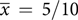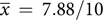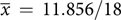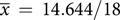Original Article
Risk factors for adverse events within one year after atrial septal closure in children: a retrospective follow-up study
- Gustaf Tanghöj, Petru Liuba, Gunnar Sjöberg, Estelle Naumburg
-
- Published online by Cambridge University Press:
- 18 December 2019, pp. 303-312
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Introduction:
Secundum atrial septal defect is one of the most common congenital heart defects. Previous paediatric studies have mainly addressed echocardiographic and few clinical factors among children associated with adverse events. The aim of this study was to identify neonatal and other clinical risk factors associated with adverse events up to one year after closure of atrial septal defect.
Methods:This retrospective case–control study includes children born in Sweden between 2000 and 2014 that were treated surgically or percutaneously for an atrial septal defect. Conditional logistic regression was used to evaluate the association between major and minor adverse events and potential risk factors, adjusting for confounding factors including prematurity, neonatal sepsis, neonatal general ventilatory support, symptomatic atrial septal defects, and pulmonary hypertension.
Results:Overall, 396 children with 400 atrial septal defect closures were included. The median body weight at closure was 14.5 (3.5–110) kg, and the median age was 3.0 (0.1–17.8) years. Overall, 110 minor adverse events and 68 major events were recorded in 87 and 49 children, respectively. Only symptomatic atrial septal defects were associated with both minor (odds ratio (OR) = 2.18, confidence interval (CI) 95% 1.05–8.06) and major (OR = 2.80 CI 95% 1.23–6.37) adverse events.
Conclusion:There was no association between the investigated neonatal comorbidities and major or minor events after atrial septal defect closure. Patients with symptomatic atrial septal defects had a two to four times increased risk of having a major event, suggesting careful management and follow-up of these children prior to and after closure.
Cardiac functions and aortic elasticity in children with inflammatory bowel disease: effect of age at disease onset
- Elif Erolu, Esra Polat
-
- Published online by Cambridge University Press:
- 22 January 2020, pp. 313-317
-
- Article
- Export citation
-
Aim:
Childhood onset inflammatory bowel disease is more aggressive and has rapidly progressive clinical course than adult inflammatory bowel disease. Early-onset inflammatory bowel disease has more severe clinical progression as a subspecialised group of monogenic inflammatory bowel disease. We studied cardiac functions and aortic elasticity in children with early- and late-onset inflammatory bowel disease in remission period.
Methods:Thirty-three paediatric patients were divided into subgroups according to age of disease onset (<10 and >10 years of age). Twenty-five healthy children were admitted as control group. M-Mode echocardiography and pulsed wave Doppler echocardiography were performed. Strain, distensibility, stiffness index of ascending, and abdominal aorta were evaluated.
Results:Interventricular septum (mm) and left ventricular end-systolic diameter were higher (6.9 ± 1.2, 26.2 ± 4.6) in early-onset inflammatory bowel disease patients than control patients (6.1 ± 1.27, 22.7 ± 4.12) (p = 0.050, p = 0.050). Mitral E/E′ ratio and myocardial performance index were increased in inflammatory bowel disease and early-onset inflammatory bowel disease groups than control group (p = 0.046, p = 0.04; p = 0.023, p = 0.033). Diastolic functions were found to be impaired in inflammatory bowel disease and early-onset inflammatory bowel disease groups according to control group, while there was no difference between late-onset inflammatory bowel disease and control groups in terms of diastolic functions. Mitral E/A ratio was lower in inflammatory bowel disease patients and early-onset inflammatory bowel disease patients (1.46 ± 0.32, 1.4 ± 0.21) than control patients (1.70 ± 0.27) (p = 0.013, p = 0.004). Aortic elasticity did not differ between groups.
Conclusion:Chronic low-grade inflammation has effects on left ventricular diameters and diastolic function in remission period. Aortic elasticity is not affected in our study groups.
P wave dispersion, Tpeak–Tend interval, and Tp-e/QT ratio in children with psoriasis
- Mecnun Çetin, İbrahim H. Yavuz, Mehmet Gümüştaş, Göknur Ö. Yavuz
-
- Published online by Cambridge University Press:
- 08 January 2020, pp. 318-322
-
- Article
- Export citation
-
Background:
Psoriasis is a chronic inflammatory, multi-system disease that often begins in childhood and characterised by inflammatory skin, nails, scalp, and joint manifestations. The inflammation in psoriasis may promote some effect on the cardiac conduction system.
Objective:The aim of this study is to investigate myocardial repolarisation anomaly on the conducting system in the paediatric psoriasis using P wave dispersion, Tpeak–Tend interval, and Tp-e/QT ratio.
Methods:Forty-two patients diagnosed with psoriasis and 37 age- and sex-matched healthy children were enrolled in the study. Electrocardiographic parameters in psoriasis and control group were recorded from an electrocardiogram for each patient.
Results:The results indicated that the parameters including Pdis, QTc dis, Tp-e dis interval, and Tp-e max/QTmax ratios, which are known to be key indicators for the prediction of severe atrial or ventricular arrhythmia and sudden cardiac death and also important parameters used as the indicators for the non-invasive evaluation of the transmural heterogeneity were significantly longer in the study group compared to the control group (p < 0.05).
Conclusions:This study includes the evidence linking psoriasis with increased myocardial repolarisation heterogeneity. These findings suggest that this patient population may be at an increased risk for arrhythmias. Our findings may be a basis for further studies.
Bovine jugular vein conduit versus pulmonary homograft in the Ross operation
- Parth M. Patel, Jeremy L. Herrmann, Mark D. Rodefeld, Mark W. Turrentine, John W. Brown
-
- Published online by Cambridge University Press:
- 18 December 2019, pp. 323-327
-
- Article
- Export citation
-
Objectives:
The Ross procedure involves using the native pulmonary valve for aortic valve replacement then replacing the pulmonary valve with an allograft or xenograft. We aimed to compare our age-matched experience with the bovine jugular vein conduit and the pulmonary homograft for pulmonary valve replacement during the Ross procedure in children.
Methods:Between 1998 and 2016, 15 patients <18 years of age underwent a Ross procedure using the bovine jugular vein conduit (Ross-Bovine Jugular Vein Conduit) at our institution. These patients were age-matched with 15 patients who had the Ross operation with a standard pulmonary homograft for right ventricular outflow tract reconstruction (Ross-Pulmonary Homograft). Paper and electronic medical records were retrospectively reviewed.
Results:The median age of the Ross-Bovine Jugular Vein Conduit and Ross-Pulmonary Homograft patients were 4.8 years (interquartile range 1.1–6.6) and 3.3 years (interquartile 1.2–7.6), respectively (p = 0.6). The median follow-up time for the Ross-Bovine Jugular Vein Conduit and Ross-Pulmonary Homograft groups were 1.7 years (interquartile range 0.5–4.9) and 6.8 years (interquartile range 1.9–13.4), respectively (p = 0.03). Overall, 5-year survival, freedom from redo aortic valve replacement, and freedom from pulmonary valve replacement were similar between groups.
Conclusion:The bovine jugular vein conduit and pulmonary homograft have favourable mid-term durability when used for right ventricular outflow tract reconstruction for the Ross operation. The bovine jugular vein conduit may be a suitable replacement for appropriately sized patients undergoing a Ross aortic valve replacement, though longer follow-up is needed.
The quality, understandability, readability, and popularity of online educational materials for heart murmur
- Derya Arslan, Mahmut Sami Tutar, Betul Kozanhan, Zafer Bagci
-
- Published online by Cambridge University Press:
- 26 December 2019, pp. 328-336
-
- Article
- Export citation
-
Objective:
Murmurs are abnormal audible heart sounds produced by turbulent blood flow. Therefore, murmurs in a child may be a source of anxiety for family members. Families often use online materials to explore possible reasons for these murmurs, given the accessibility of information on the Internet. In this study, we evaluated the quality, understandability, readability, and popularity of online materials about heart murmur.
Methods:An Internet search was performed for “heart murmur” using the Google search engine. The global quality score (on a scale of 1 to 5, corresponding to poor to excellent quality) and Health on the Net code were used to measure the quality of information presented. The understandability of the web pages identified was measured using the Patient Education Materials Assessment Tool (score range from 0 to 100%, scores below 70% reflect poor performance). The readability of each web pages was assessed using four validated indices: the Flesch Reading Ease Score, the Flesch–Kincaid Grade Level, the Gunning Frequency of Gobbledygook, and the Simple Measure of Gobbledygook. The ALEXA traffic tool was used to reference domains’ popularity and visibility.
Results:We identified 230 English-language patient educational materials that discussed heart murmur. After exclusion, a total of 86 web pages were evaluated for this study. The average global quality score was 4.34 (SD = 0.71; range from 3 to 5) indicating that the quality of information of most websites was good. Only 14 (16.3%) websites had Health on the Net certification. The mean understandability score for all Internet-based patient educational materials was 74.6% (SD = 12.8%; range from 31.2 to 93.7%). A score suggesting these Internet-based patient educational materials were “easy to understand”. The mean readability levels of all patient educational materials were higher than the recommended sixth-grade reading level, according to all indices applied. This means that the level of readability is difficult. The average grade level for all web pages was 10.4 ± 1.65 (range from 7.53 to 14.13). The Flesch–Kincaid Grade level was 10 ± 1.81, the Gunning Frequency of Gobbledygook level was 12.1 ± 1.85, and the Simple Measure of Gobbledygook level was 9.1 ± 1.38. The average Flesch Reading Ease Score was 55 ± 9.1 (range from 32.4 to 72.9).
Conclusion:We demonstrated that web pages describing heart murmurs were understandable and high quality. However, the readability level of the websites was above the recommended sixth-grade reading level. Readability of written materials from online sources need to be improved. However, care must be taken to ensure that the information of web pages is of a high quality and understandable.
Everolimus for cardiac rhabdomyomas in children with tuberous sclerosis. The ORACLE study protocol (everOlimus for caRdiac rhAbdomyomas in tuberous sCLErosis): a randomised, multicentre, placebo-controlled, double-blind phase II trial
- Erica V. Stelmaszewski, Daniella B. Parente, Alberto Farina, Anna Stein, Anthony Gutierrez, Antonio F. Raquelo-Menegassio, Carla Manterola, Carolina F. de Sousa, Carolina Victor, Dina Maki, Elias M. Morón, Fabiano F. de Abrantes, Fatima Iqbal, Jazmin Camacho-Vilchez, Joanna Jimenez-Pavón, Juan P. Polania, Lorenzo Thompson, Lygia Bonanato, Matthias Diebold, Maria V. C. P. Da Silva, Mariam W. J. Nashwan, Marianna A. G. Galvani, Osama E. A. Idris, Pierina Danos, Rocio Ortiz-Lopez, Rofida A. A. Mahmoud, Sergio Gresse, Jr, Karla L. Loss
-
- Published online by Cambridge University Press:
- 27 January 2020, pp. 337-345
-
- Article
- Export citation
-
Introduction:
Tuberous sclerosis complex is a rare genetic disorder leading to the growth of hamartomas in multiple organs, including cardiac rhabdomyomas. Children with symptomatic cardiac rhabdomyoma require frequent admissions to intensive care units, have major complications, namely, arrhythmias, cardiac outflow tract obstruction and heart failure, affecting the quality of life and taking on high healthcare cost. Currently, there is no standard pharmacological treatment for this condition, and the management includes a conservative approach and supportive care. Everolimus has shown positive effects on subependymal giant cell astrocytomas, renal angiomyolipoma and refractory seizures associated with tuberous sclerosis complex. However, evidence supporting efficacy in symptomatic cardiac rhabdomyoma is limited to case reports. The ORACLE trial is the first randomised clinical trial assessing the efficacy of everolimus as a specific therapy for symptomatic cardiac rhabdomyoma.
Methods:ORACLE is a phase II, prospective, randomised, placebo-controlled, double-blind, multicentre protocol trial. A total of 40 children with symptomatic cardiac rhabdomyoma secondary to tuberous sclerosis complex will be randomised to receive oral everolimus or placebo for 3 months. The primary outcome is 50% or more reduction in the tumour size related to baseline. As secondary outcomes we include the presence of arrhythmias, pericardial effusion, intracardiac obstruction, adverse events, progression of tumour reduction and effect on heart failure.
Conclusions:ORACLE protocol addresses a relevant unmet need in children with tuberous sclerosis complex and cardiac rhabdomyoma. The results of the trial will potentially support the first evidence-based therapy for this condition.
“Why and how did this happen?”: development and evaluation of an information resource for parents of children with CHD
- Alexis V. Hunt, Desiree C. K. Hilton, Charlotte E. Verrall, Kristine K. Barlow-Stewart, Jane Fleming, David S. Winlaw, Gillian M. Blue
-
- Published online by Cambridge University Press:
- 10 January 2020, pp. 346-352
-
- Article
- Export citation
-
Background:
The causes of CHD are complex and often unknown, leading parents to ask how and why this has happened. Genetic counselling has been shown to benefit these parents by providing information and support; however, most parents currently do not receive this service. This study aimed to develop a brochure to determine whether an information resource could improve parents’ knowledge about CHD causation and inheritance and increase psychosocial functioning.
Methods:In development, the resource was assessed against several readability scales and piloted. Parents of children attending preadmission clinic for surgery were included. Assessments occurred pre- and post-receiving the information resource using a purpose-designed knowledge measure and validated psychological measures.
Results:Participant’s (n = 52) knowledge scores increased significantly from the pre-questionnaire (
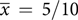 ${\overline x}\, = \,5/10$
, sd = 2.086) to post-questionnaire (
${\overline x}\, = \,5/10$
, sd = 2.086) to post-questionnaire (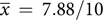 $\overline x\, = \,7.88/10$
, sd = 2.094, p < 0.001), with all aware that CHD can be caused by genetic factors after reading the brochure. Perceived personal control also increased from pre- (
$\overline x\, = \,7.88/10$
, sd = 2.094, p < 0.001), with all aware that CHD can be caused by genetic factors after reading the brochure. Perceived personal control also increased from pre- (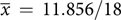 $\overline x\, = \,11.856/18$
, sd = 4.339) to post-brochure (
$\overline x\, = \,11.856/18$
, sd = 4.339) to post-brochure (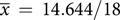 $\overline x\, = \,14.644/18$
, sd = 3.733, p < 0.001), and many reported reduced feelings of guilt. No negative emotional response to the brochure was reported. The information provided was considered relevant (88%), reassuring (86%), and 88% would recommend the brochure to other parents. However, some wanted more emotional support and assistance in what to tell their child.Conclusions:
$\overline x\, = \,14.644/18$
, sd = 3.733, p < 0.001), and many reported reduced feelings of guilt. No negative emotional response to the brochure was reported. The information provided was considered relevant (88%), reassuring (86%), and 88% would recommend the brochure to other parents. However, some wanted more emotional support and assistance in what to tell their child.Conclusions:Use of the information resource significantly enhanced parents’ knowledge of CHD causation and increased their psychosocial functioning. It is a valuable resource in the absence of genetic counselling; however, it should not replace formal genetic counselling when required.
Transplantation-free survival after Norwood surgery for hypoplastic left heart syndrome with aortic atresia: A Swedish national cohort study
- Annika Öhman, Milad El-Segaier, Gunnar Bergman, Katarina Hanseus, Torsten Malm, Boris Nilsson, Aldina Pivodic, Annika Rydberg, Sven-Erik Sonesson, Mats Mellander
-
- Published online by Cambridge University Press:
- 10 January 2020, pp. 353-360
-
- Article
- Export citation
-
Background:
Norwood surgery has been available in Sweden since 1993. In this national cohort study, we analysed transplantation-free survival after Norwood surgery for hypoplastic left heart syndrome with aortic atresia.
Methods:Patients were identified from the complete national cohort of live-born with hypoplastic left heart syndrome/aortic atresia 1993–2010. Analysis of survival after surgery was performed using Cox proportional hazards models for the total cohort and for birth period and gender separately. Thirty-day mortality and inter-stage mortality were analysed. Patients were followed until September 2016.
Results:The 1993–2010 cohort consisted of 208 live-born infants. Norwood surgery was performed in 121/208 (58%). The overall transplantation-free survival was 61/121 (50%). The survival was higher in the late period (10-year survival 63%) than in the early period (10-year survival 40%) (p = 0.010) and lower for female (10-year survival 34%) than for male patients (10-year survival 59%) (p = 0.002). Inter-stage mortality between stages I and II decreased from 23 to 8% (p = 0.008). For male patients, low birthweight in relation to gestational age was a factor associated with poor outcome.
Conclusion:The survival after Norwood surgery for hypoplastic left heart syndrome/aortic atresia improved by era of surgery, mainly explained by improved survival between stages I and II. Female gender was a significant risk factor for death or transplantation. For male patients, there was an increased risk of death when birthweight was lower than expected in relation to gestational age.
Erratum
Transplantation-free Survival after Norwood surgery for Hypoplastic Left Heart Syndrome with Aortic Atresia. A Swedish National Cohort Study. – ERRATUM
- Annika Öhman, Milad El-Segaier, Gunnar Bergman, Katarina Hanseus, Torsten Malm, Boris Nilsson, Aldina Pivodic, Annika Rydberg, Sven-Erik Sonesson, Mats Mellander
-
- Published online by Cambridge University Press:
- 04 February 2020, p. 361
-
- Article
-
- You have access Access
- HTML
- Export citation
Original Article
Effective myocardial perfusion and concomitant haemodynamic status determine the clinical diversity of anomalous left coronary artery from the pulmonary artery
- Amr A. Matoq, Takeshi Tsuda
-
- Published online by Cambridge University Press:
- 22 January 2020, pp. 362-368
-
- Article
- Export citation
-
Background:
Anomalous left coronary artery from the pulmonary artery is a rare congenital heart disease (CHD) with diverse clinical presentations despite the same anatomy. Factors determining this heterogeneous presentation are not well understood.
Method and Results:We retrospectively investigated 14 patients (12 females) who underwent surgical repair of anomalous left coronary artery from the pulmonary artery. These patients were divided into three groups based upon the severity of initial presentation: (1) severe, life-threatening condition (n = 5), (2) mild-to-moderate distress (n = 6), and (3) asymptomatic (n = 3). All patients presented with left ventricular dilation and retrograde flow in left coronary artery by echocardiogram. Eight patients in (1) and (2) presented with severe left ventricular dysfunction. All but one showed abnormal ECG consistent with myocardial ischemia or infarction. Asymptomatic patients had preserved left ventricular systolic function despite ischemic findings on ECG. In 13 patients after surgical repair, all but one normalised left ventricular geometry and systolic function, suggesting nearly full myocardial recovery upon improvement of myocardial perfusion; 8 patients had residual echogenic papillary muscle with variable degree of mitral regurgitation.
ConclusionsEvidence of myocardial ischemic injury was present in all patients with anomalous left coronary artery from the pulmonary artery regardless of their initial presentation. Retrograde flow in left coronary artery, implying collateral vessel development from right coronary artery to left coronary artery, was noted in all patients, yet only few patients had preserved systolic function at the time of diagnosis. The balance between effective myocardial perfusion and a deleterious fistulous flow provided by these collaterals and the simultaneous haemodynamic status are what determine the clinical diversity of anomalous left coronary artery from the pulmonary artery.
Changes in valvular regurgitation in mid-term follow-up of children with first attack acute rheumatic fever: first evaluation after the updated Jones criteria
- Muhlike Güler, Fuat Laloğlu, Naci Ceviz
-
- Published online by Cambridge University Press:
- 10 January 2020, pp. 369-371
-
- Article
- Export citation
-
Aim:
In present study, we aimed to evaluate the changes in valvular regurgitations in mid-term follow-up of children with first attack acute rheumatic fever diagnosed after updated Jones criteria.
Materials and methods:The medical records of the children diagnosed with acute rheumatic fever between June 2015 and November 2018 were evaluated retrospectively. When compared to the findings during diagnosis, the changes in the degree of valvular regurgitation in the last visit were coded as same, regressed, or disappeared.
Results:A total of 50 children were diagnosed with the first attack of acute rheumatic fever between the noted dates. Nine patients (18%) could be diagnosed depending on the new criteria. Eight patients did not have carditis, and 35 patients (49 valves) could be followed for a median follow-up period of 11.7 ± 3.3 months. In our study, the valvar lesions continued in 82% of patients with clinical carditis at the end of the first year and the degree of valvular regurgitation decreased in 39% of them. Despite this, in a significantly higher (p = 0.031) ratio of patients with silent carditis (41%), valvar lesions disappeared in the same follow-up period. In 18.4% of the involved valves, regurgitation regressed to physiological level.
Conclusion:Updated Jones criteria make it possible to diagnose a significant number of patients, and the ratio of complete recovery among patients with silent carditis is significantly higher. Also, it can be speculated that the normal children in whom a physiological mitral regurgitation is detected should be followed in terms of rheumatic heart disease.
Does obesity affect the short-term outcomes after cardiothoracic surgery in adolescents with congenital heart disease?
- Richard U. Garcia, Preetha L. Balakrishnan, Sanjeev Aggarwal
-
- Published online by Cambridge University Press:
- 09 January 2020, pp. 372-376
-
- Article
- Export citation
-
Background:
Obesity is a modifiable, independent risk factor for mortality and morbidity after cardiovascular surgery in adults. Our objective was to evaluate the impact of obesity on short-term outcomes in adolescents undergoing surgery for congenital heart disease (CHD).
Methods:This retrospective chart review included patients 10–18 years of age who underwent CHD surgery. Our exclusion criteria were patients with a known genetic syndrome, heart transplantation, and patients with incomplete medical records. The clinical data collected included baseline demographics and multiple perioperative variables. Charting the body mass index in the Centers for Disease Control and Prevention growth curves, the entire cohort was divided into three categories: obese (>95th percentile), overweight (85th–95th percentile), and normal weight (<85th percentile). The composite outcome included survival, arrhythmias, surgical wound infection, acute neurologic injury, and acute kidney injury.
Results:The study cohort (n = 149) had a mean standard deviation (SD), body mass index (BMI) of 22.6 ± 6.5 g/m2, and 65% were male. There were 27 obese (18.1%), 24 overweight (16.1%), and 98 normal weight (65.8%) patients. Twenty-seven (18%) patients had composite adverse outcomes. Overweight and obese patients had significantly higher adverse outcomes compared with normal weight patients (odds ratio (OR): 2.9; confidence interval (CI): 1–8.5, p = 0.04 and OR: 3; CI: 1–8.5, p = 0.03, respectively). In multivariate analysis, obesity was an independent predictor of adverse outcome in our cohort (p = 0.04).
Conclusions:Obesity is associated with short-term adverse outcome and increased health resource utilisation in adolescents following surgery for CHD. Further studies should evaluate if intervention in the preoperative period can improve outcomes in this population.
Provider perspective on the role of palliative care in hypoplastic left heart syndrome
- Sarah Lowenstein, Robert Macauley, Kathleen Perko, Christina Ronai
-
- Published online by Cambridge University Press:
- 09 March 2020, pp. 377-382
-
- Article
- Export citation
-
Objective:
Hypoplastic left heart syndrome is a single ventricle defect. While staged surgical palliative treatments have revolutionised care, patients with hypoplastic left heart syndrome continue to have significant morbidity and mortality. In 2017, the National Pediatric Cardiology Quality Improvement Collaborative recommended all single ventricle patients to receive a prenatal palliative care consult. This study aimed to elucidate provider perspectives on the implementation of prenatal palliative care consults for families expecting a child with hypoplastic left heart syndrome.
Methods:An online survey was administered to obstetric and paediatric providers of relevant disciplines to assess their experience with palliative care involvement in hypoplastic left heart syndrome cases.
Results:Nearly, all physicians (97%) and most registered nurses (79%) agreed that the initial palliative care consult for patients with hypoplastic left heart syndrome should occur during the prenatal period. Respondents also indicated that prenatal palliative care consults should also be offered in a variety of other CHD conditions. Participants believed positive aspects of this new referral protocol included an expanded support network for families, decreased family stress during the postnatal period, increased patient education about what to expect during the postnatal period, and continuity of care.
Conclusion:Multidisciplinary healthcare professionals believe that prenatal palliative care consults provide a variety of benefits for patients and families with hypoplastic left heart syndrome. Additional, multi-centre research is necessary to evaluate whether prenatal palliative care consults should become standard of care for families expecting a child with a single ventricle defect.
Resource utilisation in paediatric patients with secundum atrial septal defects
- Daniel S. Ziebell, Stephanie Ghaleb, Jeffrey Anderson, Christopher J. Statile
-
- Published online by Cambridge University Press:
- 10 February 2020, pp. 383-387
-
- Article
- Export citation
-
Background:
There is variation in care of secundum atrial septal defects. Defects <3 mm and patent foramen ovale are not clinically significant. Defects >3 mm are often followed clinically and may require closure. Variation in how these lesions are monitored may result in over-utilisation of routine studies and higher than necessary patient charges.
Purpose:To determine utilisation patterns for patients with secundum atrial septal defects diagnosed within the first year of life and compare to locally developed optimal utilisation standard to assess charge savings.
Methods:This was a retrospective chart review of patients with secundum atrial septal defects diagnosed within the first year of life. Patients with co-existing cardiac lesions were excluded. Total number of clinic visits, electrocardiograms, and echocardiograms were recorded. Total charge was calculated based on our standard institutional charges. Patients were stratified based on lesion and provider type and then compared to “optimal utilisation” using analysis of variance statistical analysis.
Results:Ninety-seven patients were included, 40 had patent foramen ovale (or atrial septal defect <3 mm), 43 had atrial septal defects not requiring intervention and 14 had atrial septal defects requiring intervention. There was a statistically significant difference in mean charge above optimal for these lesions of $1033, $2885, and $5722 (p < 0.02), respectively. There was statistically significant variation of charge among types of provider as well. Average charge savings per patient would be $2530 with total charge savings of $242,472 if the optimal utilisation pathway was followed.
Conclusion:Using optimal utilisation and decreasing variation could save the patient significant unnecessary charges.
Family history of associated disorders in patients with postural tachycardia syndrome
- Jeffrey R. Boris, Jing Huang, Timothy Shuey, Thomas Bernadzikowski
-
- Published online by Cambridge University Press:
- 03 February 2020, pp. 388-394
-
- Article
- Export citation
-
Introduction:
Postural tachycardia syndrome is more frequently being recognised in adolescents and adults. However, its pathophysiology remains undefined. We evaluated our database for patterns in family history of clinical symptoms and associated disorders in these patients.
Materials and methods:Patients with postural tachycardia syndrome diagnosed in our clinic between 2014 and 2018 and who were less than 19 years at diagnosis were included. The history was reviewed for family members with postural tachycardia syndrome, dizziness and/or syncope, joint hypermobility with or without hypermobile Ehlers–Danlos syndrome, and autoimmune disorders. Statistical analysis assessed the entire cohort plus differences in gender, presence or absence of joint hypermobility, and presence or absence of familial autoimmune disease.
Results:A total of 579 patients met inclusion criteria. We found that 14.2% of patients had a family member with postural tachycardia syndrome, with male patients more likely to have an affected family member (20% versus 12.7%, p = 0.04). If the patient also had joint hypermobility, male patients were more likely to have a family member with postural tachycardia syndrome (25% versus 12.6%, p = 0.017), more than one affected family member (7.1% versus 0.74%, p = 0.001), and a family member with joint hypermobility (37.5% versus 23.7%, p = 0.032). Autoimmune disease was seen in 45.1% of family members, but more likely in female patients with concurrent hypermobility (21.1% versus 8.9%, p = 0.035).
Discussion:This in-depth analysis of associated familial disorders in patients with postural tachycardia syndrome offers further insight into the pathophysiology of the disorder, and informs further screening of family members in these patients.
Erratum
Family history of associated disorders in patients with postural tachycardia syndrome – Erratum
- Jeffrey R. Boris, Jing Huang, Timothy Shuey, Thomas Bernadzikowski
-
- Published online by Cambridge University Press:
- 05 March 2020, p. 395
-
- Article
-
- You have access Access
- HTML
- Export citation
Original Article
Arch intervention following stage 1 palliation in hypoplastic left heart syndrome is associated with slower feed advancement: a report from the National Pediatric Quality Cardiology Improvement Collaborative
- Alicia H. Chaves, Carissa M. Baker-Smith, Geoffrey L. Rosenthal
-
- Published online by Cambridge University Press:
- 03 February 2020, pp. 396-401
-
- Article
- Export citation
-
Introduction:
Infants undergoing stage 1 palliation for hypoplastic left heart syndrome may have post-operative feeding difficulties. Although the cause of feeding difficulties in these patients is multi-factorial, residual arch obstruction may affect gut perfusion, contributing to feeding intolerance. We hypothesised that undergoing arch reintervention following stage 1 palliation would be associated with post-operative feeding difficulties.
Methods:This was a retrospective cohort study. We analysed data from the National Pediatric Cardiology Quality Improvement Collaborative, which maintains a multicentre registry for infants with hypoplastic left heart syndrome discharged home following stage 1 palliation. Patients who underwent arch reintervention (percutaneous or surgical) prior to discharge following stage 1 palliation were compared with those who underwent non-aortic arch interventions after stage 1 palliation and those who underwent no intervention. Median post-operative days to full enteral feeds and weight for age z-scores were compared. Predictors of post-operative days to full feeds were identified.
Results:Among patients who underwent arch reintervention, post-operative days to full enteral feeds were greater than for those who underwent non-aortic arch interventions (25 versus 16, p = 0.003) or no intervention (median days 25 versus 12, p < 0.001). Arch intervention, multiple interventions, gestational age, and the presence of a gastrointestinal anomaly were predictors of days to full feeds.
Conclusions:Repeat arch intervention is associated with a longer time to achieve full enteral feeding in patients with hypoplastic left heart syndrome after stage 1 palliation. Further investigation of this association is needed to understand the role of arch obstruction in feeding problems in these patients.
Advance care planning and palliative care in ACHD: the healthcare providers’ perspective
- Jill M. Steiner, Erwin N. Oechslin, Gruschen Veldtman, Craig S. Broberg, Karen Stout, James Kirkpatrick, Adrienne H. Kovacs
-
- Published online by Cambridge University Press:
- 14 February 2020, pp. 402-408
-
- Article
- Export citation
-
Background:
Advance care planning and palliative care are gaining recognition as critical care components for adults with CHD, yet these often do not occur. Study objectives were to evaluate ACHD providers’ 1) comfort managing patients’ physical symptoms and psychosocial needs and 2) perspectives on the decision/timing of advance care planning initiation and palliative care referral.
Methods:Cross-sectional study of ACHD providers. Six hypothetical patients were described in case format, followed by questions regarding provider comfort managing symptoms, initiating advance care planning, and palliative care referral.
Results:Fifty providers (72% physicians) completed surveys. Participants reported low levels of personal palliative care knowledge, without variation by gender, years in practice, or prior palliative care training. Providers appeared more comfortable managing physical symptoms and discussing prognosis than addressing psychosocial needs. Providers recognised advance directives as important, although the percentage who would initiate advance care planning ranged from 18 to 67% and referral to palliative care from 14 to 32%. Barriers and facilitators to discussing advance care planning with patients were identified. Over 20% indicated that advance care planning and end-of-life discussions are best initiated with the development of at least one life-threatening complication/hospitalisation.
Conclusions:Providers noted high value in advance directives yet were themselves less likely to initiate advance care planning or refer to palliative care. This raises the critical questions of when, how, and by whom discussion of these important matters should be initiated and how best to support ACHD providers in these endeavours.
Early and late outcomes of surgical repair of double-chambered right ventricle: a single-centre experience
- Murat Surucu, İlkay Erdoğan, Birgül Varan, Murat Özkan, N. Kürşad Tokel, Sait Aşlamacı
-
- Published online by Cambridge University Press:
- 17 February 2020, pp. 409-412
-
- Article
- Export citation
-
Objective:
Double-chambered right ventricle is characterised by division of the outlet portion of the right ventricle by hypertrophy of the septoparietal trabeculations into two parts. We aim to report our experiences regarding the presenting symptoms of double-chambered right ventricle, long-term prognosis, including the recurrence rate and incidence of arrhythmias after surgery.
Methods:We retrospectively investigated 89 consecutive patients who were diagnosed to have double-chambered right ventricle and underwent a surgical intervention from 1995 to 2016. The data obtained by echocardiography, cardiac catheterisation, and surgical findings as well as post-operative follow-up, surgical approaches, post-operative morbidity, mortality, and cardiac events were evaluated.
Results:Median age at the time of diagnosis was 2 months and mean age at the time of operation was 5.3 years. Concomitant cardiac anomalies were as follows: perimembranous ventricular septal defect (78 patients), atrial septal defect (9 patients), discrete subaortic membrane (32 patients), right aortic arch (3 patients), aortic valve prolapse and/or mild aortic regurgitation (14 patients), and left superior caval vein (2 patients). The mean follow-up period was 4.86 ± 4.6 years. In these patients, mean systolic pressure gradient in the right ventricle by echocardiography before, immediately, and long-term after surgical intervention was 66.3, 11.8, and 10.4 mmHg, respectively. There were no deaths during the long-term follow-up period. Surgical reinterventions were performed for residual ventricular septal defect (2), residual pulmonary stenosis (1), and severe tricuspid insufficiency (1).
Conclusion:The surgical outcomes and prognosis of double-chambered right ventricle are favourable, recurrence and fatal arrhythmias are unlikely in long-term follow-up.
Quality of life assessment in children before and after a successful ablation for supraventricular tachycardia
- M Cecilia Gonzalez Corcia, Laura Peters, Thierry Sluysmans, Stephane Moniotte, Karlien Carbonez, Catherine Barrea, Christophe Vo, Laetitia Vanhoutte, Christophe Scavee
-
- Published online by Cambridge University Press:
- 18 February 2020, pp. 413-417
-
- Article
- Export citation
-
Background and Objectives:
Young patients suffering from rhythm disorders have a negative impact in their quality of life. In recent years, ablation has become the first-line therapy for supraventricular arrhythmias in children. In the light of the current expertise and advancement in the field, we decided to evaluate the quality of life in young patients with supraventricular arrhythmias before and after a percutaneous ablation procedure.
Methods:The prospective cohort consisted of patients <18 years with structurally normal hearts and non-pre-excited supraventricular arrhythmias, who had an ablation in our centre from 2013 to 2018. The cohort was evaluated with the PedsQL™ 4.0 Generic Core Scales self-questionnaire prior to and post-ablation.
Results:The final cohort included 88 patients consisted of 52 males (59%), with a mean age at ablation of 12.5 ± 3.3 years. Forty-two patients (48%) had a retrograde-only accessory pathway mediating the tachycardia, 38 (43%) had atrio-ventricular nodal re-entrant tachycardia, 7 (8%) had ectopic atrial tachycardia, and 1 (1%) had atrial flutter. The main reason for an ablation was the patient’s choice in 53%. There were no severe complications. Comparison between the baseline and post-ablation assessments showed that patients reported significant improvement in the scores for physical health, emotional and social functioning, as well as in the total scores.
Conclusions:The present study demonstrates that the successful treatment of supraventricular arrhythmias by means of an ablation results in a significant improvement in the quality of self-reported life scores in young patients.