1537 results in Antimicrobial Stewardship & Healthcare Epidemiology
Capturing MRSA Diversity by Integrating Genomic and Epidemiological Data of Patients and their Spaces
- Tasmine Clement, Kristen Panson, Marco Cassone, Ali Mohammed Pirani, Evan Snitkin, Lona Mody
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, p. s15
-
- Article
-
- You have access Access
- Open access
- Export citation
-
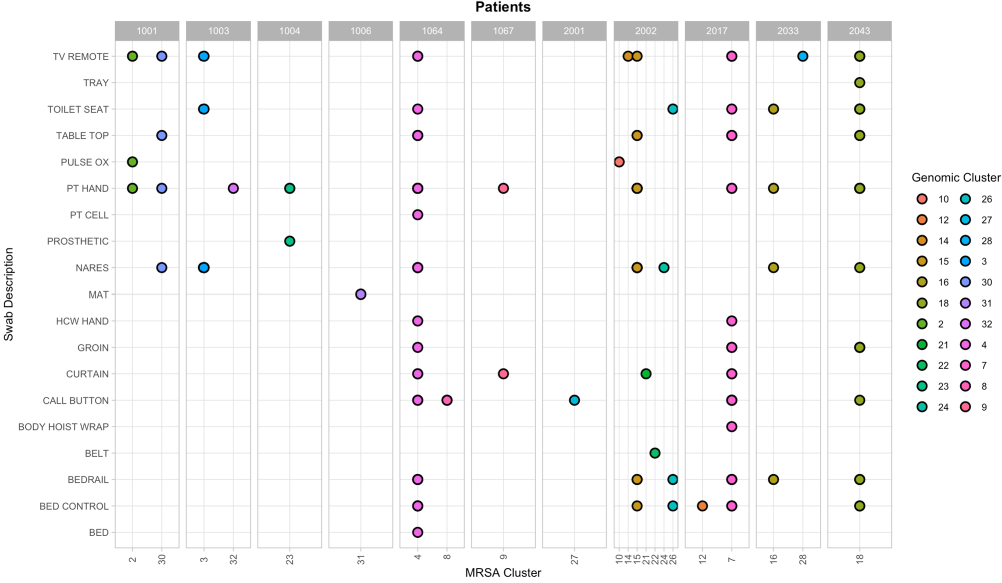
Background: Methicillin-resistant S. aureus (MRSA) is known to cause frequent and severe infections in community living centers, potentially resulting in significant mortality for elderly patients. More research is needed to understand how to utilize genomic and epidemiological data to understand characteristics that may lead to increased transmission. We hypothesized that combining genomic and epidemiological information to sample patients and their environments during long-term stays, we will be able to capture a diverse set of MRSA strains. Method: This work included genome sequencing of patient and environmental samples from 11 patients within the VA Ann Arbor Healthcare System from May 4, 2021- November 16, 2022. All 11 patients tested positive for MRSA during their stay (mean days = 31). Patient and environmental samples were taken throughout their stays, screened for MRSA, and whole-genome sequenced. Single nucleotide variants (SNVs) were identified by mapping reads and calling variants against strain-specific reference genomes. We used ape v5.6-2 in R v4.2.2 to analyze and infer evolution, acquisition, and transmission events based on pairwise SNV distances. Genomic clusters were determined using stats v3.6.2, with a SNV distance threshold of 20. Result: Samples that were collected from patient bodily sites were able to reveal 20 distinct genomic clusters of MRSA (patient hands: n = 10, nares: n = 7, groin: n = 3). Environmental samples from patient environments also revealed distinct genomic MRSA clusters (tv remote: n = 9, toilet seat and bed rail: n = 6, table top, bed control, and call button: n = 5, bed curtain: n = 4, pulse ox = 2, cell phone, tray, pulse ox, mat, body hoist wrap, and bed: n = 1). Conclusion: The identification of various genomic clusters from patients and their environmental reservoirs suggests intrahost variation that can only be captured by using a more holistic approach of integrating epidemiology and genomic sequencing. Developing studies that incorporate genomic data, various environmental sources, and multiple isolates over time within community living centers can increase our understanding of strains that are more likely to transmit, survive on living and non-living surfaces and therefore lead to improved recommendation for infection prevention interventions and drivers of endemicity.
Disclosure: Lona Mody: NIH, VA, CDC, Kahn Foundation; Honoraria: UpToDate; Contracted Research: Nano-Vibronix
Risk Factors and Outcomes of Candida auris in Southeast Michigan
- Ambreen Malik, Anita Shallal, George Alangaden, Geehan Suleyman
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, pp. s92-s93
-
- Article
-
- You have access Access
- Open access
- Export citation
-
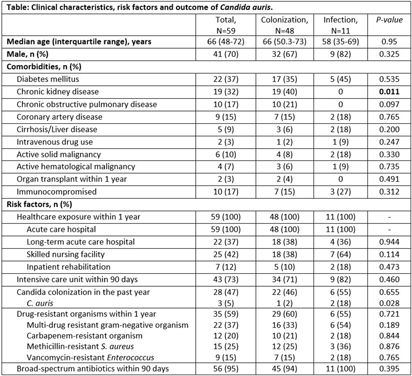
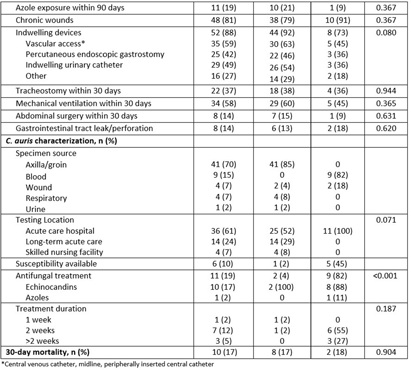
Background: Candida auris is an emerging multidrug resistant fungus that presents a serious global health threat and causes severe infections with a high mortality rate in hospitalized patients with significant underlying comorbidities. We describe the risk factors and clinical outcomes associated with C. auris in Southeast Michigan. Methods: This is a retrospective case series of culture-positive C. auris patients who had contact with our healthcare facility in Detroit from 2021 to 2023. We evaluated demographics, comorbidities, risk factors, and outcomes. A comparative analysis of colonized and infected patients was performed. Results: Forty-eight (81%) colonized and 11 (19%) infected patients were included (Table); 70% were male with median age of 66 years. All variables were comparable between the two groups except chronic kidney disease, which was significantly more prevalent among colonized patients (40% vs 0, p=0.011). All patients had prior exposure to acute care hospital (ACH), 37% to long-term acute care hospital, and 42% to skilled nursing facility within 1 year of diagnosis. Chronic wounds, prior broad-spectrum antibiotic use, and indwelling devices were prevalent in both groups; more than half required mechanical ventilation in the last month, and one third had tracheostomy at the time of C. auris detection. Almost 60% had a prior history of drug-resistant organisms, including multi-drug resistant gram negative (37%) and carbapenem-resistant (20%) organisms. Blood (82%) and wound (18%) were sources of invasive candidiasis. More than half (61%) of the testing was performed at ACH. Nine patients (82%) with invasive disease were treated with echinocandins (88%); among the colonized, two (4%) were treated with echinocandins but had persistent colonization. Thirty-day mortality was not significantly different among the two groups and was nearly 20%. Conclusions: In this large cohort study, a history of healthcare exposure, drug-resistant organisms, use of broad-spectrum antibiotics, indwelling devices, and chronic wounds were common risk factors among C. auris patients. Limiting the use of broad-spectrum antimicrobials and invasive devices, adherence to infection prevention and control practices, and interfacility transfer communication are important mitigating strategies to reduce the incidence and spread of C. auris.
Bridging the Gap: Specialized Training Programs for Infection Prevention Specialists Increase Certification Success
- Kelly Holmes, Jennifer McCarty, Sandi Steinfeld, Kelley Boston
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, pp. s107-s108
-
- Article
-
- You have access Access
- Open access
- Export citation
-
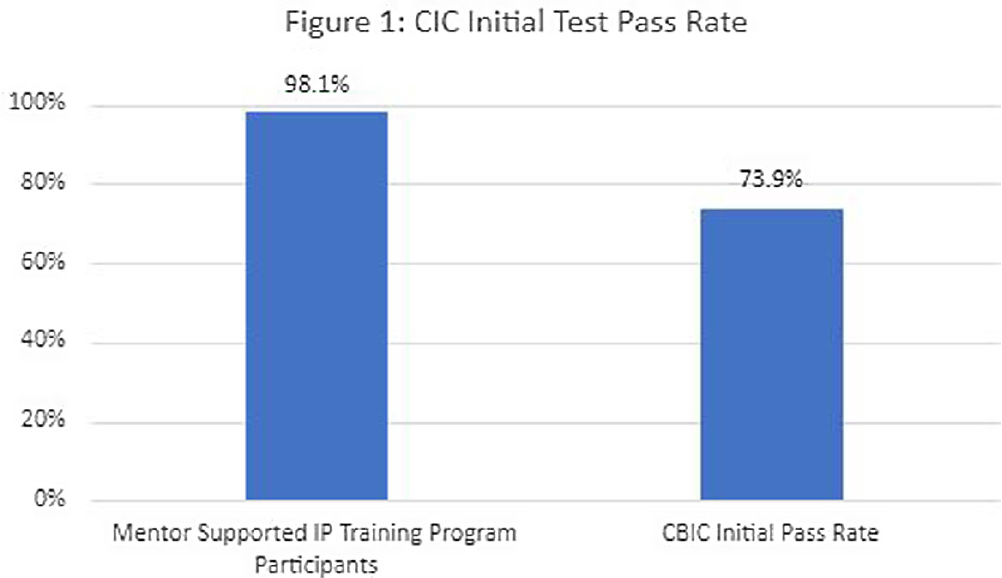
Background: The role of the infection preventionist (IP) is complex and encompasses a range of responsibilities requiring extensive knowledge in infection control practices, data analysis, surveillance, performance improvement and collaboration with multidisciplinary teams. Infection prevention certification (CIC) by the certification Board of Infection Control (CBIC) is a standardized marker of knowledge and competencies required for practice in the field. In a 2020 survey of IPs, less than half were certified or planned to become certified. Of those that do take the certification exam, less than three quarters pass on their initial exam attempt. Methods: From 2017 to 2023, fifty-two new IPs were enrolled in a competency-based training program which combined didactic and applied learning on core IP job functions, and a structured mentoring program. The initial didactic phase consisted of evidence-based learning modules with validation of competency through post-training testing and practical demonstration. Education was provided by an advanced practice IP via remote webinars, which included discussion of questions, skills coaching, and review of post-tests. Novice IPs were partnered with at least two preceptors: one advanced practice lead preceptor guided the novice IPs through assigned education modules and oversaw program management and training benchmarks. A second, near-peer preceptor or mentor collaborated with the novice IP in the facility setting. Initial training focused on facility operations, surveillance, rounding and other facility specific activities. Facility mentors were responsible for combining education module topics with practical application of skills. Mentors guided novice IPs through National Healthcare Surveillance network (NHSN) surveillance training and validated surveillance and infection coding until the novice IP had an interrater reliability validation assessing surveillance competency. After the initial training phase, the novice IPs began preparation for certification. This phase included additional training modules aligned with the CBIC certification content outline and practice exams. Results: All 52 novice IPs completed the training program and attempted the CIC examination. The initial pass rate for the certification exam among IPs in the supervised training and mentorship program was 98.1% (n=51). This is 33% higher than the initial pass rate published by CBIC, which was 73.9% (Figure 1). Conclusions: Organizing evidence-based guidelines into topic-specific modules builds a foundation of infection prevention and control knowledge, which is enhanced through remote instruction and direct application of skills under a preceptor’s supervision. This method allows IPs to be introduced to concepts covered in the board certification exam upon hire and support certification with improved outcome
Clinical Characteristics and Cycle Thresholds Among Discordant and True Positive Test Results for Clostridiodes difficile
- Michael Rossi, Emerald O’Rourke, Sara Geffert, Tao Hong, Andrea Collins, Tiffany L. Chargualaf, Francine Romo Touzard
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, p. s67
-
- Article
-
- You have access Access
- Open access
- Export citation
-
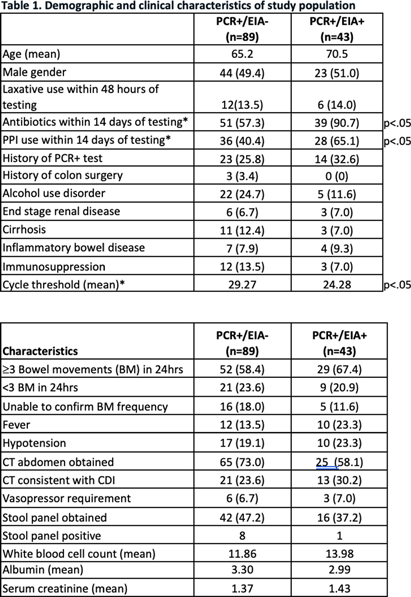
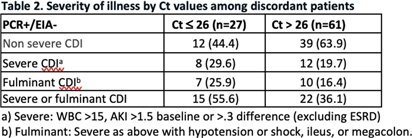
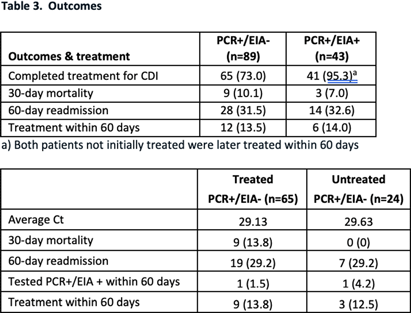
Background: The diagnosis of Clostridioides difficile infection (CDI) is challenging. Despite guideline-directed, multistep testing algorithms and diagnostic stewardship, the treatment of C. difficile colonization persists. The testing algorithm at our system utilizes an initial real-time PCR test (PCR) for Toxin B gene, which if positive, reflexes to an enzyme immunoassay (EIA) for detecting Toxins A and B. Discordant results (PCR +/EIA -) are suggestive of colonization, but the majority of patients with discordant results are treated for CDI. Correlation of C. difficile EIA B polymerase chain reaction (PCR) cycle thresholds (Ct) with the presence of free EIA and disease severity has been observed, but the ability to use Ct in the decision to treat patients with discordant results is unclear. Our study assesses if Ct values and other clinical characteristics favor treatment in select patients with discordant Methods: A retrospective chart review was performed of adult patients (≥ 18-year-old) with positive C. difficile PCR results that were admitted to our health system between June 01 and August 31, 2023. C. difficile PCR and Ct results were obtained by Cepheid GeneXpert and Toxin A and B EIA results were obtained by Meridian Bioscience Immunocard. Patients with discordant (PCR+/EIA) and true positive (PCR+/EIA+) results were compared. We assessed demographics, past medical history, clinical characteristics, severity of illness, PCR Ct values, treatment, and clinical outcomes including: 30-day all-cause mortality and re-admission, and 60-day CDI repeat testing and treatment. Results Of the 122 patients identified, 89 patients had discordant results and 43 had true positive Results: Severity of illness and other clinical and laboratory characteristics were similar between both groups. Mean Ct values were significantly lower for true positive results compared to discordant results, 24.28 vs 29.27, respectively (p26 (p=.08). Of the patients with discordant results, 73 completed treatment for CDI and no difference in clinical outcomes was observed compared to patients with discordant results that were not treated. Conclusion Ct values were lower among patients with true positive results compared to patients with discordant Conclusion: There were no statistically significant different rates of severe or fulminant CDI among patients with discordant results and Ct values < 26, although this finding may be limited by sample size and Ct may be helpful in deciding which discordant patients to treat.
Molecular and Epidemiological Characterization of Pediatric and Adult C. difficile Infection in Canadian Hospitals, 2015-2022
- Timothy Du, Kelly Baekyung Choi, Anada Silva, Cassandra Lybeck, George Golding, Romeo Hizon, Sean Ahmed, Blanda Chow, Ian Davis, Meghan Engbretson, Gerald Evans, Charles Frenette, Jennie Johnstone, Pamela Kibsey, Kevin Katz, Joanne Langley, Jenine Leal, Bonita Lee, Yves Longtin, Dominik Mertz, Jessica Minion, Michelle Science, Jocelyn Srigley, Kathryn Suh, Reena Titoria, Nisha Thampi, Alice Wong, Jeannette Comeau, Susy Hota
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, pp. s10-s11
-
- Article
-
- You have access Access
- Open access
- Export citation
-
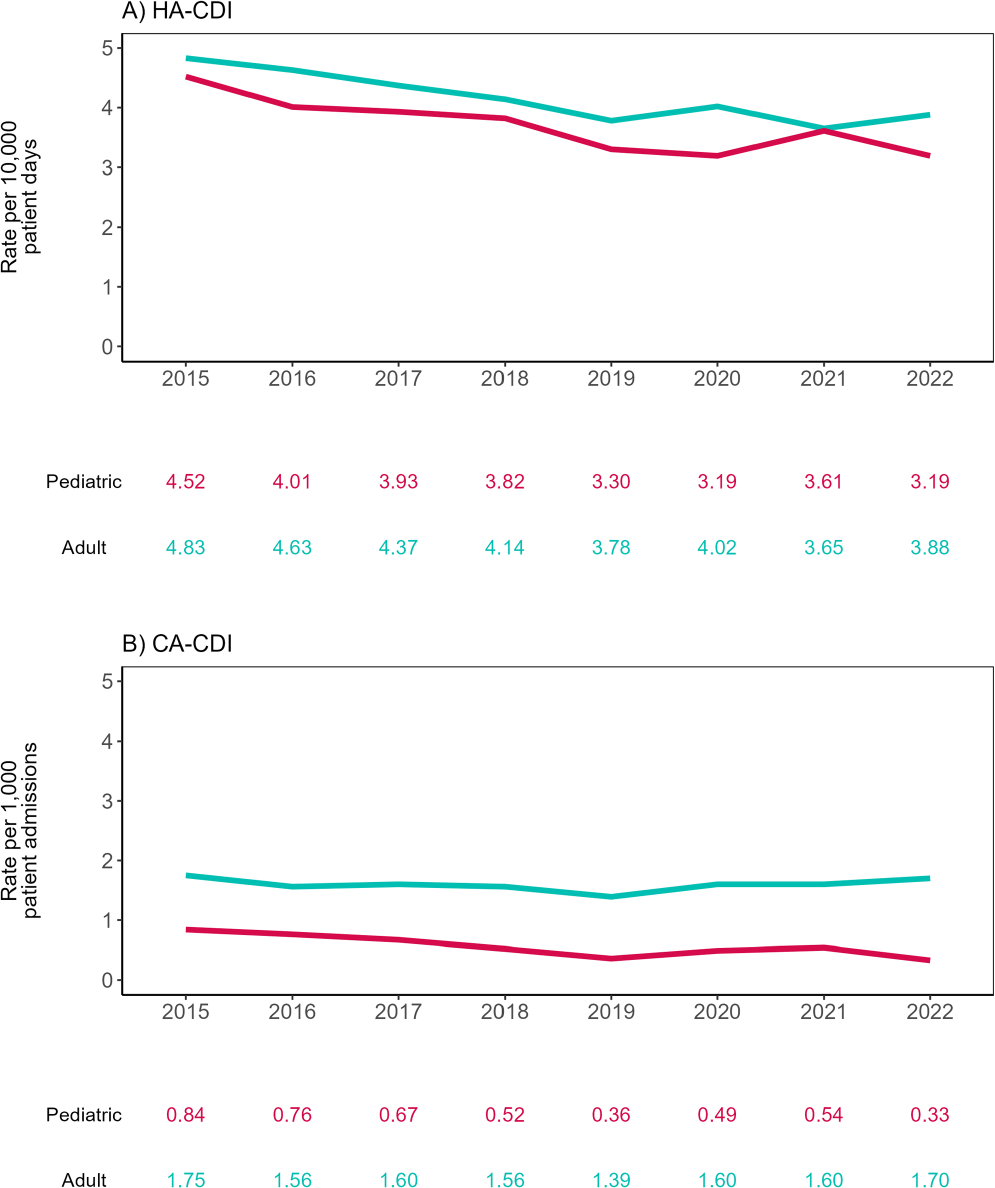
Background: The molecular and epidemiological landscape of C. difficile infection (CDI) has evolved markedly in the last decade; however, limited information is available contrasting differences between adult and pediatric populations. We describe a multicenter study evaluating healthcare-associated (HA) and community-associated (CA) adult and pediatric-CDI identified in the Canadian Nosocomial Infection Surveillance Program (CNISP) network from 2015 to 2022. Methods: Hospitalized patients with CDI were identified from up to 84 hospitals between 2015–2022 using standardized case definitions. Cases were confirmed by PCR, cultured, and further characterized using ribotyping and E-test. We used two-tailed tests for significance (p≤0.05). Results: Of 30,817 cases reported, 29,245 were adult cases [HA-CDI (73.2%), CA-CDI (26.8%)] and 1,572 were pediatric cases [HA-CDI (77.7%), CA-CDI (22.3%)]. From 2015 to 2022, HA-CDI rates decreased 19.7% (p=0.007) and 29.4% (p=0.004) in adult and pediatric populations, respectively (Figure 1). CA-CDI rates remained relatively stable in the adult population (p=0.797), while decreasing 60.7% in the pediatric population (p=0.013). Median ages of adult and pediatric patients were 70 (interquartile range (IQR), 58–80) and seven (IQR, 3–13) years, respectively. Thirty-day all-cause mortality was significantly higher among adult vs. Pediatric CDI patients (11.0% vs 1.4%, p < 0.0001). No significant differences in other severe outcomes were found. Ribotyping and susceptibility data were available for 4,620 samples: 3,558 adult (77.0%) and 1,062 pediatric (23.0%). The predominant adult and pediatric ribotypes (RT) were 106 (12.2/16.2%), 027 (11.4/3.2%), and 014 (8.8/8.2%). Overall, RT027 prevalence significantly decreased from 17.9% in 2015 to 3.2% in 2022 (p=0.003), while RT106 increased from 8.5% to 14.4%. Resistance rates among adult and pediatric isolates were similar for all antimicrobials tested except moxifloxacin (16.2% vs. 6.2%, p < 0.0001, respectively). Adult moxifloxacin resistance decreased from 30% to 6.3% from 2015 to 2022 (p=0.006). Adults with moxifloxacin-resistant CDI were older (median: 74 vs. 69 years, p < 0.001) and had higher thirty-day all-cause mortality (13% vs. 9.8%, p=0.041) and recurrence (10% vs. 5.7%, p < 0.001) compared to those with moxifloxacin non-resistant CDI, while these trends were not observed in pediatric patients. Among RT027 strains, moxifloxacin resistance decreased from 91.0% in 2015 to 7.1% in 2022. There was one metronidazole-resistant pediatric sample in 2018 and no resistance to vancomycin or tigecycline in either population. Conclusion: We have found differences in the epidemiological and molecular characteristics of adult and pediatric CDI, with higher thirty-day all-cause mortality among adults. Overall, RT106 has replaced RT027 as the predominant ribotype with a concomitant decrease in fluoroquinolone resistance.
Assessment of 19 Operation Room and Sterile Processing Units in Puerto Rico, 2023: Preliminary Findings using a new ICAR Tool
- David Nachi, Norma I. Diaz-Paris, Jonell Gonzalez-Pagan, Miguel A. Jorge-Coreano, Tanialy Rivera-Santiago, Angelica Garcia-Segui, Sylvianette Luna-Anavitate, Melissa Marzan-Rodriguez
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, pp. s105-s106
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Infection prevention and control assessments in healthcare settings serve as a primary resource for obtaining data and providing recommendations based on safety, compliance, and quality assurance guidelines. In Puerto Rico (PR), surgical site infections are underreported in the Epi Info platform used by the Puerto Rico Department of Health (PRDOH), mainly due to the complexity of their identification. By focusing on evaluating Operating Rooms/Sterile Processing and Distribution (OR/SPD) units in acute care facilities (ACFs), our goal is to generate new data within the Healthcare-Associated Infection/Antibiotic Resistance (HAI/AR) Program, specifically related to patient management throughout preoperative, intraoperative, and postoperative phases, as well as reprocessing practices. Methods: Nineteen evaluations of ACFs' OR/SPDs were conducted from May through December 2023. Direct observations, file reviews, and personnel assessments were performed using an infection control assessment and response (ICAR) tool developed collaboratively by a team from an acute facility in PR and the HAI/AR Program staff. This ICAR Tool was customized based on guidelines from the certified Board for Sterile Processing and Distribution (CBSPD), the Association of periOperative Registered Nurses (AORN), and the Association for the Advancement of Medical Instrumentation (AAMI), among other regulatory agencies. The Division of Health Quality Promotion (DHQP) reviewed and approved the tool for use in these evaluations. Results: Key findings indicate that 32% of Sterile Processing Department (SPD) units restrict access to dedicated personnel with available manufacturer’s instructions, yet only 36% of SPD personnel are certified in CBSPD and packaging practices. Only 10% of facilities had a water treatment system for sterilization and Immediate Use Steam Sterilization (IUSS) policies. Notably, 84% of endoscopy areas require additional equipment for cultivating endoscopes, and no facility possessed a borescope for visually inspecting endoscope lumens. Tray inspection occurred in 21%, and only 31% of staff knew the Spaulding Classification and Class V Indicators. Conclusion: These data underscore the necessity of evaluating OR/SPD units in ACFs to provide updated recommendations and mitigate the incidence of surgical site infections (SSI). They offer insight into the structural and functional status of OR/SPD units in Puerto Rico, aligning reporting with OR/SPD practices to enhance patient care and minimize infection risks.
Candida auris Screening of High-Risk Patients: A Descriptive Comparison of 2 Strategies.
- Laura Pedersen, Aldo Barajas-Ochoa, Kaila Cooper, Jenna Price, Kathryn Hannum, Yvette Major, Patrick R Ching, Barry Rittmann, Michelle Doll
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, p. s147
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Candida auris infection is associated with high morbidity and mortality. C. auris can persist in the healthcare environment and is associated with outbreaks. We compare screening strategies for C. auris in two high-risk patient populations. Methods: Our center is a tertiary, 865-bed hospital. In the context of known regional outbreaks of C. auris in post-acute care (PAC) facilities, we experienced extended clusters of apparent C. auris acquisition across several hospital units. Hospital acquisition was defined as new C. auris in clinical cultures in patients with no known history of C. auris colonization/infection. We performed point prevalence surveys (PPS) on affected units weekly until all tests were negative for two consecutive weeks. We also initiated admission screening for C. auris for patients admitted from PAC. All screening swabs were collected per CDC’s procedure. Tests were performed either by RT-PCR or Chromagar C. auris media, depending on availability. We compared the overall positivity rates of exposure PPS versus PAC admission screenings using Z-test for two proportions with statistical significance set at p < 0 .05 Results: From 2/2023-12/2023, a total of 533 tests on 367 unique patients were processed during PPS; 512 tests were negative and 21 were positive (3.9% positivity rate). Three additional samples were either unable to be processed or indeterminate. There were 68 patients who had repeat testing weekly for ≥2 weeks. Most remained negative, but 5 tested positive after variable amounts of negative-week intervals: 3 patients at week 2, 1 patient at week 4 and 1 patient at week 5. From 8/2023 to 12/2023, a total of 89 patients admitted from 35 different PAC facilities underwent admission screening for C. auris. Only three patients were positive (3.4%), each from a different facility. The difference in the positivity rates between PPS and PAC was not statistically significant (Z-score 0.25, p = 0.79). Discussion: Our C. auris screening strategies found similar positivity rates for patients admitted to the hospital from PACs compared to targeted PPS in the setting of apparent hospital acquisition events. These strategies may be considered as complementary. Facilities experiencing apparent acquisition events should consider screening high-risk admissions to identify and isolate colonized patients, particularly if standard infection prevention practices are being performed with high fidelity.
Reduction in IUSS (Immediate Use Steam Sterilization) Associated with Reduction in Surgical Site Infections
- Jennifer Jaffe, Linda Merz, Kathleen McMullen
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, p. s89
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Immediate use steam sterilization (IUSS) is a potential risk factor for surgical site infection (SSI). During a regulatory survey, it was discovered that IUSS rates for a 767-bed hospital exceeded what had been reported to Infection Prevention (IP) and surgery leaders (estimated at an average of 60 instances per month, with approximately 40 of those in orthopedic cases). A Quality Improvement (QI) project to reduce IUSS was implemented. Methods: The QI project started with the requirement of three signatures for every cycle of IUSS (surgery management, sterilization management, and IP). Additional trays were ordered to provide an ample supply for cases. Surgery personnel were no longer allowed to perform IUSS, and the number of sterilizers available for IUSS was reduced from 8 to 1. The project was fully implemented as of December 2019. To evaluate the impact, SSI rates for hip and knee prothesis were compared using chi square analysis (Epi Info, CDC); before QI project rates were measured from 2017-2019 and after QI project rates were measured for 2020-2022. No other changes were made that were anticipated to impact orthopedic SSI rates. Results: There were no instruments or implants processed by IUSS after December 2019. Prior to the project, there were 9 hip SSI (rate = 0.54 per 100 procedures) and 14 knee SSI (rate = 0.49 per 100 procedures). After the project, hip SSI decreased by 76% (2 SSI, rate = 0.13 per 100 procedures, p = < 0 .05) and knee SSI decreased by 18% (7 SSI, rate = 0.41 per 100 procedures, p=0.67). Conclusion: A multidisciplinary QI project was successful at drastically reducing the use of IUSS, and a correlating statistically significant decrease in hip SSI and clinically significant decrease in knee SSI was seen for 3 years after the project was completed.
Disclosure: Kathleen McMullen: Speaker - 3M
Diagnostic Stewardship Opportunities for Emergency Department Evaluation of Children with Suspected Urinary Tract Infection
- Rachel Wattier, Prachi Singh, Israel Green-Hopkins, Adam Hersh, Andrew Auerbach, Sunitha Kaiser
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, p. s77
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Among children who start antibiotics for suspected urinary tract infection (UTI) in emergency departments (EDs), 40-60% have negative urine cultures or other results inconsistent with UTI. Practices contributing to excess antibiotic exposure are not well understood. The goal of this study was to understand diagnostic and post-encounter follow-up processes in children who received antibiotics, in order to define targets for intervention. Methods: We identified encounters by children evaluated in two pediatric EDs, over 2 months in the first ED and 9 months in the second ED, to balance different visit volumes. Children 2 months-17 years old were included if they had a urinalysis (UA) and/or urine culture performed, were assigned a primary or secondary diagnosis code for UTI, and initiated antibiotics. Patients were excluded if they received antibiotics prior to the encounter, had prior urologic surgery or device placement, or were immunocompromised or pregnant. Data abstracted by chart review included demographics, documented symptoms, test results, and documented urine culture review and management. Possible UTI symptoms per pediatric criteria included fever, dysuria, urinary frequency, urgency, or hesitancy, suprapubic, abdominal or flank pain, foul smelling urine, or new urinary incontinence. In both EDs, nurses review urine cultures and document changes to treatment plans. Final urine culture results were considered inconsistent with UTI if there was 1) no growth or 2) only mixed growth reported with quantity < 1 00,000 colony forming units/ml. Results: Of 150 eligible children, 146 (97%) had at least one UTI symptom and 146 (97%) had abnormal UA Results: Urine cultures were not performed in 27 (18%) children. Of 123 encounters with urine cultures performed, 71 (58%) had results inconsistent with UTI. Though 67/71 cultures were marked as reviewed, 43/67 (64%) of the patients who could have stopped antibiotics per guideline recommendations did not have documented plans to stop. In those who had documented plans to stop antibiotics, nurses reached 20/23 (87%) caregivers by phone to communicate these recommendations. Conclusion: Many children suspected to have UTI at the time of ED evaluation do not meet criteria for UTI. We found that the most frequent departures from evidence-based practice recommendations were 1) not sending urine cultures, and 2) not stopping antibiotics when culture results did not support the suspected UTI diagnosis. Further investigation should explore barriers and facilitators to these evidence-based practices to develop population- and context-specific diagnostic stewardship strategies.
Impacts of Hospital Acquired Bloodstream Infections in Patients Undergoing Hemodialysis Through a Central Venous Catheter
- Mary Michaud, Sharada Weir, Peter Sullivan, Elizabeth Hurlburt, Jared Crandon
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, p. s73
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Hospital acquired infections (HAI) are of interest given their resultant morbidity, mortality, and hospital utilization. Among HAIs, central line associated bloodstream infections result in the highest rates of mortality and additional costs. While all central venous catheters (CVC) carry risk for BSI, long-term catheter use is at increased risk. One population that utilize CVCs for extended durations are those undergoing hemodialysis. While data are available characterizing BSI impacts on outpatient hemodialysis patients, little data exist describing inpatients. The purpose of this study was to characterize the demographics, outcomes, and economics associated with the development of hospital acquired BSI (HA-BSI) in patients undergoing hemodialysis through a CVC (HD-CVC). Methods: All admissions of adult patients in the Premier Healthcare Database with hospital stays including HD-CVC with discharge dates during 2020-2022 were retrospectively evaluated. BSIs were identified by ICD-10 codes and blood culture collection dates. A BSI was deemed hospital acquired if the blood culture date was ≥3 calendar days after admission. Descriptive analyses were undertaken for HA-BSI patients including: baseline demographics, clinical characteristics, and outcomes. Length of stay (LOS), ICU utilization, and estimated costs were evaluated for HAI-BSI and non-BSI populations. Results: 166,394 admissions from 91,448 patients were identified. Of these, 5,722 patients (6.3%) had 5,842 admissions with a HA-BSI. These patients were 58.9% white, 28.3% black, 56.8% male, and 62.9% were aged ≥60years. Patients had considerable comorbidities at baseline with 88.9% having ≥2 Charlson comorbid conditions and 46.9% with ≥6. During the study period, all-cause mortality was 27.8% for HA-BSI patients with 85.5% of deaths occurring while inpatient. Median LOS for patients with HA-BSI was 25 days compared with 6 days for HD-CVC without BSI; patients with HA-BSI were also more likely to require the ICU (65.6% vs. 27.6%). The median ICU LOS was 12 days for HA-BSI versus 34 days for HD-CVC without BSI. Greater intensity of healthcare utilization was reflected in median costs of $402K for HA-BSI, compared with $43K for HD-CVC without BSI. Discussion: We described the characteristics of HD-CVC patients that developed HA-BSI. These patients had many comorbidities and relatively high rates of all-cause in-hospital mortality. Patients were likely to have long LOS, both in-hospital and within the ICU. Collectively, care of these patients was associated with considerable healthcare costs, particularly as compared with HD-CVC patients not developing a HA-BSI. Future studies should characterize risk factors and evaluate potential prevention strategies for this high-risk population.
Nationwide analysis of antimicrobial prescription in Korean hospitals between 2018 and 2021: The 2023 KONAS report
- Yong Chan Kim, I Ji Yun, Hyo Jun Park, Jungmi Chae, Hyung-sook Kim, Song Mi Moon, Eunjeong Heo, Se Yoon Park, Dong Min Seo, Ha-Jin Chun, Myung Jin Lee, Kyungmin Huh, Su Jin Jeong, Jun Yong Choi, Bongyoung Kim
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, pp. s38-s40
-
- Article
-
- You have access Access
- Open access
- Export citation
-
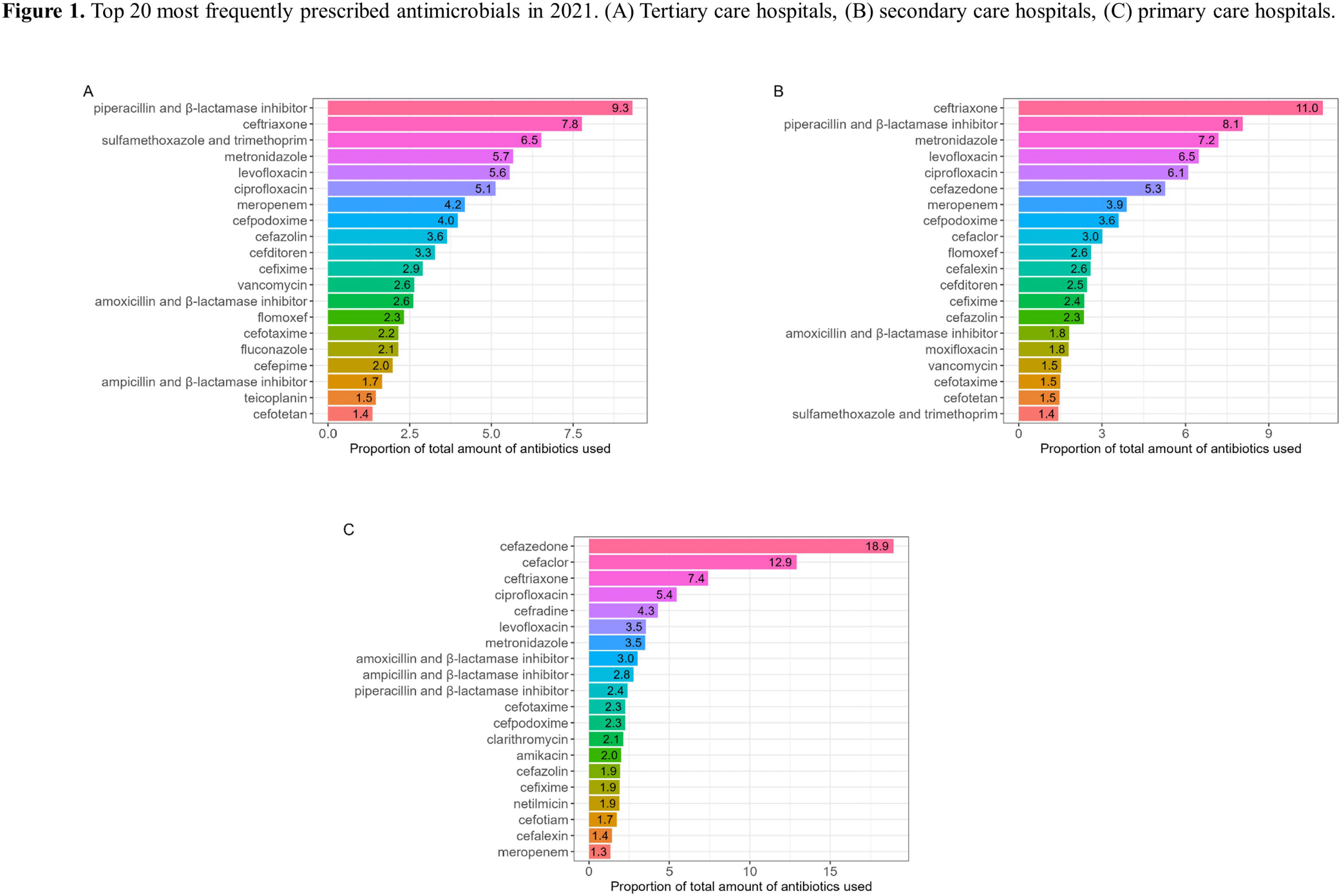
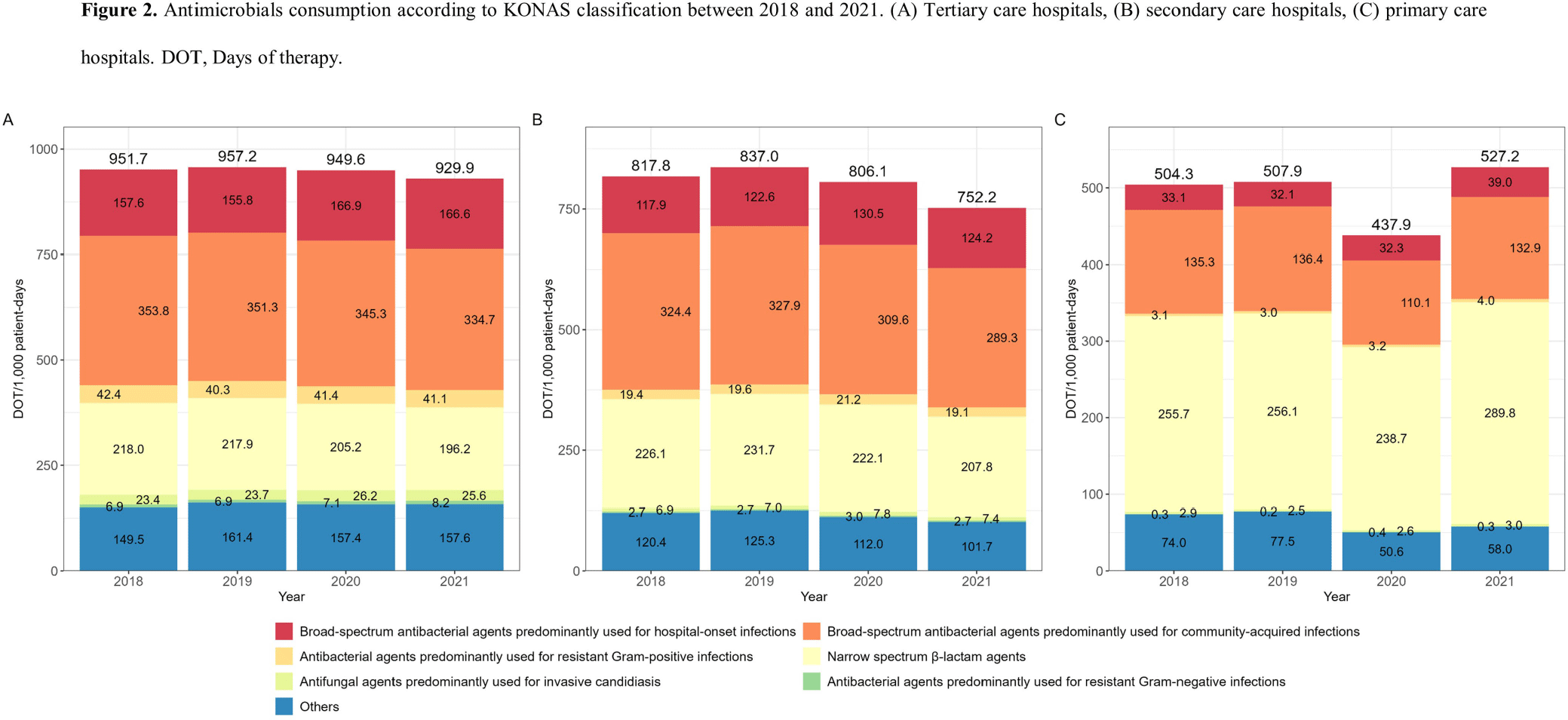
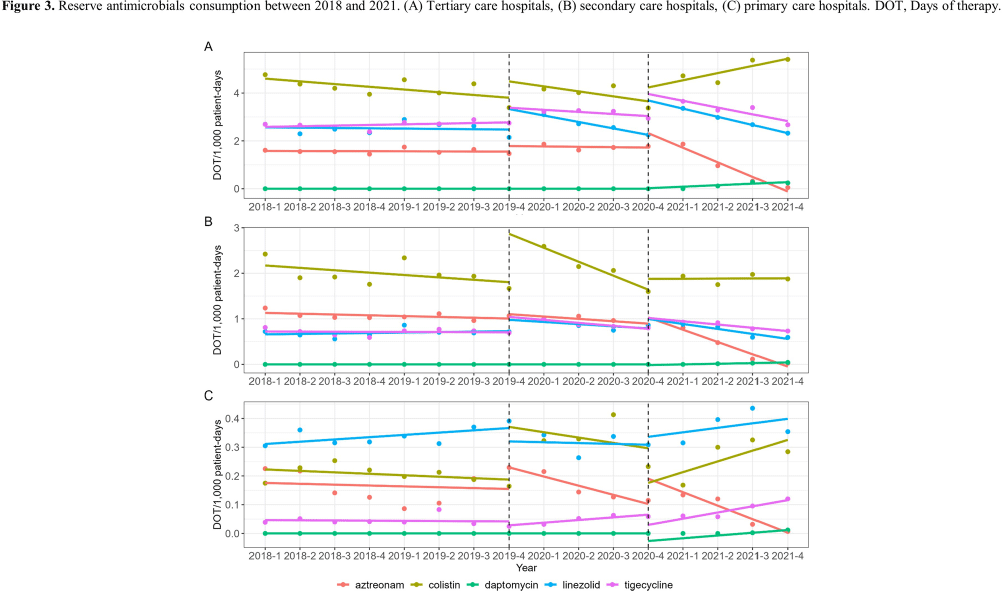
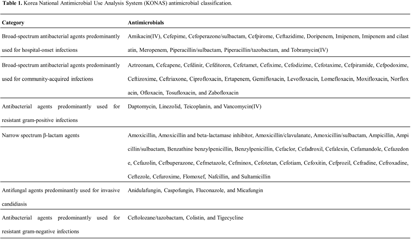
Background: Data on antimicrobial use at the national level is crucial to establish domestic antimicrobial stewardship policies and enable medical institutions to benchmark against each other. This study aimed to analyze antimicrobial use in Korean hospitals. Methods: We investigated the antimicrobials prescribed in Korean hospitals between 2018 and 2021, using data from the Health Insurance Review and Assessment. Primary care hospitals (PCHs), secondary care hospitals (SCHs), and tertiary care hospitals (TCHs) were included in this analysis. Antimicrobials were categorized according to the Korea National Antimicrobial Use Analysis System (KONAS) classification, which is suitable for measuring antimicrobial use in Korean hospitals. Results: Out of more than 1,900 hospitals, PCHs and TCHs represented the largest and lowest percentage of hospitals, respectively. The most frequently prescribed antimicrobial in 2021 was piperacillin/β-lactamase inhibitor (9.3%) in TCHs, ceftriaxone (11.0%) in SCHs, and cefazedone (18.9%) in PCHs. Between 2018 and 2021, the most used antimicrobial class according to the KONAS classification was ‘broad-spectrum antibacterial agents predominantly used for community-acquired infections’ in TCHs and SCHs, and 'narrow spectrum beta-lactam agents' in PCH. Total consumption of antimicrobials has decreased from 951.7 to 929.9 days of therapy (DOT)/1,000 patient-days in TCHs and from 817.8 to 752.2 DOT/1,000 patient-days in SCHs during study period, but not in PCHs (from 504.3 to 527.2 DOT/1,000 patient-days). Moreover, in 2021, while use of reserve antimicrobials has decreased from 13.6 to 10.7 DOT/1,000 patient-days in TCHs and from 4.6 to 3.3 DOT/1,000 patient-days in SCHs, it has increased from 0.7 to 0.8 DOT/1,000 patient-days in PCHs. Conclusion: This study confirms that antimicrobial use differs by hospital type in Korea. Recent increases of use of antimicrobials, including reserve antimicrobials, in PCHs reflect the challenges that must be addressed.
Qualitative Evaluation of an Antimicrobial Stewardship Tele-Mentoring Program in US Rural & Critical Access Hospitals
- Elizabeth Moore, Ellen MacLachlan, Natalia Martinez-Paz, Maria Bajenov, Rupali Jain, Jeannie Chan, John Lynch, Paul Pottinger, Zahra Kassamali Escobar, Chloe Bryson-Cahn
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, pp. s58-s59
-
- Article
-
- You have access Access
- Open access
- Export citation
-
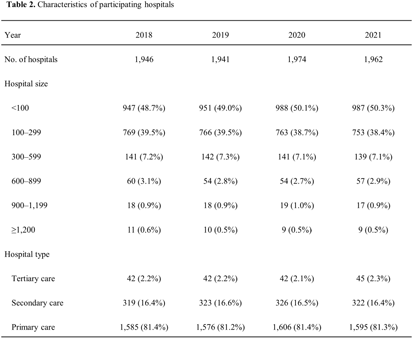
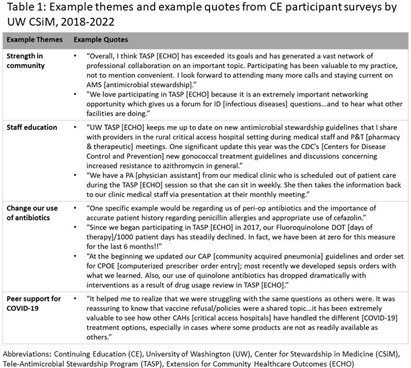
Background: The University of Washington (UW) Center for Stewardship in Medicine (CSiM) supports a tele-antimicrobial stewardship (AMS) program (TASP) using the ECHO approach (Extension for Community Healthcare Outcomes) in small, rural, and Critical Access Hospitals (primarily in the western U.S.) with education, mentoring, organizational capacity building, and a community of peers. To evaluate the continuing education (CE) component of UW-TASP ECHO, CSiM surveyed individuals receiving CE credits as part of the program. This survey was designed to track individuals’ satisfaction with the program and to assess the impact of UW-TASP ECHO on AMS in participating facilities. Methods: The CE participants’ survey was completed annually by individuals participating in UW TASP ECHO using online survey software. The survey included closed-ended and open-ended questions. Responses to open-ended questions were entered into Atlas.ti qualitative analysis software and coded iteratively according to themes that emerged. When a new code emerged partway through the coding process, earlier surveys were re-coded for the new code. Final codes were grouped into themes and sub-themes and quotes from each theme identified were summarized and attached to the theme and reported. Results: Data from three administrations of this survey were available: 2018-2019 (n=66); 2020-2021 (n=27); and 2021-2022 (n=30). These surveys were completed by a total of 95 individuals from 53 hospitals. Seven of these individuals completed a survey in each year, 14 completed a survey in two years, and 74 completed only one survey. Themes identified were COVID-19 support (including procedures and policies, being kept up-to-date, research summaries, and peer support), the antibiotic pocket guide developed by UW, strength in community, staff education, role of CSiM in developing/strengthening the AMS program at the facility, change in use of antibiotics, UW imprimatur, learning/growing as a healthcare provider, and importance for small, rural hospitals (see examples in Table 1). Conclusions: This qualitative analysis provides evidence from surveys of individuals participating in CE that UW TASP ECHO has had a meaningful impact in such domains as building a strong community among small, rural and critical access hospitals, educating staff, changing antibiotic use and providing peer support, among others.

Managerial Influence on Infection Prevention and Control (IPC) Implementation in Israeli Hospitals: A Doctoral Research Study
- Dafna Chen, Stefan Cojocaru
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, pp. s102-s104
-
- Article
-
- You have access Access
- Open access
- Export citation
-
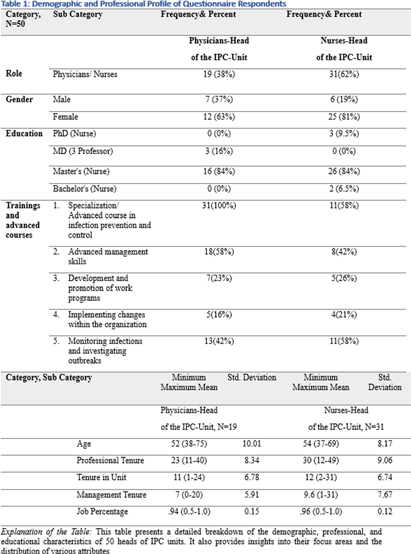
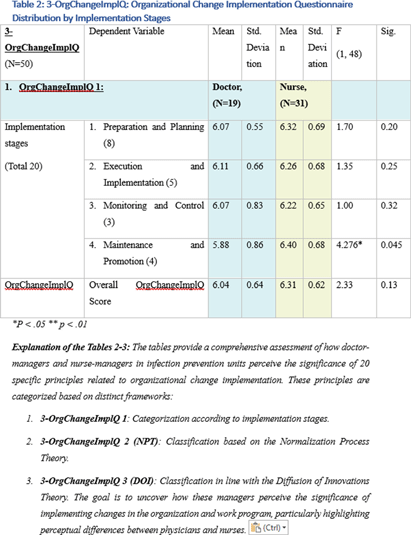
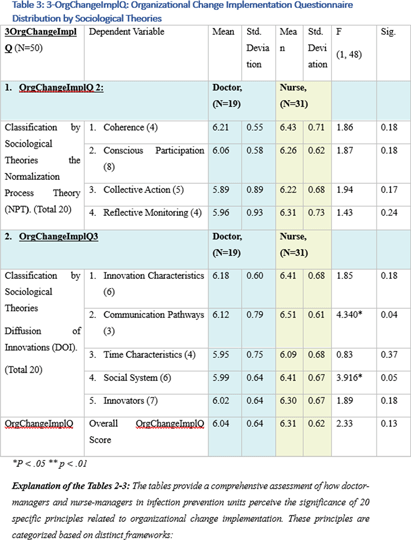
Background: This research, part of a doctoral study, aims to examine the impact of managerial factors on the implementation of Infection Prevention and Control (IPC) measures in Israeli hospitals. The study focuses on identifying key facilitators and barriers from the perspectives of physician and nurse managers, with an emphasis on understanding the integration of managerial strategies and theoretical frameworks in IPC implementation. Objective: The objective is to explore specific managerial factors, both facilitators and barriers, influencing the effective implementation of IPC measures. The research investigates these influences through the lens of physicians and nurses managing IPC units in public hospital settings. Methodology: A mixed-method approach was adopted, involving in-depth interviews with ten IPC-Unit managers (five physicians and five nurses) and a comprehensive questionnaire distributed among IPC-Unit heads. The study’s demographic and professional profiles of participants are detailed in Table 1. The data collection process encompassed an Activity Assessment Questionnaire (2-AAQ) and an Organizational Change Implementation Questionnaire (3-OrgChangeImplQ), with the distribution of responses categorized by implementation stages and sociological theories (Tables 2-4). Result: Managerial autonomy emerged as a significant catalyst for IPC implementation, with supportive leadership and resource allocation being critical. Differences in approaches between physician and nurse managers were observed, reflecting diverse strategies in planning, execution, monitoring, and maintenance of IPC measures. The findings also revealed a natural alignment with sociological theories, particularly Normalization Process Theory (NPT) and Diffusion of Innovations (DOI), despite a lack of formal training in these areas. Conclusions: The study underscores the multifaceted nature of IPC implementation, highlighting the importance of managerial autonomy, supportive leadership, and a deep understanding of organizational culture. The inherent alignment of IPC strategies with NPT and DOI theories suggests the potential of these frameworks in guiding IPC implementation. The research advocates for the integration of these theoretical perspectives into formal training programs to enhance the effectiveness of IPC measures in healthcare settings.
Environmental Fungal Contamination Characterization of Three Inpatient Units Utilizing Optimized Detection Methods
- Bobby Warren, Guerbine Fils-aime, Amanda Graves, Aaron Barrett, Matthew Steigel, Becky Smith, Ilan Schwartz, Deverick Anderson
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, pp. s97-s98
-
- Article
-
- You have access Access
- Open access
- Export citation
-
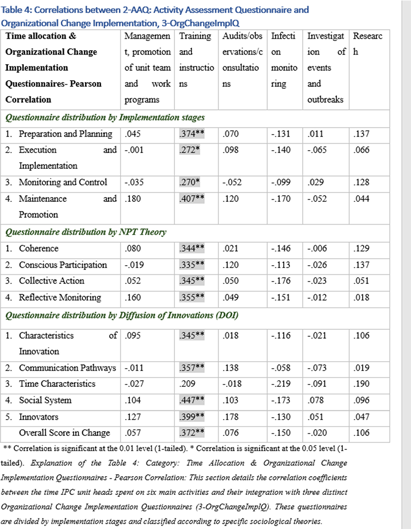
Background: Environmental sampling and detection methods for fungi in healthcare settings are not well-established. We previously refined methods for fungal sampling and detection in a controlled laboratory environment and aimed to validate them in a real-world healthcare setting. Methods: We performed a microbiological analysis of air and surfaces in three inpatient units at a tertiary care center. Surface samples were obtained with foam sponges from 3 locations in patient rooms (Patient bedrails, bathroom floor, HVAC export) and 5 locations in units (HVAC exports 3x, clean linen storage, soiled linen storage). Air samples were taken with an active air sampler directly below HVAC exports. Sponges were processed using the stomacher technique. Samples underwent DNA extraction followed by qPCR with FungiQuant primers targeting the 18S rRNA gene. Amplicons from positive samples were sequenced (NextSeq 1000, 300bp PE) and SmartGene databases were used to interpret sequence data. For comparison to culture methods, samples were also plated onto Sabouraud and HardyCHROM Candida + auris medias. Fungal growth underwent DNA extraction, 18S PCR and Sanger sequencing for genus and species identification. Results: A total of 85 samples were obtained, from 15 patient rooms and three units resulting in 61 surface and 24 air samples. Patients in study rooms had a median age of 53, 9 (60%) were male, and no patients had an invasive fungal infection during their hospital encounter. 44 (53%) and 39 (46%) samples were positive for fungi via qPCR and culture, respectively. Of the 44 positive qPCR samples, microbiome analyses identified at least one fungi to the species, genus and family levels in 43 (98%), 28 (64%), 18 (41%) samples, respectively (Table 1). 114 total isolates were identified of which the most common were Mallassezia restricta (30 [26%]), Malassezia globose (29 [25%]), and Pennicillium paradoxum (4 [4%]). 39 genera were identified of which the most common were Mucor (19 [49%]) and Candida (8 [21%]). Of the 39 culture positive samples, 90 total isolates were recovered. The most common species were Paradendryphiella arenariae (19 [21%]), Aspergillus niger (12 [13%]) and Penicillium commune (12 [13%]). Conclusion: These results demonstrate the presence of diverse fungal species in both air and surface samples across inpatient units. Higher sensitivity was noted utilizing qPCR, however, identified genera and species were markedly different between qPCR and culture methods. Larger studies are needed to assess the efficacy of qPCR for fungal detection in the healthcare environment.
Large-Scale S. aureus Screening with Molecular Epidemiology; the Role of MSSA and Community MRSA in Hospital Transmissions
- Courtney Takats, Gregory Putzel, Drew Siskin, Alejandro Pironti, Bo Shopsin, Sarah Hochman
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, p. s15
-
- Article
-
- You have access Access
- Open access
- Export citation
-
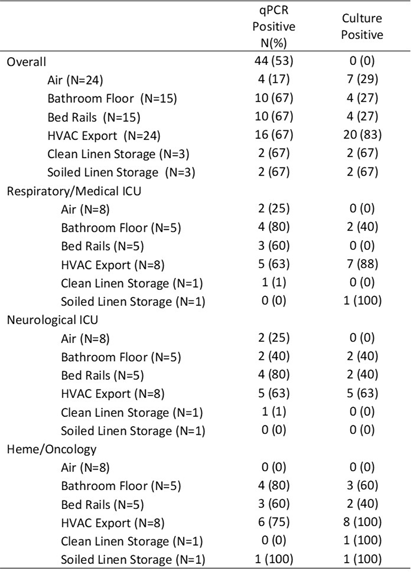
Background: The frequency of Staphylococcus aureus transmission in hospitals is unknown: symptomatic infection may occur months after transmission and colonization, and infection prevention efforts rely on indirect measurements, rather than direct detection of transmission events. We implemented a hospital-based S. aureus screening program, combined with whole genome sequencing of S. aureus surveillance and clinical cultures and data extracted from the electronic health record, to identify S. aureus clonal complex-, patient- and location-specific factors associated with S. aureus transmission in our health system. Methods: Screening S. aureus cultures were obtained at admission by nasal swab for adults admitted to Medicine, Transplant, Oncology and intensive care, and weekly by swab of nares, axilla and groin for children admitted to intensive care and Oncology at NYU Langone Health in New York City. All methicillin-resistant S. aureus (MRSA) from screening and clinical (blood, wound, sputum) cultures and all methicillin-susceptible S. aureus (MSSA) from screening and blood cultures underwent whole genome sequencing. Isolates from distinct patients with < 2 0 single nucleotide pair differences were considered genetically related. Electronic health data was extracted for descriptive statistics and for spatiotemporal plots to assess plausible transmissions. We used REDCap electronic data capture tools hosted at NYU Grossman School of Medicine and SAS software for data analysis to evaluate S. aureus transmissions between November 2022 and November 2023. Results: We analyzed 8,567 S. aureus isolates: including 6,552 screening cultures, 1,008 blood cultures, and 1,007 clinical cultures. We found 424 plausible S. aureus hospital transmissions using sequencing and electronic health data. Screening cultures identified 75% of transmissions that would have otherwise been missed with blood and clinical cultures alone. The majority of positive screening cultures isolated MSSA, but the proportion of transmissions due to MSSA differed by age. In children, MSSA colonization accounted for 62% of transmissions. In adults, only 15% of transmissions were due to MSSA colonization, whereas MRSA colonization accounted for 56% of transmissions. Analysis of adult MRSA isolates by clonal complex found that 45% of transmissions were due to CC8, higher than the 17% among isolates agnostic of transmissions. Emergency departments and the neonatal intensive care unit had the highest number of transmissions. Patients involved in transmissions had longer lengths of stay and frequent hospitalizations. Conclusions: A S. aureus screening program, coupled with genome sequencing and electronic health data, can identify patient group, hospital locations and clonal complexes that are at high risk for S. aureus transmissions.
Not Your Usual Exposure: Tuberculosis Contact Investigation Related to Contaminated Bone Allograft
- Christy Scipione, Laraine Washer, Emily Stoneman, Amanda Valyko, Jennifer Sweeney
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, pp. s125-s126
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Mycobacterium tuberculosis transmission through contaminated bone allograft product is unusual and was first described in 2021 with a second outbreak in 2023. In July 2023, Michigan Medicine conducted contact tracing for healthcare personnel (HCP), patients, and visitors following exposure to an immunocompromised patient with surgical site infection and subsequent widely disseminated tuberculosis (bacteremia, pulmonary, lymphadenopathy) following spinal fusion with bone allograft in April 2023. The patient was in the emergency department, operating room (OR), and inpatient units for 9 days prior to initiation of Airborne Precautions (AP). Methods: Michigan Medicine is a 1,107 bed academic hospital. HCP are screened for tuberculosis with interferon-gamma release assay (IGRA) testing upon hire and following tuberculosis exposure. Exposure testing includes baseline IGRA testing and follow-up testing at 10-12 weeks post exposure. Exposure criteria for this investigation was defined as sharing room airspace with the tuberculosis patient prior to initiation of airborne precautions or Central Sterile Processing Department (CSPD) staff involved with instrument decontamination without the use of a respirator. Of note, universal masking with surgical masks was not required during this time for staff and patients/visitors, with the exception of CSPD and OR staff. Contact tracing was performed by Infection Prevention and Occupational Health Services managed all test results and conversions. Results: 176 employees from perioperative care areas (n=30), CSPD (n=7), OR (n=9) and inpatient units (n=130) were IGRA tested. Five employee conversions were identified: one surgeon, one circulating OR nurse, two CSPD decontamination staff, and one respiratory therapist. At time of detection, none of the conversions had evidence of active tuberculosis. Additionally, 46 patients and visitors were tested with zero conversions. HCP compliance with IGRA testing was initially 15% before engagement from hospital and unit leadership and human resources. With intervention, employee compliance reached 100%. Conclusion: Despite standard use of surgical masks for OR and CSPD staff, aerosolization of infected bone graft material played an important role in tuberculosis transmission during surgery and instrument cleaning. Respiratory therapy practices in the ICU setting likely also increased risk for pulmonary tuberculosis transmission. Achieving 100% HCP compliance for baseline and follow-up IGRA testing is challenging and requires engagement of both unit and hospital leadership and human resources to ensure all HCP are tested.
Validation and Use of a Measure in Critical Access Hospitals to Reduce Treatment of Asymptomatic Bacteriuria
- Hannah Imlay, Claire Ciarkowski, Zahra Kassamali Escobar, Chloe Bryson-Cahn, Adam Hersh, Natalia Martinez-Paz, Whitney Hartlage, Jeannie Chan, Hannah Hardin, Andrea White, Chaorong Wu, Valerie Vaughn
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, pp. s81-s82
-
- Article
-
- You have access Access
- Open access
- Export citation
-
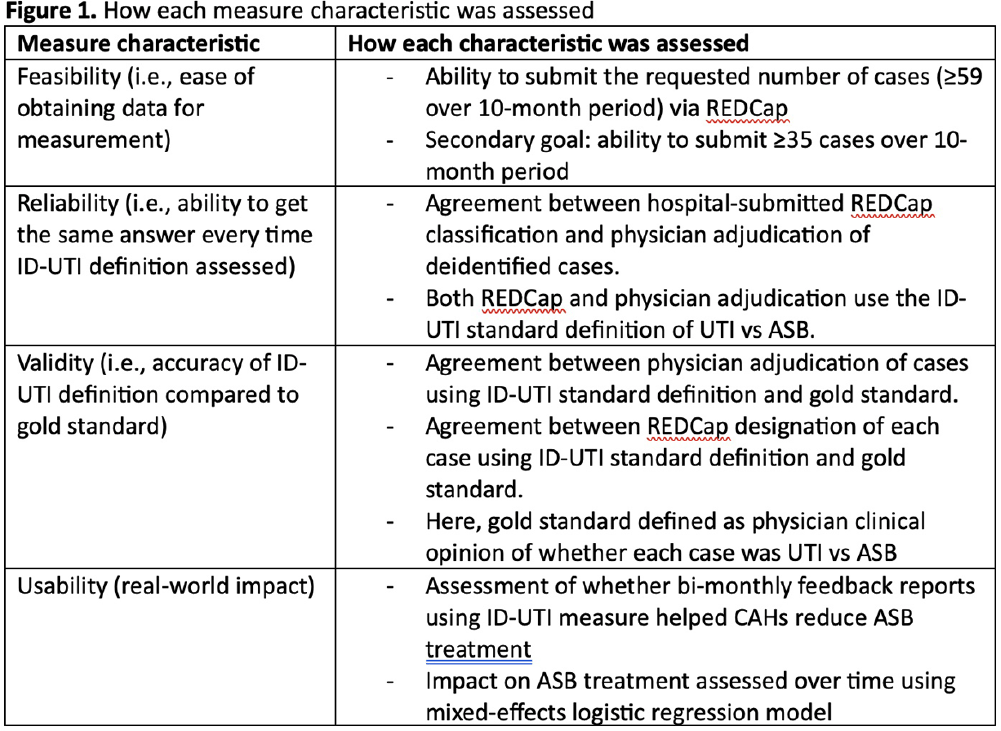
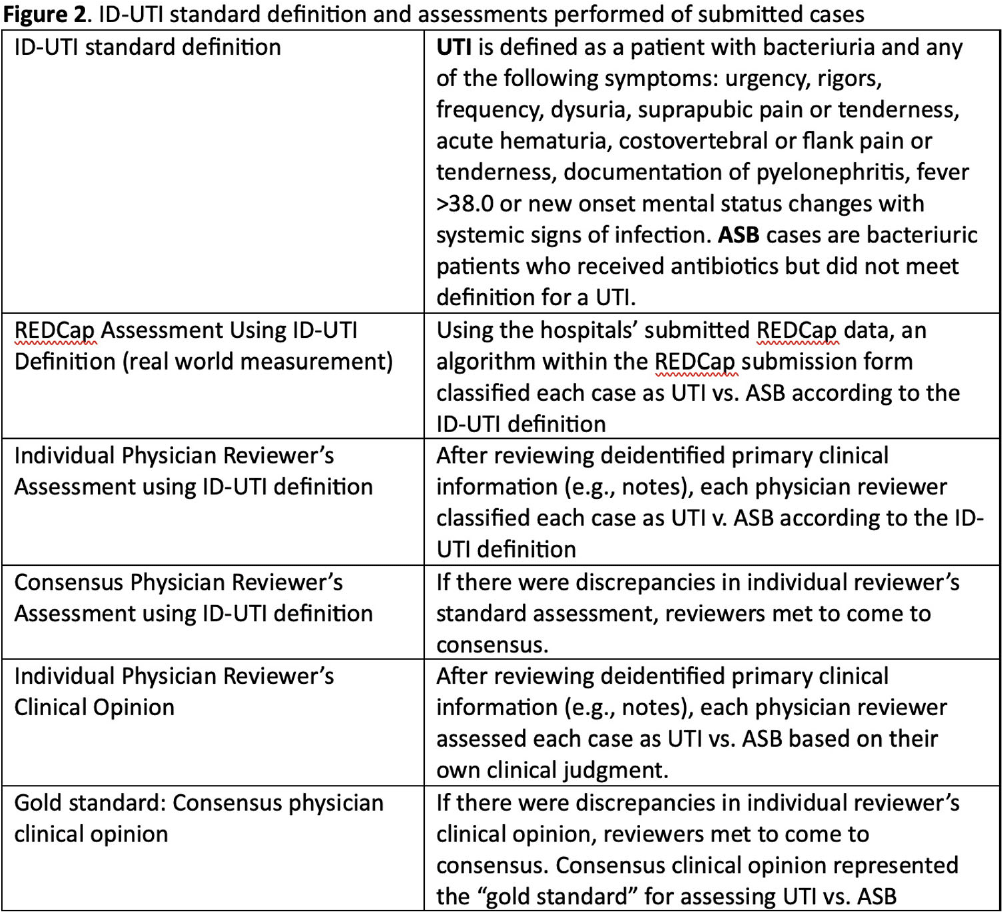
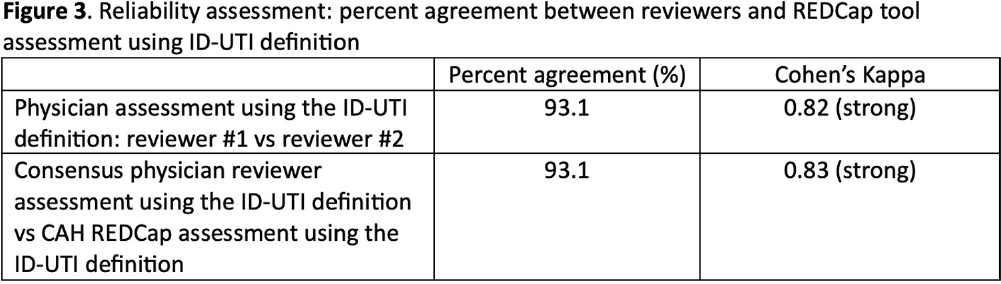
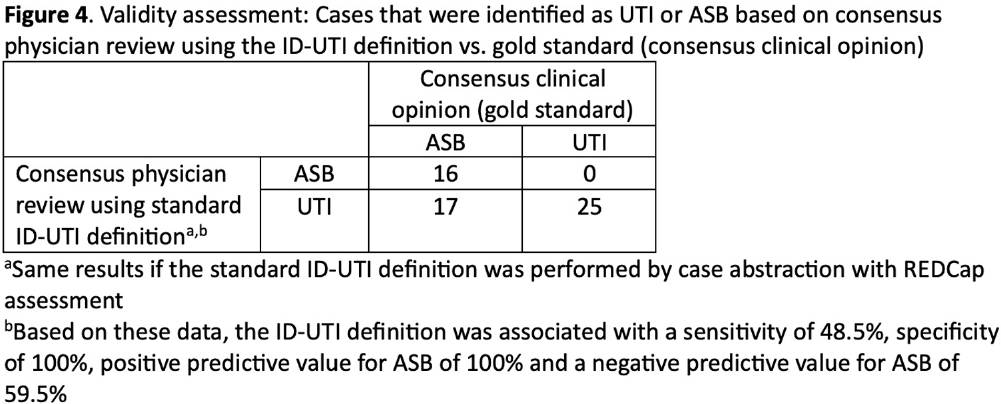
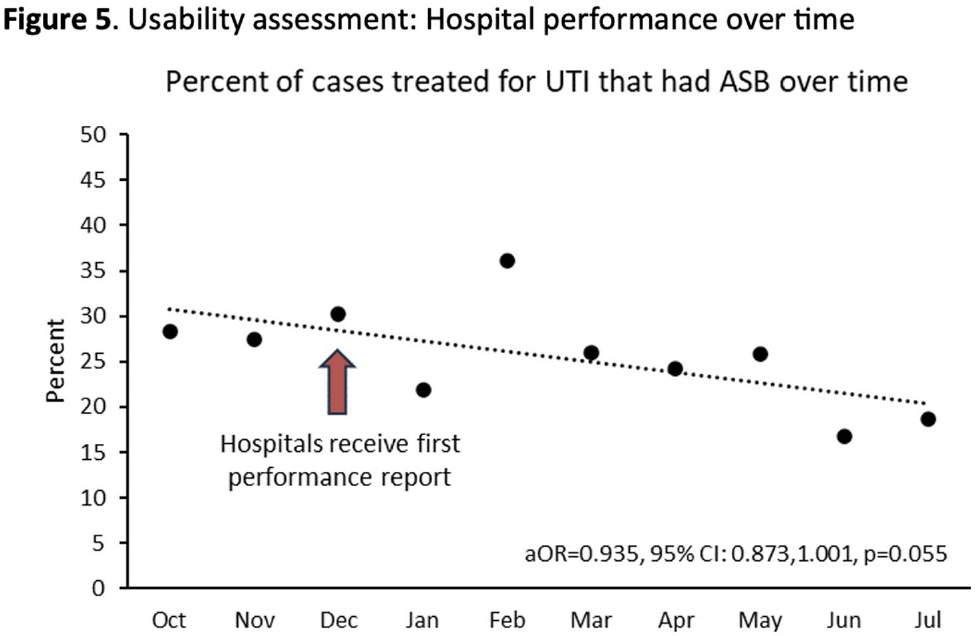
Background: Inappropriate diagnosis and treatment of urinary tract infections (UTI) contributes to antibiotic overuse. The Inappropriate Diagnosis of UTI (ID-UTI) measure—which quantifies the percentage of treated bacteriuria that is asymptomatic (ASB) using a standard definition of UTI—has been validated in acute care hospitals, but not in critical access hospitals (CAHs) where resources differ. Methods: From October 2022-July 2023, ten CAHs participated in a program to reduce ASB treatment, including education, coaching, and hospital feedback using the ID-UTI measure. Our primary aim was to assess performance characteristics of the ID-UTI standard definition and measure in CAHs (Figure 1). Non-physician abstractors from each CAH submitted clinical data (e.g., signs/symptoms) via REDCap for consecutive adult patients who were admitted or discharged from the emergency department and received antibiotics for bacteriuria. The case abstraction goal for each CAH was 5-6 cases/month. To assess feasibility, we evaluated the ability of each CAH to achieve goal case abstractions. To assess validity and reliability of the ID-UTI standard definition, two physicians reviewed 10% of submitted cases using deidentified patient notes and assessed agreement with the standard ID-UTI definition and consensus clinical opinion. Based on submitted data, we provided bi-monthly feedback reports to CAHs including the hospital-level ID-UTI measure to benchmark progress and for peer comparison. We measured monthly change in the ID-UTI measure using a mixed-effects logistic regression model (Figure 1, Figure 2). Results: Among 10 CAHs, 4 (40%) submitted >59 cases over 10 months (goal) while 3 (30%) submitted >35 cases (secondary goal). Physician reviewers assessed 9.5% (58/608) of cases. Utilizing the ID-UTI standard definition, there was high agreement (93%) in ASB vs UTI designation between each physician reviewer and the CAH’s REDCap assessment (Figure 3). Compared to clinical opinion, the ID-UTI standard definition identified 48% (16/33) of ASB cases and 100% (25/25) of UTI cases (Figure 4). Over the program, the percentage of cases treated for UTI that were ASB decreased from 28.4% (range 0-63%) to 18.6% (range, 0-33%; p=0.055) (Figure 5). Conclusions: Case abstraction with use of the ID-UTI measure was feasible and reliable to implement with modifications for CAHs. Data collection by untrained staff was as reliable as physician adjudication. Though the ID-UTI standard definition undercounted ASB cases (low sensitivity), cases reported as ASB were always ASB when adjudicated (high specificity). The program, including performance feedback using the ID-UTI measure, was associated with a trend toward lower treatment of ASB.
Filtered handheld far-ultraviolet disinfection device in reducing environmental pathogens from high-touch clinical surfaces
- Layale Yaghi, Rita Wilson-Dib, Sherry Cantu, Piyali Chatterjee, Chetan Jinadatha, Roy Chemaly, Amy Spallone
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, p. s97
-
- Article
-
- You have access Access
- Open access
- Export citation
-
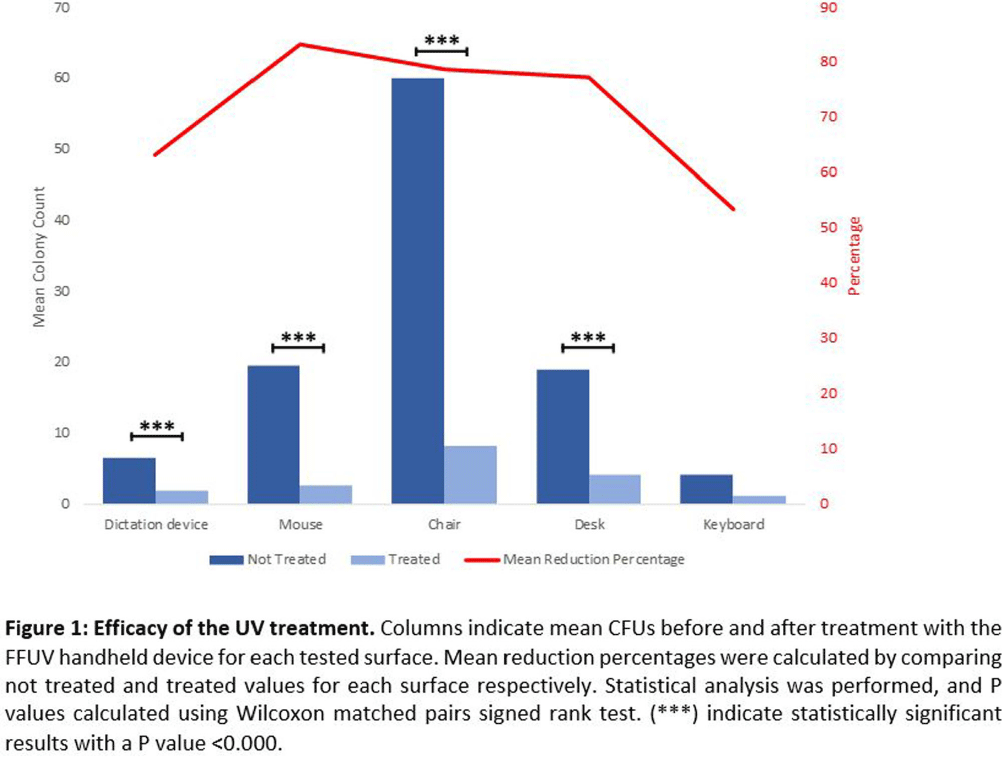
Background: Healthcare-acquired infections (HAIs) continue to be a major challenge. In fact, an increased risk of HAIs has been linked to high-touch surfaces contaminated with multidrug-resistant organisms (MDROs), and enhanced environmental disinfection is linked to reduced HAI rates. Recently, more focus has been placed on emerging disinfection technologies, such as UV light-producing portable device that emits light at a wavelength of 222 nm, which has previously demonstrated germicidal capabilities at short contact times. In this study, we aim i) to evaluate the efficacy of a filtered far-UV-C handheld device (FFUHH) to reduce bacterial loads on high-touch surfaces in clinical workrooms in a cancer center, and ii) to isolate, identify and establish a genetic relationship between these environmental clinically significant pathogens and the ones recovered from patients. Methods: Samples were collected weekly on a rotating schedule over a 24-week period from five high-touch items (dictation device, mouse, armchair, desk, and keyboard) in multiple clinical work rooms on hematologic malignancy and stem cell transplant units. Contact plates for colony count and swabs were collected pre- and post-intervention with the FFUHH on standardized adjacent areas respectively for each surface. The swabs were enriched and cultured on selective media to isolate clinically significant pathogens. Whole genome sequencing (WGS) was then performed on environmental pathogens validated by MALDI-TOF as well as clinical samples collected from patients in the same unit around the time of environmental sample collection. Results: A total of 440 plates, 220 pre- and 220 post-interventions, were collected and analyzed. The highest mean colony count pre-treatment was detected from the armchairs and the lowest for the keyboards. The mean reduction of colony forming units (CFUs) ranged between 53% for the keyboard and 83% for the mouse. The reduction was statistically significant across all surfaces with P values < 0.05, except for the keyboard (Figure 1). We isolated many pathogens of the human microbiota identified by MALDI-TOF such as Micrococcus luteus, S. capitis as well as methicillin-resistant S. epidermidis, S. haemolyticus and S. hominis. We also identified several Candida parapsilosis, Pseudomonas stutzeri, one Listeria grayi and one Acinetobacter baumanni. Finally, WSG allowed us to further characterize an environmental multi-drug resistant S. epidermidis ST5 strain associated with patient bacteremia, and ST16 strains detected on surfaces both pre- and post-FFUHH treatment. Conclusion: The FFUHH effectively reduced the microbial burden on high-touch surfaces in clinical workrooms on hematologic malignancy and stem cell units.
Ensuring Accuracy: Making the Case for Inter-rater Reliability in Hospital Acquired Infection Surveillance
- Kelly Holmes, Mishga Moinuddin, Sandi Steinfeld
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, pp. s147-s148
-
- Article
-
- You have access Access
- Open access
- Export citation
-
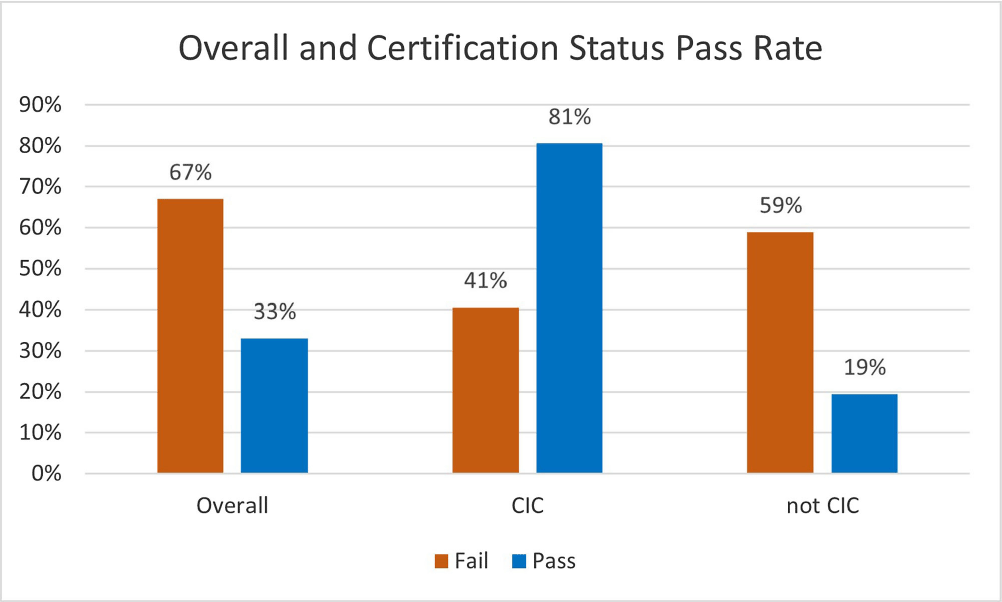
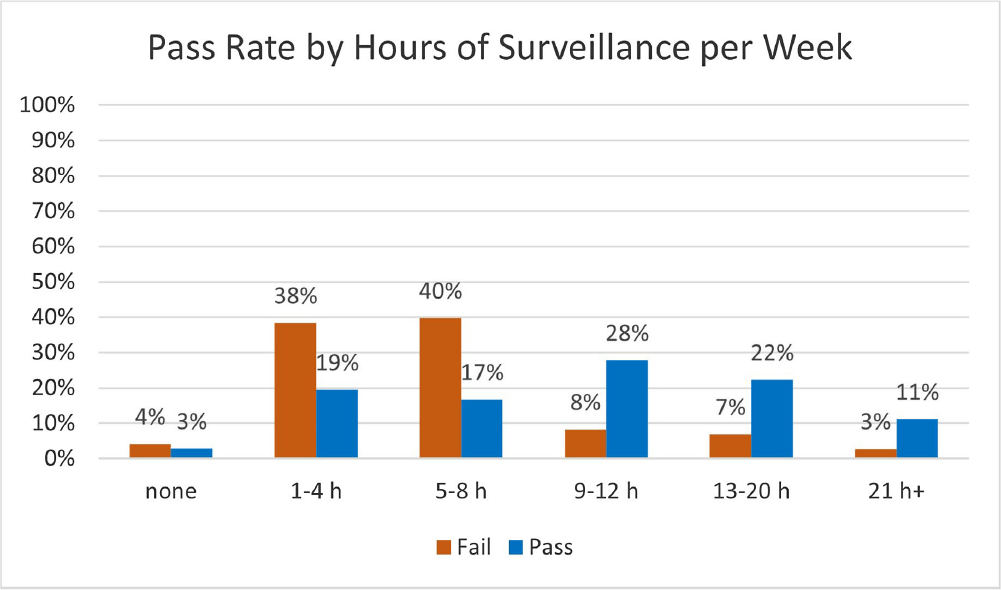
Background: Infection preventionists (Ips) have self-reported surveillance as the most time-consuming job task (1,2). APIC’s MegaSurvey 2020 reported that 60% of Ips consider themselves proficient or expert within this competency domain (2). Accurate coding of health care acquired infections is critical to identifying epidemiologically significant events, using data to improve practice, and compliance with state and federal mandated CMS reporting (3,4). Validated case study scenarios were distributed to infection preventionists to better understand how experience level and time spent performing surveillance affects interrater reliability (IRR) in applying the National Healthcare Safety Network (NHSN) surveillance definitions (5,6). Methods: Case study scenarios determined to have high item discrimination were added to an online test bank and distributed annually to Ips of varying experience levels and care settings as part of a mandatory training program (5). The test bank currently consists of forty-two validated questions. Each year, the participants receive approximately thirty questions, including twenty randomly selected from the test bank and ten beta scenarios under development. Only validated test bank scenarios are used to calculate the passing score of 85%. Participants are blinded to which questions are test bank scenarios versus beta scenarios. Additional information was gathered at the beginning of the test to determine CIC status, years of experience, and weekly hours spent doing surveillance. Data was analyzed for passing score on the first attempt for testing years 2019, 2021, 2022, and 2023. Results: Thirty-six Ips passed the IRR test on the first attempt (33%). Of those who passed on the first attempt, twenty-nine (81%) were certified and twenty-two (61%) reported at least nine hours a week performing surveillance. Of the seventy-three Ips (67%) who did not pass on the first attempt, thirty were certified (41%) and sixty (82%) reported performing surveillance for 8 hours or less per week. Conclusion: The first-time pass rate for certified and non-certified Ips was 33%, markedly lower than the self-reported proficiency rate of 60%. The majority of Ips who passed on the first attempt were certified and spent at least nine hours per week performing surveillance. certified and non-certified Ips who did not regularly perform surveillance as part of their weekly job tasks were less likely to pass the test on the first attempt. Given the first-time pass rate among all participants is below optimal, establishing inter-rater reliability systems and ongoing surveillance education for Ips is crucial to ensure accuracy of publicly reported data.
From Swiffers to Solutions: The Impact of Environmental Sampling in the Veterinary Medical Center at OSU
- Christy King, Thomas Wittum, Dixie Mollenkopf, Dubraska Diaz-Campos, Joany Van Balen
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, p. s157
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: In 2018, the Ohio State University College of Veterinary Medicine (OSU CVM) implemented an Antimicrobial Stewardship Program, central to which was the integration of an environmental surveillance (ES) program. The ES focuses on pathogens recognized as urgent threats to public health by the Centers for Disease Control and Prevention. The pathogens currently targeted include carbapenemase-producing Enterobacterales (CPE), Salmonella spp., methicillin-resistant Staphylococcus spp. (MRSs), vancomycin resistant Enterococcus spp., and enrofloxacin resistant Pseudomonas aeruginosa. Identification of these pathogens allows the hospital to be aware of the local environmental microflora which can act as a sentinel for disease in the hospital, potentially causing healthcare associated infections. Therefore, the objective of this program is to identify resistant bacterial pathogens, characterize their resistance profiles, analyze prevalence patterns, and initiate infection control interventions where needed in the OSU VMC. Method: From January 2018 through December 2023, a total of 5449 samples were collected from approximately 86 locations across the OSU VMC encompassing the small animal, equine, and farm animal sections. A majority (64%, n=3561) of samples were collected from the small animal hospital, with the farm animal section contributing 1055 samples and the equine section 899. Areas sampled were frequented by both humans and animals, as well as surfaces exclusively touched by humans. Samples were collected using Swiffers® and processed through selective culture media. Result: Approximately half (52%, n=2890) of the samples collected represented human-touch only surfaces. A total of 3794 bacterial isolates were recovered, with an overall low prevalence for all targeted pathogens. Prevalence of CPE was 2% (n=103), with Enterobacter species being the most common. Recovery of MRSs was 8.5% (n=464) and Salmonella species was 1% (n=47). Conclusion: Through this initiative, the equine division of the OSU VMC collaborated with the antimicrobial stewardship team to enhance their Salmonella fecal and ES practices. In 2019, ES was critical in identifying persistent CPE and extended-spectrum cephalosporin-resistant Enterobacteriaceae in the ICU and surrounding areas of the small animal hospital. Effective measures were taken to halt the spread of ESC among patients and eliminate CPE in the environment. With the discovery of a new CPE in early 2023 in the small animal ICU and nearby areas, the program initiated targeted ES and cleaning and disinfection protocols, to identify contaminated areas and control disease transmission. These efforts have increased patient safety, health, and well-being, demonstrating how ES can be an important tool for infection control and prevention in veterinary settings.




























