The involvement of service users in research is increasingly acknowledged as important within the mental health field. The term ‘user-led research’ refers to research where service users control all stages of the research process, including design, data collection and analysis, writing-up and dissemination (Reference RoseRose, 2003). Service users, rather than being the objects of research, become active agents in decisions about the research process. This benefits the research by ensuring that the work done is relevant to the concerns of service users. In addition, the rapport developed by user interviewers can lead to the collection of data not otherwise accessible. The research outlined in this paper was conducted by two user researchers (L.P. and M.K.). They met regularly with a steering committee of further service users and together they made decisions about the topic and design of the study, and conducted all stages of the research into recovery from psychosis. Research supervision was provided by clinical psychologists (S.N., M.W. and A.P.M.) with experience of research methods, data analysis and dissemination of research findings.
With increasing interest in the concept of recovery from psychosis it is useful to examine the background to this. Historically, the application of the medical approach, as a means of understanding mental health problems, meant that ‘recovery’ in terms of symptom absence was viewed as unlikely. The prognosis for someone with a diagnosis of schizophrenia, for example, was poor and individuals were often provided with little hope about their future.
However, the 1980s saw the publication of a number of first-hand accounts of recovery from mental distress (Reference DeeganDeegan, 1988; Reference LeeteLeete, 1989; Reference UnzickerUnzicker, 1989), highlighting the unique nature of the experience and characterising it as an ongoing process rather than an end-result. These accounts provided the basis for the growing recognition that recovery does not simply mean the absence of symptoms, cure or a return to the former self. Definitions include the concept of personal change in which the development of a new sense of self can lead to the establishment of a fulfilling life, whether or not symptoms are present (for definitions see Reference DeeganDeegan, 1988; Reference AnthonyAnthony, 1993; Reference Andresen, Oades and CaputiAndresen et al, 2003). In this context, the medical approach, which relies primarily on pharmacological interventions, is seen as limiting, as it does not address the wider personal, psychological and social dimensions so central to the broader conceptualisation of recovery.
The concept of recovery was promoted further in the 1990s by Anthony (Reference Anthony1993) who raised professional awareness of the need for more recovery-orientated mental health services. Initially these ideas were more influential in other countries, such as the USA and New Zealand, but more recently there has been growing recognition of the need for more recovery-orientated services in Britain (Reference Allott, Loganathan and FulfordAllott et al, 2002; Reference Turner-Crowson and WallcraftTurner-Crowson & Wallcraft, 2002; Reference Repper and PerkinsRepper & Perkins, 2003). The wider conceptualisation of recovery promoted by individual service users and practitioners has been acknowledged as important by the British government in recent years. A policy document published in November 2001, outlining the government's vision for mental healthcare, was significantly entitled The Journey to Recovery and claimed ‘ Services of the future will talk as much about recovery as they do about symptoms and illness’ (Department of Health, 2001). This was accompanied by a shift in policy, which focused on combating social exclusion for those with serious mental health problems. The change in emphasis at a political level has strengthened the case for those calling for more recovery-orientated services in Britain. However, if these are to be developed in a way that is meaningful to service users there is a need for greater understanding of recovery from this perspective.
Postmodernist qualitative research methods are particularly suited to exploring the individualised journey of recovery. A number of qualitative studies have analysed narratives of recovery stories and data from semi-structured interviews. These studies have identified common themes, including the importance of acceptance, hope, redefining of self, empowerment, social support and establishment of meaning and purpose in life (Reference SmithSmith, 2000; Reference RidgewayRidgeway, 2001; Reference TandyTandy, 2003; Reference Andresen, Oades and CaputiAndresen et al, 2003; Reference WarrenWarren, 2003). The emphasis has been on the importance of developing coping mechanisms to manage symptoms more effectively in order to lead a fulfilling life rather than their complete eradication. It is also recognised that people are recovering not simply from the debilitating effects of the symptoms themselves, but from the wider impact that mental distress and using mental health services has on their sense of self and ability to participate equally in society. Stigma and discrimination adversely affect those experiencing mental health problems, creating negative self-beliefs and leading to unemployment and loss of social networks. All these experiences need to be addressed holistically when promoting a person's recovery. The results of a survey conducted by Mind suggested that recovery meant different things to different people and that helpful strategies included talking to family and friends, eating well, working and volunteering, hobbies and physical activity (Reference Baker and StrongBaker & Strong, 2001).
Building on earlier qualitative work, the aim of this study was to carry out user-led research looking at recovery from psychosis from a service user perspective. The objectives were to explore the subjective experience of people's recovery from psychosis, to define recovery from a user perspective, to identify themes associated with the recovery process from individual accounts and to disseminate the findings so they can inform future practice.
Method
Participants
The seven people (five male, two female) interviewed were aged between 18 and 65 years; six were White and one was of mixed race. The participants were recruited through mental health groups, including user groups, and all had personal experience of psychosis and of using mental health services.
Design
A steering committee of service users was set up to decide the topic, provide guidance on the design of the study and have input into the analysis. The study involved the use of semi-structured interviews, which focused on people's experience of psychosis and recovery. The chosen methodology was interpretative phenomenological analysis (IPA), which is a form of analysis that is particularly suited to the exploration of subjective experience. It is concerned with the participants’ perception of their experience and the sense they make of it themselves. However, IPA is also an interpretative form of methodology as it recognises the investigator's role in making sense of the participant's experience. As the process of analysis requires researchers to gain an ‘insider perspective’, this was helped by the fact that the researchers were service users with personal experience of recovery from psychosis (Reference Smith, Osborn and SmithSmith & Osborn, 2003).
Procedure
The semi-structured interviews lasted between 45 and 60 min, were audiotaped and transcribed verbatim.
Data analysis
Initially, in order to become familiar with the data, tapes were listened to and transcripts were read. Initial thoughts from the researchers were then recorded and the themes arising from the data were identified. Each researcher carried out this process independently for each transcript. The two researchers then met jointly to agree the themes. Finally, members of the steering committee were involved in deciding upon the final themes.
Results
The research suggests that recovery is a gradual and uneven process, occurring in stages involving turning points and milestones, without definitive end. It is a relative concept, which means different things to different people. Service users’ definitions of recovery include:
‘The normal function gained or regained point where I am able to re-engage with society, regain my economic independence’. (Interview 1)
‘Recovery means, what it means to me, well getting on the path where I am now, being able to go back to work, hold a job down, you know, carry on with other normal things what people can’. (Interview 2)
‘Just that I have got to get on with my life, getting married, getting a house, getting a job, to me that's recovery’. (Interview 3)
‘My understanding of recovery is basically you’re feeling inwardly all right’. (Interview 4)
‘Being stabilised, being well’. (Interview 5)
‘I think I see it as learning that psychiatry is not the only way of looking at things… I think for most of us when we come to psychiatry we see it as a benign and helpful institution that is going to get us right. And when we have been in a little while we find that it confines us. It keeps us as mentally ill people for the rest of our lives, you know. So first of all you have to realise that there is life beyond mental illness’. (Interview 6)
‘Learning to cope to accept that you hear voices or whatever your symptoms are. Recovery is… to be able to live with it. And like going up the ladder… but sometimes you get pushed down a few rungs’. (Interview 7)
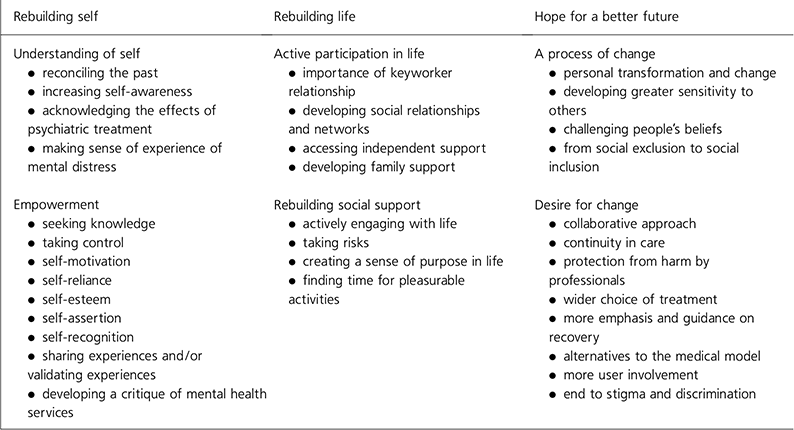
The following three key themes emerged from the research: the rebuilding of self, the rebuilding of life, and hope for a better future. Each sub-theme also had several smaller themes, and these are summarised in Table 1 and discussed in more detail below. Certain themes are illustrated using quotes from the participants.
Table 1. Key themes, sub-themes and smaller themes of recovery
| Rebuilding self | Rebuilding life | Hope for a better future |
|---|---|---|
| Understanding of self | Active participation in life | A process of change |
| • reconciling the past | • importance of keyworker relationship | • personal transformation and change |
| • increasing self-awareness | • developing greater sensitivity to others | |
| • acknowledging the effects of psychiatric treatment | • developing social relationships and networks | |
| • challenging people's beliefs | ||
| • making sense of experience of mental distress | • accessing independent support | • from social exclusion to social inclusion |
| • developing family support | ||
| Empowerment | Rebuilding social support | Desire for change |
| • seeking knowledge | • actively engaging with life | • collaborative approach |
| • taking control | • taking risks | • continuity in care |
| • self-motivation | • creating a sense of purpose in life | • protection from harm by professionals |
| • self-reliance | • finding time for pleasurable activities | |
| • self-esteem | • wider choice of treatment | |
| • self-assertion | • more emphasis and guidance on recovery | |
| • self-recognition | ||
| • sharing experiences and/or validating experiences | • alternatives to the medical model | |
| • more user involvement | ||
| • developing a critique of mental health services | • end to stigma and discrimination |
Rebuilding of the self
Mental distress frequently involves the loss of the sense of the self, often coupled with what can be a disempowering experience of mental health services. This research suggests that the rebuilding of the self is a key element to the recovery process. This involves both increasing understanding of the self and a process of empowerment.
Increasing understanding of the self
Many people identified issues relating to their problematic past that needed to be reconciled as they moved on. For example:
‘There is also a point that I have discovered in the past few months having run through my childhood stuff in counselling and sorted out long-standing things that I have been meaning to sort out. I’m now saying I can now step away from this and get on with other things’. (Interview 1 — smaller theme ‘reconciling the past’)
The research indicates that increased self-awareness is needed to progress recovery. This involves acknowledging the effects of psychiatric treatment and making sense of the experience of mental distress on one's own terms.
Empowerment
The research suggests that empowerment is central to the recovery process and people who experience psychosis employ a variety of strategies to empower themselves. They seek knowledge about their experience of psychosis that enables them to have more control. They become motivated to recover and learn to rely more readily on themselves. They seek out activities that increase their self-esteem which, in turn, enables them to assert their needs better. They learn to recognise their achievements. For some people sharing their experiences of psychosis with others has been important to their recovery and this, in some instances, can lead to them developing a critique of mental health services. For example:
‘The most positive has been finding the hearing voices group, talking to other voice hearers and realising that the sort of diagnostic process and the medical model isn't the only way of looking at things’. (Interview 6 — smaller theme‘sharing experiences/validating experiences’)
This critique can enable them to become more active in deciding what support, if any, they need from mental health services.
Rebuilding life
Social isolation is often an outcome of mental distress. This research suggests that the recovery process involves the rebuilding of life through rebuilding social support and active participation in life.
Rebuilding social support
This research suggests that professionals in mental health services and voluntary sector groups can also provide much needed social support, particularly when the individual is socially isolated. The ability to access independent support is beneficial to the recovery process. However, the development of wider social networks, including support from friends and family, is of considerable importance. For example:
‘I got ill and they [her parents] realised I was ill and then started reading literature about what I was going through so they understood what was happening. They… just don't see it as anything wrong with me really, just think its me and support me completely’. (Interview 3 — smaller theme‘developing family support’)
Active participation in life
The initial stage of the recovery process can involve a period of withdrawal but our research suggests that, although this may be beneficial initially, ultimately recovery requires active participation in life. This involves taking risks and suffering setbacks. The research points to the importance of voluntary work in creating a sense of purpose in life.
‘I spend most of my time working for the network… I go out and do training and we kick start the Hearing Voices groups in various towns and that sometimes you have a group to talk to a group of CPNs [community psychiatric nurses] or social workers’. (Interview 6 — smaller theme‘creating a sense of purpose in life’)
For some people employment is a goal and voluntary work can be a stepping stone towards this. For others voluntary sector work is an end in itself, a means of creating a meaningful role for themselves in life. It is also important to find time for pleasurable activities that enable relaxation.
Hope for a better future
Recovery involves our hopes for a better future, which involves a process of change and desire for change.
A process of change
This research suggests that recovery involves a process of personal transformation and change that includes developing a greater sensitivity to others. The process also involves challenging other people's beliefs about one's experience of mental distress and changing their attitudes about the possibility of recovery. Overall, the recovery journey involves a process from social exclusion to social inclusion
‘Basically it is a proof to me that I am returning to society rather than being in some sort of exile whether self-imposed or from outside’. (Interview 1 — smaller theme‘from social exclusion to social inclusion’)
Discrimination takes its toll on those who experience mental distress leading to unemployment, dependency on benefits and lack of social networks. The process of social inclusion is central to the recovery process and involves, among other things, better access to the social and economic world.
Desire for change
This research suggests that recovery involves the development of a more collectivist outlook and a desire to see changes in mental health services and society in general. In relation to mental health services, those interviewed recognised the need for a more collaborative approach, greater continuity in care, protection from harm by professionals, wider choice of treatment, more emphasis and guidance on recovery, alternatives to the medical model and more user involvement. At a societal level there was recognition of the problems caused by stigma and discrimination and a call for greater educational initiatives to raise awareness about mental health problems:
‘I think they [her friends] were very scared of it, hearing voices. They just don't understand it at all. Just think it's really bizarre to their experience and I think they think I might go and kill them or something. Just don't understand it at all. I think it's bad but I think there should be more education about it’. (Interview 3)
Discussion
Findings
These findings clearly demonstrate that recovery is a dynamic process, rather than a definitive end-point or cure. This study elucidates the process as a unique experience for every individual. Recovery is a relative concept that means different things to different people. The study suggests that recovery is not necessarily a linear process, but consists of turning points and milestones whereby key elements of the process interact with one another, facilitating the recovery process as a whole. However, the study also identifies common themes to the process of recovery that are evident throughout the data. These broadly fall under three key themes, each of which comprises two subordinate themes: rebuilding self (increasing understanding of self and empowerment); rebuilding life (rebuilding social support and active participation in life); and hope for a better future (a process of change and desire for change).
The findings of this study are consistent with other research that highlights recovery as a process (Reference DeeganDeegan, 1988; Reference LeeteLeete, 1989; Reference UnzickerUnzicker, 1989) and further validates the key themes identified here (Reference SmithSmith, 2000; Reference RidgewayRidgeway, 2001; Reference Andresen, Oades and CaputiAndresen et al, 2003; Reference TandyTandy, 2003; Reference WarrenWarren 2003). Finally, the survey by Mind (Reference Baker and StrongBaker & Strong, 2001) also supports the findings of this study. In accordance with previous studies (Reference Jacobson and GreenleyJacobson & Greenley, 2001), this study illustrates that recovery is dependent on both internal and external mechanisms of change. For example, in relation to hope for a better future, factors such as personal transformation and change, developing a critique of mental health services and increased self-awareness contribute to a more collectivist outlook and recognition of a need for changes within services.
Strengths and limitations
In what other ways did this study differ from previous work in the area of recovery? A steering committee of service users was commissioned which had a direct impact on the study undertaken. This allowed for a broader ‘user perspective’ which helped to counter personal bias from the primary investigators. Equally the steering committee also influenced the choice of methodology and design of the study, which perhaps helped to gain more insight into the participants’ subjective experiences of recovery. In addition, both primary researchers were also service users, and hence the research was genuinely user-led.
One of the limitations of this study was the small sample size, which may raise questions about whether or not these findings are generalisable. However, the aim of qualitative research is to explore subjective experiences rather than produce generalisable knowledge. Nevertheless, our own findings are consistent with other previous studies of the recovery process. Future research could address this by exploring specific questions, for example, examining the relationship of ethnicity to the recovery process, and include larger sample sizes. Indeed, we are currently conducting a larger quantitative study exploring these issues.
Implications
The study has a number of implications which are particularly relevant for psychiatry. These include the importance of promoting and encouraging active participation by service users and the need for strengthening key relationships with professionals who are able to engage in active dialogue with the service user. This study identified empowerment as a key theme and supported the views of Tew (Reference Tew2002), which are characterised by a collaborative working relationship built on trust, respect and equality. The following discussion provides suggestions for ways of addressing some of these issues, and how practitioners can actively facilitate a collaborative and trusting relationship.
An example of good practice in relation to empowerment might be in the case of a meeting to discuss a care programme approach (CPA). Although the attendance at CPA meetings is often routine for many mental health workers, it is worth remembering that it is usually only an annual event for many service users. Attendance can induce considerable anxiety in certain individuals and every attempt should be made to minimise their distress. Care should be taken over the choice of venue, providing a comfortable environment that is large enough to accommodate all those present without being too cramped. The service user should be advised beforehand that they can bring along an independent representative of their choice. This could be a family member, a close friend or a colleague. In addition, practitioners should also make every effort to ensure sufficient time is given to all parties present. Any points made and raised by those present should also be fed back to the contributor to ensure clarity and respect of an individual's opinion. This includes mental health professionals and service users alike.
The importance of continuity in care is pinpointed as another key factor for the improvement of services and advancement of meaningful relationships. Unfortunately, within mental health services there is not only a rapid turnover of staff but also in some instances expectations of practitioners that service users will be seen by many different doctors. It is worth considering whether on such occasions sufficient thought has been given to the implications for service users. Given the importance of meaningful key relationships as highlighted in this study, this inconsistency may not progress such an important aspect of care. However, it also has to be acknowledged that there are often numerous reasons for the lack of continuity in care (for example lack of resources or recruitment difficulties) that will not always make this possible; such problems could be shared with service users.
The study demonstrates a need for greater choice in available treatments and greater access to alternative options and models of care. This could include psychological, social and pharmacological therapeutic interventions thus enabling service users to make informed choices about the different options available and interventions that might best suit their needs. Information could be on hand to facilitate discussions about treatment options. Important information about outside voluntary organisations, self-help groups and other relevant literature would also help this process. There is also a need for access to stories of recovery, sources of inspiration and hope that will offer insight and knowledge of people's journeys of recovery and the recovery process as a whole. This last point has particular significance for psychiatry, as psychiatrists are well placed to offer service users specific information and encouragement on a variety of treatments and strategies to help progress recovery. More emphasis could be put on the possibility of recovery generally, offering service users a much more hopeful prognosis. One such example whereby practitioners could demonstrate more recovery-focused practice is when imparting the news of a clinical diagnosis. It is worth remembering that such knowledge can have major negative and damaging implications for service users if they do not have a proper understanding. However, if the diagnosis is sensitively explained this can help to highlight a course of treatment and might ultimately promote an individual's recovery.
Finally, the study reaffirms the importance of more individualised recovery care plans. This could be achieved in an official format via the CPA and include the three key themes identified in this research (rebuilding the self, rebuilding life and hope for a better future), thus reinforcing a recovery orientated approach. This will hopefully retain the relevance of a CPA to the service user perspective, with the emphasis placed on the goals and aspirations that the service user identifies as important to them. Equally, it will provide the opportunity to highlight sources of support and strategies that are of help and will work towards permanent life changes to allow for opportunities in the future. This study calls for services to become more recovery orientated and for those involved to work in collaboration, not only with service users and carers, but also across the various trusts and professional bodies; this can effect change, promote recovery and harness support and sharing of expertise.
The study highlights the problems around power-sharing and the predominance of the medical approach, along with professional expertise. The promotion and growth of user-led research will serve to highlight the ability of non-professionals to direct and undertake their own research. Hopefully, the benefits of user-led research will become more widely accepted and produce changes in service delivery, and this will cut to the heart of issues that are important to service users themselves, dispelling the preconceived beliefs of mental health professionals.
Declaration of interest
None.



eLetters
No eLetters have been published for this article.