hormone. Peak, rather than basal salivary levels, may thus reflect an additional peripheral index of hypothalamic—pituitary—adrenal axis dysregulation. Cortisol has a lower affinity for type 2 than type 1 corticoid receptors and a distinct population of these receptors might be activated by peak levels (Reference Reul and de KloetReul & de Kloet, 1985). There are also specific type 2 associated effects such as those on glucose transport, and suppressant effects on neuronal excitability (Reference Joels and de KloetJoels & de Kloet, 1994). Measures reflecting steroid reactivity may be an additional index of psychological difficulty in young people. For example, in well children it is morning cortisol levels in the highest interquartile range, rather than the daily mean, that are associated with a solitary and negative affective behavioural style (Reference GunnarGunnar, 1998).
This paper shows, for the first time, that the occurrence of peaks in morning cortisol is predictive of subsequent MDD in high-risk adolescents. Peaks in evening DHEA were also associated with subsequent MDD. There is no relation between peaks for either hormone, higher self-report depression scores and the occurrence of life events, further suggesting that these factors may be independent. Peaks were also more likely in older high-risk adolescents of either gender. The origins of individual variation in peak levels for both hormones may arise in more distal adverse environments and/or from genetic influences.
The validity of the peak measure requires further investigation. Only 4 days of saliva collection was undertaken and it is unclear whether this is sufficient to obtain a representative sample of subjects liable to ‘peak’ levels. It also remains to be determined whether peaks in morning cortisol and evening DHEA are of psychopathological significance only in high-risk adolescents.
Hormone reactivity to environmental demands
The current design is not an adequate test of a possible physiological reactivity model where hour-to-hour variation can be a function of minor events or hassles in people's lives rather than major events in recent weeks. Such rapid changes require measurement of hormones before and within 30-60 minutes or so after the stimulus. There is evidence that cortisol reactivity does occur when subjects are put into stressful circumstances, particularly those that are associated with an increase in negative mood (Reference van Eck, Berkhof and Nicolsonvan Eck et al, 1996). There is also evidence suggesting an association between higher cortisol levels and specific impairments in verbal declarative memory, implying a potential neural basis for the effect of cortisol peaks on the liability for psychopathology (Reference Newcomer, Selke and MelsonNewcomer et al, 1999). Whether DHEA exhibits similar demand characteristics of this nature is not known. The functional effects of steroid variability on everyday cognitive performance, and particularly memory, in at-risk populations require further investigation.
Puberty, hormones and subsequent MDD
There may be a second set of endocrine risk factors for MDD associated with puberty. For example, it is postulated that rising levels of testosterone and/or oestrogen are themselves related to increased risk for MDD in girls (Reference Angold, Costello and ErkanlAngold et al, 1999). Since nearly all our subjects were post-pubertal, we cannot assess this risk in relation to that presented by peaks in cortisol or DHEA. As for the latter, it is well known that DHEA levels increase during puberty in both boys and girls, whereas cortisol levels remain relatively unaltered (Reference Kroboth, Salek and PittengerKroboth et al, 1999; Reference ParkerParker, 1999). Levels of (or peaks in) DHEA may, therefore, be another endocrine index of maturation, and this may account for the relationship we find between DHEA and subsequent MDD. The findings in this paper suggest a putative causal role for cortisol and DHEA that is not a consequence of highly proximal recent life events or subclinical depressive symptoms. Further research into the origins of individual differences in steroid variability for each gender is required.
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
▪ Highly proximal (within 1 month) disappointments or personal losses are associated with the onset of major depressive disorder in high-risk adolescents.
-
▪ Daily peaks of morning cortisol or evening dehydroepiandrosterone also predict onset.
-
▪ The origins of these hormonal predictors are not related to the immediate psychosocial environment.
LIMITATIONS
-
▪ The findings may not generalise to adolescents not at high risk as defined.
-
▪ The findings are constrained by the number of daily salivary samples.
-
▪ The number of cases prevents more detailed analyses of gender differences.
ACKNOWLEDGEMENTS
This work was supported by a project grant from the Wellcome Trust and completed within the Medical Research Council cooperative in Brain Behaviour and Neuropsychiatry.






eLetters
No eLetters have been published for this article.