Open access
Review Article
Effects of Smoking on COVID-19 Management and Mortality: An Umbrella Review
- SeyedAhmad SeyedAlinaghi, Amir Masoud Afsahi, Ramin Shahidi, Shaghayegh Kianzad, Zahra Pashaei, Maryam Mirahmad, Pooria Asili, Hengameh Mojdeganlou, Armin Razi, Paniz Mojdeganlou, Iman Amiri Fard, Sara Mahdiabadi, Arian Afzalian, Mohsen Dashti, Afsaneh Ghasemzadeh, Zohal Parmoon, Hajar Badri, Esmaeil Mehraeen, Daniel Hackett, Haniki Mohamed
-
- Published online by Cambridge University Press:
- 01 January 2024, e6
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Introduction. Smoking status appears to lead to a poor prognosis in COVID-19 patients. However, findings from the studies conducted on this topic have not been consistent, and further exploration is required. Methods. The objective of this umbrella review was to examine the effects of smoking on COVID-19 management and mortality. Online databases that included PubMed, Embase, Scopus, and Web of Science were searched using relevant keywords up to July 27, 2022. Articles were restricted to the English language, and the PRISMA protocol was followed. Results. A total of 27 systematic reviews, published from 2020 to 2022, were included. Individual studies included in the systematic reviews ranged from 8 to 186, with various population sizes. The consensus from the majority of systematic reviews was that COVID-19 smoker patients experience greater disease severity, disease progression, hospitalization rate, hospital admission duration, mechanical ventilation, ICU admission, and mortality rate. Conclusions. COVID-19 patients with a history of smoking (current and former) are vulnerable to adverse hospital outcomes and worse COVID-19 progression. Effective preventive and supportive approaches are required to decrease the risk of COVID-19 morbidity and mortality in patients with a history of smoking.
Research Article
“It Is A Carrot-Stick Model”: A Qualitative Study of Rural-Serving Clinician and Rural-Residing Veteran Perceptions of Requirements to Quit Smoking prior to Elective Surgery
- Sara E. Golden, Allison Young, Christina J. Sun, Marissa Song Mayeda, David A. Katz, Mark W. Vander Weg, Kenneth R. Gundle, Steffani R. Bailey, Deborah Ossip
-
- Published online by Cambridge University Press:
- 01 January 2024, e10
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Introduction. Some medical centers and surgeons require patients to stop smoking cigarettes prior to elective orthopaedic surgeries in an effort to decrease surgical complications. Given higher rates of smoking among rural individuals, rural patients may be disproportionately impacted by these requirements. We assessed the perceptions and experiences of rural-residing Veterans and clinicians related to this requirement. Methods. We conducted qualitative semistructured one-on-one interviews of 26 rural-residing veterans, 10 VA orthopaedic surgery staff (from two Veterans Integrated Services Networks), 24 PCPs who serve rural veterans (14 VA; 10 non-VA), and 4 VA pharmacists. Using the knowledge, attitudes, and behavior framework, we performed conventional content analysis. Results. We found three primary themes across respondents: (1) knowledge of and the evidence base for the requirement varied widely; (2) strong personal attitudes toward the requirement; and (3) implementation and possible implications of this requirement. All surgery staff reported knowledge of requirements at their institution. VA PCPs reported knowledge of requirements but typically could not recall specifics. Most patients were unaware. The majority of respondents felt this requirement could increase motivation to quit smoking. Some PCPs felt a more thorough explanation of smoking-related complications would result in increased quit attempts. About half of all patients reported belief that the requirement was reasonable regardless of initial awareness. Respondents expressed little concern that the requirement might increase rural-urban disparities. Most PCPs and patients felt that there should be exceptions for allowing surgery, while surgical staff disagreed. Discussion. Most respondents thought elective surgery was a good motivator to quit smoking; but patients, PCPs, and surgical staff differed on whether there should be exceptions to the requirement that patients quit preoperatively. Future efforts to augment perioperative smoking cessation may benefit from improving coordination across services and educating patients more about the benefits of quitting.
The Efficacy of Individualized, Community-Based Physical Activity to Aid Smoking Cessation: A Randomized Controlled Trial
- Michelle B. Stockton, Kenneth D. Ward, Barbara S. McClanahan, Mark W. Vander Weg, Mace Coday, Nancy Wilson, George Relyea, Mary C. Read, Stephanie Connelly, Karen C. Johnson, Haniki Mohamed
-
- Published online by Cambridge University Press:
- 01 January 2024, e4
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Objective. The efficacy of individualized, community-based physical activity as an adjunctive smoking cessation treatment to enhance long-term smoking cessation rates was evaluated for the Lifestyle Enhancement Program (LEAP). Methods. The study was a two-arm, parallel-group, randomized controlled trial. All participants (n = 392) received cessation counseling and a nicotine patch and were randomized to physical activity (n = 199; YMCA membership and personalized exercise programming from a health coach) or an equal contact frequency wellness curriculum (n = 193). Physical activity treatment was individualized and flexible (with each participant selecting types of activities and intensity levels and being encouraged to exercise at the YMCA and at home, as well as to use “lifestyle” activity). The primary outcome (biochemically verified prolonged abstinence at 7-weeks (end of treatment) and 6- and 12-months postcessation) and secondary outcomes (7-day point prevalent tobacco abstinence (PPA), total minutes per week of leisure time physical activity and strength training) were assessed at baseline, 7 weeks, 6 months, and 12 months. Results. Prolonged abstinence in the physical activity and wellness groups was 19.6% and 25.4%, respectively, at 7-weeks, 15.1% and 16.6% at 6-months, and 14.1% and 17.1% at 12 months (all between-group P values >0.18). Similarly, PPA rates did not differ significantly between groups at any follow-up. Change from baseline leisure-time activity plus strength training increased significantly in the physical activity group at 7 weeks (P = 0.04). Across treatment groups, an increase in the number of minutes per week in strength training from baseline to 7 weeks predicted prolonged abstinence at 12 months (P ≤ 0.001). Further analyses revealed that social support, fewer years smoked, and less temptation to smoke were associated with prolonged abstinence over 12 months in both groups. Conclusions. Community-based physical activity programming, delivered as adjunctive treatment with behavioral/pharmacological cessation treatment, did not improve long-term quit rates compared to adjunctive wellness counseling plus behavioral/pharmacological cessation treatment. This trial is registered with https://beta.clinicaltrials.gov/study/NCT00403312, registration no. NCT00403312.
Tobacco Use and Cessation among a Nationally Representative Sample of Men in India, 2019–2021
- S. K. Singh, Shubham Kumar, Gyan Chandra Kashyap, Kenneth Ward
-
- Published online by Cambridge University Press:
- 01 January 2024, e7
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Tobacco users are exposed to a higher risk of noncommunicable diseases, leading to premature mortality and disability-adjusted life years (DALYs). The future prediction indicates that tobacco-related mortality and morbidity rates will substantially increase in coming years. The study is aimed at assessing the prevalence of tobacco consumption and cessation attempts for different tobacco products among adult men in India. The study utilized information from India’s latest National Family Health Survey-5 (NFHS-5) data which was conducted during 2019-21, including 988,713 adult men aged 15 years and above and 93,144 men aged 15-49. Results suggest that 38 percent of men consume tobacco, including 29% in urban and 43% in rural areas. Among the men aged 35-49 years, the odds were significantly higher for consuming any form of tobacco (AOR: 7.36, CI: 6.72-8.05), smoking cigarettes (AOR: 2.56, CI: 2.23-2.94), and smoking bidi (AOR: 7.12, CI: 4.75-8.82) as compared to those aged 15-19. The application of multilevel model indicates that tobacco usages are not evenly distributed. In addition, there is maximum clustering of tobacco usages found around household level factors. Further, 30% of men aged 35-49 years attempted to stop consuming tobacco. Though 27% of men tried to quit tobacco in the last 12 months and 69% of men are exposed to secondhand smoke, 51% of men who received advice for quitting tobacco and visited the hospital in the last 12 months belong to the lowest wealth quintile. These findings prioritize promoting awareness about adverse effects of tobacco use, especially in rural areas, and capacitate them to adopt cessation efforts so that those who want to quit may be successful in their efforts. In addition, the health system’s response to the tobacco epidemic in the country should be strengthened by training of service providers to promote cessation efforts through appropriate counselling of all the patients visiting them in the context of tobacco use in any form as key drivers of the increasing burden of noncommunicable diseases (NCDs) in the country.
Review Article
Hospitalised Smokers’ and Staff Perspectives of Inpatient Smoking Cessation Interventions and Impact on Smokers’ Quality of Life: An Integrative Review of the Qualitative Literature
- Leah Epton, Shane Patman, Tracey Coventry, Caroline Bulsara, Kenneth Ward
-
- Published online by Cambridge University Press:
- 01 January 2024, e8
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Aim. To identify, integrate, and appraise the evidence on hospitalised smokers’ and staff perspectives of inpatient smoking cessation interventions and the impact on smokers’ quality of life. Design. The integrative review method was used to present hospitalised smokers’ and staff perspectives of inpatient smoking cessation interventions. Search Method. This integrative review consisted of a comprehensive search on smoking cessation interventions that take place during an inpatient admission to hospital for adults (> age 18 years) of the following online databases: Ovid Medline, Joanna Briggs Institute, APA PsycInfo, CINAHL, Cochrane, Google Scholar, PEDro, and Scopus. The search strategy was inclusive of peer-reviewed studies limited to the English language or translated to English. A search of grey literature and manual searching of reference lists was also conducted to identify further studies not identified in the online database search. All studies that produced any qualitative data (i.e., qualitative, mixed methods, and surveys) on inpatient-initiated smoking cessation programs were included. Outcomes of interest are included but were not limited to education, counselling, and the use of pharmacotherapy. Studies undertaken in the psychiatric, adolescent, and paediatric settings were excluded. Results. The key findings from this integrative review included positive evaluations from both patients and staff involved in inpatient smoking cessation interventions, reporting that hospitalisation was an appropriate opportunity to address smoking cessation. A number of facilitators and barriers to inpatient smoking cessation interventions included creating a supportive patient-centred environment and consideration of the cost of nicotine replacement therapy and time to deliver inpatient smoking cessation interventions. Recommendations/preferences for future inpatient smoking cessation interventions included the use of a program champion and ongoing education to demonstrate the effectiveness of the intervention, and despite the cost of nicotine replacement therapy being identified as a potential barrier, it was identified as a preference for most patients. Although quality of life was only evaluated in two studies, statistically significant improvements were identified in both. Conclusion. This qualitative integrative review provides further insight into both clinician and patient participants’ perspectives on inpatient smoking cessation interventions. Overall, they are seen to produce positive benefits, and staff training appears to be an effective means for service delivery. However, insufficient time and lack of resources or expertise appear to be consistent barriers to the delivery of these services, so they should be considered when planning the implementation of an inpatient smoking cessation intervention.
Research Article
Indexing Quit-Smoking Interest among Norwegian Smokers 2019-2021
- Gunnar Sæbø, Karl Erik Lund, Haniki Mohamed
-
- Published online by Cambridge University Press:
- 01 January 2024, e9
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Even if smoking prevalence is declining in several western countries, continued smoking cessation is required to reduce tobacco-related harms and to achieve future goals of smoke-free societies or the tobacco endgame. But how many of the current smokers want to quit? Estimates vary and depend on the type of question asked. We investigate how a pooled sample of Norwegian smokers (N = 1321) is distributed over four indicators of interest in quitting: (i) degree of desire to quit, (ii) prediction of future smoking status, (iii) reported plan for quitting smoking, and (iv) statements on previous attempts to quit. Based on these variables, we constructed an index. One-third of the smokers (32.6%) was categorized as having a high or very high interest in quitting. However, nearly half of the smokers (47.8%) had low or very low interest in quitting. Like several other countries, Norway has legislated a vision of a smoke-free society and, under the government’s plans; this goal will be achieved by intensified use of structural measures such as tax hikes, tighter restrictions on outdoor smoking, and reduced availability of cigarettes. For the third who want to quit smoking, such constraints on their behaviour may help them to pursue their desire to quit. However, for the half who want to continue smoking, these measures may not be helpful but instead be experienced as a loss of welfare, less freedom to act, and increased social disqualification.
Attitudes about Cigarette Smoking, Perceived Consequences of Smoking, and Seeking Assistance with Cessation among Black and White Cigarette Smokers: A Qualitative Study
- Alina Shevorykin, Lesia M. Ruglass, Roberta Freitas-Lemos, Alexandria G. Bauer, Shannyl Baez, Christine E. Sheffer, Haniki Mohamed
-
- Published online by Cambridge University Press:
- 01 January 2024, e5
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Introduction. Research has identified significant racial differences in cigarette smoking behavior, associated disease risk, likelihood of cessation, and mortality from smoking-related diseases. The current study assessed, via qualitative narrative analysis, racial differences in participants’ motivations for smoking, perceived consequences of smoking, and how participants deal with cravings/withdrawal, as well as thoughts and feelings about quitting, seeking assistance with quitting, and the importance of social support in quitting. Methods. Semistructured interviews were conducted with 11 Black and 11 White cigarette smokers. Data were analyzed using the Thematic Networks Analysis process, which entailed coding the data and constructing thematic networks by identifying basic and organizing themes. Results. While there were no descriptive racial differences identified in participants’ motivation for smoking or perceived consequences of smoking, differences existed between Blacks and Whites in terms of approaches in dealing with smoking cravings and withdrawal, perceived self-efficacy in controlling cravings, preferred methods of learning about and receiving smoking cessation assistance, and overall preference for receiving cessation-related support. Conclusions. Further investigation is needed into racial differences in methods to deal with cigarette cravings and withdrawal, preferences for receiving cessation information, and social support for cessation. This research will further develop our understanding of and ability to address factors underlying racial disparities in smoking behavior and cessation, as well as inform the development of future smoking cessation interventions.
Prevalence, Correlates, and Perception of E-cigarettes among Undergraduate Students of Kathmandu Metropolitan City, Nepal: A Cross-Sectional Study
- Gayatri Khanal, Abhishek Karna, Suresh Kandel, Hari Krishna Sharma, Kenneth Ward
-
- Published online by Cambridge University Press:
- 01 January 2024, e11
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Introduction. The use of e-cigarettes has been increasing globally especially among the youth population due to rigorous advertisement, marketing, and promotion which has become a significant public health concern. Hence, this study is aimed at identifying the prevalence, correlates, and perception of e-cigarettes among undergraduate students of Kathmandu city. Methods. A cross-sectional study was conducted among 405 undergraduates of capital city of Nepal from April 2022 to December 2022. A two-stage systematic random sampling was used to select the respondents. An anonymous, semistructured, self-administered questionnaire was used for data collection. A descriptive, bivariable, and multivariable analysis was done using SPSS version 20. Results. The prevalence of ever use and current use of e-cigarettes was 21.2% and 5.9%, respectively. Number of close friends (AOR = 5.23, CI: 1.26, 16.39), number of friends using e-cigarettes (AOR = 7.23, CI: 0.93, 22.82), male sex (AOR = 2.88, CI: 2.15, 10.35), and age (COR = 5.07, CI: 0.93, 8.19) were the major predictors of current e-cigarette usage. Similarly, number of friends using e-cigarettes (AOR = 5.90, CI: 2.15, 10.35), male sex (AOR = 3.53, CI: 2.15, 10.35), age (COR = 4.56, CI: 0.98, 6.24), and place of residence (COR: 5.19, CI: 0.83, 8.02) were the major predictors of ever e-cigarette usage. The prevalence of e-cigarette consumption was higher in males than females (5.4% vs. 0.5%). Approximately, 34.8% respondents had perceived e-cigarettes as a means to help in smoking cessation. 56.5% adults knew that e-cigarettes promoted conventional smoking. Majority (64.7%) of the undergraduate students had presumed e-cigarettes as less harmful to conventional smoking. Conclusion. Ever use, current use, and misconception on e-cigarettes were widespread among the undergraduate students. Age, male sex, number of close friends, number of peers using e-cigarette, and place of residence were the major predictors for e-cigarette usage. To deal with the increased e-cigarette consumption state, awareness on the harmful addictive properties of e-cigarettes along with its adverse health consequences must be propagated and an appropriate intervention must be implemented.
Integrating the “Quit and Stay Quit Monday” Model into Smoking Cessation Services for Smokers with Mental Health Conditions: A Pilot Randomized Controlled Trial
- Mahathi Vojjala, Christina N. Wysota, Ololade Oketunbi, Quiann King, Erin S. Rogers, Kenneth Ward
-
- Published online by Cambridge University Press:
- 01 January 2024, e2
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Introduction. People with mental health conditions (MHCs) are less likely to achieve long-term abstinence than people without MHCs. The Quit and Stay Quit Monday (QSQM) model offers a long-term approach to treating tobacco use by encouraging people to quit, requit, or recommit to quit smoking every Monday. Aim. To evaluate the efficacy, patient satisfaction, and patient engagement with an intervention that integrated the QSQM model into multicomponent smoking cessation services among people with an MHC. Methods. This was a randomized controlled pilot trial. Eligibility criteria were as follows: (1) ≥18 years old, (2) smoked a cigarette in the past 30 days, (3) diagnosis of an ICD-10 MHC, (4) interest in quitting smoking, (5) able to receive services in English, and (5) had an active email and a cell phone. The intervention group (n = 33) received QSQM-focused telephone coaching, a weekly QSQM email newsletter, a SmokefreeTXT anchored around a Monday quit date, and 4 weeks of nicotine replacement therapy (NRT). The control group (n = 36) received information about contacting their state Quitline for usual services. Primary outcomes were self-reported quit attempts, 7-day abstinence, and intervention satisfaction at 3 months. Results. Twenty-four participants (73%) in the intervention group began telephone coaching, 26 (79%) enrolled in the QSQM email newsletter, 19 (58%) enrolled in SmokefreeTXT, and 15 (46%) used NRT. Using a penalized intent-to-treat approach, quit attempts in the intervention and control groups were 63.6% and 38.9% (OR 2.75, 95% CI 1.03-7.30), respectively. Seven-day abstinence in the two groups was 12.1% and 5.6% (OR 2.35, 95% CI 0.40-13.74), respectively. Of the 15 intervention group participants who set a quit date during the intervention, 13 (86.7%) selected a Monday quit day. Qualitative interviews revealed positive participant experiences with picking a Monday quit day. On follow-up surveys, 89.5%, 69.3%, and 64.3% of intervention participants reported that the counseling, QSQM email, and text messaging, respectively, were very or somewhat helpful. Conclusions. The QSQM model was acceptable and potentially efficacious among people with MHCs, but intervention engagement and satisfaction were modest. Future research should adapt or develop new QSQM delivery approaches to improve patient engagement and potential efficacy of the model. This trial is registered with clinicaltrials.gov (NCT04512248).
The Evaluation of an Integrated Tobacco Treatment Specialist in Primary Care
- Rachel E. Miller, Jennifer M. Hill, Amanda F. Meyer, Kenneth Ward
-
- Published online by Cambridge University Press:
- 01 January 2024, e1
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background. Primary care providers play a key role in screening for tobacco use and assessing desire to quit. Tobacco treatment specialists (TTS) are certified in helping patients who desire tobacco cessation. A primary care nurse practitioner within one Midwestern healthcare organization obtained TTS certification and integrated specialized tobacco cessation visits within a primary care clinic from February 2021 to February 2022. Purpose. To determine the efficiency and effectiveness of an integrated TTS-certified nurse practitioner (TTS-NP) in a primary care setting 1-year postimplementation. Method. This program evaluation utilized retrospective electronic health record review and included thirty-three patients. The logic model served as a framework to define efficiency and effectiveness. Results. Patients were referred by a provider (57.6%), nurse (15.2%), or self (27.3). Patients opted for in-person initial visits (81.8%) more than virtual (18.2%). Of a total of 73 scheduled visits, 8 (11%) were no-showed. Patients who self-referred had the lowest no-show rate (5.6%) compared to those referred by a provider (12.8%) or nurse (12.5%). Of the patients included, 87.9% set a goal quit date. Average time until first and second follow-up was 34.6 and 130.4 days after goal quit date. Follow-up was defined as the date of the patient’s first message reply to the TTS-NP, or first visit following the goal quit date. A total of 51.9% (n = 14) and 63% (n = 17) reported cessation at the first and second follow-up. TTS-NP visit’s cost, independent of any other coverage, was less than other specialty visits in primary care. Conclusion. TTS-NP visits in primary care enabled patients to benefit from lower cost and longitudinal follow-up within a familiar setting. Over half of patients achieved cessation. Results of this program evaluation suggest support for TTS-certified providers in primary care.
Review Article
Patients’ Views on Medical Events in Lung Cancer Screening as Teachable Moments for Smoking Behaviour Change: A Systematic Review and Metasynthesis
- Anvita Vikram, Claire Muller, Lucy Hulme, Kenneth Ward
-
- Published online by Cambridge University Press:
- 01 January 2024, e3
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Although medical events in lung cancer screening (LCS) such as receiving scan results or interactions with clinicians are recognised as teachable moments (TMs), the views of patients about why this is the case for smoking behaviour change remain uncertain. This systematic review and metasynthesis study is aimed at identifying the reasons why patients believed that medical events during LCS act as TMs for smoking behaviour change. A search strategy was developed for use with MEDLINE, PsycINFO, EMBASE, CINAHL-P, Web of Science databases, and Google Scholar. This helped identify qualitative and mixed-method research which mentioned patients’ views of how these TMs result in smoking behaviour change. After screening, final articles were critically appraised; general characteristics and data relevant to the aims were extracted to conduct a line-of-argument metasynthesis. After screening 695 papers, 11 were included. Undergoing LCS scans was seen to act on their intrinsic motivation to reduce smoking as it served as a “wake-up call” and increased awareness of the health consequences of smoking. Receiving positive or negative LCS results resulted in cessation as it was a “health scare” and challenged smoking habits. Interactions with clinicians addressed misconceptions and signposted them to specialist cessation services. Attendees believed that the following encouraged them to change their smoking behaviour: having an intrinsic motivation to quit, their beliefs on smoking and health reframed, their negative emotions appraised, and using LCS to access specialist support. In line with the TM heuristic, these experiences provided the necessary skills, confidence, and motivation to quit. Future research should explore whether the views of the clinicians match those of the attendees to address misconceptions and further develop clinical guidelines.
Research Article
If You Pay, Will They Come? Evaluating the Impact of Subsidies on Cessation Outcomes in the Walk or Run to Quit Program
- Kelly B. Wunderlich, Daniel Do, Hannah Martin, Carly S. Priebe, Guy E. J. Faulkner, Kenneth Ward
-
- Published online by Cambridge University Press:
- 01 January 2024, e7
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Introduction. Exercise interventions may assist smoking cessation attempts. One such publicly available 10-week program, Walk or Run to Quit (WRTQ), demonstrated success in smoking cessation and physical activity (PA) outcomes. However, initial WRTQ participants (2016-2017) were fairly homogenous in their demographic profile. To increase diversity, subsidies for participation were offered in 2018. This study assessed how the subsidies affected participant demographics, running frequency, smoking cessation, intention to quit, and program attendance and completion. Methods. The $70 registration fee was subsidized for 41% of participants in 2018. A pre-postdesign was used, with participants completing surveys on their demographics and smoking and physical activity behaviours. Descriptive statistics compared the year subsidies were available (2018) and unsubsidized years (2016-2017) and subsidized and unsubsidized participants’ data from 2018. Results. The 2018 participants had lower average attendance and program completion rates compared to 2016-2017 and no statistically significant differences in demographics or smoking cessation and PA outcomes. There were no differences in smoking cessation, run frequency, or demographic variables between the subsidized and unsubsidized participants in 2018. Conclusions. Offering subsidies did not diversify the participant profile. Subsidies did not have a negative impact on attendance nor primary outcomes. Subsidies may not have addressed barriers that prevented a more diverse sample from participating in WRTQ, such as program location, timing, and design. Equitable access to smoking cessation programs remains essential. As subsidies may play a role in reducing financial barriers disproportionately faced by marginalized groups, the implementation of, and recruitment for, such subsidized programs requires further investigation.
Review Article
How Electronic Cigarette Affects the Vascular System
- Vito Anggarino Damay, Setiawan Setiawan, Ronny Lesmana, Mohammad Rizki Akbar, Antonia Anna Lukito, Renee Bittoun
-
- Published online by Cambridge University Press:
- 01 January 2024, e4
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
The popularity of the electronic cigarette has soared in the last decades. However, the health effect of smoking electronic cigarettes on the vascular system is unclear. This systematic review examines the electronic cigarettes’ effect on the vascular system from recent evidence. A systematic search was conducted in MEDLINE (PubMed) database from January 2016 to August 2021 for studies assessing the vascular effect of chronic use of electronic cigarettes on human and animal. The Cochrane Risk of Bias 2, NIH Quality Assessment for Cross-Sectional Study, and SYRCLE’s Risk of Bias were used to assess the risk of bias in interventional, observational, and animal study, respectively. A narrative synthesis of evidence is provided to describe results. From 101 retrieved studies related to electronic cigarettes effect on the vascular system, a total of 16 studies are included in this review. The overall results indicated that electronic cigarette use is associated with adverse events in the vascular, including the incident of elevated oxidative stress, endothelial dysfunction, inflammation, arterial stiffness, and the development of atherosclerotic lesion. Further studies should broaden perspectives and reveal more about the mechanism of how electronic cigarettes impact on vascular system.
Research Article
Estimated Failure to Report Unsuccessful Quit Attempts by Type of Cessation Aid: A Population Survey of Smokers in England
- Olga Perski, Robert West, Jamie Brown, Haniki Mohamed
-
- Published online by Cambridge University Press:
- 01 January 2024, e13
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Introduction. It has been estimated that smokers tend to fail to report unsuccessful quit attempts that lasted a short time and occurred a longer time ago. However, it is unclear whether the failure to report unsuccessful quit attempts varies by the type of cessation aid used. Methods. A total of 5,892 smokers aged 16+ years who had made 1+ quit attempts in the past year were surveyed between January 2014 and December 2020 as part of the Smoking Toolkit Study. Respondents indicated when their most recent quit attempt started, how long it lasted, and which cessation aid(s) were used (e.g., unaided, varenicline, and behavioural support). The percentage failure to report for each cessation aid and 95% bootstrap confidence intervals (CIs) were estimated with an established method. Test for equality of proportions was performed to examine whether quit attempts lasting between one day and one week and that started >6 months ago failed to be reported at a different rate depending on the cessation aid used. Results. We estimated that after three months, 97% (95% CI = 96%-98%) of unaided quit attempts lasting less than one day, 80% (95% CI = 79%-81%) of those lasting between one day and one week, and 60% (95% CI = 59%-61%) of those lasting between one week and one month fail to be reported. Compared with unaided attempts, the estimated percentage failure to report quit attempts that lasted between one day and one week and that started >6 months ago was significantly lower for attempts involving behavioural support (92% of unaided attempts vs. 75% of attempts involving behavioural support,
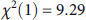 , p = 0.002). No other significant differences were detected. Conclusions. Smokers in England appear to fail to report a substantial proportion of unsuccessful quit attempts. This failure appears particularly prominent for attempts that last a short time or occurred longer ago and appears lower for attempts involving behavioural support compared with unaided attempts.
, p = 0.002). No other significant differences were detected. Conclusions. Smokers in England appear to fail to report a substantial proportion of unsuccessful quit attempts. This failure appears particularly prominent for attempts that last a short time or occurred longer ago and appears lower for attempts involving behavioural support compared with unaided attempts.
Modeling Health Event Impact on Smoking Cessation
- Edwin D. Boudreaux, Erin O’Hea, Bo Wang, Eugene Quinn, Aaron L. Bergman, Beth C. Bock, Bruce M. Becker, Haniki Mohamed
-
- Published online by Cambridge University Press:
- 01 January 2024, e14
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background. This study examined how cognitive and affective constructs related to an acute health event predict smoking relapse following an acute cardiac health event. Methods. Participants were recruited from emergency departments and completed cognitive and emotional measures at enrollment and ecological momentary assessments (EMA) for 84 days postvisit. Results. Of 394 participants, only 35 (8.9%) remained abstinent 84 days postvisit. Time to relapse was positively associated with age, actual illness severity, self-efficacy, and quit intentions. Conclusions. Older, seriously ill patients with strong confidence and intentions to quit smoking remain abstinent longer after discharge, but most still relapse within three months.
Effects of Smoking on Aggression, Big Five Personality Factors, and Polymorphisms in HTR2A, DRD4, and MAOA among Egypt University Students
- Marina Aboelsaad, Omar Soliman, Ahmed Medhat, Omar Khalil, Mawada AlWahsh, Yasmeen Wageh, Amira ElSaied, Hadeer ElShrkawy, Huda Abdulhafiz, Moustafa Sayed, Renee Bittoun
-
- Published online by Cambridge University Press:
- 01 January 2024, e6
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Introduction. To find genetic variants in the DRD4 and HTR2A genes’ promoter regions and exons that are associated with tobacco smoking and nicotine addiction in Egyptian university students as well as to study the association between personality traits and smoking status. Methods. A self-administered questionnaire about cigarette smoking and personality attributes (Big Five Inventory, ESPAD Questionnaire on Substance Abuse, and Buss-Perry Aggression Questionnaire). The participants in the study were 90 nonsmokers (NS) and 88 current smokers (CS), who were divided into two groups depending on their cigarette consumption per day (cpd): 55 heavy smokers (HS, >20 cpd) and 33 light smokers (LS, 1–10 cpd). Four and eight single nucleotide polymorphisms (SNPs) in the DRD4, HTR2A, and MOA genes, respectively, were genotyped. Results. Smokers scored lower on neuroticism, agreeableness, conscientiousness, openness, and extraversion than nonsmokers, but higher on aggression. Furthermore, the C allele of rs1800955 in DRD4 was associated with cigarette smoking in the HS vs. NS and LS vs. NS studies. The T allele of the HTR2A rs6313 gene was discovered to be strongly associated with cigarette smoking. There was no link discovered between MOA rs1137070 and MOA rs1137070. Conclusions. Using a comprehensive personality model (FFM), this study repeats and extends earlier research. Personality and genetic studies may aid in the development of a more complete and conclusive understanding of cigarette smoking, as well as more precise policies and guidelines for smoking cessation and quitting.
Review Article
Colliding Epidemics: Research Gaps and Implementation Science Opportunities for Tobacco Use and HIV/AIDS in Low- and Middle-Income Countries
- Mark Parascandola, Gila Neta, Michele Bloch, Satish Gopal, Kenneth Ward
-
- Published online by Cambridge University Press:
- 01 January 2024, e11
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Introduction. Tobacco use is a leading cause of cancer death among people living with HIV (PLWH) worldwide, and smoking prevalence tends to be higher among PLWH. The burden of both HIV/AIDS and tobacco use is increasingly concentrated in low- and middle-income countries (LMICs), where resources to address these challenges are often limited. However, there has been limited effort to date to integrate tobacco cessation into HIV programs in LMICs. Methods. We searched the literature (searching was conducted between October 1 and December 31, 2020) using PubMed including search terms “tobacco” and “HIV” and “cessation” over the past ten years (searching for articles published between December 1, 2010, and December 1, 2020) to identify original research studies on tobacco cessation interventions conducted in LMICs for PLWH. We also conducted an analysis of NCI-funded research grants on tobacco cessation and HIV awarded during fiscal years 2010 to 2020. Results and Discussion. Existing evidence suggests that conventional tobacco cessation treatments may be less effective among PLWH. Moreover, while substantial evidence exists to support a range of cessation interventions, most of this evidence comes from HICs and is only partly applicable to the evolving social, economic, and cultural climate of many LMICs. There is an urgent need to develop, adapt, and implement effective tobacco control and cessation interventions targeted to PLWH in LMICs, as well as to generate evidence from these settings. Implementation science provides tools develop and test strategies to overcome barriers and to integrate and scale up cessation services within existing HIV treatment settings. Conclusion. There is a unique opportunity to address HIV and tobacco use in a coordinated way in LMICs by integrating evidence-based tobacco cessation into HIV programs.
Research Article
Knowledge, Attitudes, and Beliefs about Relapse Prevention Research Involving Bupropion among Current and Former Pregnant Individuals Who Smoke
- Melissa Adkins-Hempel, Sandra J. Japuntich, Janet Thomas, Pearl Fang, Katherine Harrison, Rebecca L. Emery Tavernier, Jonathan P. Winickoff, Michael Kotlyar, Sharon Allen, Kenneth Ward
-
- Published online by Cambridge University Press:
- 01 January 2024, e1
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Introduction. While many individuals quit smoking during pregnancy, most relapse within one year postpartum. Research into methods to decrease smoking relapse postpartum has been hampered by difficulties with recruitment. Method. We conducted individual interviews with pregnant women (N = 22) who were interested in quitting smoking while pregnant about their attitudes regarding smoking and quitting during pregnancy, clinical trial participation, and smoking cessation medication use. Results. Participants were aware of the risks of smoking while pregnant. Many wanted to quit smoking before delivery. Few used empirically supported treatments to quit. While research was viewed positively, interest in taking on new commitments postpartum and taking a medication to prevent relapse was low. Medication concerns were evident among most participants, especially among those planning to breastfeed. Further, several women noted medication was unnecessary, as they did not believe they would relapse postpartum. Financial incentives, childcare, and fewer and/or remote visits were identified as facilitators to participating in research. However, these factors did not outweigh women’s concerns about medication use and time commitments. Conclusions. Women are aware that quitting smoking during pregnancy and remaining smoke-free postpartum are important. However, beliefs that personal relapse risk is low and that medications are dangerous reduced enthusiasm for taking medication for postpartum relapse prevention. Future medication trials should educate women about the high likelihood of relapse, prepare to answer detailed questions about risks of cessation medications, and connect with participants’ clinicians. For new mothers, studies conducted remotely with few scheduled appointments would reduce barriers to participation.
A Qualitative Study of Factors Influencing Implementation of Tobacco Control in Pediatric Practices
- Emara Nabi-Burza, Jonathan P. Winickoff, Jeremy E. Drehmer, Maurice P. Zeegers, Bethany Hipple Walters, Kenneth Ward
-
- Published online by Cambridge University Press:
- 01 January 2024, e12
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Introduction. Clinical effort against secondhand smoke exposure (CEASE) is an evidence-based intervention that prepares child healthcare clinicians and staff with the knowledge, skills, and resources needed to ask family members about tobacco use, provide brief counseling and medication assistance, and refer to free cessation services. Aim. This study sought to identify factors that influenced the implementation of CEASE in five pediatric intervention practices in five states that participated in a cluster randomized clinical trial of the CEASE intervention. Methods. Guided by questions from the consolidated framework for implementation research (CFIR) interview guide, semistructured qualitative interviews were conducted with 11 clinicians and practice staff from five intervention practices after the practices had implemented CEASE for two years. Interviews were conducted by a trained qualitative researcher, recorded with permission, and transcribed verbatim. An interview codebook was inductively developed; two researchers used the codebook to code data. After coding, data was analyzed to identify factors, as described by the CFIR domains that influenced the implementation of CEASE. Results. The implementation of CEASE in practices was influenced by the adaptability and complexity of the intervention, the needs of patients and their families, the resources available to practices to support the implementation of CEASE, other competing priorities at the practices, the cultures of practices, and clinicians’ and office staffs’ knowledge and beliefs about family-centered tobacco control. Conclusion. Identifying and influencing certain critical factors guided by information gathered through interviews may help improve implementation and sustainability of family-centered tobacco control interventions in the future. Trial Registration: ClinicalTrials.gov Identifier: NCT01882348.
Integration of a Tobacco Treatment Specialist into Primary Care: Perception from Multidisciplinary Team
- Amanda F. Meyer, Abby Cervenka, Lacey Lammers, Joseph Furst, Kenneth Ward
-
- Published online by Cambridge University Press:
- 01 January 2024, e10
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background. Tobacco continues to be on the leading cause of avoidable death. Primary care practices are ideal locations to provide tobacco cessation visits. Tobacco treatment specialists are trained individuals with expertise in providing medication and counseling management to patients to help with tobacco cessation. Purpose. The purpose of this study was to examine the integration of a tobacco treatment specialist into the primary care setting and the perception of this role from the multidisciplinary team. Method. We conducted an electronic cross-sectional survey to evaluate awareness and perception of the integration of a tobacco treatment specialist into a primary care facility that is part of a large Midwestern tertiary healthcare center. The sample for this study included all the primary clinic staff that directly work with patients and included licensed practical nurses, registered nurses, physician assistants, certified nurse practitioners, and medical doctors. Results. 55% (n = 22) of staff had utilized the tobacco treatment specialist with direct patient care. Reasons for using the specialist was for referral for follow-up tobacco cessation visit (54%), curbside consultations (21%), medication management (21%), and other reasons (5%). The majority of staff strongly agreed that utilizing the TTS was valuable. Conclusion. This study reinforced the positive impact a tobacco treatment specialist can have being integrated into the primary care practice from the perception of the multidisciplinary team.